Submitted:
27 May 2024
Posted:
28 May 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
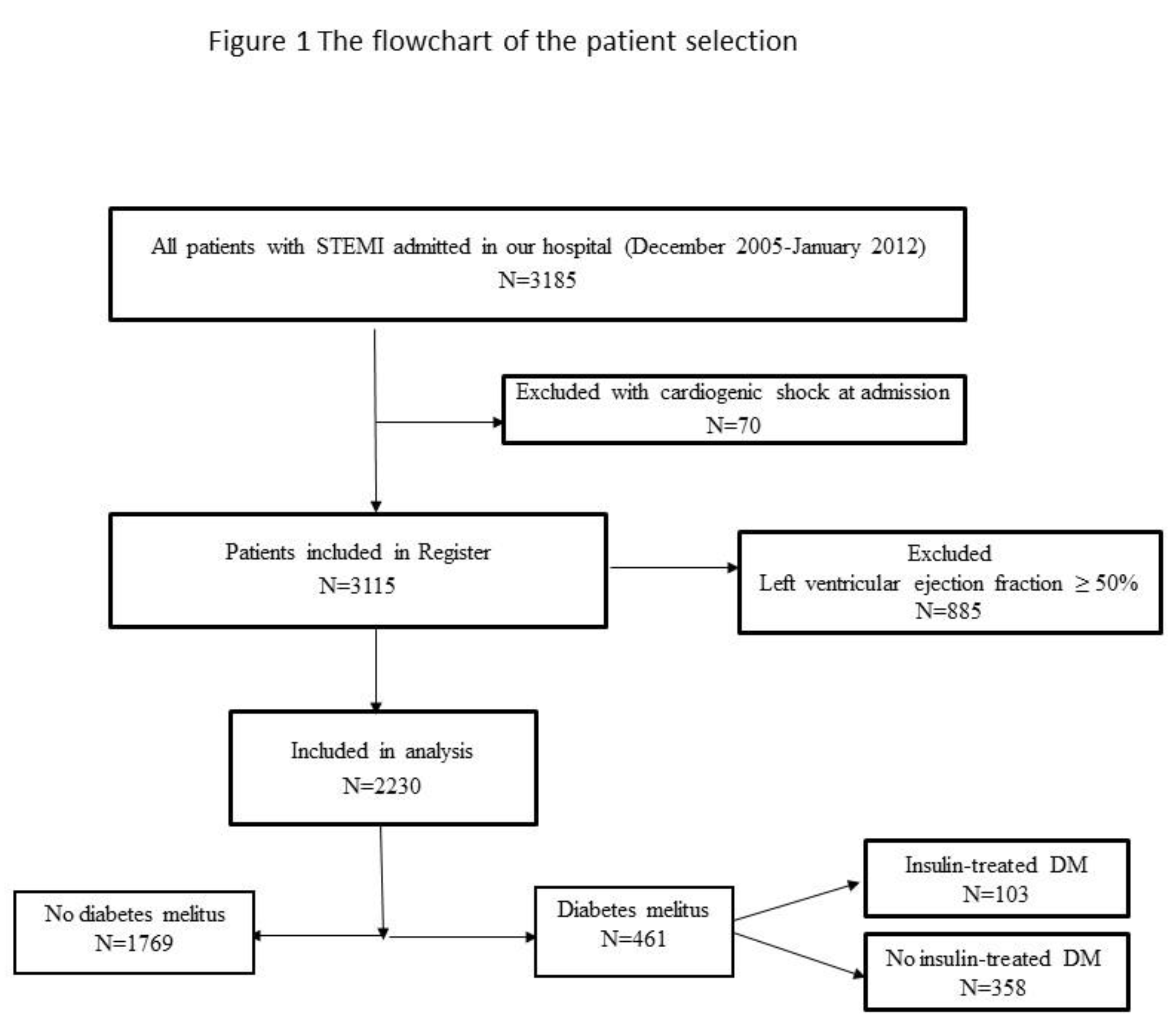
2.1. Study Population, Inclusion and Exclusion Criteria, Data Collection, and Definitions
2.2. Ethics
2.3. Statistical Analysis
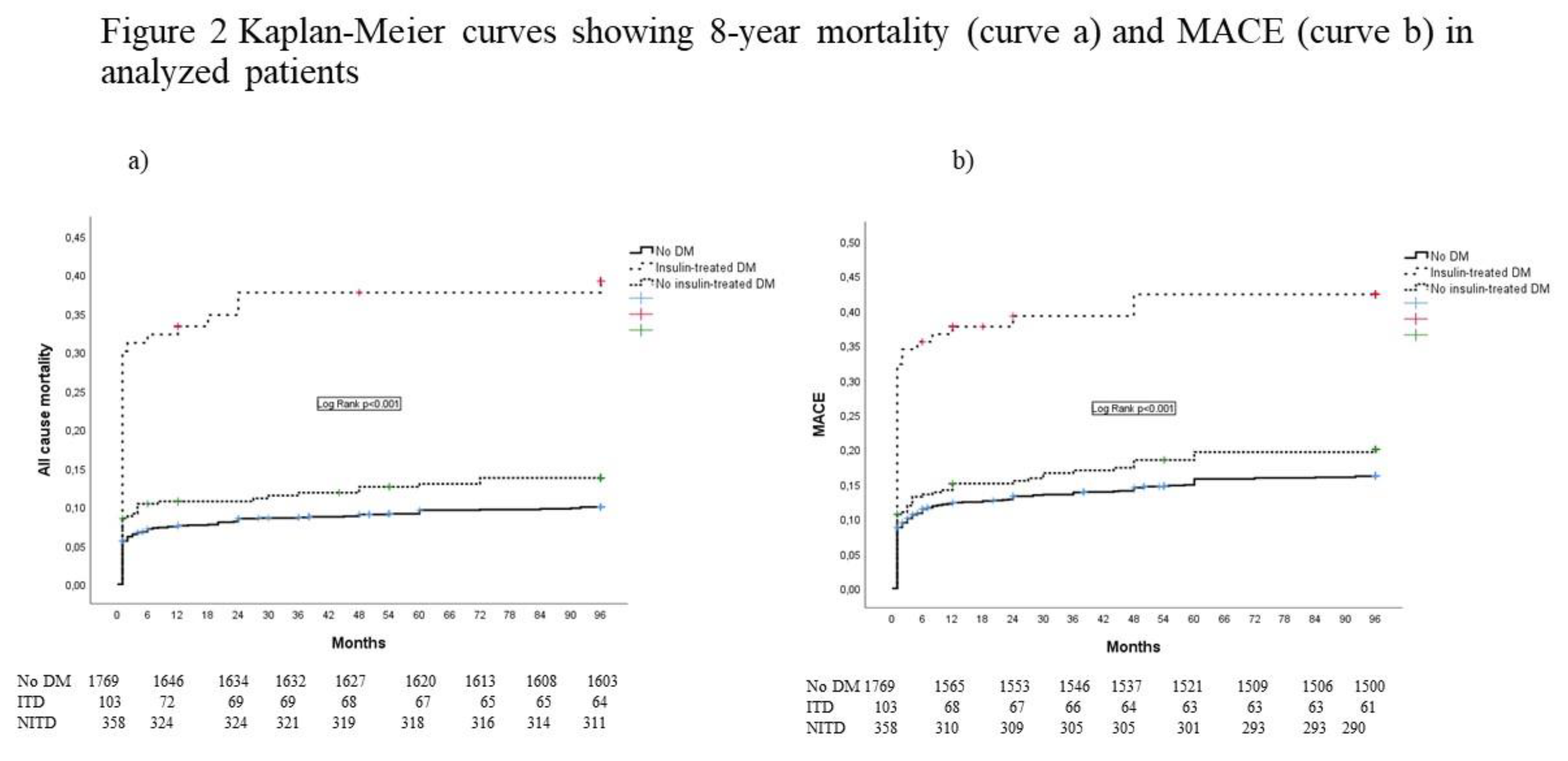
3. Results
4. Discussion
4.1. Baseline Characteristics
4.2. Prognostic Impact of ITDM and NITD in Patients with Myocardial Infarction and/or Heart Failure
4.3. Possible Mechanisms for Higher Adverse Events Rates in Patients with ITDM
4.4. Clinical Implications
4.5. Study Limitations
5. Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Acknowledgments
Conflicts of Interest
References
- Ng, V.G.; Lansky, A.J.; Meller, S.; Witzenbichler, B.; Guagliumi, G.; Peruga, J.Z.; et al. The prognostic importance of left ventricular function in patients with ST-segment elevation myocardial infarction: the HORIZONS-AMI trial. Eur Heart J Acute Cardiovasc Care 2014, 3, 67–77. [Google Scholar] [CrossRef] [PubMed]
- Rossello, X.; Ferreira, J.P.; McMurray, J.J.; Aguilar, D.; Pfeffer, M.A.; Pitt, B.; et al. High-Risk Myocardial Infarction Database Initiative. Editor's Choice- Impact of insulin-treated diabetes on cardiovascular outcomes following high-risk myocardial infarction. Eur Heart J Acute Cardiovasc Care 2019, 8, 231–241. [Google Scholar] [CrossRef] [PubMed]
- Tajik, A.A.; Dobre, D.; Aguilar, D.; Kjekshus, J.; Zannad, F.; Dickstein, K. High-Risk MI Database Scientific Committee. A history of diabetes predicts outcomes following myocardial infarction: an analysis of the 28 771 patients in the High-Risk MI Database. Eur J Heart Fail 2017, 19, 635–642. [Google Scholar] [CrossRef] [PubMed]
- Lin, M.J.; Chen, C.Y.; Lin, H.D.; Wu, H.P. Impact of diabetes and hypertension on cardiovascular outcomes in patients with coronary artery disease receiving percutaneous coronary intervention. BMC Cardiovasc Disord 2017, 17, 12. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Tong, Y.; Zhang, Y.; Tang, L.; Lv, Q.; Zhang, F.; et al. Effects on All-cause Mortality and Cardiovascular Outcomes in Patients With Type 2 Diabetes by Comparing Insulin With Oral Hypoglycemic Agent Therapy: A Meta-analysis of Randomized Controlled Trials. Clin Ther 2016, 38, 372–386. [Google Scholar] [CrossRef] [PubMed]
