Submitted:
19 June 2024
Posted:
20 June 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Intervention
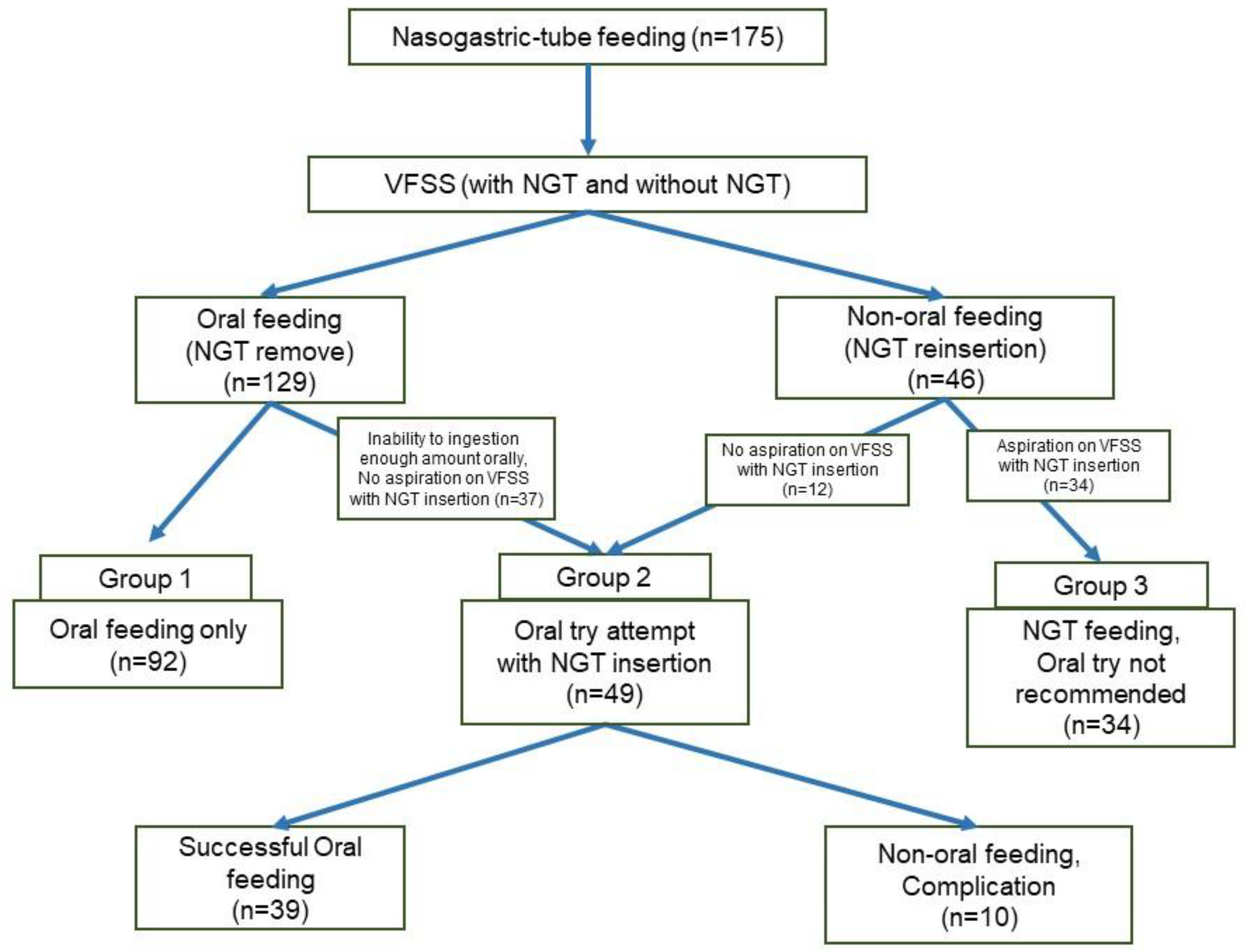
2.2. Patient Grouping
2.3. Evaluations
3. Results
4. Discussion
4.1. Factors Associated with Successive Oral Feeding
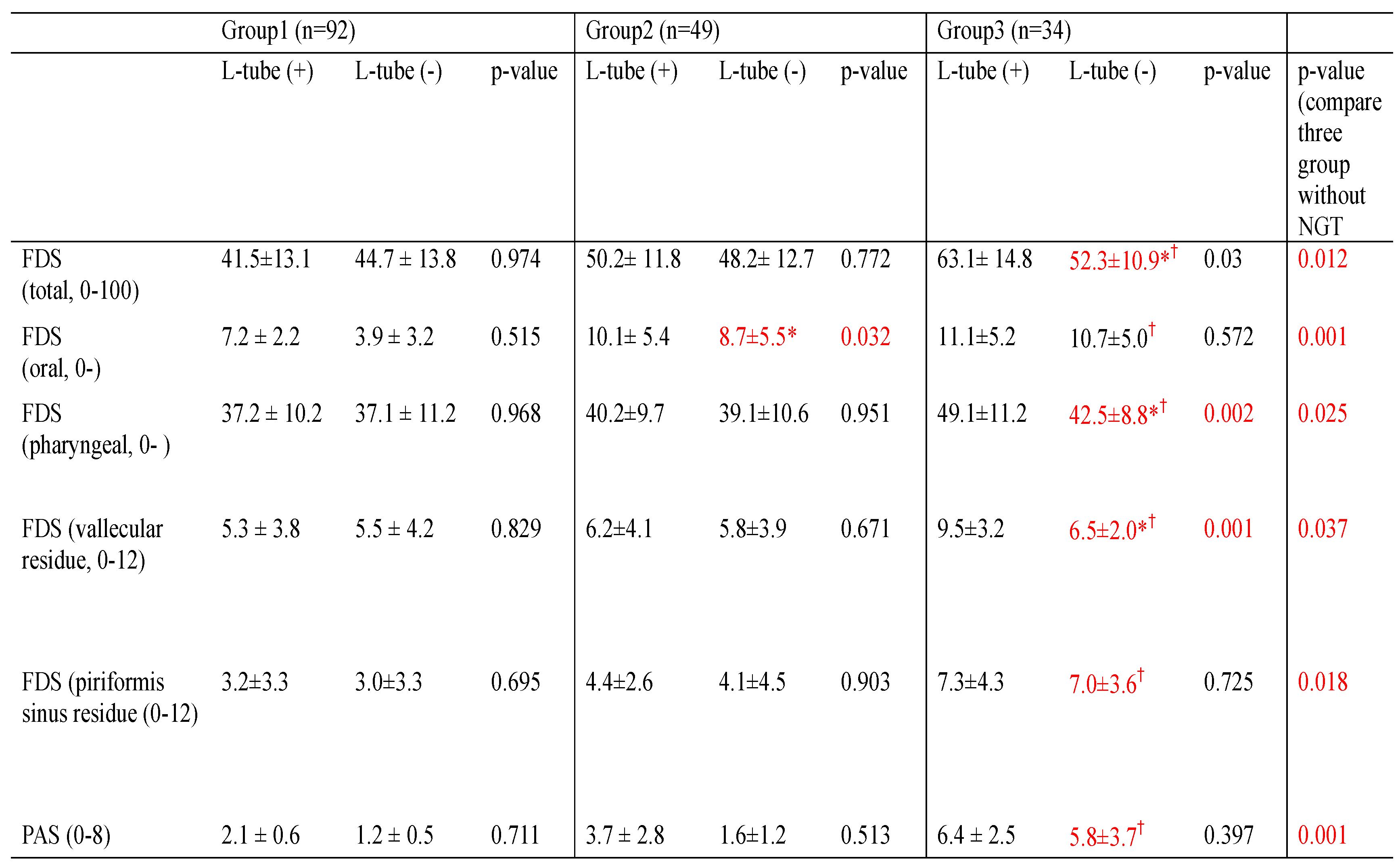
4.2. Effect of NGT on Swallowing Function
4.3. Therapeutic Effect of Oral Diet Training with an Indwelling NGT
4.4. Percutaneous Endoscopic Gastrostomy Tube Insertion
4.5. Limitations
5. Conclusions
6. Patents
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Disclosures
Abbreviations
| FDS: functional dysphagia scale |
| NGT: nasogastric tube |
| PAS: penetration aspiration scale |
| PEG: percutaneous endoscopic gastrostomy |
| VFSS: videofluoroscopic swallowing study |
Appendix A. The VFSS video file of Group 2 patient (swallowing with NGT insertion)
Appendix B. The VFSS video file of Group 3 patient (swallowing with NGT insertion)
References
- Gomes, G.F.; Pisani, J.C.; Macedo, E.D.; Campos, A.C. The nasogastric feeding tube as a risk factor for aspiration and aspiration pneumonia. Curr Opin Clin Nutr Metab Care 2003, 6, 327–333. [Google Scholar] [CrossRef]
- Shin, H.K.; Koo, K.I.; Hwang, C.H. Intermittent Oroesophageal Tube Feeding via the Airway in Patients With Dysphagia. Ann Rehabil Med 2016, 40, 794–805. [Google Scholar] [CrossRef] [PubMed]
- Kim, G.; Baek, S.; Park, H.W.; Kang, E.K.; Lee, G. Effect of Nasogastric Tube on Aspiration Risk: Results from 147 Patients with Dysphagia and Literature Review. Dysphagia 2018, 33, 731–738. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.Y.; Chen, J.M.; Ni, G.X. Effect of an indwelling nasogastric tube on swallowing function in elderly post-stroke dysphagia patients with long-term nasal feeding. BMC Neurol 2019, 19, 83. [Google Scholar] [CrossRef] [PubMed]
