Submitted:
09 June 2024
Posted:
12 June 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
- Describing the current challenges with AI-driven decision-making in HIS.
- Undertaking studies regarding AI-powered decision-making in HIS.
- Evaluating specific AI-driven methodologies for advantages, drawbacks, datasets, and simulations.
- Highlighting important features of particular methodologies for subsequent research.
- Investigating research approaches based on AI.
2. Related Works
3. Methodology of Research
3.1. Formalization of Question
Research Question 1: How can AI-driven decision-making processes in the field of HIS be classified? The answer to this question is in Part 5.
Research Question 2: What approaches do scholars use to do their research? Parts 5.1 through 5.7 answer this question.
Research Question 3: What parameters received the greatest attention in the papers? What is the most common AI-driven decision-making methodologies used in HIS? The answer to this question is found in section 6.
Research Question 4: What untapped opportunities exist in this area? section 7 provides the answer to this question.
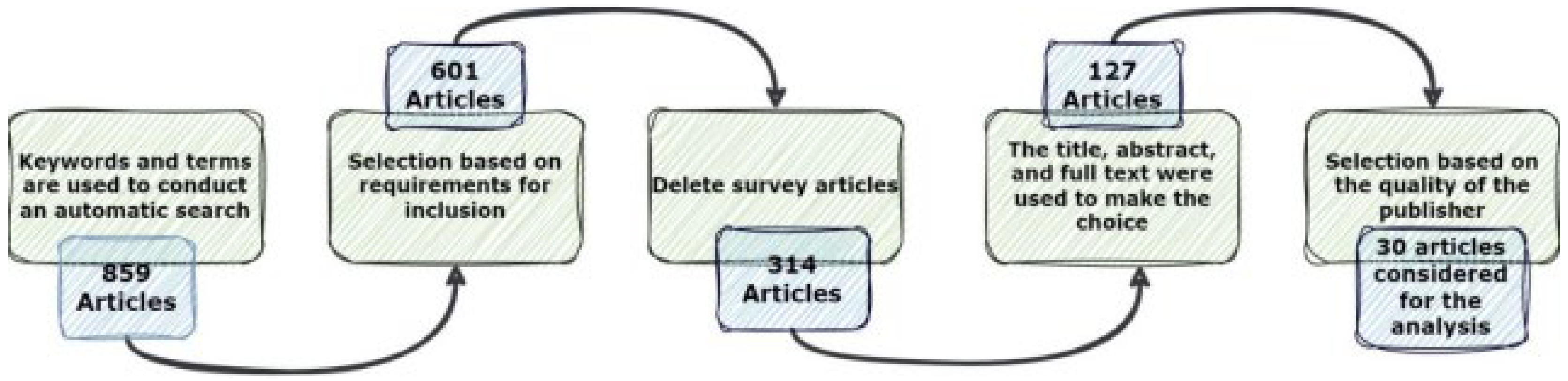
3.2. The Procedure of Paper Exploration
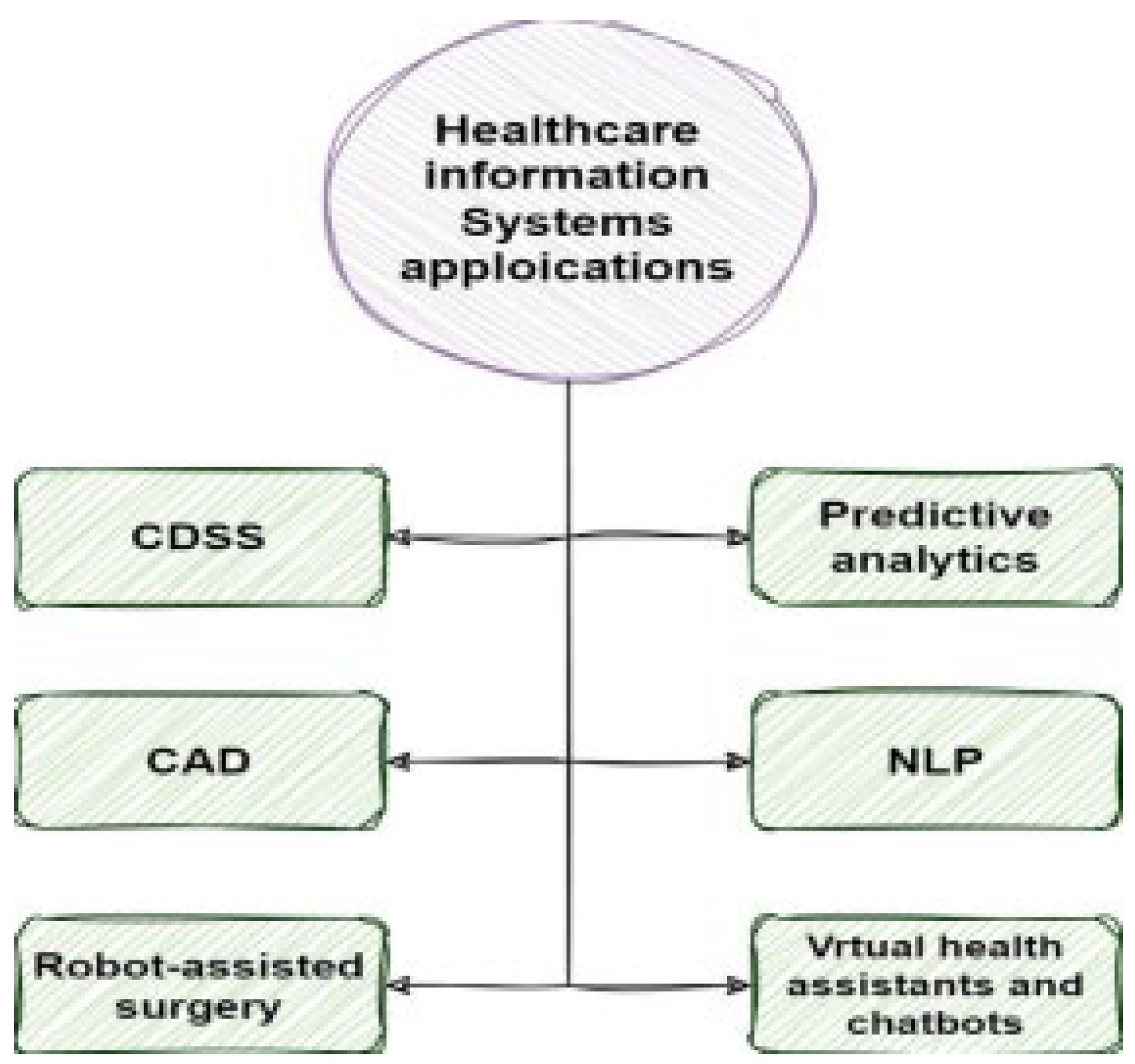
4. AI-Driven Decision-Making Techniques in HIS
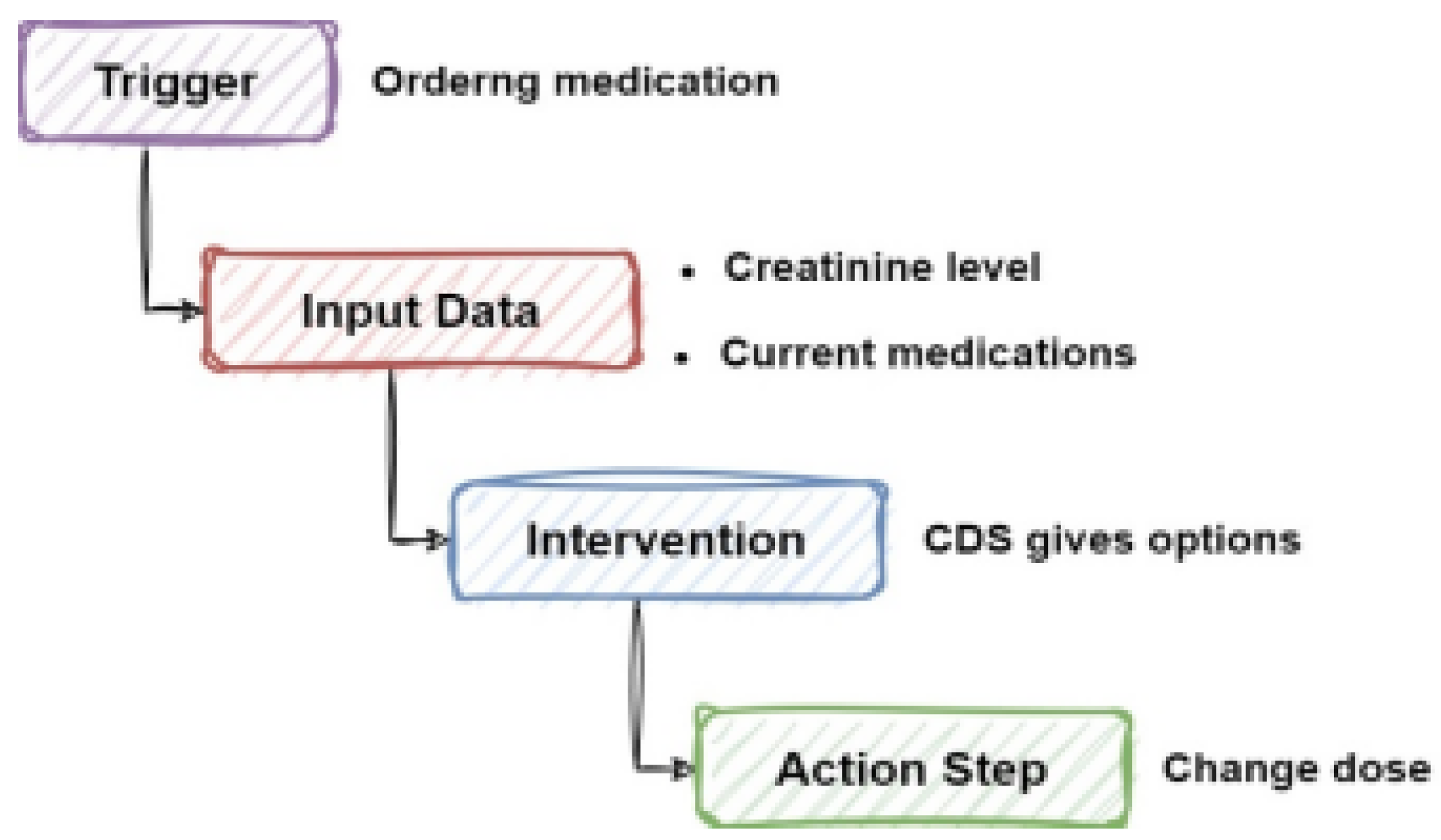
4.1. CDSS
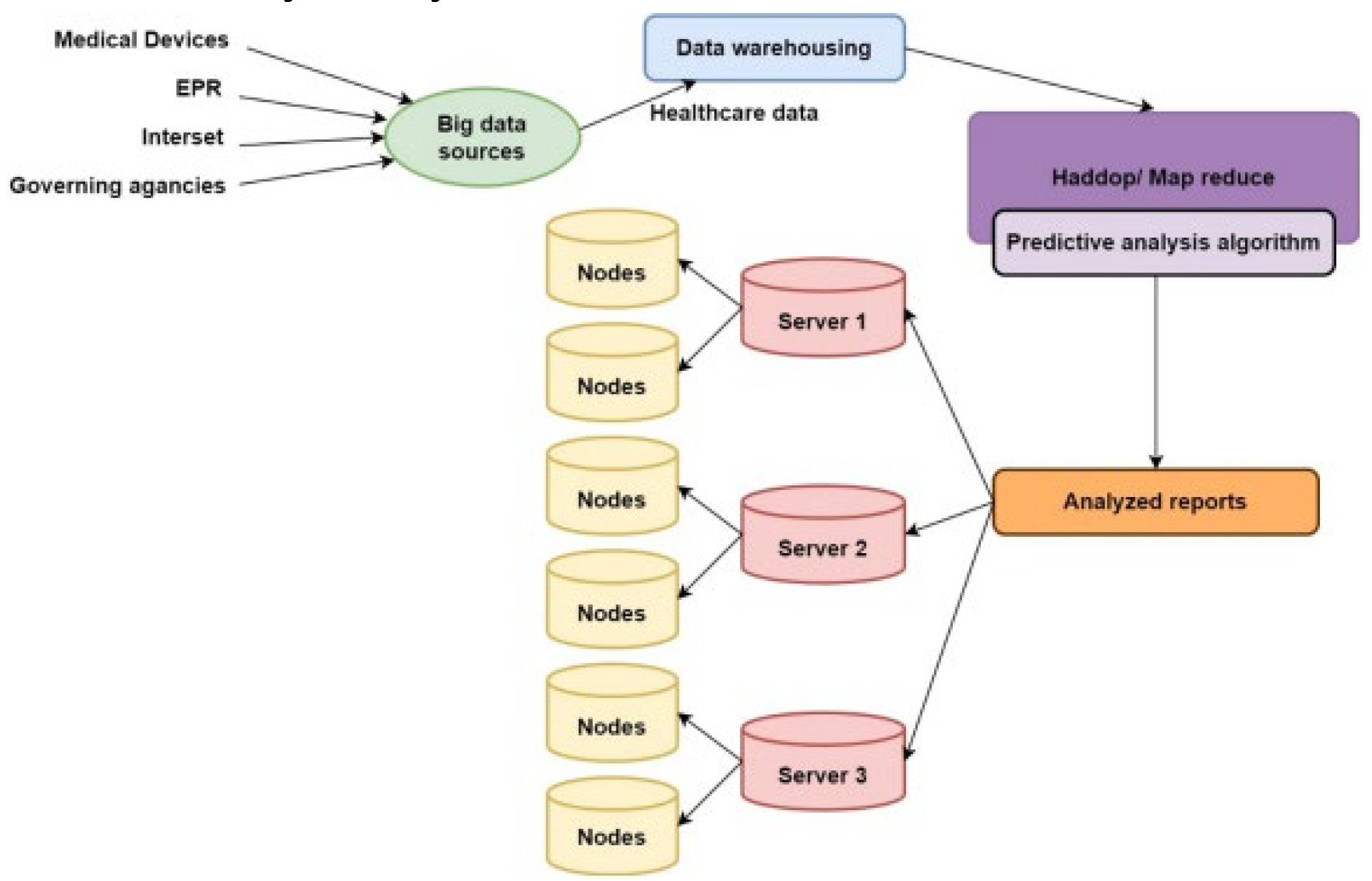
4.2. Predictive Analytics
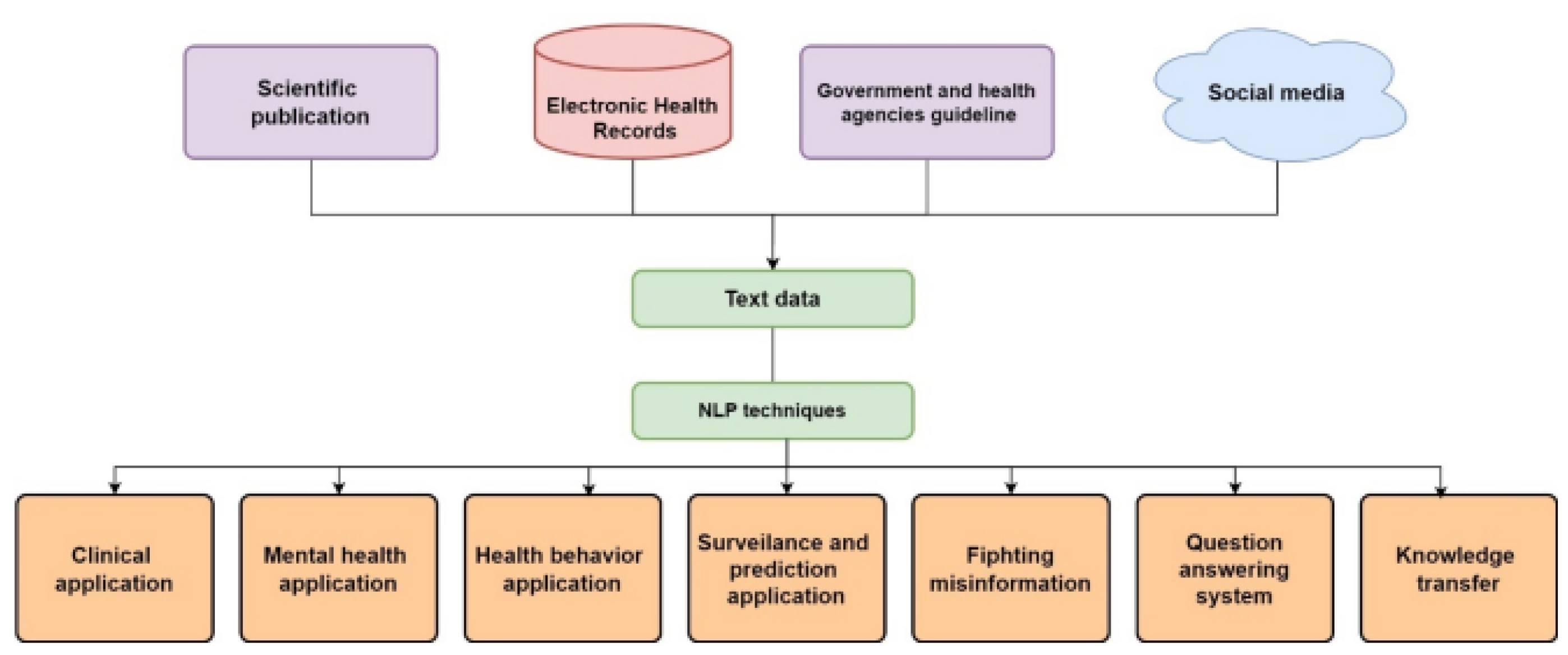
4.3. NLP
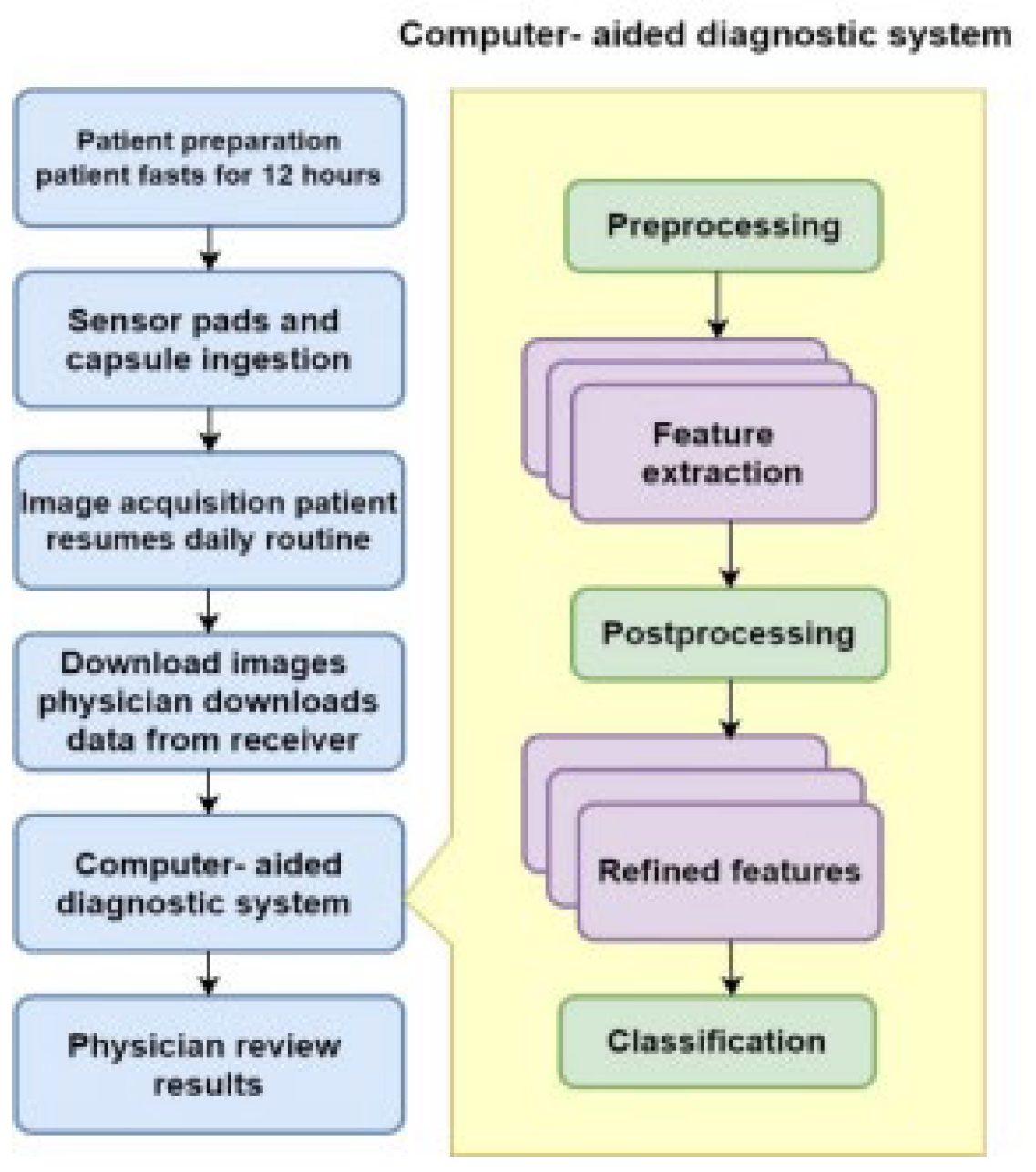
4.4. CAD
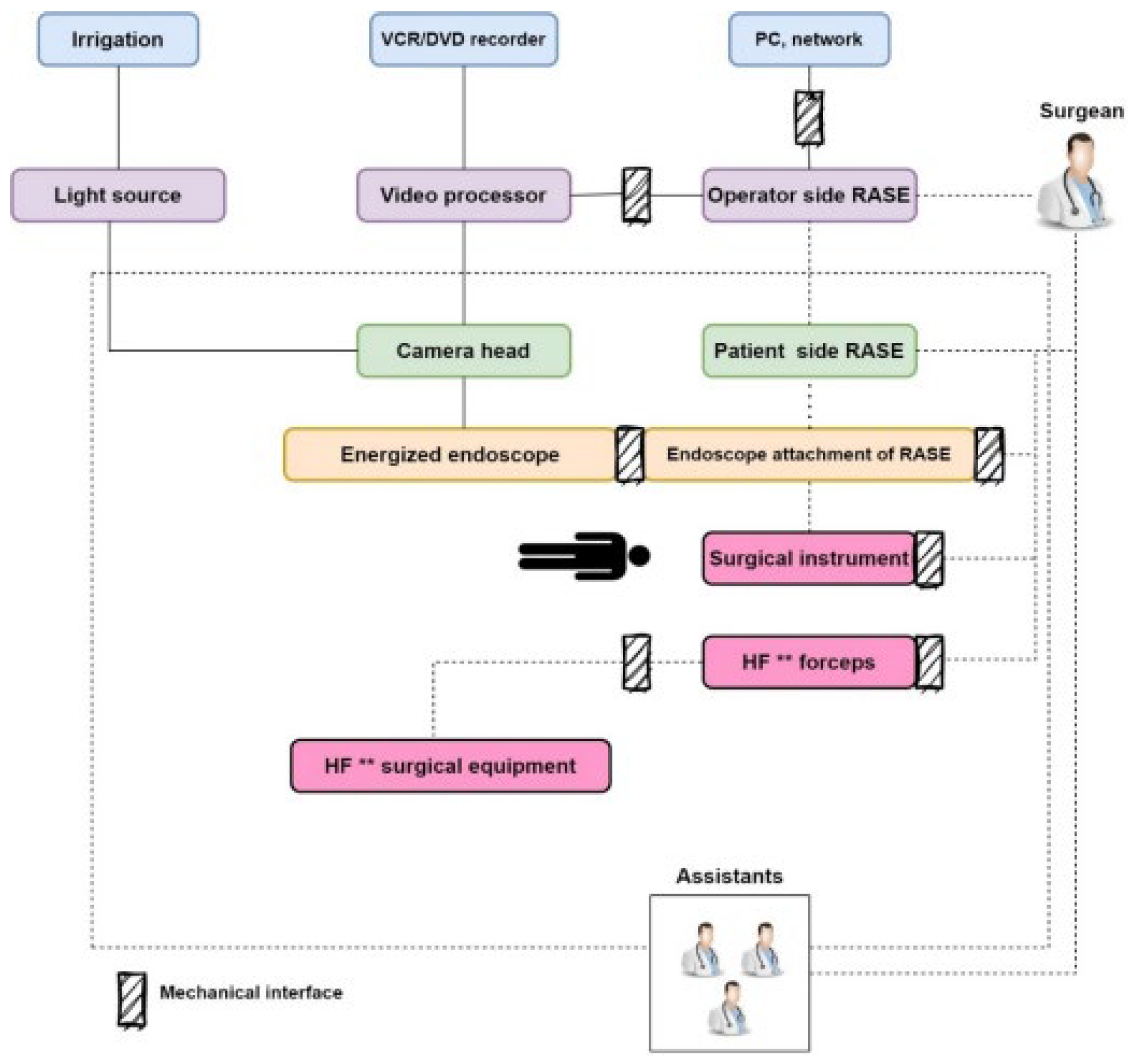
4.5. Robot-Assisted Surgery
4.6. VHAs and Chatbots
5. Results and Comparison
I. CDSS
II. Predictive Analytics
III. NLP
IV. CAD
V. Robot-Assisted Surgery
VI. VHAs and Chatbots
5.1. Prevalent Criteria
5.2. Challenges of the AI Applications in Decision-Making in HIS
5.3. Datasets Commonly Used in ML Implementation for Decision-Making in HIS
- EHRs: Patient data produced in EHRs operate as the main dataset, involving data like medical records, diagnoses, treatments, prescriptions, and test outcomes [75].
