Submitted:
20 April 2024
Posted:
22 April 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Population
2.2. Data Collection
2.3. Statistical Investigations
3. Results
4. Discussion
Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Singer, M.; Deutschman, C.S.; Seymour, C.W.; Shankar-Hari, M.; Annane, D.; Bauer, M.; Bellomo, R.; Bernard, G.R.; Chiche, J.-D.; Coopersmith, C.M.; et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 2016, 315, 801–810. [CrossRef]
- Vincent, J.-L.; Jones, G.; David, S.; Olariu, E.; Cadwell, K.K. Frequency and mortality of septic shock in Europe and North America: a systematic review and meta-analysis. Crit. Care 2019, 23, 1–11. [CrossRef]
- Tsalik, E.L.; Woods, C.W. Sepsis redefined: the search for surrogate markers. Int. J. Antimicrob. Agents 2009, 34, S16–S20. [CrossRef]
- Gullo, A., Intensive and Critical Care Medicine Reflections, Recommendations and Perspectives. 2005: Springer.
- Gunning, K.; Rowan, K. ABC of intensive care: Outcome data and scoring systems. BMJ 1999, 319, 241–244. [CrossRef]
- Kumar, S., et al., Comparison of the performance of APACHE II, SOFA, and mNUTRIC scoring systems in critically ill patients: a 2-year cross-sectional study. Indian Journal of Critical Care Medicine: Peer-reviewed, Official Publication of Indian Society of Critical Care Medicine, 2020. 24(11): p. 1057.
- Xu, X.-l., et al., The role of fibrosis index FIB-4 in predicting liver fibrosis stage and clinical prognosis: A diagnostic or screening tool? Journal of the Formosan Medical Association, 2022. 121(2): p. 454-466.
- Blanco-Grau, A.; Gabriel-Medina, P.; Rodriguez-Algarra, F.; Villena, Y.; Lopez-Martínez, R.; Augustín, S.; Pons, M.; Cruz, L.-M.; Rando-Segura, A.; Enfedaque, B.; et al. Assessing Liver Fibrosis Using the FIB4 Index in the Community Setting. Diagnostics 2021, 11, 2236. [CrossRef]
- Sterling, R.K.; Oakes, T.; Gal, T.S.; Stevens, M.P.; Dewit, M.; Sanyal, A.J. The Fibrosis-4 Index Is Associated With Need for Mechanical Ventilation and 30-Day Mortality in Patients Admitted With Coronavirus Disease 2019. J. Infect. Dis. 2020, 222, 1794–1797. [CrossRef]
- Zhu, X.; Hu, X.; Qin, X.; Pan, J.; Zhou, W. An elevated liver fibrosis index FIB 4 score is associated with poor clinical outcomes in patients with sepsis: an observational cohort study. Pol. Arch. Intern. Med. 2020, 130, 1064–1073. [CrossRef]
- Sumida, Y.; Yoneda, M.; Tokushige, K.; Kawanaka, M.; Fujii, H.; Yoneda, M.; Imajo, K.; Takahashi, H.; Eguchi, Y.; Ono, M.; et al. FIB-4 First in the Diagnostic Algorithm of Metabolic-Dysfunction-Associated Fatty Liver Disease in the Era of the Global Metabodemic. Life 2021, 11, 143. [CrossRef]
- Houot, M.; Ngo, Y.; Munteanu, M.; Marque, S.; Poynard, T. Systematic review with meta-analysis: direct comparisons of biomarkers for the diagnosis of fibrosis in chronic hepatitis C and B. Aliment. Pharmacol. Ther. 2016, 43, 16–29. [CrossRef]
- Parajuli, P.; Sabo, R.; Alsaadawi, R.; Robinson, A.; French, E.; Sterling, R.K. Fibrosis-4 (FIB-4) Index as a Predictor for Mechanical Ventilation and 30-day Mortality Across COVID-19 Variants. J. Clin. Transl. Sci. 2023, 7, 1–25. [CrossRef]
- Park, J.G., et al., Fibrosis-4 index as a predictor for mortality in hospitalised patients with COVID-19: a retrospective multicentre cohort study. BMJ open, 2020. 10(11): p. e041989.
