Submitted:
01 June 2024
Posted:
03 June 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Snapshot of Physician Workforce across the OECD
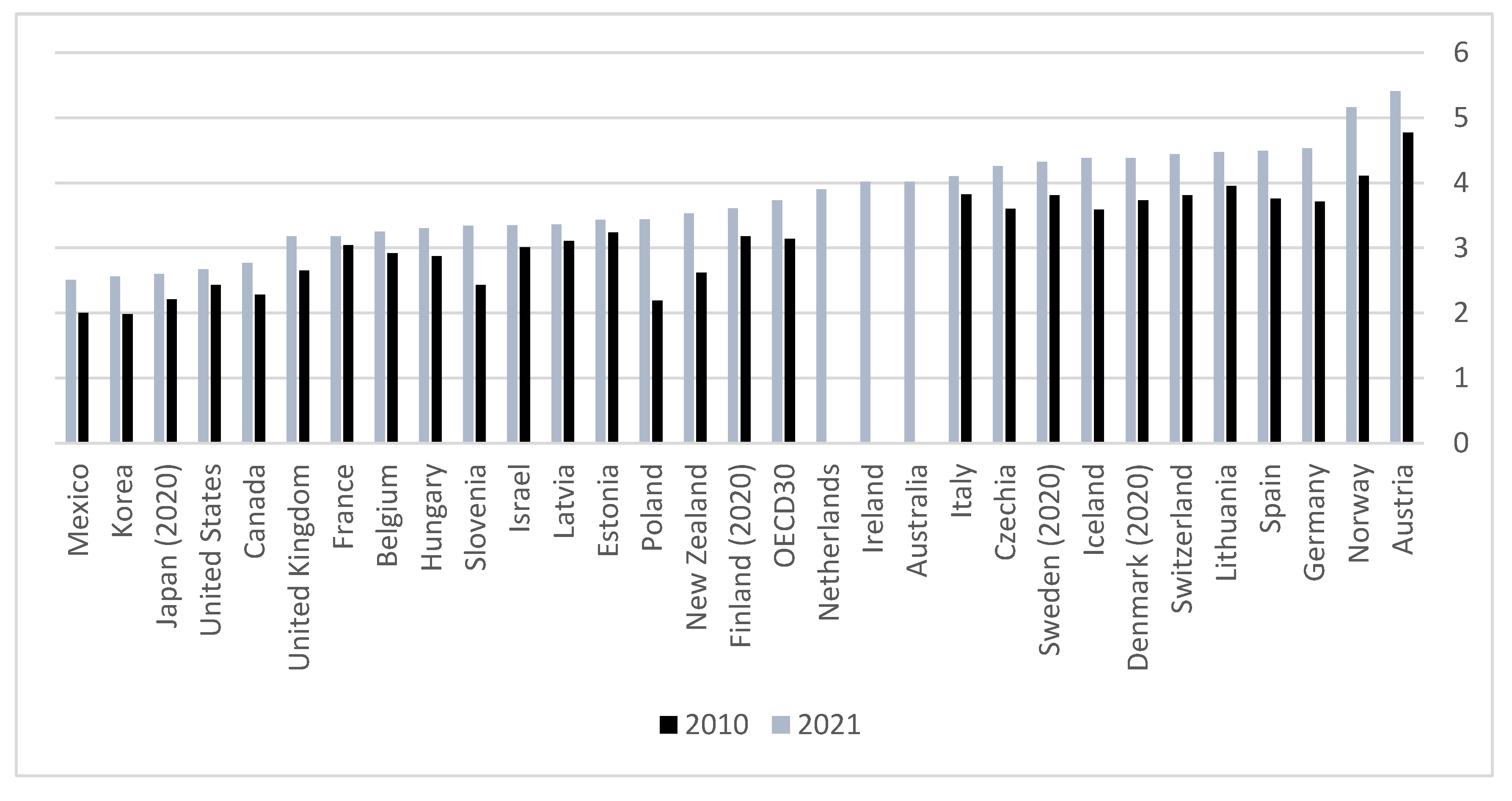
