Submitted:
04 June 2024
Posted:
05 June 2024
You are already at the latest version
Abstract
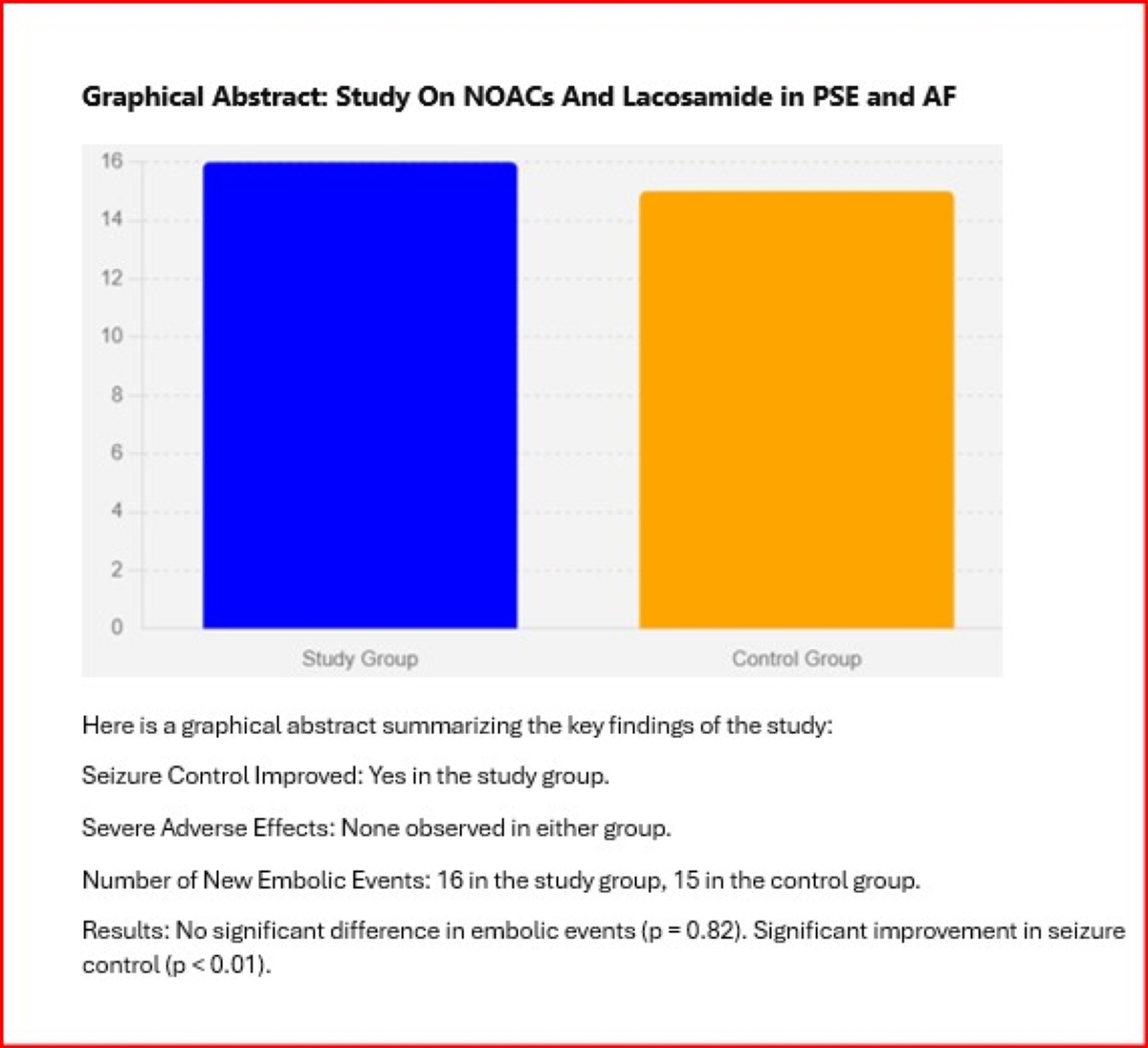
Keywords:
Introduction
Post-Stroke Seizures (PSS)
- Early Seizures: Occurring within the first week after a stroke, these are typically provoked by the acute effects of the stroke, such as brain injury, hemorrhage, or metabolic disturbances.