- Reinstadler, S.J.; Stiermaier, T.; Eitel, C.; Metzler, B.; de Waha, S.; Fuernau, G.; et al. Relationship between diabetes and ischaemic injury among patients with revascularized ST-elevation myocardial infarction. Diabetes Obes Metab 2017, 19, 1706–1713. [Google Scholar] [CrossRef] [PubMed]
- Ritsinger, V.; Lagerqvist, B.; Lundman, P.; Hagström, E.; Norhammar, A. Diabetes, metformin and glucose lowering therapies after myocardial infarction: Insights from the SWEDEHEART registry. Diab Vasc Dis Res 2020, 17, 1479164120973676. [Google Scholar] [CrossRef] [PubMed]
- Kerola, A.M.; Semb, A.G.; Juonala, M.; Palomäki, A.; Rautava, P.; Kytö, V. Long-term cardiovascular prognosis of patients with type 1 diabetes after myocardial infarction. Cardiovasc Diabetol 2022, 21, 177. [Google Scholar] [CrossRef] [PubMed]
- Schupp, T.; Abumayyaleh, M.; Weidner, K.; Lau, F.; Reinhardt, M.; Abel, N.; et al. Prognostic Implications of Type 2 Diabetes Mellitus in Heart Failure with Mildly Reduced Ejection Fraction. J Clin Med 2024, 13, 742. [Google Scholar] [CrossRef]
- Li, L.; Li, G.; Chen, H.; Feng, Z.; Zhang, L.; Chen, L.; et al. Role of Diabetes Mellitus in Acute Coronary Syndrome Patients with Heart Failure and Midrange Ejection Fraction Who Have Undergone Percutaneous Coronary Intervention: A 3-Year Case-Series Follow-Up Retrospective Study. Diabetes Metab Syndr Obes 2021, 14, 4931–4944. [Google Scholar] [CrossRef]
- Hoebers, L.P.; Claessen, B.E.; Woudstra, P.; DeVries, J.H.; Wykrzykowska, J.J.; Vis, M.M.; et al. Long-term mortality after primary percutaneous coronary intervention for ST-segment elevation myocardial infarction in patients with insulin-treated versus non-insulin-treated diabetes mellitus. EuroIntervention 2014, 10, 90–96. [Google Scholar] [CrossRef] [PubMed]
- Mrdovic ISavic, L.; Lasica, R.; Krljanac, G.; Asanin, M.; Brdar, N.; et al. Efficacy and safety of tirofiban-supported primary percutaneous coronary intervention in patients pretreated with 600 mg clopidogrel: Results of propensity analysis using the clinical center of serbia STEMI register. Eur. Heart J Acute Cardiovasc Care 2014, 3, 56–66. [Google Scholar] [CrossRef]