- Galovic, M.; Stauber, A.J.; Leisi, N.; Krammer, W.; Brugger, F.; Vehoff, J.; Balcerak, P.; Müller, A.; Müller, M.; Rosenfeld, J. , et al. Development and Validation of a Prognostic Model of Swallowing Recovery and Enteral Tube Feeding After Ischemic Stroke. JAMA Neurol 2019, 76, 561–570. [Google Scholar] [CrossRef] [PubMed]
- Lee, W.H.; Lim, M.H.; Seo, H.G.; Seong, M.Y.; Oh, B.M.; Kim, S. Development of a Novel Prognostic Model to Predict 6-Month Swallowing Recovery After Ischemic Stroke. Stroke 2020, 51, 440–448. [Google Scholar] [CrossRef] [PubMed]
- Gomes, C.A., Jr.; Andriolo, R.B.; Bennett, C.; Lustosa, S.A.; Matos, D.; Waisberg, D.R.; Waisberg, J. Percutaneous endoscopic gastrostomy versus nasogastric tube feeding for adults with swallowing disturbances. Cochrane Database Syst Rev 2015, 2015, Cd008096. [Google Scholar] [CrossRef]
- Dietrich, C.G.; Schoppmeyer, K. Percutaneous endoscopic gastrostomy - Too often? Too late? Who are the right patients for gastrostomy? World J Gastroenterol 2020, 26, 2464–2471. [Google Scholar] [CrossRef]
- Tae, C.H.; Lee, J.Y.; Joo, M.K.; Park, C.H.; Gong, E.J.; Shin, C.M.; Lim, H.; Choi, H.S.; Choi, M.; Kim, S.H. , et al. Clinical practice guidelines for percutaneous endoscopic gastrostomy. Clin Endosc 2023, 56, 391–408. [Google Scholar] [CrossRef]
- Wong, A.; Sowa, P.M.; Banks, M.D.; Bauer, J.D. Home Enteral Nutrition in Singapore’s Long-Term Care Homes-Incidence, Prevalence, Cost, and Staffing. Nutrients 2019, 11. [Google Scholar] [CrossRef]
- Hsu, C.Y.; Lai, J.N.; Kung, W.M.; Hung, C.H.; Yip, H.T.; Chang, Y.C.; Wei, C.Y. Nationwide Prevalence and Outcomes of Long-Term Nasogastric Tube Placement in Adults. Nutrients 2022, 14. [Google Scholar] [CrossRef]