- Late Seizures: These occur after the first week post-stroke and are considered more likely to indicate the development of epilepsy.
Post-Stroke Epilepsy (PSE)
- Stroke Severity: Larger and more severe strokes have a higher risk of resulting in PSE.
- Stroke Type: Hemorrhagic strokes carry a greater risk compared to ischemic strokes.
- Location: Cortical involvement significantly increases the risk of developing PSE.
- Early Seizures: The presence of early post-stroke seizures is a strong predictor of subsequent epilepsy. (Table 1)
Clinical Implications and Management
Diagnosis
Treatment
Aim of the Study
Study Design and Population
Objectives
- 3.
- Efficacy of Seizure Control: The effectiveness of lacosamide in managing and controlling seizures in patients with PSE.
- 4.
- Safety Profile: The safety of the combination therapy, particularly focusing on the recurrence rate of minor or major embolic events over a 24-month follow-up period. This included monitoring for ischemic strokes, hemorrhagic strokes, and other embolic complications.
Methodology
Patient Monitoring and Follow-Up
Data Collection and Analysis
Results
Discussion
Conclusions
References
- Feyissa, A.M.; Hasan, T.F.; Meschia, J.F. Stroke-related epilepsy. Eur. J. Neurol. 2018, 26, 18. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, T.; Ihara, M. Post-stroke epilepsy. Neurochem. Int. 2017, 107, 219–228. [Google Scholar] [CrossRef]
- Zelano, J.; Holtkamp, M.; Agarwal, N.; Lattanzi, S.; Trinka, E.; Brigo, F. How to diagnose and treat post-stroke seizures and epilepsy. Epileptic Disord. 2020, 22, 252–263. [Google Scholar] [CrossRef] [PubMed]
- Tröscher, A.R.; Gruber, J.; Wagner, J.N.; Böhm, V.; Wahl, A.-S.; von Oertzen, T.J. Inflammation Mediated Epileptogenesis as Possible Mechanism Underlying Ischemic Post-stroke Epilepsy. Front. Aging Neurosci. 2021, 13, 781174. [Google Scholar] [CrossRef] [PubMed]