- Medical Imaging Datasets: Radiological images, consisting X-rays, MRIs, and CT scans, are pivotal for ML-based diagnostic decision-making. These datasets enable developing the algorithms for image recognition, lesion detection, and disease categorization [76].
- Genomic and Molecular Datasets: Genomic data may generate significant data regarding general variations and disease risk. ML models apply genomic dat to increase the precision of medicine, adjust drugs, and predict sickness risks emloying genetic profiles [77].
- Clinical Trials and Research Databases: Datasets from clinical research and research give a wealth of data regarding treatment results, experimental drugs, and patient responses. ML models can apply this data to make evidence-based decisions and detect trends in efficiency of treatments [78].
- Patient Outcome Databases: Datasets tracking patient findings, readmission rates, and post-therapy follow-ups might predict outcome of treatment and aid in decision-making for optimal treatment for patients [79].
- Health Monitoring Devices: Wearable technology and health monitoring devices generate real-time data on the patient’s health activity levels, and physiological metrics, which could be analyzed by ML systems to allow continual health monitoring and early detection of abnormalities [80].
- NLP Datasets: Unstructured data, like clinical notes, research articles, and medical literature, is evaluated applying NLP methods to extract useful information for decision support. These datasets aid to understand contextual subtleties in medical data [81].
6. Open Issues
7. Conclusion and Limitation
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Ramírez, J.G.C., AI in Healthcare: Revolutionizing Patient Care with Predictive Analytics and Decision Support Systems. Journal of Artificial Intelligence General science (JAIGS) ISSN: 3006-4023, 2024. 1(1): p. 31-37. [CrossRef]
- Bertl, M., P. Ross, and D. Draheim, Systematic AI support for decision-making in the healthcare sector: Obstacles and success factors. Health Policy and Technology, 2023. 12(3): p. 100748. [CrossRef]
- Patil, S. and H. Shankar, Transforming healthcare: harnessing the power of AI in the modern era. International Journal of Multidisciplinary Sciences and Arts, 2023. 2(1): p. 60-70.
- Heilig, T. and I. Scheer, Decision Intelligence: Transform Your Team and Organization with AI-Driven Decision-Making. 2023: John Wiley & Sons.
- Kasula, B.Y. and P. Whig, AI-Driven Machine Learning Solutions for Sustainable Development in Healthcare—Pioneering Efficient, Equitable, and Innovative Health Service. International Journal of Sustainable Development Through AI, ML and IoT, 2023. 2(2): p. 1-7.
- Sylolypavan, A., et al., The impact of inconsistent human annotations on AI driven clinical decision making. NPJ Digital Medicine, 2023. 6(1): p. 26. [CrossRef]
- Harry, A., The future of medicine: harnessing the power of AI for revolutionizing healthcare. International Journal of Multidisciplinary Sciences and Arts, 2023. 2(1): p. 36-47. [CrossRef]
- Sarella, P.N.K. and V.T. Mangam, AI-Driven Natural Language Processing in Healthcare: Transforming Patient-Provider Communication. Indian Journal of Pharmacy Practice, 2024. 17(1). [CrossRef]
- Kazi, K., AI-Driven IoT (AIIoT) in Healthcare Monitoring, in Using Traditional Design Methods to Enhance AI-Driven Decision Making. 2024, IGI Global. p. 77-101.
- Wysocki, O., et al., Assessing the communication gap between AI models and healthcare professionals: Explainability, utility and trust in AI-driven clinical decision-making. Artificial Intelligence, 2023. 316: p. 103839. [CrossRef]
- Vyas, B., Java-Powered AI: Implementing Intelligent Systems with Code. Journal of Science & Technology, 2023. 4(6): p. 1-12.
- Suha, S.A. and T.F. Sanam, Exploring dominant factors for ensuring the sustainability of utilizing artificial intelligence in healthcare decision making: An emerging country context. International Journal of Information Management Data Insights, 2023. 3(1): p. 100170.
- Saxena, P.D., et al., Impact of Artificial Intelligence on Healthcare Informatics: Opportunities and Challenges. Journal of Informatics Education and Research, 2023. 3(2). [CrossRef]
- Gudigantala, N., S. Madhavaram, and P. Bicen, An AI decision-making framework for business value maximization. AI Magazine, 2023. 44(1): p. 67-84. [CrossRef]
- Ray, P.P. and P. Majumder, The potential of ChatGPT to transform healthcare and address ethical challenges in artificial intelligence-driven medicine. Journal of Clinical Neurology (Seoul, Korea), 2023. 19(5): p. 509. [CrossRef]
- Božić, V., “Artificial Intelligence–powered” Expert Systems in Hospitals.
- Van Berkel, N., et al., Measurements, algorithms, and presentations of reality: Framing interactions with AI-enabled decision support. ACM Transactions on Computer-Human Interaction, 2023. 30(2): p. 1-33.
- Durga, K., Intelligent Support for Cardiovascular Diagnosis: The AI-CDSS Approach, in Using Traditional Design Methods to Enhance AI-Driven Decision Making. 2024, IGI Global. p. 64-76.
- Chen, C. and Y. Zheng, When consumers need more interpretability of artificial intelligence (AI) recommendations? The effect of decision-making domains. Behaviour & Information Technology, 2023: p. 1-9. [CrossRef]
- Jeyaraman, M., et al., Unraveling the ethical enigma: artificial intelligence in healthcare. Cureus, 2023. 15(8). [CrossRef]
- Kaul, R., et al., The role of AI for developing digital twins in healthcare: The case of cancer care. Wiley Interdisciplinary Reviews: Data Mining and Knowledge Discovery, 2023. 13(1): p. e1480.
- Dogheim, G.M. and A. Hussain, Patient care through AI-driven remote monitoring: Analyzing the role of predictive models and intelligent alerts in preventive medicine. Journal of Contemporary Healthcare Analytics, 2023. 7(1): p. 94-110.