- Li, Y.; Xu, Z.; Zhang, X.; Ma, D.; Meng, X.; Zhang, M.; Sun, J. Predictors of complete oral feeding resumption after feeding tube placement in patients with stroke and dysphagia: A systematic review. J Clin Nurs 2023, 32, 2533–2546. [Google Scholar] [CrossRef] [PubMed]
- Palmer, J.B.; Kuhlemeier, K.V.; Tippett, D.C.; Lynch, C. A protocol for the videofluorographic swallowing study. Dysphagia 1993, 8, 209–214. [Google Scholar] [CrossRef]
- Han, T.R.; Paik, N.J.; Park, J.W. Quantifying swallowing function after stroke: A functional dysphagia scale based on videofluoroscopic studies. Arch Phys Med Rehabil 2001, 82, 677–682. [Google Scholar] [CrossRef]
- Rosenbek, J.C.; Robbins, J.A.; Roecker, E.B.; Coyle, J.L.; Wood, J.L. A penetration-aspiration scale. Dysphagia 1996, 11, 93–98. [Google Scholar] [CrossRef]
- Kimura, Y.; Takahashi, M.; Wada, F.; Hachisuka, K. Differences in the peak cough flow among stroke patients with and without dysphagia. J uoeh 2013, 35, 9–16. [Google Scholar] [CrossRef] [PubMed]
- Park, M.K.; Lee, S.J. Changes in Swallowing and Cough Functions Among Stroke Patients Before and After Tracheostomy Decannulation. Dysphagia 2018, 33, 857–865. [Google Scholar] [CrossRef]
- Huggins, P.S.; Tuomi, S.K.; Young, C. Effects of nasogastric tubes on the young, normal swallowing mechanism. Dysphagia 1999, 14, 157–161. [Google Scholar] [CrossRef] [PubMed]
- Pryor, L.N.; Ward, E.C.; Cornwell, P.L.; O’Connor, S.N.; Finnis, M.E.; Chapman, M.J. Impact of nasogastric tubes on swallowing physiology in older, healthy subjects: A randomized controlled crossover trial. Clin Nutr 2015, 34, 572–578. [Google Scholar] [CrossRef]