- Altman, K.; Shavit-Stein, E.; Maggio, N. Post Stroke Seizures and Epilepsy: From Proteases to Maladaptive Plasticity. Front. Cell. Neurosci. 2019, 13, 397. [Google Scholar] [CrossRef] [PubMed]
- Freiman, S.; Hauser, W.A.; Rider, F.; Gulyaeva, N.; Guekht, A. Post-stroke epilepsy: From clinical predictors to possible mechanisms. Epilepsy Res. 2024, 199, 107282. [Google Scholar] [CrossRef]
- Mafla-Mendoza, A.P.; Paredes-Urbano, E.D.; Gea-Izquierdo, E. Risk Factors Associated with Epilepsy Related to Cerebrovascular Disease: A Systematic Review and Meta-Analysis. Neuropsychiatr. Dis. Treat. 2023, ume 19, 2841–2856. [Google Scholar] [CrossRef]
- Lee, D.A.; Jang, T.; Kang, J.; Park, S.; Park, K.M. Functional Connectivity Alterations in Patients with Post-stroke Epilepsy Based on Source-level EEG and Graph Theory. Brain Topogr. 2024, 1–10. [Google Scholar] [CrossRef]
- Šmigelskytė, A.; Rimkuvienė, G.; Žukaitė, D.; Repečkaitė, G.; Jurkevičienė, G. The Association of Epileptic Seizures after Acute Ischemic Stroke with Cerebral Cortical Involvement and Electroencephalographic Changes. Medicina 2024, 60, 768. [Google Scholar] [CrossRef]
- Wen, L.-M.; Li, R.; Wang, Y.-L.; Kong, Q.-X.; Xia, M. Electroencephalogram findings in 10 patients with post-stroke epilepsy: A retrospective study. World J. Clin. Cases 2024, 12, 249–255. [Google Scholar] [CrossRef]
- Trinka, E. , & Höfler, J. (2019). Antiepileptic drug treatment in post-stroke seizures: An update. Journal of Neurology, Neurosurgery & Psychiatry, 90(2), 142-149. [CrossRef]
