Submitted:
05 June 2024
Posted:
06 June 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
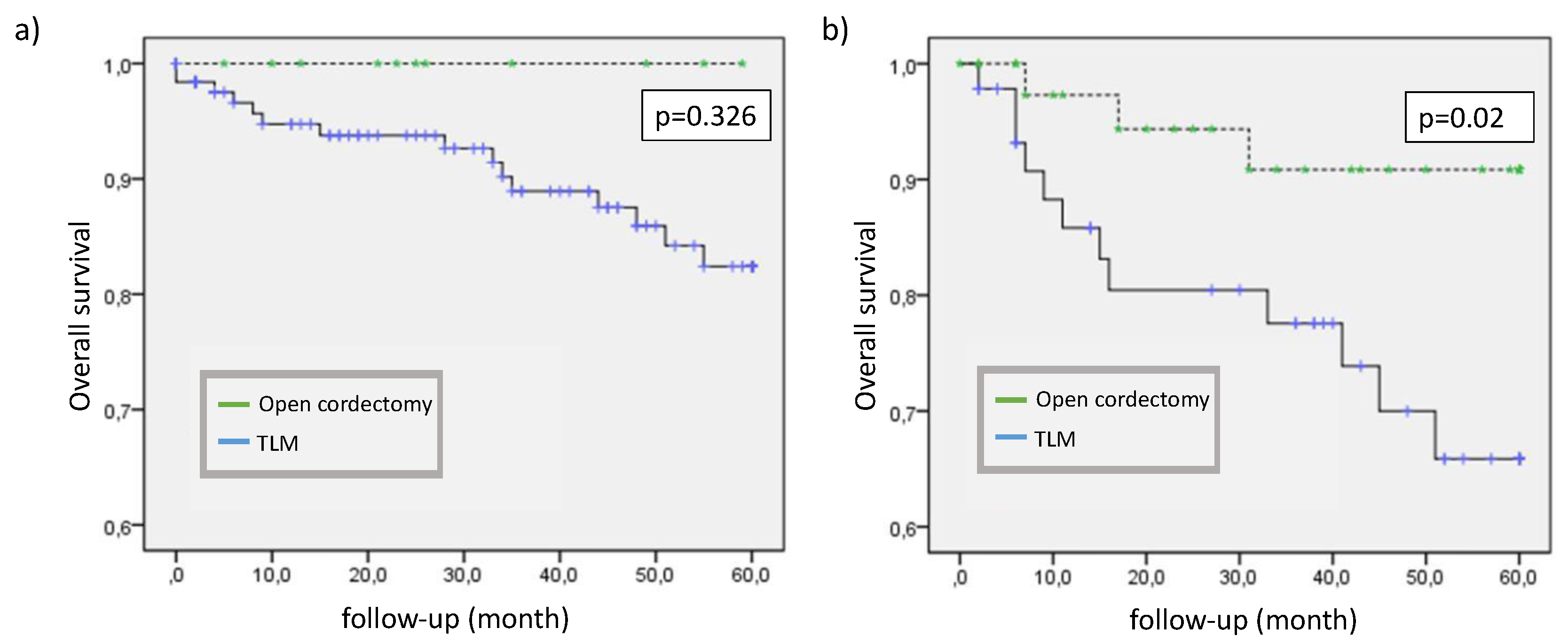
3.1. Oncological Outcome
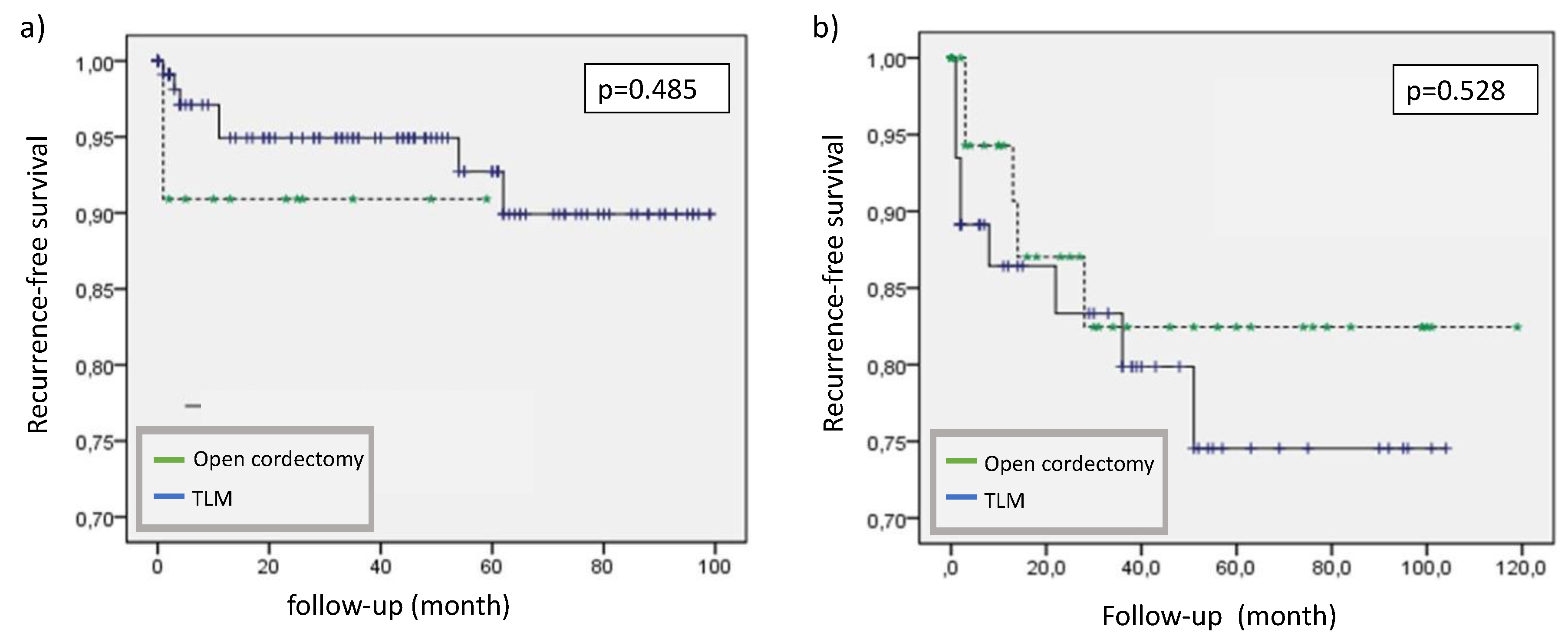
3.2. Functional Outcome
3.3. Perioperative Course and Complications
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Warner L, Chudasama J, Kelly CG, et al. Radiotherapy versus open surgery versus endolaryngeal surgery (with or without laser) for early laryngeal squamous cell cancer. Cochrane Database Syst Rev. 2014, 2014, CD002027. Published 2014 Dec 12.
- Arboleda LPA, Neves AB, Kohler HF, Vartanian JG, Candelária LM, Borges MF, Fernandes GA, de Carvalho GB, Kowalski LP, Brennan P, Santos Silva AR, Curado MP. Overview of glottic laryngeal cancer treatment recommendation changes in the NCCN guidelines from 2011 to 2022. Cancer Rep (Hoboken). 2023, 6, e1837, Epub 2023 Jun 7. [CrossRef] [PubMed] [PubMed Central]
- Thomas L, Drinnan M, Natesh B, Mehanna H, Jones T, Paleri V. Open conservation partial laryngectomy for laryngeal cancer: a systematic review of English language literature. Cancer Treat Rev. 2012 May;38, 203-11 Epub 2011 Jul 20. [CrossRef] [PubMed]
- Luna-Ortiz K, Campos-Ramos E, Villavicencio-Valencia V, Contreras-Buendía M, Pasche P, Gómez AH. Vertical partial hemilaryngectomy with reconstruction by false cord imbrication. ANZ J Surg. 2010, 80, 358–363. [Google Scholar] [CrossRef] [PubMed]
- de Campora E, Radici M, de Campora L. External versus endoscopic approach in the surgical treatment of glottic cancer. Eur Arch Otorhinolaryngol. 2001, 258, 533–536. [Google Scholar] [CrossRef] [PubMed]
- Glatt, F. Onkologisches und funktionelles Outcome nach Therapie des frühen Stimmlippenkarzinoms. Inauguraldissertation des Fachbereichs Medizin der Justus Liebig Universität Giessen. Giessen, 2018.