- Thygesen, K.; Alpert, J.S.; Jaffe, A.S.; Chaitman, B.R.; Bax, J.J.; Morrow, D.A.; White, H.D.; ESC Scientific Document Group. Fourth universal definition of myocardial infarction (2018). Eur. Heart J 2019, 40, 237–269. [Google Scholar] [CrossRef] [PubMed]
- Rosselló, X.; Huo, Y.; Pocock, S.; Van de Werf, F.; Chin, C.T.; Danchin, N.; Lee, S.W.; Medina, J.; Vega, A.; Bueno, H. Global geographical variations in ST-segment elevation myocardial infarction management and post-discharge mortality. Int J Cardiol 2017, 245, 27–34. [Google Scholar] [CrossRef] [PubMed]
- Massalha, S.; Luria, L.; Kerner, A.; Roguin, A.; Abergel, E.; Hammerman, H.; et al. Heart failure in patients with diabetes undergoing primary percutaneous coronary intervention. Eur Heart J Acute Cardiovasc Care 2016, 5, 455–462. [Google Scholar] [CrossRef] [PubMed]
- Biswas, S.; Dinh, D.; Andrianopoulos, N.; Lefkovits, J.; Ajani, A.; Duffy, S.J.; et al. Comparison of Long-Term Outcomes After Percutaneous Coronary Intervention in Patients With Insulin-Treated Versus Non-Insulin Treated Diabetes Mellitus. Am J Cardiol 2021, 148, 36–43. [Google Scholar] [CrossRef] [PubMed]
- van der Schaaf, R.J.; Henriques, J.P.; Wiersma, J.J.; Koch, K.T.; Baan JJr Mulder, K.J.; et al. Primary percutaneous coronary intervention for patients with acute ST elevation myocardial infarction with and without diabetes mellitus. Heart. 2006, 92, 117–118. [Google Scholar] [CrossRef] [PubMed]
- Antoniucci, D.; Valenti, R.; Migliorini, A.; Parodi, G.; Moschi, G.; Memisha, G.; et al. Impact of insulin-requiring diabetes mellitus on effectiveness of reperfusion and outcome of patients undergoing primary percutaneous coronary intervention for acute myocardial infarction. Am J Cardiol 2004, 93, 1170–1172. [Google Scholar] [CrossRef] [PubMed]
- Bundhun, P.K.; Li, N.; Chen, M.H. Adverse cardiovascular outcomes between insulin-treated and non-insulin treated diabetic patients after percutaneous coronary intervention: a systematic review and meta-analysis. Cardiovasc Diabetol 2015, 14, 135. [Google Scholar] [CrossRef]