- Babarinde, A.O., et al., Review of AI applications in Healthcare: Comparative insights from the USA and Africa. International Medical Science Research Journal, 2023. 3(3): p. 92-107. [CrossRef]
- Bao, Y., W. Gong, and K. Yang, A Literature Review of Human–AI Synergy in Decision Making: From the Perspective of Affordance Actualization Theory. Systems, 2023. 11(9): p. 442. [CrossRef]
- Mahdi, S.S., et al., How does artificial intelligence impact digital healthcare initiatives? A review of AI applications in dental healthcare. International Journal of Information Management Data Insights, 2023. 3(1): p. 100144. [CrossRef]
- Nawrat, Z., Introduction to AI-driven surgical robots. Artif Intell Surg, 2023. 3(2): p. 90-7. [CrossRef]
- Wang, L., et al., Human-centered design and evaluation of AI-empowered clinical decision support systems: a systematic review. Frontiers in Computer Science, 2023. 5: p. 1187299. [CrossRef]
- Moazemi, S., et al., Artificial intelligence for clinical decision support for monitoring patients in cardiovascular ICUs: A systematic review. Frontiers in Medicine, 2023. 10: p. 1109411. [CrossRef]
- Loftus, T.J., et al., Artificial intelligence-enabled decision support in nephrology. Nature Reviews Nephrology, 2022. 18(7): p. 452-465. [CrossRef]
- Xu, Q., et al., Interpretability of Clinical Decision Support Systems Based on Artificial Intelligence from Technological and Medical Perspective: A Systematic Review. Journal of Healthcare Engineering, 2023. 2023. [CrossRef]
- Lau, P.L., M. Nandy, and S. Chakraborty. Accelerating UN sustainable development goals with ai-driven technologies: A systematic literature review of women’s healthcare. in Healthcare. 2023. MDPI. [CrossRef]
- Marino, N., et al., Towards AI-driven longevity research: An overview. Frontiers in Aging, 2023. 4: p. 1057204. [CrossRef]
- Comito, C., D. Falcone, and A. Forestiero, AI-Driven Clinical Decision Support: Enhancing Disease Diagnosis Exploiting Patients Similarity. IEEE Access, 2022. 10: p. 6878-6888. [CrossRef]
- Vasey, B., et al., Reporting guideline for the early-stage clinical evaluation of decision support systems driven by artificial intelligence: DECIDE-AI. Nature medicine, 2022. 28(5): p. 924-933.
- Choudhury, A., Factors influencing clinicians’ willingness to use an AI-based clinical decision support system. Frontiers in Digital Health, 2022. 4: p. 920662. [CrossRef]
- Liu, X., et al., Discrepancy between perceptions and acceptance of clinical decision support Systems: implementation of artificial intelligence for vancomycin dosing. BMC Medical Informatics and Decision Making, 2023. 23(1): p. 157. [CrossRef]
- Amann, J., et al., Explainability for artificial intelligence in healthcare: a multidisciplinary perspective. BMC medical informatics and decision making, 2020. 20: p. 1-9. [CrossRef]
- Elvas, L.B., et al., AI-Driven Decision Support for Early Detection of Cardiac Events: Unveiling Patterns and Predicting Myocardial Ischemia. Journal of Personalized Medicine, 2023. 13(9): p. 1421. [CrossRef]
- Rehman, A., A. Farrakh, and U.F. Mushtaq, Improving Clinical Decision Support Systems: Explainable AI for Enhanced Disease Prediction in Healthcare. International Journal of Computational and Innovative Sciences, 2023. 2(2): p. 9-23.
- Chen, J., et al., Artificial intelligence-based human-centric decision support framework: an application to predictive maintenance in asset management under pandemic environments. Annals of Operations Research, 2021: p. 1-24. [CrossRef]
- Wang, J., et al., Managerial decision support system using an integrated model of AI and big data analytics. Annals of Operations Research, 2022: p. 1-18. [CrossRef]
- Hasan, I., et al., Data analytics and knowledge management approach for COVID-19 prediction and control. International Journal of Information Technology, 2023. 15(2): p. 937-954. [CrossRef]
- Afshar, M., et al., Deployment of Real-time Natural Language Processing and Deep Learning Clinical Decision Support in the Electronic Health Record: Pipeline Implementation for an Opioid Misuse Screener in Hospitalized Adults. JMIR Medical Informatics, 2023. 11: p. e44977. [CrossRef]
- Elkin, P.L., et al., Using artificial intelligence with natural language processing to combine electronic health record’s structured and free text data to identify nonvalvular atrial fibrillation to decrease strokes and death: Evaluation and case-control study. Journal of medical Internet research, 2021. 23(11): p. e28946. [CrossRef]
- Stewart, R., J. Chaturvedi, and A. Roberts, Natural language processing–relevance to patient outcomes and real-world evidence. 2023, Taylor & Francis. p. 1-5. [CrossRef]
- Joyce, C., et al., The evaluation of a clinical decision support tool using natural language processing to screen hospitalized adults for unhealthy substance use: protocol for a quasi-experimental design. JMIR Research Protocols, 2022. 11(12): p. e42971. [CrossRef]
- Barrera, N., et al., A recommender system for occupational hygiene services using natural language processing. Healthcare Analytics, 2023. 3: p. 100148. [CrossRef]
- Creswell, J., et al., Early user perspectives on using computer-aided detection software for interpreting chest X-ray images to enhance access and quality of care for persons with tuberculosis. BMC Global and Public Health, 2023. 1(1): p. 30. [CrossRef]
- Tran, W.T., et al., Computational radiology in breast cancer screening and diagnosis using artificial intelligence. Canadian Association of Radiologists Journal, 2021. 72(1): p. 98-108. [CrossRef]
- Ibrahim, A.U., A.G. Kibarer, and F. Al-Turjman, Computer-aided Detection of Tuberculosis from Microbiological and Radiographic Images. Data Intelligence, 2023: p. 1-26. [CrossRef]
- Shukla, P.K., et al., AI-DRIVEN novel approach for liver cancer screening and prediction using cascaded fully convolutional neural network. Journal of Healthcare Engineering, 2022. 2022. [CrossRef]
- Khanna, M., et al., Radiologist-level two novel and robust automated computer-aided prediction models for early detection of COVID-19 infection from chest X-ray images. Arabian Journal for Science and Engineering, 2023. 48(8): p. 11051-11083. [CrossRef]
- Zeineldin, R.A., et al., Development of an AI-driven system for neurosurgery with a usability study: a step towards minimal invasive robotics. at-Automatisierungstechnik, 2023. 71(7): p. 537-546. [CrossRef]
- Parry, M.W., et al., Patient Perspectives on Artificial Intelligence in Healthcare Decision Making: A Multi-Center Comparative Study. Indian Journal of Orthopaedics, 2023. 57(5): p. 653-665. [CrossRef]
- Kotha, S., et al., ARTEMIS: AI-driven Robotic Triage Labeling and Emergency Medical Information System. arXiv preprint arXiv:2309.08865, 2023.