- Robbins, J.; Hamilton, J.W.; Lof, G.L.; Kempster, G.B. Oropharyngeal swallowing in normal adults of different ages. Gastroenterology 1992, 103, 823–829. [Google Scholar] [CrossRef]
- de Sire, A.; Ferrillo, M.; Lippi, L.; Agostini, F.; de Sire, R.; Ferrara, P.E.; Raguso, G.; Riso, S.; Roccuzzo, A.; Ronconi, G. , et al. Sarcopenic Dysphagia, Malnutrition, and Oral Frailty in Elderly: A Comprehensive Review. Nutrients 2022, 14. [Google Scholar] [CrossRef] [PubMed]
- Goldsmith, T. Evaluation and treatment of swallowing disorders following endotracheal intubation and tracheostomy. Int Anesthesiol Clin 2000, 38, 219–242. [Google Scholar] [CrossRef] [PubMed]
- Betts, R.H. POST-TRACHEOSTOMY ASPIRATION. N Engl J Med 1965, 273, 155. [Google Scholar] [CrossRef]
- Shaker, R.; Milbrath, M.; Ren, J.; Campbell, B.; Toohill, R.; Hogan, W. Deglutitive aspiration in patients with tracheostomy: effect of tracheostomy on the duration of vocal cord closure. Gastroenterology 1995, 108, 1357–1360. [Google Scholar] [CrossRef]
- Kwak, H.J.; Kim, L.; Ryu, B.J.; Kim, Y.H.; Park, S.W.; Cho, D.G.; Lee, C.J.; Ha, K.W. Influence of Nasogastric Tubes on Swallowing in Stroke Patients: Measuring Hyoid Bone Movement With Ultrasonography. Ann Rehabil Med 2018, 42, 551–559. [Google Scholar] [CrossRef] [PubMed]
- Nam du, H.; Jung, A.Y.; Cheon, J.H.; Kim, H.; Kang, E.Y.; Lee, S.H. The Effects of the VFSS Timing After Nasogastric Tube Removal on Swallowing Function of the Patients With Dysphagia. Ann Rehabil Med 2015, 39, 517–523. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.G.; Wu, M.C.; Chang, Y.C.; Hsiao, T.Y.; Lien, I.N. The effect of nasogastric tubes on swallowing function in persons with dysphagia following stroke. Arch Phys Med Rehabil 2006, 87, 1270–1273. [Google Scholar] [CrossRef] [PubMed]