- Komajda, M.; Tavazzi, L.; Francq, B.G.; Böhm, M.; Borer, J.S.; Ford, I.; et al. SHIFT Investigators. Efficacy and safety of ivabradine in patients with chronic systolic heart failure and diabetes: an analysis from the SHIFT trial. Eur J Heart Fail 2015, 17, 1294–1301. [Google Scholar] [CrossRef]
- Dries, D.L.; Sweitzer, N.K.; Drazner, M.H.; Stevenson, L.W.; Gersh, B.J. Prognostic impact of diabetes mellitus in patients with heart failure according to the etiology of left ventricular systolic dysfunction. J Am Coll Cardiol 2001, 38, 421–428. [Google Scholar] [CrossRef] [PubMed]
- Nahser, P.J., Jr.; Brown, R.E.; Oskarsson, H.; Winniford, M.D.; Rossen, J.D. Maximal coronary flow reserve and metabolic coronary vasodilation in patients with diabetes mellitus. Circulation 1995, 91, 635–640. [Google Scholar] [CrossRef] [PubMed]
- Norhammar, A.; Malmberg, K.; Rydén, L.; Tornvall, P.; Stenestrand, U.; Wallentin, L. Register of Information and Knowledge about Swedish Heart Intensive Care Admission (RIKS-HIA). Under utilisation of evidence-based treatment partially explains for the unfavourable prognosis in diabetic patients with acute myocardial infarction. Eur Heart J 2003, 24, 838–844. [Google Scholar] [CrossRef] [PubMed]
- McDonagh, T.A.; Metra, M.; Adamo, M.; Gardner, R.S.; Baumbach, A.; et al. ESC Scientific Document Group, 2023 Focused Update of the 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: Developed by the task force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) With the special contribution of the Heart Failure Association (HFA) of the ESC. European Heart Journal 2023, 44, 3627–3639. [Google Scholar]
| Characteristics | No DM N= 1769 |
P value | ITDM N= 103 |
NITDM N=358 |
P value |
|---|---|---|---|---|---|
| Age, years med(IQR) | 60(52,70) | <0.001 | 63(57, 72) | 64(58, 73) | 0.971 |
| Female, n(%) | 459(25.9) | <0.001 | 37(35.9) | 131(36.6) | 0.901 |
| BMI, med (IQR) | 25.9(24.2, 27.8) | 0.493 | 27.3(24.5, 29.7) | 26.8(24.8, 29.4) | 0.644 |
| Previous MI, n(%) | 197(11.1) | 0.009 | 22(21.3) | 49(13.7) | 0.037 |