- Kaoud, M.A.; Nissan, R.; Segev, A.; Sabbag, A.; Orion, D.; Maor, E. Levetiracetam Interaction with Direct Oral Anticoagulants: A Pharmacovigilance Study. CNS Drugs 2023, 37, 1111–1121. [Google Scholar] [CrossRef] [PubMed]
- Mavri, A.; Ilc, S. The efficacy of direct oral anticoagulants in patients on concomitant treatment with levetiracetam. Sci. Rep. 2023, 13, 9257. [Google Scholar] [CrossRef] [PubMed]
- Goldstein, R.; Rabkin, N.; Buchman, N.; Jacobs, A.R.; Sandouka, K.; Raccah, B.; Negev, T.F.; Matok, I.; Bialer, M.; Muszkat, M. The Effect of Levetiracetam Compared with Enzyme-Inducing Antiseizure Medications on Apixaban and Rivaroxaban Peak Plasma Concentrations. CNS Drugs 2024, 38, 399–408. [Google Scholar] [CrossRef] [PubMed]
- Veroniki, A. A., Straus, S. E., & Rücker, G. (2018). Comparative safety and effectiveness of anti-seizure medications for post-stroke seizures: A systematic review and network meta-analysis. PLoS ONE, 13(7), e0200702. [CrossRef] [PubMed]
- Holtkamp, M.; Beghi, E.; Benninger, F.; Kälviäinen, R.; Rocamora, R.; Christensen, H.; European Stroke Organisat. European Stroke Organisation guidelines for the management of post-stroke seizures and epilepsy. Eur. Stroke J. 2017, 2, 103–115. [Google Scholar] [CrossRef] [PubMed]
- Rosenow, F.; Brandt, C.; Bozorg, A.; Dimova, S.; Steiniger-Brach, B.; Zhang, Y.; Ferrò, B.; Holmes, G.L.; Kälviäinen, R. Lacosamide in patients with epilepsy of cerebrovascular etiology. Acta Neurol. Scand. 2020, 141, 473–482. [Google Scholar] [CrossRef] [PubMed]
- Tomson, T., Battino, D., & Perucca, E. (2020). The management of epilepsy in the elderly: A critical review. Epileptic Disorders, 22(5), 441-461. [CrossRef] [PubMed]
- Hirsch, L. J., & LaRoche, S. M. (2021). Optimizing antiseizure medication therapy: Evidence-based recommendations and clinical guidance. Neurology Clinical Practice, 11(1), 49-61. [CrossRef] [PubMed]