- Demir, N.; Yüzbasıoglu, B.; Calhan, T.; Ozturk, S. Prevalence and Prognostic Importance of High Fibrosis-4 Index in COVID-19 Patients. Int. J. Clin. Pr. 2022, 2022, 1–8. [CrossRef]
- Shibata, N.; Kondo, T.; Kazama, S.; Kimura, Y.; Oishi, H.; Arao, Y.; Kato, H.; Yamaguchi, S.; Kuwayama, T.; Hiraiwa, H.; et al. Impact of predictive value of Fibrosis-4 index in patients hospitalized for acute heart failure. Int. J. Cardiol. 2021, 324, 90–95. [CrossRef]
- Pranata, R.; Yonas, E.; Huang, I.; Lim, M.A.; Nasution, S.A.; Kuswardhani, R.A.T. Fibrosis-4 index and mortality in coronavirus disease 2019: a meta-analysis. Eur. J. Gastroenterol. Hepatol. 2021, 33, e368–e374. [CrossRef]
- Maeda, D.; Kanzaki, Y.; Sakane, K.; Tsuda, K.; Akamatsu, K.; Hourai, R.; Okuno, T.; Tokura, D.; Nakayama, S.; Hasegawa, H.; et al. Prognostic value of the liver fibrosis marker fibrosis-5 index in patients with acute heart failure. ESC Hear. Fail. 2022, 9, 1380–1387. [CrossRef]
- Font, M.D.; Thyagarajan, B.; Khanna, A.K. Sepsis and Septic Shock – Basics of diagnosis, pathophysiology and clinical decision making. Med Clin. North Am. 2020, 104, 573–585. [CrossRef]
- Li, Y., et al., Liver fibrosis index FIB-4 is associated with mortality in COVID-19. Hepatology communications, 2021. 5(3): p. 434-445.
- Peleg, N.; Issachar, A.; Sneh-Arbib, O.; Shlomai, A. AST to Platelet Ratio Index and fibrosis 4 calculator scores for non-invasive assessment of hepatic fibrosis in patients with non-alcoholic fatty liver disease. Dig. Liver Dis. 2017, 49, 1133–1138. [CrossRef]
| n (%) | ||
|---|---|---|
| Gender | Female | 130 (42.1) |
| Male | 179 (57.9) | |
| Age | Mean±Ss | 74.78±13.92 |
| Median (Min-Max) | 77 (27-98) | |
| ºComorbidity | HT | 214 (69.3) |
| DM | 90 (29.1) | |
| CKD | 117 (37.9) | |
| CVD | 48 (15.5) | |
| CAD | 102 (33.0) | |
| Nasocomial infection | No | 84 (27.2) |
| Yes | 225 (72.8) | |
| Septic shock | No | 204 (66.0) |
| There is | 105 (34.0) | |
| ºBreeding place | Blood | 124 (40.1) |
| Catheter | 21 (6.8) | |
| Tracheal aspirate culture/ Phlegm | 112 (36.2) | |
| Urine | 93 (30.1) | |
| Wound site | 20 (6.5) | |
| Other (pleural fluid.,peritoneum, etc.) | 4 (1.3) | |