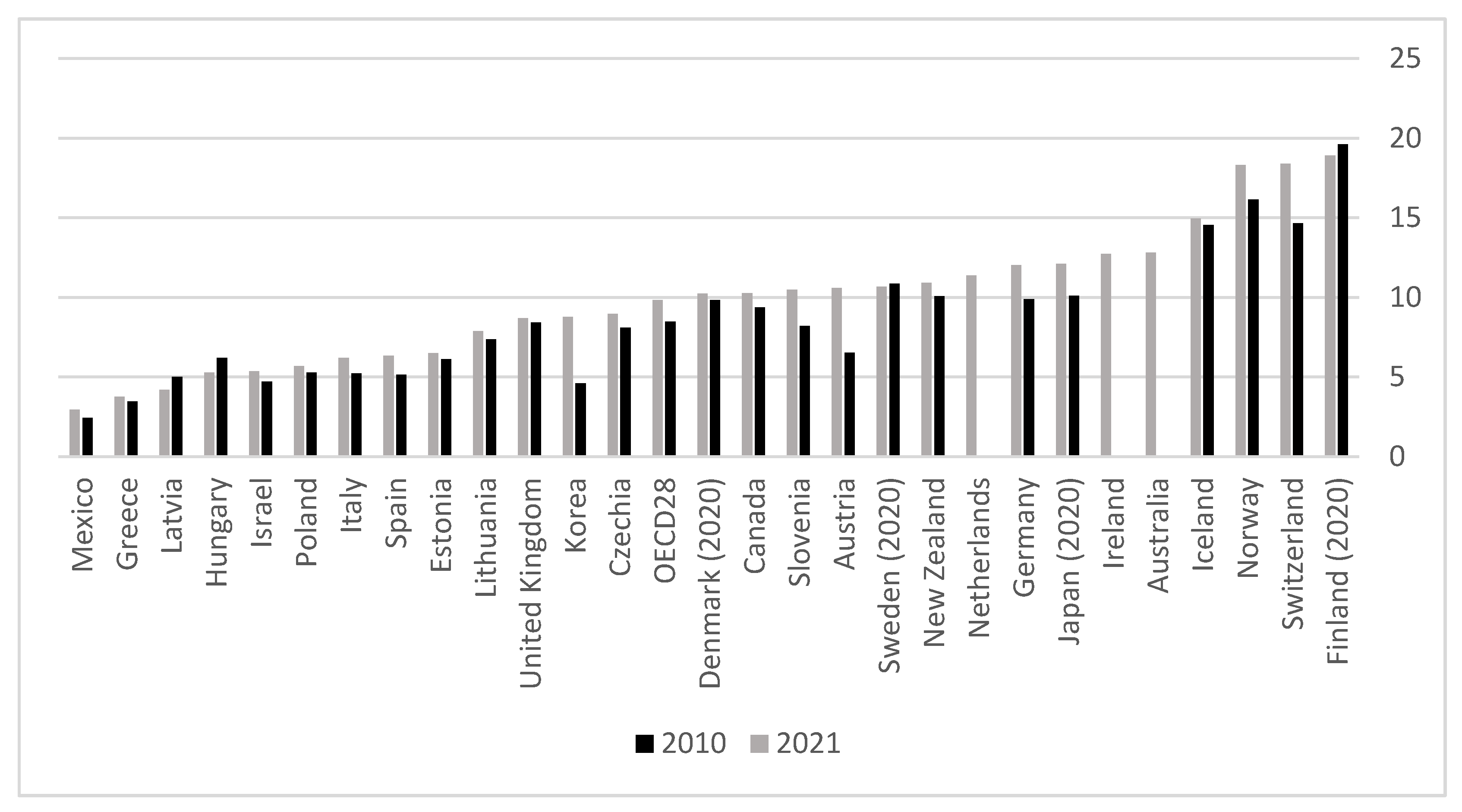
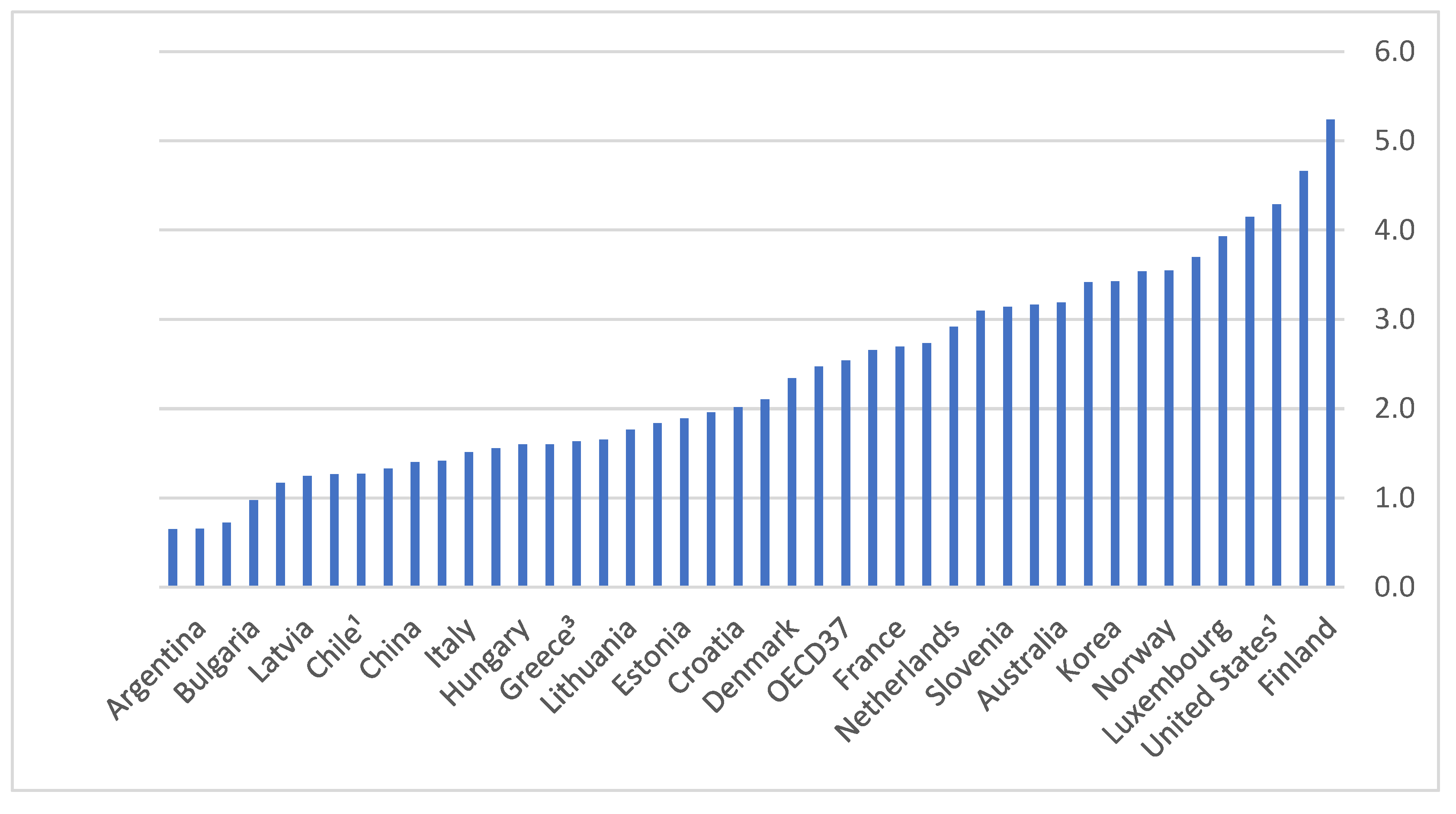
3.1. Foreign Training

3.2. Medical School Graduates
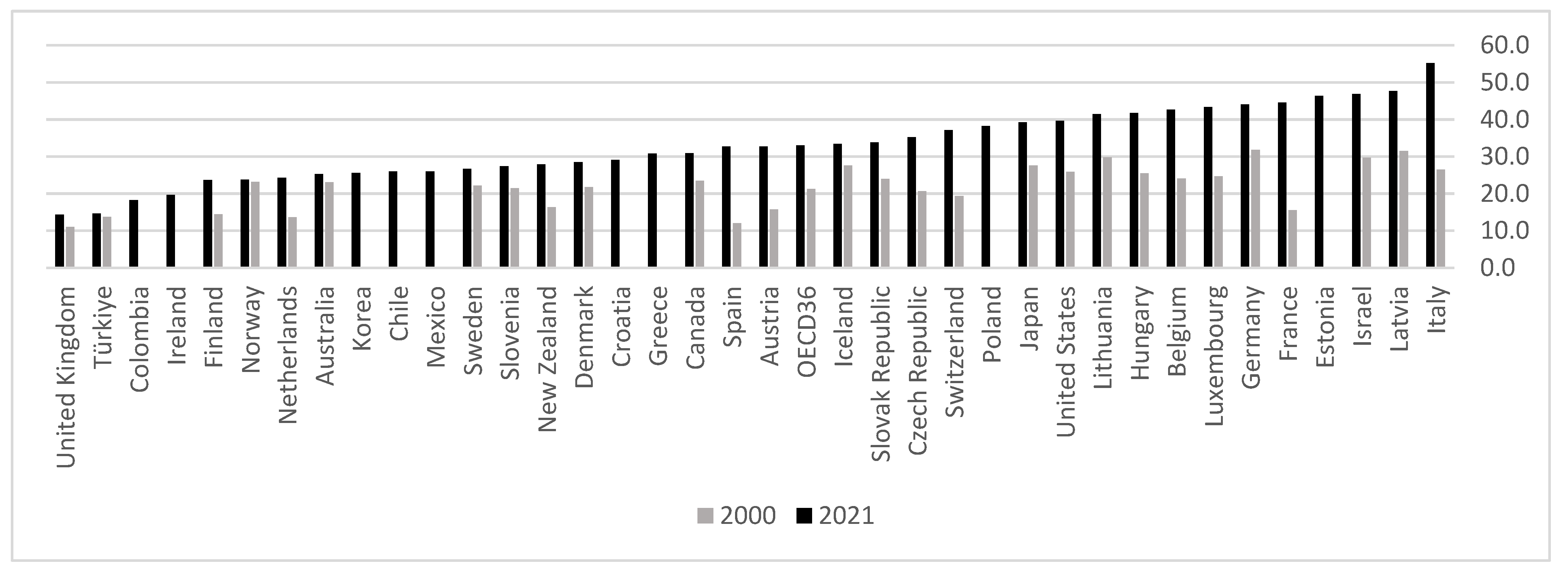
3.3. Aging