| Previous angina, n(%) | 126(7.1) | 0.032 | 10(9.7) | 38(10.6) | 0.791 |
| Previous stroke, n(%) | 69(3.9) | <0.001 | 8(7.7) | 25(7.9) | 0.786 |
| Hypertension, n(%) | 1130(63.9) | <0.001 | 80(77.7) | 295(82.1) | 0.277 |
| HLP, n(%) | 1030(58.2) | 0.192 | 58(56.3) | 225(62.8) | 0.230 |
| Smoking, n(%) | 965(54.6) | <0.001 | 29(28.2) | 112(31.3) | 0.544 |
| Family hystory, n(%) | 577(32.6) | <0.001 | 20(19.4) | 85(23.7) | 0.356 |
| Pain duration, hours med(IQR) | 2.5(1.5, 4.5) | <0.001 | 3(1.5, 5) | 3(2, 5.5) | 0.861 |
| Atrial fibrillation on initial ECG, n(%) | 147(8.3) | 0.950 | 20(19.4) | 21(5.9) | <0.001 |
| Complete AV block, n(%) | 86(4.9) | 0.086 | 18(17.4) | 11(3.1) | <0.001 |
| Killip class >1, n(%) | 262(14.8) | <0.001 | 49(47.5) | 76(21.1) | <0.001 |
| Systolic BP at admission, med(IQR) | 130(120, 150) | <0.001 | 130(110, 150) | 140(130, 160) | <0.001 |
| Heart rate at admission med(IQR) | 80(70, 90) | <0.001 | 80(70, 100) | 82(75, 97) | 0.235 |
| Multivessel disease, n(%) | 991(56) | <0.001 | 89(5.1) | 239(66.7) | 0.002 |
| 3-vessel disease, n(%) | 455(25.7) | <0.001 | 61(59.2) | 128(35.7) | <0.001 |
| LM stenosis, n(%) | 113(6.9) | 0.030 | 10(9.8) | 30(8.4) | 0.679 |
| Postprocedural flow TIMI <3, n(%) | 94(5.3) | 0.019 | 16(15.5) | 23(6.4) | 0.003 |
| Stent implanted, n(%) | 1634(92.4) | 0.091 | 92(89.4) | 325(90.8) | 0.958 |
| Acute stent thrombosis, n(%) | 22(1.2) | 0.261 | 4(3.9) | 4(1.1) | 0.058 |
| Glicoprotein IIb/IIIa inhibitor, n(%) | 701(39.6) | 0.007 | 42(40.1) | 112(31.2) | 0.078 |
| CK MB max, med (IQR) | 2389(1598, 4025) | 0.024 | 1788(952, 4003) | 1673(708, 3054) | 0.102 |
| Troponin max, med (IQR) | 37.5(11.9, 103) | 0.045 | 53(12.6, 119) | 27.4(7.8, 96.2) | 0.219 |
| Hemoglobin at admission g/L, med (IQR) | 141(131, 152) | <0.001 | 141(124, 158) | 150(138, 159) | 0.081 |
| Baseline CKD, n(%) | 282(15.9) | <0.001 | 38(36.9) | 85(23.7) | 0.008 |
| EF, med(IQR) | 44(40, 49) | <0.001 | 40(34, 45) | 42(39, 45) | <0.001 |
| EF<40%, n(%) | 704(39.7) | 66(64.1) | 178(49.7) | <0.001 | |
| EF 40-49%, n(%) | 1065(60.2) | 37(35.9) | 180(50.3) | <0.001 | |
| Therapy at discharge* | |||||