| ºEffective | Acineto | 20 (6.5) |
| Klebsiella | 44 (14.2) | |
| Pseudomonas | 46 (14.9) | |
| E.coli | 96 (31.1) | |
| Enterococcus | 34 (11.0) | |
| MRSA | 10 (3,2) | |
| MSSA | 15 (4,9) | |
| Candida | 17 (5,5) | |
| Other | 33 (10,7) | |
| 28-day mortality | Survival | 167 (54,0) |
| Non-survival | 142 (46,0) |
| 28-Day Mortality | p | |||
|---|---|---|---|---|
| Survival (n=167) | Non-Survival (n=142) | |||
| Gender | Woman | 67 (40.1) | 63 (44.4) | a0.451 |
| Male | 100 (59.9) | 79 (55.6) | ||
| Comorbidity | HT | 119 (71.3) | 95 (66.9) | a0.408 |
| DM | 59 (35.3) | 31 (21.8) | a0.009** | |
| CKD | 66 (39.5) | 51 (35.9) | a0.515 | |
| CVD | 32 (19.2) | 16 (11.3) | a0.056 | |
| CAD | 60 (35.9) | 42 (29.6) | a0.237 | |
| Nasocomial | No | 39 (23.4) | 45 (31.7) | a0.101 |
| Yes | 128 (76.6) | 97 (68.3) | ||
| Septic shock | No | 93 (55.7) | 111 (78.2) | a0.001** |
| Yes | 74 (44.3) | 31 (21.8) | ||
|
Place of reproduction Blood |
0.65 (38.9) | 59 (41.5) | a0.639 | |
| Catheter | 11 (6.6) | 10 (7.0) | a0.874 | |
| TAC / Phlegm | 58 (34.7) | 54 (38.0) | a0.548 | |
| Urine | 47 (28.1) | 46 (32.4) | a0.417 | |
| Wound site | 17 (10.2) | 3 (2.1) | a0.004** | |
| Other (pleural fluid. peritoneum. etc.) | 2 (1.2) | 2 (1.4) | b1.000 | |
| Agent | Acinetobacter | 10(6) | 10(7) | a0.707 |
| Kleasiella | 22(13.2) | 22(15.5) | a0.561 | |
| Pseudomonas | 25(15.0) | 21(14.8) | a0.964 | |
| E.coli | 57(34.1) | 39(27.5) | a0.207 | |
| Enterococcus | 17(10.2) | 17(12.0) | a0.616 | |
| MRSA | 4(2.4) | 6(4.2) | b0.522 | |
| MSSA | 8(4.8) | 7(4.9) | a0.955 | |
| Candida | 8(4,8) | 9(6,3) | a0,552 | |
| Other | 17(10,2) | 16(11,3) | a0,758 | |
| Total | 28-Day Mortality | p | |||
|---|---|---|---|---|---|
| Survival (n=167) | Non- Survival (n=142) | ||||
| Age | Mean±Ss | 74.78±13.92 | 73.85±14.21 | 75.87±13.54 | c0.189 |
| Median (Min-Max) | 77 (27-98) | 77 (27-98) | 78 (32-98) | ||
| APAPCHE II | Mean±Ss | 30.99±6.43 | 28.75±5.98 | 33.63±5.94 | d0.001** |
| Median (Min-Max) | 30 (15-51) | 28 (15-46) | 33 (18-51) | ||
| SOFA | Mean±Ss | 9.17±2.93 | 8.20±2.70 | 10.32±2.77 | d0.001** |