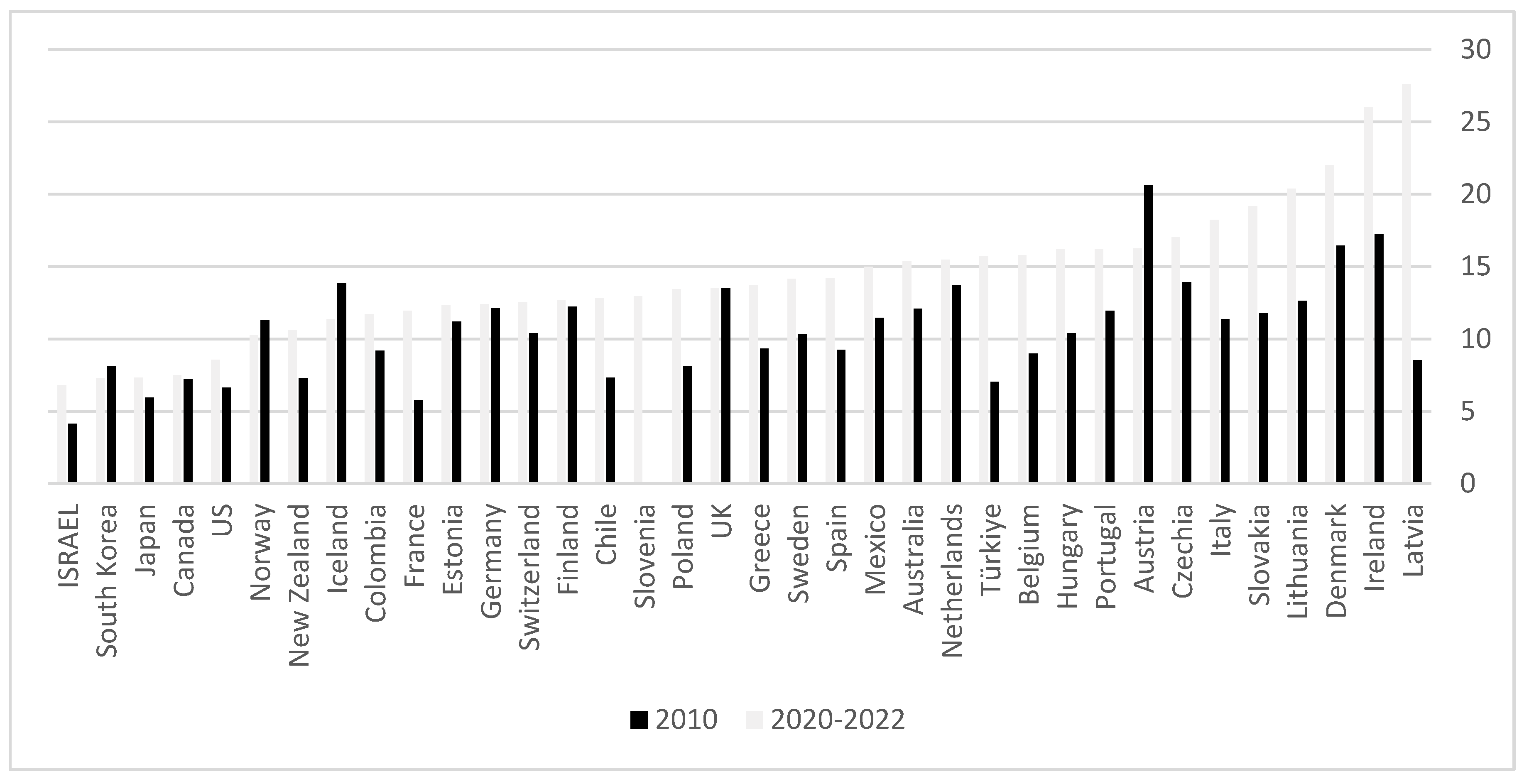
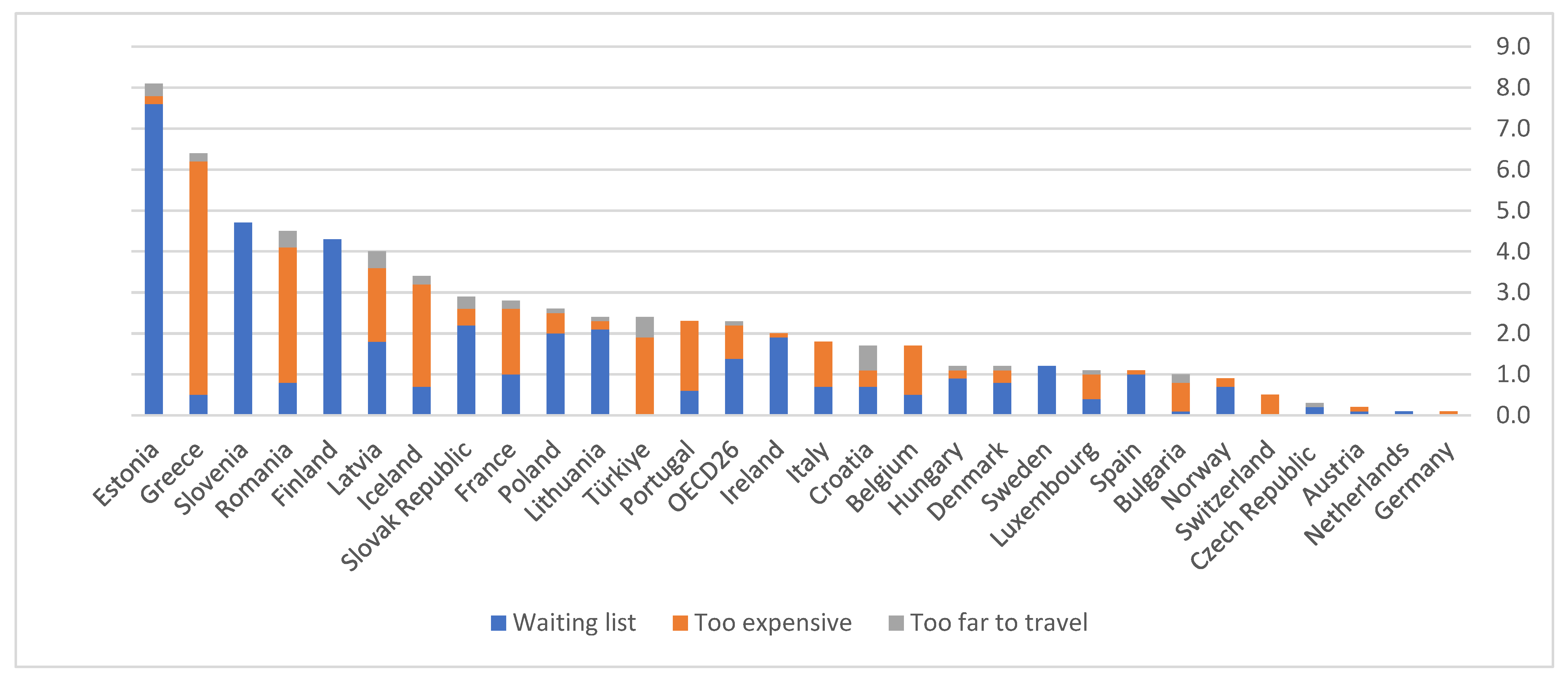
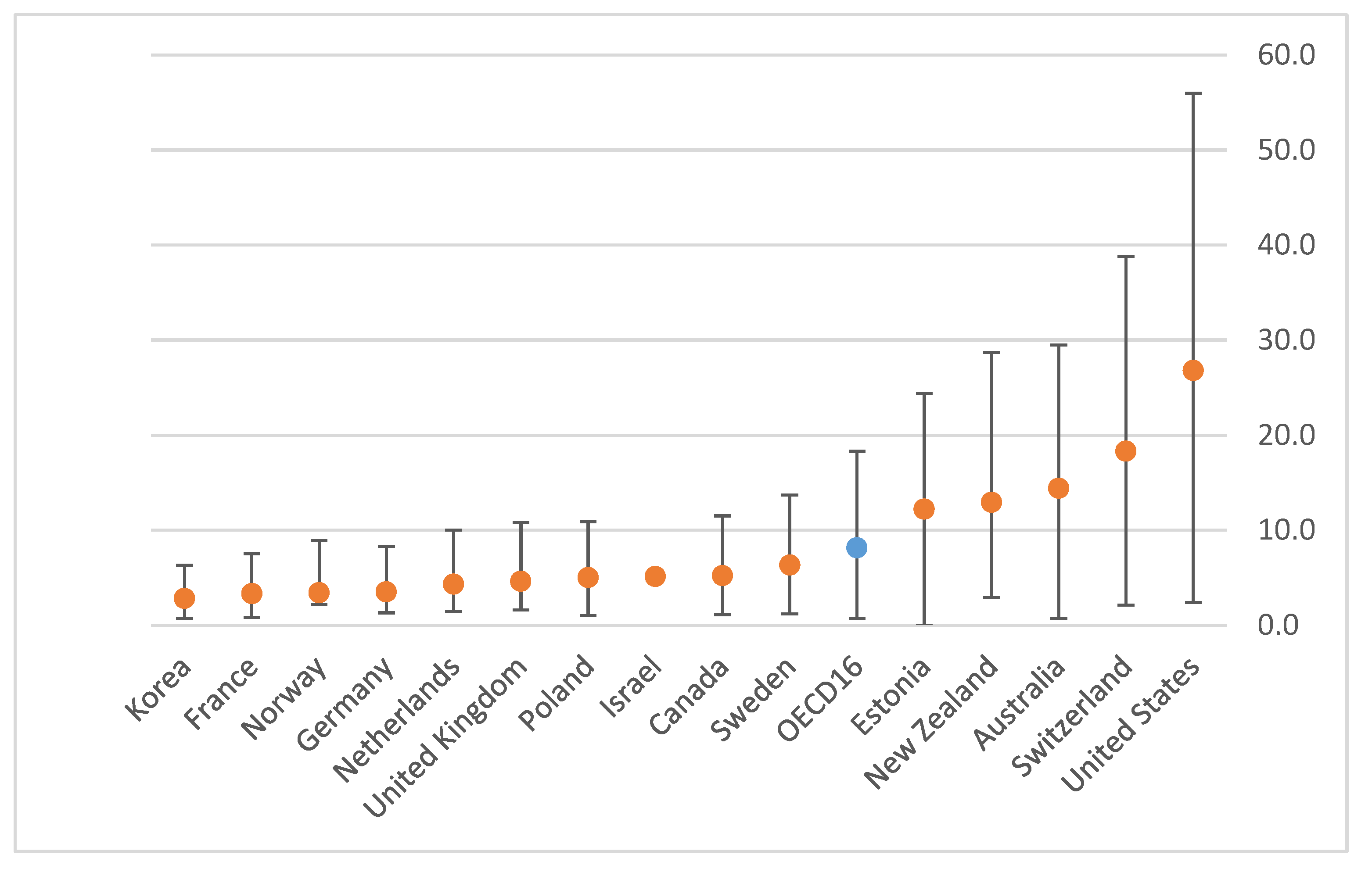
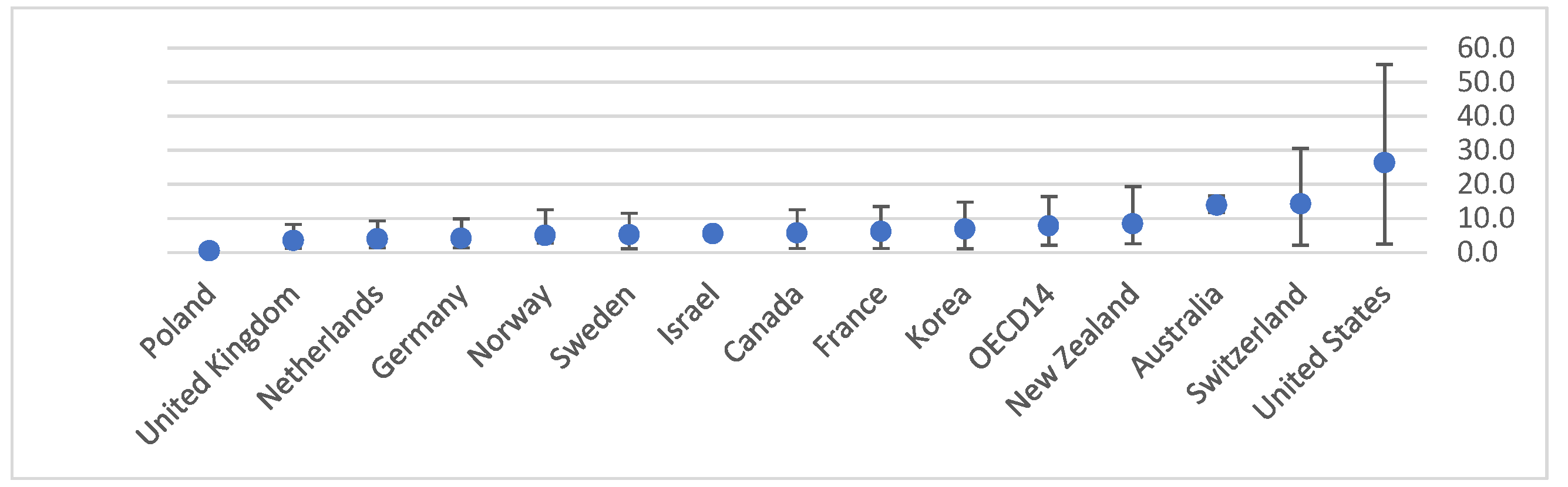
4. Snapshot of Healthcare Services and Access across the OECD
5. Strategic Physician Workforce Planning in Israel
6. Strategic Physician Workforce Planning in Germany
7. Strategic Physician Workforce Planning in Australia
8. Strategic Physician Workforce Planning in Norway
9. Discussion
- Data based forecasting of medical care supply and demand, achieved through a wide collaboration of stakeholders.