- Kolbinger, F.R., et al., Artificial Intelligence for context-aware surgical guidance in complex robot-assisted oncological procedures: An exploratory feasibility study. European Journal of Surgical Oncology, 2023: p. 106996. [CrossRef]
- Ai, Y., et al., Control system design for a novel minimally invasive surgical robot. Computer Assisted Surgery, 2016. 21(sup1): p. 45-53. [CrossRef]
- Wang, H., et al., An artificial intelligence chatbot for young people’s sexual and reproductive health in india (snehai): Instrumental case study. Journal of Medical Internet Research, 2022. 24(1): p. e29969. [CrossRef]
- Fan, X., et al., Utilization of self-diagnosis health chatbots in real-world settings: case study. Journal of medical Internet research, 2021. 23(1): p. e19928. [CrossRef]
- Chakraborty, S., et al., An AI-Based Medical Chatbot Model for Infectious Disease Prediction. Ieee Access, 2022. 10: p. 128469-128483. [CrossRef]
- Esmaeilzadeh, P., T. Mirzaei, and S. Dharanikota, Patients’ perceptions toward human–artificial intelligence interaction in health care: experimental study. Journal of medical Internet research, 2021. 23(11): p. e25856.
- Chow, J.C., et al. Developing an AI-Assisted Educational Chatbot for Radiotherapy Using the IBM Watson Assistant Platform. in Healthcare. 2023. MDPI. [CrossRef]
- Shamszare, H. and A. Choudhury. Clinicians’ Perceptions of Artificial Intelligence: Focus on Workload, Risk, Trust, Clinical Decision Making, and Clinical Integration. in Healthcare. 2023. MDPI.
- Bayyapu, S., R.R. Turpu, and R.R. Vangala, ADVANCING HEALTHCARE DECISION-MAKING: THE FUSION OF MACHINE LEARNING, PREDICTIVE ANALYTICS, AND CLOUD TECHNOLOGY.
- Zhang, P. and M.N. Kamel Boulos, Generative AI in medicine and healthcare: Promises, opportunities and challenges. Future Internet, 2023. 15(9): p. 286. [CrossRef]
- Mardiani, E., L. Judijanto, and A.Y. Rukmana, Improving Trust and Accountability in AI Systems through Technological Era Advancement for Decision Support in Indonesian Manufacturing Companies. West Science Interdisciplinary Studies, 2023. 1(10): p. 1019-1027. [CrossRef]
- Bhavaraju, S.R., Artificial intelligence in healthcare: doctor as a stakeholder. 2023.
- Ayo-Farai, O., et al., Engineering innovations in healthcare: a review of developments in the USA. Engineering Science & Technology Journal, 2023. 4(6): p. 381-400. [CrossRef]
- Batra, P. and D.M. Dave, Revolutionizing Healthcare Platforms: The Impact of AI on Patient Engagement and Treatment Efficacy. International Journal of Science and Research (IJSR), 2024. 13(10.21275): p. 613-624.
- Yelne, S., et al., Harnessing the power of AI: a comprehensive review of its impact and challenges in nursing science and healthcare. Cureus, 2023. 15(11). [CrossRef]
- Pradhan, B., et al., An AI-Assisted Smart Healthcare System Using 5G Communication. IEEE Access, 2023. [CrossRef]
- Amin, A., et al. An explainable ai framework for artificial intelligence of medical things. in 2023 IEEE Globecom Workshops (GC Wkshps). 2023. IEEE.
- Goktas, P., A. Kucukkaya, and P. Karacay, Leveraging the efficiency and transparency of artificial intelligence-driven visual Chatbot through smart prompt learning concept. Skin Research and Technology, 2023. 29(11). [CrossRef]
- Husnain, A., et al., AI’S healing touch: examining machine learning’s transformative effects on healthcare. Journal of World Science, 2023. 2(10): p. 1681-1695. [CrossRef]
- Ogbuke, N., et al., Data-driven technologies for global healthcare practices and COVID-19: opportunities and challenges. Annals of Operations Research, 2023: p. 1-36. [CrossRef]
- Abbas, A., AI in Healthcare: Applications, Challenges, and Future Prospects.
- Singh, A., et al., Revolutionizing Breast Healthcare: Harnessing the Role of Artificial Intelligence. Cureus, 2023. 15(12). [CrossRef]
- Alam, M.N., M. Kaur, and M.S. Kabir, Explainable AI in Healthcare: Enhancing transparency and trust upon legal and ethical consideration. Int Res J Eng Technol, 2023. 10(6): p. 1-9.
- Mergen, M., et al., Immersive training of clinical decision making with AI driven virtual patients–a new VR platform called medical tr. AI. ning. GMS Journal for Medical Education, 2023. 40(2).
- Gupta, B.B., et al., Analysis of cutting-edge technologies for enterprise information system and management. Enterprise Information Systems, 2023. 17(11): p. 2197406. [CrossRef]
- Raut, R., et al. Intelligent Information System for Detection of COVID-19 Based on AI. in Proceedings of 3rd International Conference on Recent Trends in Machine Learning, IoT, Smart Cities and Applications: ICMISC 2022. 2023. Springer.
- Fawaz, A., A. Ferraresi, and C. Isidoro, Systems Biology in Cancer Diagnosis Integrating Omics Technologies and Artificial Intelligence to Support Physician Decision Making. Journal of Personalized Medicine, 2023. 13(11): p. 1590. [CrossRef]
- Khan, A., Harnessing the Power of AI: A Review of Advancements in Healthcare. BULLET: Jurnal Multidisiplin Ilmu, 2023. 2(3): p. 546-556.