| Median (Min-Max) | 9 (1-17) | 8 (2-17) | 10 (1-17) | ||
| Lactate | Mean±Ss | 3.32±2.54 | 2.89±1.95 | 3.83±3.01 | c0.001** |
| Median (Min-Max) | 2.4 (1.4-24) | 2.3 (1.4-18) | 2.8 (1.6-24) | ||
| AST | Mean±Ss | 96.57±181.19 | 76.58±154.54 | 120.08±206.31 | c0.011* |
| Median (Min-Max) | 39 (6-1572) | 35 (8-1572) | 46.5 (6-1185) | ||
| ALT | Mean±Ss | 55.36±114.46 | 46.49±96.48 | 65.8±132.12 | c0.252 |
| Median (Min-Max) | 19 (2-849) | 18 (2-753) | 20 (5-849) | ||
| Total bilirubin | Mean±Ss | 1.60±3.52 | 0.99±1.53 | 2.30±4.83 | c0.001** |
| Median (Min-Max) | 0.7 (0.1-29.6) | 0.6 (0.1-14.4) | 0.8 (0.2-29.6) | ||
| Direct bilirubin | Mean±Ss | 1.14±2.92 | 0.63±1.32 | 1.74±3.98 | c0.001** |
| Median (Min-Max) | 0.3 (0.1-22.4) | 0.3 (0.1-12.1) | 0.4 (0.1-22.4) | ||
| Urea | Mean±Ss | 121.32±76.9 | 110.57±76.62 | 133.95±75.55 | c0.001** |
| Median (Min-Max) | 103 (14-494) | 90 (14-494) | 117.5 (19-404) | ||
| Creatinine | Mean±Ss | 2.65±1.86 | 2.59±2.04 | 2.73±1.63 | c0.087 |
| Median (Min-Max) | 2.2 (0.3-10.8) | 2 (0.3-10.8) | 2.4 (0.3-7.7) | ||
| FIB-4 | Mean±Ss | 6.49±7.89 | 4.83±6.37 | 8.44±9.02 | c0.001** |
| Median (Min-Max) | 3.8 (0.3-54.6) | 3.3 (0.3-54.6) | 5.3 (0.4-45) | ||
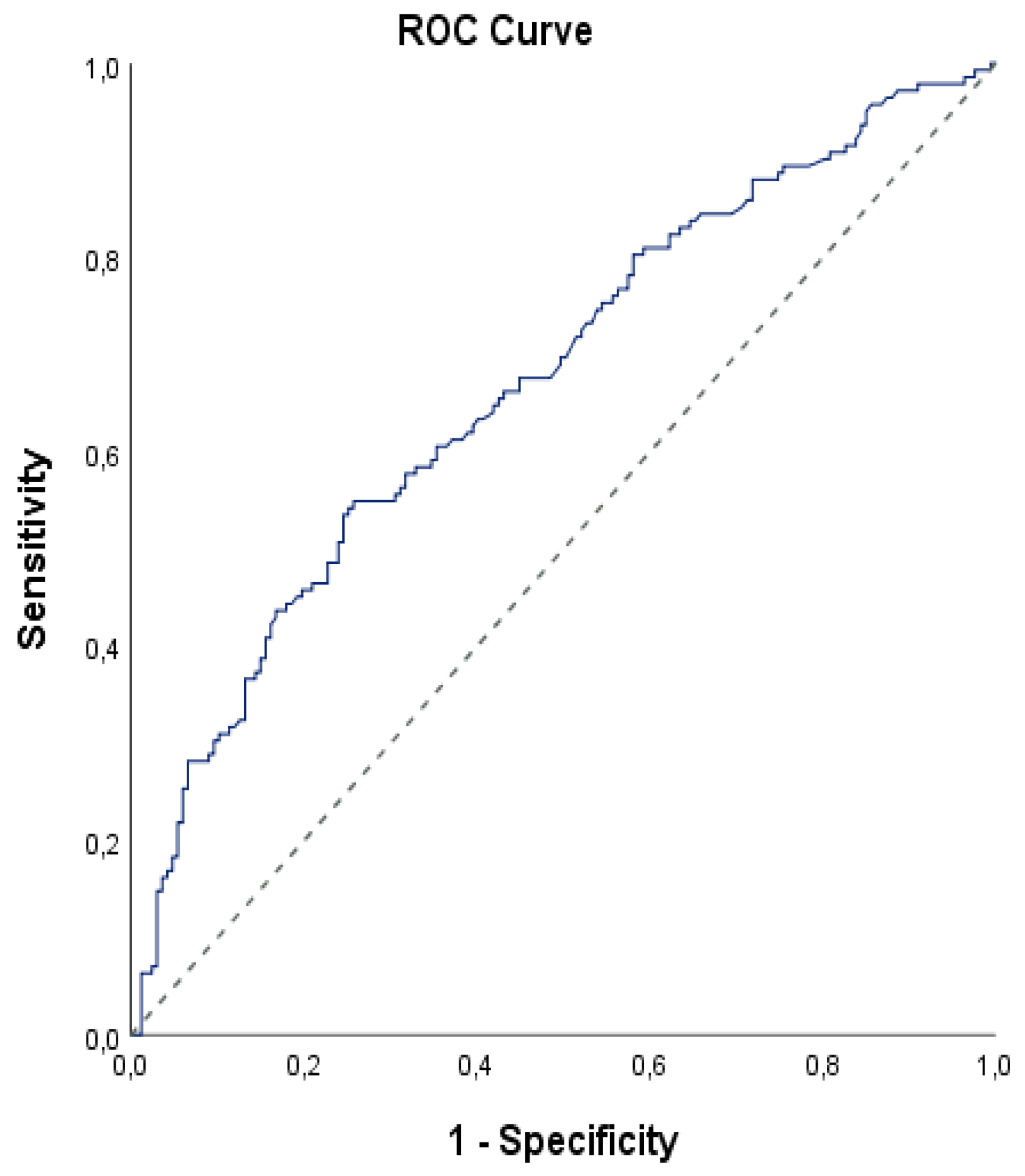
| Diagnostic Scan | ROC Curve | p | ||||||
|---|---|---|---|---|---|---|---|---|
| cut -off | sensitivity | specificity | Positive Predictive Value | Negative predictive Value |
Area | 95% Confidence Interval |
||
| FIB-4 | 4.9 | 4.92 | 4.25 | 4.46 | 4.95 | 0.672 | 0.612-0.732 | 0.001** |
| p | ODDS | 95% C.I.ODDS | ||
|---|---|---|---|---|
| Lower | Upper | |||
| DM(+) | 0.105 | 0.606 | 0.331 | 1.110 |
| Septic shock(+) | 0.528 | 0.810 | 0.421 | 1.558 |
| Wound site infection | 0.058 | 0.258 | 0.064 | 1.045 |
| Lactate | 0.519 | 1.043 | 0.918 | 1.184 |
| AST | 0.775 | 1.000 | 0.998 | 1.001 |
| Total Bilirubin | 0.680 | 0.872 | 0.456 | 1.669 |
| Urea | 0.695 | 0.999 | 0.995 | 1.003 |
| APAPCHEII | 0.000** | 1.101 | 1.008 | 1.156 |
| SOFA | 0.037* | 1.122 | 1.007 | 1.251 |
| Direct Bilirubin | 0.042* | 1.228 | 1.080 | 1.497 |
| FIB-4(≥ 4.9) | 0.006** | 2.127 | 1.237 | 3.659 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