- Cosentino, G.; Todisco, M.; Giudice, C.; Tassorelli, C.; Alfonsi, E. Assessment and treatment of neurogenic dysphagia in stroke and Parkinson’s disease. Curr Opin Neurol 2022, 35, 741–752. [Google Scholar] [CrossRef]
- Min, K.C.; Seo, S.M.; Woo, H.S. Effect of oral motor facilitation technique on oral motor and feeding skills in children with cerebral palsy : a case study. BMC Pediatr 2022, 22, 626. [Google Scholar] [CrossRef]
- Arvedson, J.; Clark, H.; Lazarus, C.; Schooling, T.; Frymark, T. The effects of oral-motor exercises on swallowing in children: an evidence-based systematic review. Dev Med Child Neurol 2010, 52, 1000–1013. [Google Scholar] [CrossRef]
- Ikegami, T.; Kobayashi, M.; Matsumoto, S. FACTORS ASSOCIATED WITH ORAL INTAKE ABILITY IN PATIENTS WITH ACUTE-STAGE STROKE. J Rehabil Med Clin Commun 2021, 4, 2657. [Google Scholar] [CrossRef] [PubMed]
| Parameters | Group 1 (n=92) | Group 2 (n=49) | Group 3 (n=34) | p-value |
| Age | 74.7±11.2 | 68.2±24.5 | 82.4±10.9 | 0.037 |
| Gender (M/F) | 58/34 | 22/27 | 18/16 | |
| Cause of Dysphagia | ||||
| Stroke | 66 (71.7%) | 34 (69.4%) | 20 (58.8%) | |
| Hemorrhagic | 32 (34.8%) | 8 (16.3%) | 14 (41.2%) | |
| Ischemic | 34 (37.0%) | 26 (53.1%) | 6 (17.6%) | |
| Traumatic brain injury | 12 (13.0%) | 8 (16.3%) | 0 | |
| Parkinson | 0 | 2 (4.1%) | 5 (14.7%) | |
| ALS | 0 | 1 (2.0%) | 1 (3.0%) | |
| Myopathy | 3 (3.3%) | 2 (4.1%) | 0 | |
| Dementia | 8 (8.7%) | 0 | 6 (17.6%) | |
| Others (medical condition) | 3 (3.3%) | 2 (4.1%) | 2 (5.9%) | |
| L-tube feeding duration (days) | 51.6±35.4 | 66.1±40.6 | 79.1±14.8 | 0.01 |
| Tracheostomy | 2 (2.2%) | 13 (26.5%) | 19 (55.9%) | 0.001 |
| PCF | 168.0±78.5 | 138.7±28.5 | 84.4±47.2 | 0.001 |
| MBI | 38.3±12.6 | 21.4±9.0 | 19.6±14.5 | 0.951 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