- Arens, C.; Schwemmle, C.; Voigt-Zimmermann, S. [Surgical reconstruction in laryngeal carcinoma]. HNO 2020, 68, 666–677. [Google Scholar] [CrossRef] [PubMed]
- Elicin, O.; Giger, R. Comparison of Current Surgical and Non-Surgical Treatment Strategies for Early and Locally Advanced Stage Glottic Laryngeal Cancer and Their Outcome. Cancers (Basel) 2020, 12. [Google Scholar] [CrossRef] [PubMed]
- Higgins, K.M.; Shah, M.D.; Ogaick, M.J.; Enepekides, D. Treatment of early-stage glottic cancer: meta-analysis comparison of laser excision versus radiotherapy. J Otolaryngol Head Neck Surg 2009, 38, 603–612. [Google Scholar] [PubMed]
- Kujath, M.; Kerr, P.; Myers, C.; Bammeke, F.; Lambert, P.; Cooke, A.; Sutherland, D. Functional outcomes and laryngectomy-free survival after transoral CO(2) laser microsurgery for stage 1 and 2 glottic carcinoma. J Otolaryngol Head Neck Surg 2011, 40 Suppl 1, S49–58. [Google Scholar]
- Vaculik, M.F.; MacKay, C.A.; Taylor, S.M.; Trites, J.R.B.; Hart, R.D.; Rigby, M.H. Systematic review and meta-analysis of T1 glottic cancer outcomes comparing CO2 transoral laser microsurgery and radiotherapy. J Otolaryngol Head Neck Surg 2019, 48, 44. [Google Scholar] [CrossRef] [PubMed]
- Campo F, Zocchi J, Ralli M, De Seta D, Russo FY, Angeletti D, Minni A, Greco A, Pellini R, de Vincentiis M. Laser Microsurgery Versus Radiotherapy Versus Open Partial Laryngectomy for T2 Laryngeal Carcinoma: A Systematic Review of Oncological Outcomes. Ear Nose Throat J. 2021 Feb;100(1_suppl):51S-58S. [CrossRef] [PubMed]
- Peretti, G.; Piazza, C.; Mora, F.; Garofolo, S.; Guastini, L. Reasonable limits for transoral laser microsurgery in laryngeal cancer. Curr Opin Otolaryngol Head Neck Surg 2016, 24, 135–139. [Google Scholar] [CrossRef]
- Jacobi C, Freundorfer R, Reiter M. Transoral laser microsurgery in early glottic cancer involving the anterior commissure. Eur Arch Otorhinolaryngol. 2019 Mar;276, 837-845. Epub 2019 Jan 2. [CrossRef] [PubMed]
- Milovanovic, J.; Jotic, A.; Djukic, V.; Pavlovic, B.; Trivic, A.; Krejovic-Trivic, S.; Milovanovic, A.; Milovanovic, A.; Artiko, V.; Banko, B. Oncological and functional outcome after surgical treatment of early glottic carcinoma without anterior commissure involvement. Biomed Res Int 2014, 2014, 464781. [Google Scholar] [CrossRef]
- Pantel, M.; Wittekindt, C.; Altendorf-Hofmann, A.; Boeger, D.; Buentzel, J.; Esser, D.; Mueller, A.; Wendt, T.G.; Guntinas-Lichius, O.; Thuringia, H.; et al. Diversity of treatment of T2N0 glottic cancer of the larynx: lessons to learn from epidemiological cancer registry data. Acta Otolaryngol 2011, 131, 1205–1213. [Google Scholar] [CrossRef] [PubMed]
- Sachse, F.; Stoll, W.; Rudack, C. Evaluation of treatment results with regard to initial anterior commissure involvement in early glottic carcinoma treated by external partial surgery or transoral laser microresection. Head Neck 2009, 31, 531–537. [Google Scholar] [CrossRef] [PubMed]
- Mendelsohn AH, Kiagiadaki D, Lawson G, Remacle M. CO2 laser cordectomy for glottic squamous cell carcinoma involving the anterior commissure: voice and oncologic outcomes. Eur Arch Otorhinolaryngol. 2015 Feb;272, 413-8. Epub 2014 Oct 29. [CrossRef] [PubMed]
- Hendriksma M, Montagne MW, Langeveld TPM, Veselic M, van Benthem PPG, Sjögren EV. Evaluation of surgical margin status in patients with early glottic cancer (Tis-T2) treated with transoral CO2 laser microsurgery, on local control. Eur Arch Otorhinolaryngol. 2018 Sep;275, 2333-2340. Epub 2018 Jul 19. [CrossRef] [PubMed]