| Beta blockers, n(%) | 1432(80.9) | 0.077 | 60(3.4) | 284(79.3) | 0.085 |
| ACE inhibitors, n(%) | 1349(76.2) | 0.015 | 58(3.3) | 275(76.8) | 0.275 |
| Statin, n(%) | 1430(80.8) | 0,779 | 62(3.5) | 271(75.7) | 0.162 |
| Diuretic, n(%) | 320(18.1) | <0.001 | 25(1.4) | 82(22.9) | 0.080 |
| Calcium antagonist, n(%) | 64(3.6) | 0.589 | 1(0.9) | 13(36.3) | 0.823 |
| Amiodarone, n(%) | 54(3.1) | 0.065 | 1(0.9) | 5(1.4) | 0.934 |
| In-hospital mortality, n(%) | 82(4.6) | <0.001 | 24(23.3) | 24(6.7) | <0.001 |
| No DM N=1769 |
P value | ITDM N=103 |
NITDM N=358 |
P value | |
|---|---|---|---|---|---|
| All-cause death, n(%) | 166(9.4) | <0.001 | 39(37.8) | 47(13.1) | <0.001 |
| MACE, n(%) | 269(15.2) | <0.001 | 42(40.8) | 68(18.9) | <0.001 |
| Cardiovascular death, (%) | 154(8.7) | <0.001 | 36(34.9) | 43(12) | <0.001 |
| Non-fatal recurrent infarction, n(%) | 96(5.5) | 0.943 | 9(8.7) | 18(5.1) | 0.226 |
| TVR, n(%) | 116(6.5) | 0.070 | 19(18.4) | 39(10.9) | 0.607 |
| Non-fatal stroke, n(%) | 23(1.3) | 0.022 | 3(2.9) | 6(1.7) | 0.250 |
| Univariable analysis | Multivariable analysis | |||
| HR (95%CI) | p value | HR (95%CI) | p value | |
| All-cause mortality | ||||
| Age, years | 1.04(1.02-1.06) | <0.001 | 1.05(1.03-1.06) | <0.001 |
| Killip >1 at admission | 2.81(2.11-3.73) | <0.001 | 2.80(2.14-3.62) | <0.001 |
| Postprocedural TIMI<3 | 2.67(1.91-3.96) | <0.001 | 2.61(1.87-3.69) | <0.001 |
| AF at admission | 1.88(1.36-2.59) | <0.001 | 1.84(1.33-2.54) | <0.001 |
| Previous infarction | 1.51(1.06-2.12) | 0.020 | 1.50(1.08-2.16) | 0.016 |
| ITDM | 1.78(1.16-2.35) | 0.008 | 1.72(1.12-2.62) | 0.013 |
| 3-vessel disease | 1.32(1.10-1.89) | 0.051 | ||
| CKD | 1.29(1.10-1.88) | 0.050 | ||
| MACE | ||||
| Age, years | 1.04(1.02-1.06) | <0.001 | 1.02(1.01-1.03) | <0.001 |
| Postprocedural TIMI<3 | 2.19(1.61-2.98) | <0.001 | 2.13(1.57-2.91) | <0.001 |
| Killip >1 at admission | 2.0(1.57-2.54) | <0.001 | 2.0(1.56-2.48) | <0.001 |
| ITDM | 1.59(1.09-2.13) | 0.017 | 1.49(1.01-2.19) | 0.041 |
| Complete AV block at admission | 1.41(1.05-1.52) | 0.022 | 1.36(1.01-1.43) | 0.044 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