- Chen, Y.; Li, W.; Lu, C.; Gao, X.; Song, H.; Zhang, Y.; Zhao, S.; Cai, G.; Guo, Q.; Zhou, D.; et al. Efficacy, tolerability and safety of add-on third-generation antiseizure medications in treating focal seizures worldwide: a network meta-analysis of randomised, placebo-controlled trials. EClinicalMedicine 2024, 70, 102513. [Google Scholar] [CrossRef]
- Rosenow, F.; Brandt, C.; Bozorg, A.; Dimova, S.; Steiniger-Brach, B.; Zhang, Y.; Ferrò, B.; Holmes, G.L.; Kälviäinen, R. Lacosamide in patients with epilepsy of cerebrovascular etiology. Acta Neurol. Scand. 2020, 141, 473–482. [Google Scholar] [CrossRef]
- Hlauschek, G.; Nicolo, J.; Sinclair, B.; Law, M.; Yasuda, C.L.; Cendes, F.; Lossius, M.I.; Kwan, P.; Vivash, L. Role of the glymphatic system and perivascular spaces as a potential biomarker for post-stroke epilepsy. Epilepsia Open 2023, 9, 60–76. [Google Scholar] [CrossRef] [PubMed]
- Abraira, L.; López-Maza, S.; Quintana, M.; Fonseca, E.; Toledo, M.; Campos-Fernández, D.; Lallana, S.; Grau-López, L.; Ciurans, J.; Jiménez, M.; et al. Exploratory study of blood biomarkers in patients with post-stroke epilepsy. Eur. Stroke J. 2024. [Google Scholar] [CrossRef] [PubMed]
- Abraira, L.; Santamarina, E.; Cazorla, S.; Bustamante, A.; Quintana, M.; Toledo, M.; Fonseca, E.; Grau-López, L.; Jiménez, M.; Ciurans, J.; et al. Blood biomarkers predictive of epilepsy after an acute stroke event. Epilepsia 2020, 61, 2244–2253. [Google Scholar] [CrossRef]
- Stöllberger, C.; Finsterer, J.; Schneider, B. Interactions between antiepileptic drugs and direct oral anticoagulants for primary and secondary stroke prevention. Expert Opin. Drug Metab. Toxicol. 2024, 359–376. [Google Scholar] [CrossRef] [PubMed]
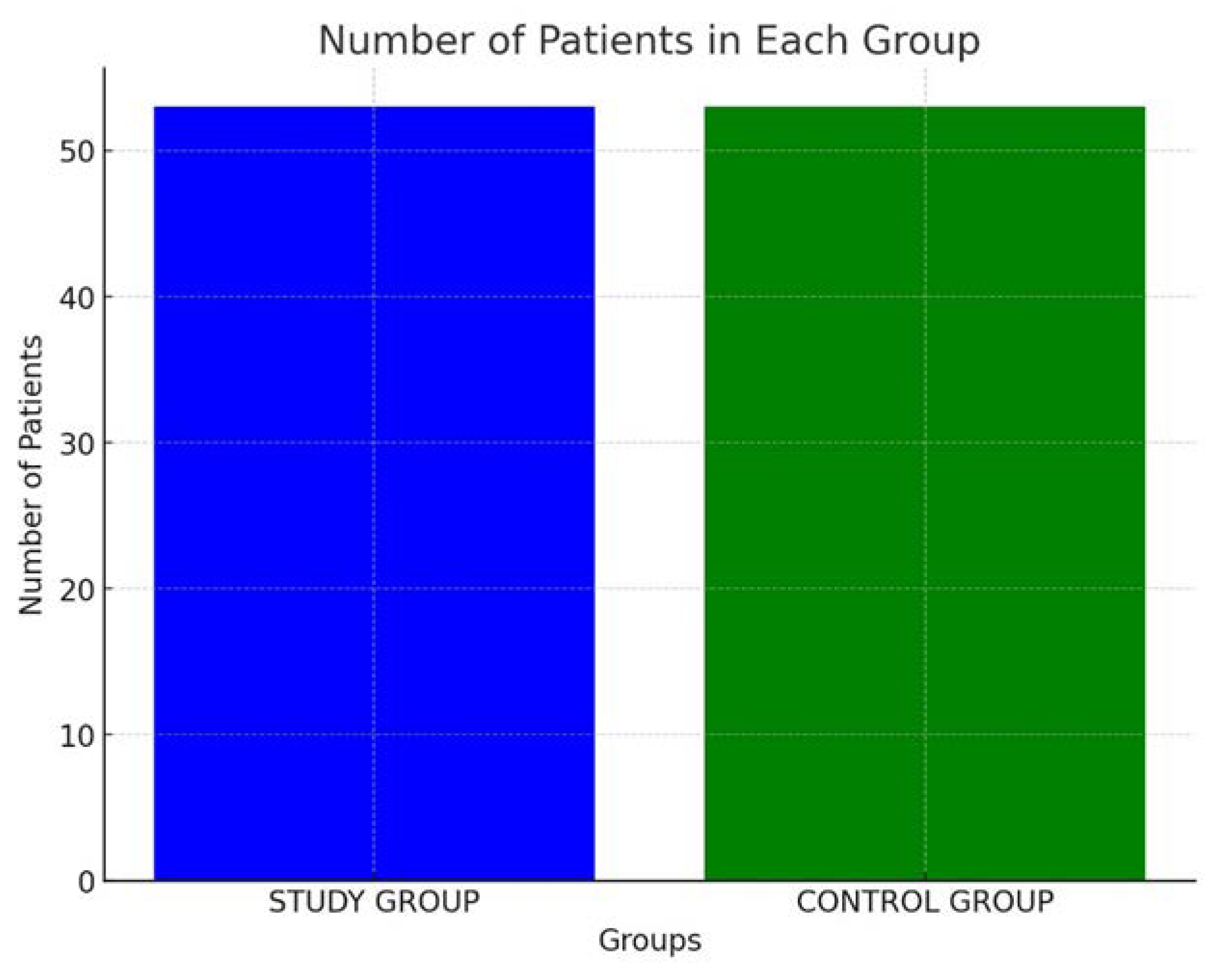