- Fiz I, Koelmel JC, Sittel C. Nature and role of surgical margins in transoral laser microsurgery for early and intermediate glottic cancer. Curr Opin Otolaryngol Head Neck Surg. 2018 Apr;26, 78-83. [CrossRef] [PubMed]
- Peretti, G.; Nicolai, P.; Redaelli De Zinis, L.O.; Berlucchi, M.; Bazzana, T.; Bertoni, F.; Antonelli, A.R. Endoscopic CO2 laser excision for tis, T1, and T2 glottic carcinomas: cure rate and prognostic factors. Otolaryngol Head Neck Surg 2000, 123, 124–131. [Google Scholar] [CrossRef] [PubMed]
- Zapater, E.; Hernandez, R.; Reboll, R.; Perez, A.; Alba, J.R.; Basterra, J. Pathological examination of cordectomy specimens: analysis of negative resection. Auris Nasus Larynx 2009, 36, 321–325. [Google Scholar] [CrossRef] [PubMed]
- Aluffi Valletti, P.; Taranto, F.; Chiesa, A.; Pia, F.; Valente, G. Impact of resection margin status on oncological outcomes after CO2 laser cordectomy. Acta Otorhinolaryngol Ital 2018, 38, 24–30. [Google Scholar] [CrossRef] [PubMed]
- Hartl, D.M.; Ferlito, A.; Brasnu, D.F.; Langendijk, J.A.; Rinaldo, A.; Silver, C.E.; Wolf, G.T. Evidence-based review of treatment options for patients with glottic cancer. Head Neck 2011, 33, 1638–1648. [Google Scholar] [CrossRef]
- Chone, C.T.; Yonehara, E.; Martins, J.E.; Altemani, A.; Crespo, A.N. Importance of anterior commissure in recurrence of early glottic cancer after laser endoscopic resection. Arch Otolaryngol Head Neck Surg 2007, 133, 882–887. [Google Scholar] [CrossRef]
- Tulli, M.; Re, M.; Bondi, S.; Ferrante, L.; Dajko, M.; Giordano, L.; Gioacchini, F.M.; Galli, A.; Bussi, M. The prognostic value of anterior commissure involvement in T1 glottic cancer: A systematic review and meta-analysis. Laryngoscope 2020, 130, 1932–1940. [Google Scholar] [CrossRef]
- Carreras A, Martínez-Torre MI, Zabaleta M, Sanchez-Del-Rey A, Santaolalla F, Diaz-de-Cerio P. Prognosis and Outcomes in Early Stage Glottic Carcinoma Involving the Anterior Commissure Treated with Laser CO2 Surgery: A Retrospective Observational Analysis. Indian J Otolaryngol Head Neck Surg. 2022 Dec;74(Suppl 3):6048-6053. Epub 2021 Jun 27. [CrossRef] [PubMed]
- Lechien JR, Crevier-Buchman L, Circiu MP, Lisan Q, Hans S. Evolution of Voice Quality in Type 1-2 Transoral CO2 Laser Cordectomy: A Prospective Comparative Study. Laryngoscope. 2022 Jul;132, 1421-1426. Epub 2021 Oct 27. [CrossRef] [PubMed]
- Colizza A, Ralli M, D’Elia C, Greco A, de Vincentiis M. Voice quality after transoral CO2 laser microsurgery (TOLMS): systematic review of literature. Eur Arch Otorhinolaryngol. 2022 Sep;279, 4247-4255. Epub 2022 May 3. [CrossRef] [PubMed]
- Greulich, M.T.; Parker, N.P.; Lee, P.; Merati, A.L.; Misono, S. Voice outcomes following radiation versus laser microsurgery for T1 glottic carcinoma: systematic review and meta-analysis. Otolaryngol Head Neck Surg 2015, 152, 811–819. [Google Scholar] [CrossRef]
- Ma Y, Green R, Pan S, McCabe D, Goldberg L, Woo P. Long-term Voice Outcome Following Radiation Versus Laser Microsurgery in Early Glottic Cancer. J Voice. 2019 Mar;33, 176-182. Epub 2017 Dec 8. [CrossRef] [PubMed]
- Bindewald, J.; Herrmann, E.; Dietz, A.; Wulke, C.; Meister, E.; Wollbruck, D.; Singer, S. [Quality of life and voice intelligibility in laryngeal cancer patients--relevance of the “satisfaction paradox”]. Laryngorhinootologie 2007, 86, 426–430. [Google Scholar] [CrossRef]
- Friedrich, G.; Dejonckere, P.H. [The voice evaluation protocol of the European Laryngological Society (ELS) -- first results of a multicenter study]. Laryngorhinootologie 2005, 84, 744–752. [Google Scholar] [CrossRef] [PubMed]