- Considering the changing boundaries of health professions, with an emphasis on the nursing workforce, while conducting physician workforce forecasting.
- Increasing the number of medical graduates, preferably domestically trained, but also foreign trained as needed.
- Reducing the uneven distribution of physician workforce between regions and specialties, with a special emphasis on general practitioners such as family physicians and rural, remote, or peripheral areas.
- Improving mechanisms for data supported, supply and demand based, physician workforce planning: Promoting a structured work method that entails creating models and databases to be used for workforce planning and which strengthen the link between workforce planning and policy formulation [12,27,38]. Towards this goal, a designated governmental body dealing with healthcare workforce planning can be established. The responsibilities of this body include collecting relevant information for the evaluation of medical supply and demand, publishing current forecasts of future needs, and evaluating the implications for medical training frameworks [12].
- Alternatively, the Dutch model may be considered. This model includes establishing an independent non-governmental advisory body, similar to the Dutch Advisory Council on Medical Manpower Planning (ACMMP), in which central stakeholders (such as professional associations, medical schools, health funds, and more) will collaborate in an equal partnership. Working jointly, they will formulate predictions concerning the workforce, update these predictions and present recommendations to the government concerning the necessary number of medical students. Adopting this model requires conducting a cost-benefit analysis, defining the proposed organization’s structure, defining the various roles of stakeholders in such a way that a balance of power is maintained, and defining the relations with governmental agencies [12].
- Restructuring medical education to align with population needs and the requirements of the healthcare systems: Updating the educational curriculum and promoting the accreditation of medical education centers. This needs to be done in such a way that the physicians of tomorrow will receive the necessary training to meet emerging challenges and to supply the increased demand in specific fields such as mental health, geriatrics, palliative care, etc. [1,39].
- Increasing the number of domestically trained medical students: Increasing the capacity of existing domestic medical schools to accept new candidates, while also considering opening additional medical schools as needed. A common problem in this field is the limited capacity of clinical training frameworks in hospitals. Therefore, it is recommended to expand clinical rotations and increase total training capacity, through methods such as increasing the quantity of shifts that include clinical training, increasing the size of training groups, and establishing clinical rotations in out of hospital frameworks (such as community based primary care institutions and public health institutions). A critical component of this is including sufficient budgets for teaching staff and additional teaching hours [12,39].
- Encouraging the return of medical students studying abroad: Offering financial assistance to students studying in foreign medical schools which meet predefined standards of medical education, under the condition that they return after the completion of their studies and work in geographic areas and professional fields of national preference. This measure is supplementary to increasing the number of domestic medical school students, serving as a source for increasing the number of medical graduates despite possible limitations of the domestic training system [12].
- Defining a standardized method for managing residency programs and placement of candidates: Creating a central system to manage residency programs, using estimates based on workforce forecasts to decide the number of available positions. Another important measure is ensuring that there be a designated budget for the different residency programs, allocated based on the quantity and type of residency positions offered, to avoid reliance on the hospitals’ general budget resulting in low wages and difficult working conditions for residents [12].
- Utilizing strategies to recruit new physicians, and retain current physicians, in areas facing current or projected shortages: Acting to reduce the burden of care on physicians in underserved areas by reducing clinical teaching hours, delegating tasks to other healthcare professionals, such as nurses, and incentivizing physicians practicing in those areas by providing monetary benefits and work hour flexibility [1,39]. Another important measure is increasing the number of medical students intending to practice in underserved areas and fields when they finish their training, by providing academic priority and monetary support for them during medical school [1,12,39].
- Moving toward a multi-professional approach in healthcare workforce planning: In order to better respond to population needs, improve access to healthcare and reduce costs, forecasting models need to assess the impact of changing healthcare delivery models in an integrated way [39]. This is especially important in the field of primary care which commonly faces shortages, and in which different healthcare professions, with an emphasis on the nursing workforce, have been shown to contribute to reducing physician work burden when their scope of practice was increased [38,39].
10. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- World Health Organization. (2022). Health and care workforce in Europe: Time to act. World Health Organization, Regional Office for Europe.
- World Health Organization. (2016). Global strategy on human resources for health: Workforce 2030. World Health Organization. https://iris.who.int/handle/10665/250368.
- World Health Organization. (2022). Retention of the health workforce in rural and remote areas: A systematic review. Geneva: World Health Organization; Human Resources for Health Observer Series No. 25.