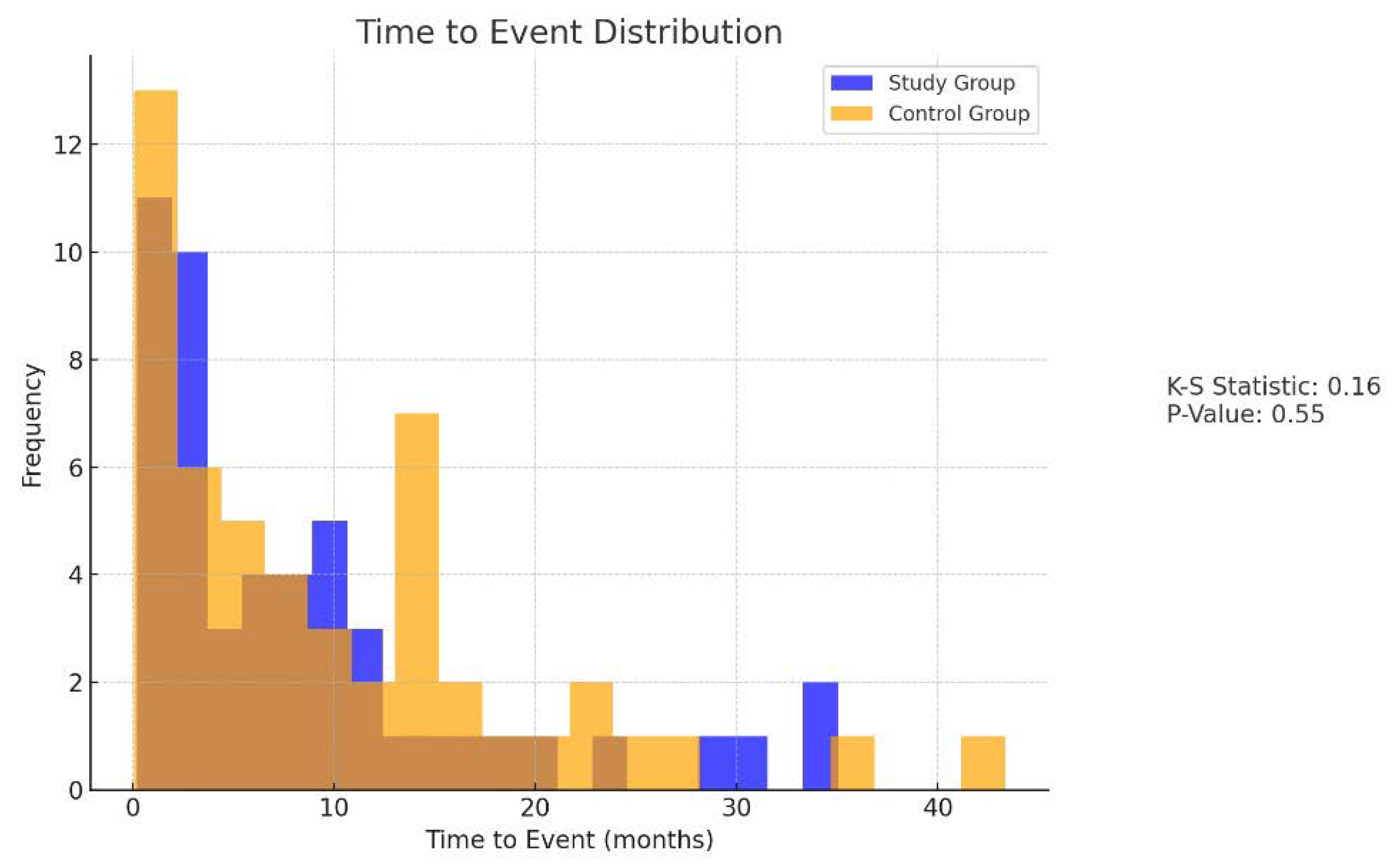
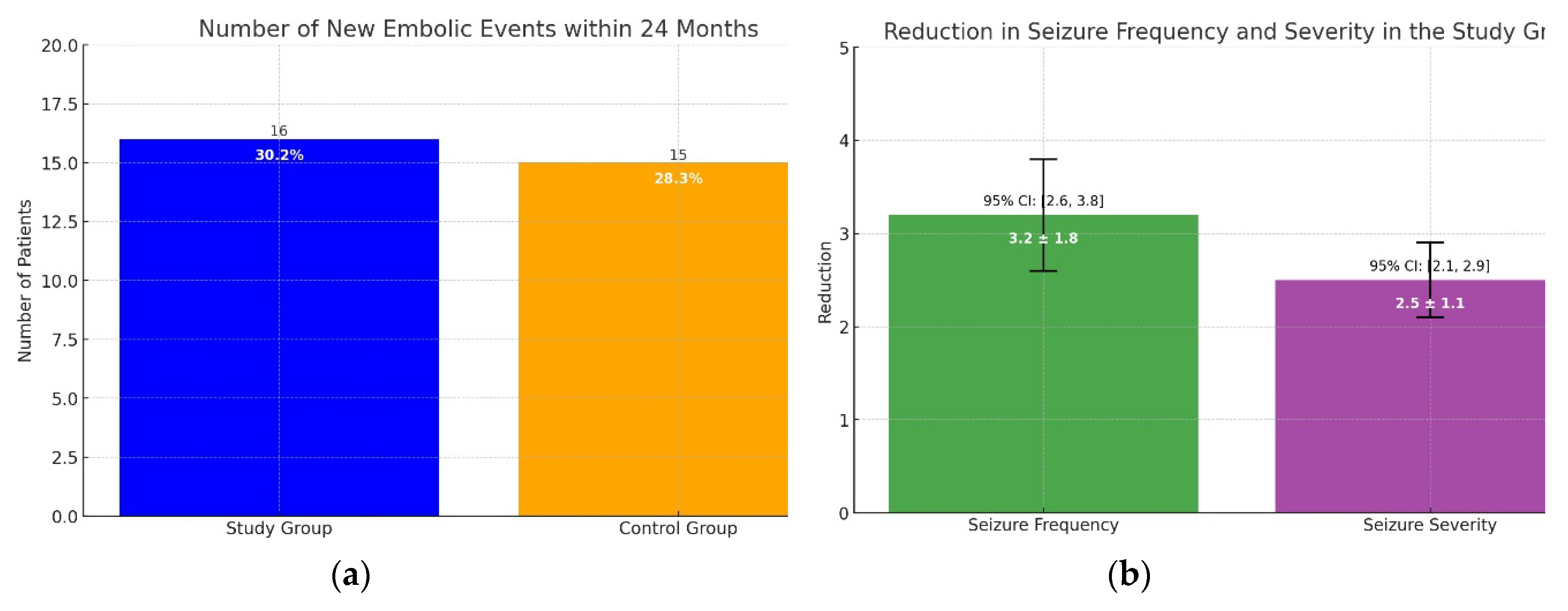
| Risk Factor | Description |
|---|---|
| Stroke Severity | Larger and more severe strokes increase the likelihood of PSE. |
| Stroke Type | Hemorrhagic strokes have a higher risk of leading to PSE compared to ischemic strokes. |
| Cortical Involvement | Strokes affecting the cerebral cortex are more likely to result in PSE. |
| Early Post-Stroke Seizures | The occurrence of seizures within the first week post-stroke is a strong predictor of later epilepsy. |
| Age | Younger patients are at a higher risk of developing PSE compared to older patients. |
| Stroke Location | Strokes in the temporal and frontal lobes are more associated with PSE. |
| Previous History of Seizures | Patients with a history of seizures before the stroke are more likely to develop PSE. |
| Stroke Recurrence | Multiple strokes increase the risk of developing PSE. |
| Genetic Factors | Family history of epilepsy may increase susceptibility to PSE. |
| Comorbid Conditions | Conditions like hypertension, diabetes, and heart disease can elevate the risk of PSE. |
| Stroke-Induced Neuroinflammation | Inflammatory responses post-stroke can contribute to the development of epilepsy. |
| Subarachnoid Hemorrhage | This specific type of hemorrhagic stroke has a high association with PSE. |
| Intraventricular Hemorrhage | Presence of blood in the brain's ventricular system can be a risk factor for PSE. |
| Infectious Complications | Post-stroke infections, especially central nervous system infections, can increase PSE risk. |
| Blood-Brain Barrier Disruption | Stroke-induced damage to the blood-brain barrier can lead to epileptogenic changes. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