- Schindler, A.; Cuccarini, V.; Bottero, A.; Dobrea, C.; Capaccio, P.; Ottaviani, F. Long-term vocal functional results after glottectomy: a multi-dimensional analysis. Eur Arch Otorhinolaryngol 2007, 264, 1039–1044. [Google Scholar] [CrossRef] [PubMed]
- Bohlender, JE. Patient-Reported Outcome Measures zur Erfassung der gesundheitsbezogenen Lebensqualität bei Patienten mit Stimm- und Schluckstörungen [Patient-reported outcome measures for assessing health-related quality of life in patients with voice and swallowing disorders]. HNO. 2023 Sep;71, 549-555. German. Epub 2023 Aug 7. [CrossRef] [PubMed]
- Narasimhan SV, Rashmi R. Multiparameter Voice Assessment in Dysphonics: Correlation Between Objective and Perceptual Parameters. J Voice. 2022 May;36, 335-343. Epub 2020 Jul 7. [CrossRef] [PubMed]
- Böckler, R.; Bonkowsky, V.; Seidler, T.; Hacki, T. [Comparative voice quality evaluation after laser surgical versus fronto-lateral partial laryngectomy in T1b and T2 vocal cord carcinoma]. Laryngorhinootologie 1999, 78, 512–515. [Google Scholar] [CrossRef] [PubMed]
- Sittel, C.; Eckel, H.E.; Eschenburg, C.; Vossing, M.; Pototschnig, C.; Zorowka, P. [Voice quality after partial laser laryngectomy]. Laryngorhinootologie 1998, 77, 219–225. [Google Scholar] [CrossRef] [PubMed]
- Lechien JR, Crevier-Buchman L, Circiu MP, De Mones E, de Pemille GV, Julien-Laferriere A, Saussez S, Baudouin R, Remacle M, Hans S. Voice Quality Outcomes After Transoral CO2 Laser Cordectomy: A Longitudinal Prospective Study. Otolaryngol Head Neck Surg. 2023 Mar;168, 422-428. Epub 2023 Jan 29. [CrossRef] [PubMed]
| n | TLM (n=168) | TCC (n=51) | p | ||
|---|---|---|---|---|---|
| Age | mean ± SD | 67.3 ± 10.0 | 61.9 ± 11.2 | 0.003** | |
| Gender | Male (%) | 200 | 151 (75.5) | 49 (24.5) | 0.257* |
| Female (%) | 19 | 17 (89.5) | 2 (10.5) | ||
| Stage | T1a (%) | 134 | 123 (91.8) | 11 (8.2) | <0.01* |
| T1b/T2 (%) | 85 | 45 (53.0) | 40 (47.0) |
| Endoscopic surgery | Open surgery | ||||
|---|---|---|---|---|---|
| (min-max) | median | (min-max) | median | p-value* | |
| Perzeption Analysis (RBH) | |||||
| R | 0-3 | 1 | 0-3 | 1 | 0.474 |
| B | 0-3 | 1 | 0-3 | 1 | 0.774 |
| H | 0-3 | 2 | 0-3 | 2 | 0.163 |
| Total | 0-8 | 4 | 0-7 | 5 | 0.179 |
| Aerodynamics | |||||
| Max. Phonation Time [s] | 3-37 | 11.5 | 3-29 | 10 | 0.575 |
| Vital Capacity [ml] | 1400-5500 | 2800 | 1300-4800 | 2900 | 0.635 |
| Phonation Quotient [ml/s] | 73-1066.7 | 250 | 121.43-640.0 | 272.5 | 0.895 |
| Acoustic Measurements: | |||||
| Dynamic [dB] | 3-47 | 23 | 9-33 | 20 | 0.161 |
| Semitone range [semitones] | 8-49 | 23 | 10-40 | 19 | 0.215 |
| Jitter [%] | 0.4-36.4 | 4.41 | 0.33-26.3 | 8.24 | 0.202 |
| Shimmer [%] | 5.48-64.72 | 20.98 | 2.22-50.44 | 27.84 | 0.358 |
| Base frequency [Hz] | 115.1-334.4 | 158 | 103.1-362.1 | 165.6 | 0.739 |
| GNE (glottal to noise excitation ratio) | 0.125-0.701 | 0.333 | 0.16-0.659 | 0.285 | 0.153 |
| Periodic Correlation | 0.522-0.994 | 0.924 | 0.565-0.998 | 0.836 | 0.063 |
| Self-evaluation | |||||
| Visual analogue scale (VAS) | 1-5 | 4 | 1-5 | 3 | 0.014 |
| Type of complication | Endoscopic surgery | Open surgery | p-value 1 |
|---|---|---|---|
Bleeding
|
7 (3.6%) | 0 | 0.21 |
| 4 | 0 | ||
| 3 | 0 | ||
| Wound infection | 0 | 0 | |
| Pneumonia | 0 | 2 (3.9%) | 0.05 1 |
| Emphysema | 0 | 5 (9.8%) | < 0.011 |
| Dysphagia | 0 | 1 (2.0%) | 0.23 1 |
| Other | 4* (2.4%) | 4** (7.8%) | 0.09 1 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