- Ford, J., Sowden, S., Olivera, J., Bambra, C., Gimson, A., Aldridge, R., & Brayne, C. (2021). Transforming health systems to reduce health inequalities. Future Healthcare Journal, 8(2), e204–e209. [CrossRef]
- Ziemann, M. , Chen, C., Forman, R., Sagan, A., & Pittman, P. (2023). Global Health Workforce responses to address the COVID-19 pandemic: What policies and practices to recruit, retain, reskill, and support health workers during the COVID-19 pandemic should inform future workforce development? European Observatory on Health Systems and Policies. http://www.ncbi.nlm.nih.gov/books/NBK594085/.
- Pittman, P., Chen, C., Erikson, C., Salsberg, E., Luo, Q., Vichare, A., Batra, S., & Burke, G. (2021). Health Workforce for Health Equity. Medical Care, 59(Suppl 5), S405–S408. [CrossRef] [PubMed]
- Denis, J.-L., & van Gestel, N. (2016). Medical physicians in healthcare leadership: Theoretical and practical challenges. BMC Health Services Research, 16 Suppl 2(Suppl 2), 158. [CrossRef]
- Htay, M., & Whitehead, D. (2021). The effectiveness of the role of advanced nurse practitioners compared to physician-led or usual care: A systematic review. International Journal of Nursing Studies Advances, 3, 100034. [CrossRef]
- Starfield, B., Shi, L., Grover, A., & Macinko, J. (2005). The effects of specialist supply on populations’ health: Assessing the evidence. Health Affairs (Project Hope), Suppl Web Exclusives, W5-97-W5-107. [CrossRef]
- World Health Organization. (2020). Norway health system review. WHO Regional Office for Europe. https://www.euro.who.int/__data/assets/pdf_file/0005/443398/Norway-Hit-oct2020-rev.pdf.
- Skudal, K. E. , Garratt, A. M., Eriksson, B., & Leinonen, T. (2016). Psychometric properties of the Nordic Patient Experiences Questionnaire (NORPEQ): Patient safety culture in Norwegian nursing homes. Scandinavian Journal of Caring Sciences, 30(2), 280–285. [CrossRef]
- Lafortune, G. , Dedet, G., Balestat, G., Gellie, V., Turatto, F., Dagistan, E., & Slenter, V. (2023). OECD Report on Medical Education and Training in Israel, OECD. https://search.oecd.org/health/OECD-report-on-medical-education-and-training-in-Israel.pdf.
- Pugh, R. , & Dubois, A. (2021). Peripheries within economic geography: Four “problems” and the road ahead of us. Journal of Rural Studies, 87, 267–275. [CrossRef]
- Hart, L. G., Larson, E. H., & Lishner, D. M. (2005). Rural definitions for health policy and research. American Journal of Public Health, 95(7), 1149–1155. [CrossRef] [PubMed]
- McIntyre, D. , & Chow, C. K. (2020). Waiting Time as an Indicator for Health Services Under Strain: A Narrative Review. INQUIRY: The Journal of Health Care Organization, Provision, and Financing, 57, 004695802091030. [CrossRef]
- Regionale Verteilung der Ärzte in der vertragsärztlichen Versorgung. (n.d.). KBV - Region; Kassenärztliche Bundesvereinigung (KBV). Retrieved March 31, 2024, from https://gesundheitsdaten.kbv.de/cms/html/16402.php.
- Bedarfsplanung. (n.d.). KBV - Bedarfsplanung; Kassenärztliche Bundesvereinigung (KBV). Retrieved March 31, 2024, from https://www.kbv.de/html/bedarfsplanung.php.
- Arztzeit-Mangel. (2023, June 21). KBV - Arztzeit-Mangel; Kassenärztliche Bundesvereinigung (KBV). https://www.kbv.de/html/themen_38343.php.
- Kunnskapsdepartementet. 2022. Muligheter og kostnader ved økning av utdanningskapasiteten i medisin [Rapport]. https://www.regjeringen.no/no/dokumenter/muligheter-og-kostnader-ved-okning-av-utdanningskapasiteten-i-medisin/id2912736/.
- Omsorgsdepartementet. (2020, May 11). Handlingsplan for allmennlegetjenesten 2020-2024; Attraktiv, kvalitetssikker og teambasert [Plan]. https://www.regjeringen.no/no/dokumenter/handlingsplan-for-allmennlegetjenesten/id2701926/.
- Helsedirektoratet. 2020. Leger i Kommunene Og Spesialisthelsetjenesten. https://www.helsedirektoratet.no/rapporter/leger-i-kommune-og-spesialisthelsetjenesten/Leger%20i%20kommunene%20og%20spesialisthelsetjenesten%20-%20rapport%202020.pdf/_/attachment/inline/9bcf5459-80e6-4716-ab00-1766ee0cc0db:ac1f2b4e2a8216bf8aa6246e843249ffc49721db/Leger%20i%20kommunene%20og%20spesialisthelsetjenesten%20-%20rapport%202020.pdf.
- Ministry of Health (2022). Health inequalities and dealing with them 2021. Ministry of Health. https://www.gov.il/he/departments/publications/reports/inequality-2021-n.
- Australian Government department of health and aged care. (2019). Medical practitioners. https://hwd.health.gov.au/resources/publications/factsheet-mdcl-2019.pdf.
- Australian Government department of health and aged care. (2022). National Medical Workforce Strategy. https://www.health.gov.au/sites/default/files/documents/2022/03/national-medical-workforce-strategy-2021-2031.pdf.