- Ghanvatkar, S. and V. Rajan, Evaluating Explanations from AI Algorithms for Clinical Decision-Making: A Social Science-based Approach. medRxiv, 2024: p. 2024.02. 26.24303365. [CrossRef]
- Olabanji, S.O., et al., AI-Driven cloud security: Examining the impact of user behavior analysis on threat detection. Asian Journal of Research in Computer Science, 2024. 17(3): p. 57-74. [CrossRef]
- Mykhalko, Y., et al., FROM TEXT TO DIAGNOSE: CHATGPT’S EFFICACY IN MEDICAL DECISION-MAKING. INDEXED IN PUBMED/MEDLINE, SCOPUS, EMBASE, EBSCO, INDEX COPERNICUS, POLISH MINISTRY OF EDUCATION AND SCIENCE, POLISH MEDICAL BIBLIOGRAPHY, 2023. 76(11): p. 2345-2350. [CrossRef]
- Chintala, S., AI-Driven Personalised Treatment Plans: The Future of Precision Medicine. Machine Intelligence Research, 2023. 17(02): p. 9718-9728.
- Cipriano, L.E., Evaluating the impact and potential impact of machine learning on medical decision making. 2023, SAGE Publications Sage CA: Los Angeles, CA. p. 147-149. [CrossRef]
- Sarker, M., Assessing the Integration of AI Technologies in Enhancing Patient Care Delivery in US Hospitals. Journal of Knowledge Learning and Science Technology ISSN: 2959-6386 (online), 2023. 2(2): p. 338-351. [CrossRef]
- Martins, A., et al., PharmiTech: Addressing Polypharmacy Challenges Through AI-Driven Solutions. Available at SSRN 4668688.
- Wahab, N.A.B.A. and R.B.M. Nor, Challenges and Strategies in Data Management and Governance for AI-Based Healthcare Models: Balancing Innovation and Ethical Responsibilities. AI, IoT and the Fourth Industrial Revolution Review, 2023. 13(12): p. 24-32.
- Parsa, A.D., et al., Artificial Intelligence for Global Healthcare, in Artificial Intelligence in Medical Virology. 2023, Springer. p. 1-21.
- Andolina, S. and J.A. Konstan, Introduction to the special issue on AI, decision-making, and the impact on humans. 2023, Taylor & Francis. p. 1367-1370. [CrossRef]
- Sharma, R., AI Fusion: Unleashing Synergies in M&A, IT Supply Chain, and IoT-Driven Medical Device Sales with SAP Integration. 2024, EasyChair.





| Authors | Main Idea | Advantages | Disadvantages |
|---|---|---|---|
| Wang, Zhang [27] |
|
|
|
| Moazemi, Vahdati [28] |
|
|
|
| Loftus, Shickel [29] |
|
|
|
| Xu, Xie [30] |
|
|
|
| Lau, Nandy [31] |
|
|
|
| Marino, Putignano [32] |
|
|
|
| Ours |
|
|
|
| S# | Keywords and search criteria | S# | Keywords and search criteria |
|---|---|---|---|
| S1 | “AI” and “Information Systems” | S6 | “Healthcare” and “Information Systems” |
| S2 | “Decision-making” and “AI” | S7 | “Clinical Decision Support Systems” and “AI-driven Decision-making” |
| S3 | “Predictive Analytics” and “AI” | S8 | “NLP” and “AI” |
| S4 | “Computer-aided diagnostics” and “AI” | S9 | “Robot-assisted Surgery” and “AI” |
| S10 | “Virtual Health Assistants and Chatbots” and “AI” | S11 | “AI-driven Decision-making” and “Healthcare Information Systems” |
| Author | Main Idea | Advantage | Disadvantage | Simulation Environment | Dataset |
|---|---|---|---|---|---|
| Comito, Falcone [33] |
|
|
|
Cyhon | 38,597 samples |
| Vasey, Nagendran [34] |
|
|
|
Python | 43,986 samples |
| Choudhury [35] |
|
|
|
- | 273 samples |
| Liu, Barreto [36] |
|
|
|
Python | 215 samples |
| Amann, Blasimme [37] |
|
|
|
Python | 400 samples |
| Author | Main Idea | Advantage | Disadvantage | Simulation Environment | Dataset |
|---|---|---|---|---|---|
| Elvas, Nunes [38] |
|
|
|
Python | 512,724 samples |
| Rehman, Farrakh [39] |
|
|
|
Python | PIMA |
| Chen, Lim [40] |
|
|
|
- | 15 samples |
| Wang, Zhao [41] |
|
|
|
- | 130 samples |
| Hasan, Dhawan [42] |
|
|
|
Python | 14,000 samples |
| Author | Main Idea | Advantage | Disadvantage | Simulation Environment | Dataset |
|---|---|---|---|---|---|
| Afshar, Adelaine [43] |
|
|
|
Tensorflow | 12,500 samples |
| Elkin, Mullin [44] |
|
|
|
Keras | 2722 samples |
| Stewart, Chaturvedi [45] |
|
|
|
MATLAB | 60 samples |
| Joyce, Markossian [46] |
|
|
|
MATLAB | 2400 samples |
| Barrera, Torres [47] |
|
|
|
Python | 200,000 samples |
| Author | Main Idea | Advantage | Disadvantage | Simulation Environment | Dataset |
|---|---|---|---|---|---|
| Creswell, Vo [48] |
|
|
|
Python | 281,550 samples |
| Tran, Sadeghi-Naini [49] |
|
|
|
Python | 25,856 samples |
| Ibrahim, Kibarer [50] |
|
|
|
MATLAB | 600 samples |
| Shukla, Zakariah [51] |
|
|
|
Tensoorflow | 2012 samples |
| Khanna, Agarwal [52] |
|
|
|
Python | 16 samples |
| Author | Main Idea | Advantage | Disadvantage | Simulation Environment | Dataset |
|---|---|---|---|---|---|
| Zeineldin, Junger [53] |
|
|
|
Keras | 1251 samples |
| Parry, Markowitz [54] |
|
|
|
MATLAB | 1684 samples |
| Kotha, Viswanath [55] |
|
|
|
Raspberry Pi | 425,087 samples |
| Kolbinger, Bodenstedt [56] |
|
|
|
Pytorch | 3000 samples |
| Ai, Pan [57] |
|
|
|
- | 100 samples |
| Author | Main Idea | Advantage | Disadvantage | Simulation Environment | Dataset |
|---|---|---|---|---|---|
| Wang, Gupta [58] |
|
|
|
Python | 135,263 samples |
| Fan, Chao [59] |
|
|
|
- | 16,519 samples |
| Chakraborty, Paul [60] |
|
|
|
Python | 20 samples |
| Esmaeilzadeh, Mirzaei [61] |
|
|
|
Tensorflow | 105 samples |
| Chow, Wong [62] |
|
|
|
MATLAB | 20 samples |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