- the Senate Community Affairs Committee Secretariat. (2012). The factors affecting the supply of health services and medical professionals in rural areas (pp. 83–104). https://www.aph.gov.au/parliamentary_business/committees/senate/community_affairs/completed_inquiries/2010-13/rurhlth/report/~/media/wopapub/senate/committee/clac_ctte/completed_inquiries/2010-13/rur_hlth/report/report.ashx.
- Medical Deans Australia and New Zealand. (2019, October). Policy proposal: Medical schools’ contribution to addressing the medical workforce shortage in regional and rural Australia. https://medicaldeans.org.au/md/2020/01/2019-Oct_Policy-proposal_Rural-Medical-Workforce_MDANZ_FINAL.pdf.
- Ministry of Health. (2023). Healthcare workforce reform: Ministry of Health policy in response to the shortage of physicians in Israel and strengthening the Negev and the Galil. Ministry of Health. https://www.gov.il/BlobFolder/reports/health-human-resources-reform-n/he/files_publications_units_financial-strategic-planning_publications_man-power_health-human-resources-reform.pdf.
- Ministry of Health. (n.d.). New Physicians 2023 Summary. Ministry of Health. https://www.gov.il/he/Departments/publications/reports/the-new-physicians-2023.
- Davidovitch, N., Lev, N., & Levi, B. (n.d.). The Healthcare System in Israel: Between the NewNormal and the OldNormal. Taub Center for Social Policy Studies in Israel. https://www.taubcenter.org.il/en/research/healthcare-between-new-and-old/.
- Saunes, I. , Karanikolos, M., & Sagan, A. (2020). Norway: Health system review (Health Systems in Transition). https://iris.who.int/bitstream/handle/10665/331786/HiT-22-1-2020-eng.pdf?sequence=1.
- Chelak, K. , & Chakole, S. (2023). The Role of Social Determinants of Health in Promoting Health Equality: A Narrative Review. Cureus, 15(1), e33425. [CrossRef]
- Ziegler, C. , & Muchira, J. (2023). Climate Change. Primary Care: Clinics in Office Practice, 50(4), 645–655. [CrossRef]
- Kuhlmann, E. , Denis, J.-L., Côté, N., Lotta, G., & Neri, S. (2023). Comparing Health Workforce Policy during a Major Global Health Crisis: A Critical Conceptual Debate and International Empirical Investigation. International Journal of Environmental Research and Public Health, 20(6), Article 6. [CrossRef]
- Nancarrow, S. A. , & Borthwick, A. M. (2005). Dynamic professional boundaries in the healthcare workforce. Sociology of Health & Illness, 27(7), 897–919. [CrossRef]
- Bourcier, D. , Collins, B. W., Tanya, S. M., Basu, M., Sayal, A. P., Moolla, S., Dong, A., Balas, M., Molcak, H., & Punchhi, G. (2022). Modernising physician resource planning: A national interactive web platform for Canadian medical trainees. BMC Health Services Research, 22(1), 116. [CrossRef]
- Schmitt, T. , Czabanowska, K., & Schröder-Bäck, P. (2024). What is context in knowledge translation? Results of a systematic scoping review. Health Research Policy and Systems, 22(1), 52. [CrossRef]
- Abelsen, B. , Strasser, R., Heaney, D., Berggren, P., Sigurðsson, S., Brandstorp, H., Wakegijig, J., Forsling, N., Moody-Corbett, P., Akearok, G. H., Mason, A., Savage, C., & Nicoll, P. (2020). Plan, recruit, retain: A framework for local healthcare organizations to achieve a stable remote rural workforce. Human Resources for Health, 18(1), 63. [CrossRef]
- Ready for the Next Crisis? Investing in Health System Resilience. (2023). OECD Publishing. [CrossRef]
- OECD. (2016). Health Workforce Policies in OECD Countries: Right Jobs, Right Skills, Right Places. OECD. [CrossRef]
- OECD (2019), Health in the 21st Century: Putting Data to Work for Stronger Health Systems, OECD Health Policy Studies, OECD Publishing, Paris. [CrossRef]
- Delamaire, M. and G. Lafortune (2010), "Nurses in Advanced Roles: A Description and Evaluation of Experiences in 12 Developed Countries", OECD Health Working Papers, No. 54, OECD Publishing, Paris. [CrossRef]
- Australian Government department of Health and Aged Care (2023), Nurse Practitioner Workforce Plan. https://www.health.gov.au/sites/default/files/2023-05/nurse-practitioner-workforce-plan.pdf.
- Ministry of health. (2024). The Committee for Addressing the Medical Manpower Shortage in the Health System; the subcommittee for determining mechanisms for significant enlargement and national regulation of clinical fields. https://www.gov.il/he/pages/the-committee-dealing-shortage-medical-personnel-health-system.
| Challenges | |
| Physician workforce shortage | Israel, Germany |
| Domestic medical graduate shortage | Israel, Norway |
| Aging of physician workforce | Israel, Germany |
| Unequal distribution of physician workforce | Israel, Germany, Australia, Norway |
| Oversupply of physician workforce | Australia, Norway |
| Limited capacity of domestic medical education system | Israel, Norway |
| Key points of strategic planning | |
| Data based forecasting of medical supply and need. | Israel, Germany, Australia |
| Guiding choice of specialty by national needs. | Germany, Australia |
| Increasing allocation for students from peripheral and rural areas. | Israel, Australia |
| Financial incentivization: For students to return from abroad, for medical students from the periphery, for specialists in areas of national interest. | Israel, Norway |
| Creating wide collaboration between stakeholders for workforce planning. | Germany, Australia |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




