Submitted:
18 April 2024
Posted:
19 April 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methods and Data
2.1. Sampling Techniques and Sample Size
2.2. Variables Definitions
2.3. Independent Variables and Rationale
2.4. Model Specification
2.5. Data Analysis
- In view of the hierarchical nature of the data sets, coupled with the ordinal classifications of the outcome variable, a three-level mixed effect ordinal logistic regression (MMEOLR) was used to determine the significance of the predictors, such that individual variables at level 1 are nested in the community at level 2 and are nested in the state at level 3. The three-level model was found to be more appropriate than the two-level model or a single-level by the application of likelihood ratio test (the likelihood-ratio test for Level-2 nested in Level-3). The results here are displayed on the supplementary file.
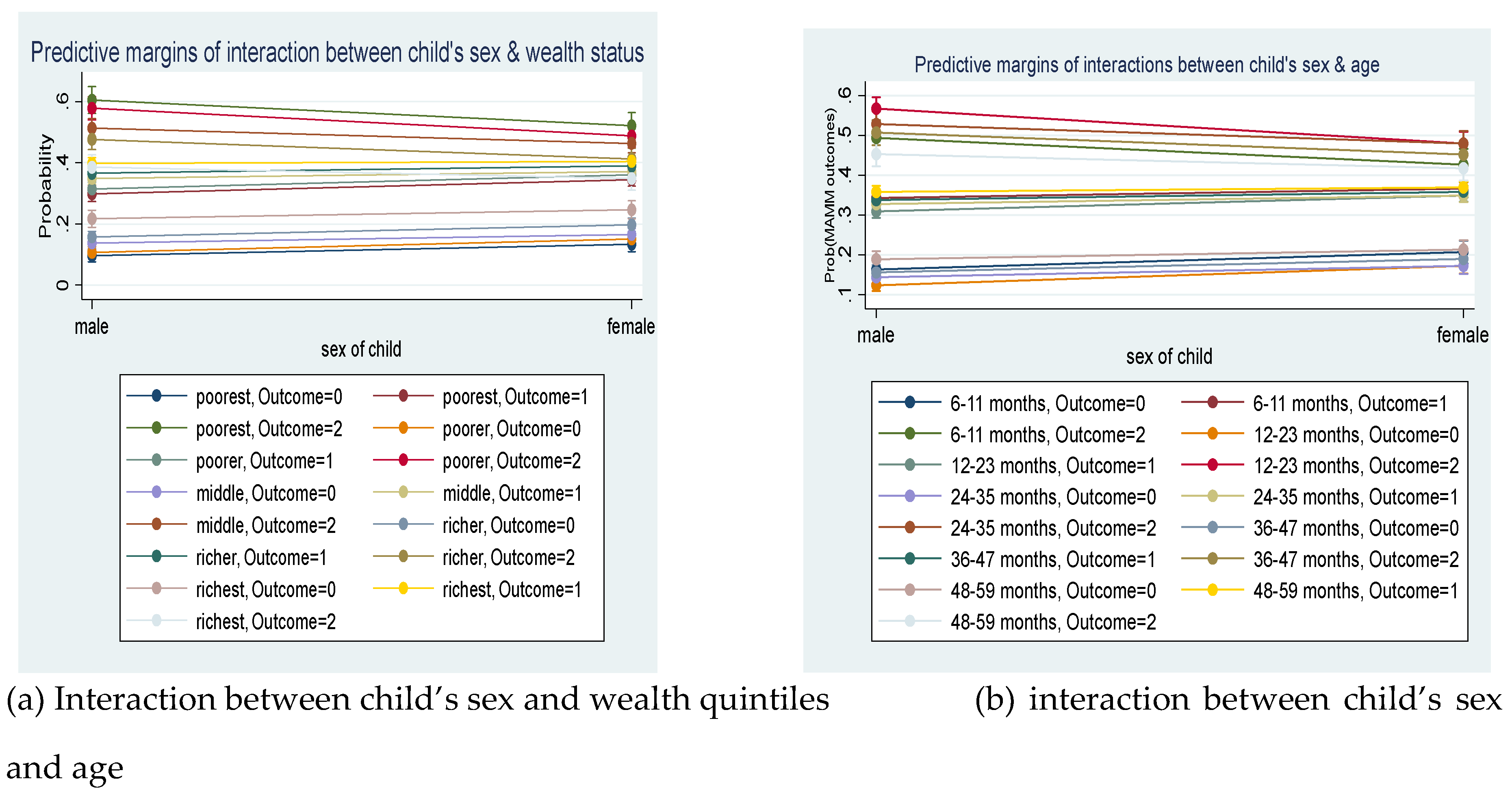
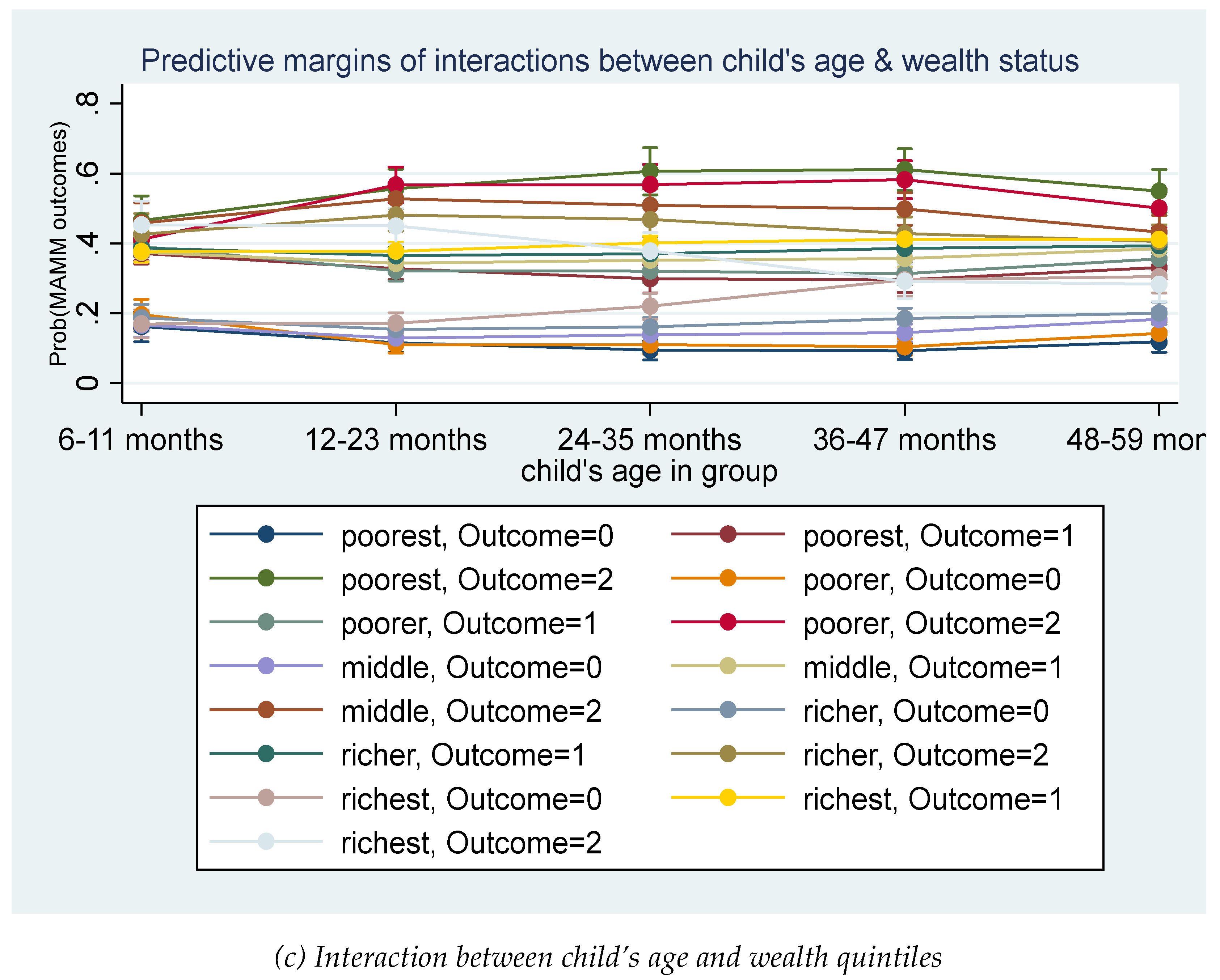
- To better understand the associations of the intersecting independent variables, interaction plots (Dawson, 2014) were drawn for each intersection.
3. Results
3.1. Model Comparison and Fit
3.2. Accounting for the Intersections
4. Discussion
5. Conclusion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Obasohan, P.E. Investigating Multiple Overlaps in the Determinants of Risk Factors of Anaemia, Malaria, and Malnutrition, and Their Multimorbidity, among Children Aged 6 to 59 Months in Nigeria. phd, University of Sheffield, 2022.
- Obasohan, P.E.; Walters, S.J.; Jacques, R.; Khatab, K. Individual, Household and Area Predictors of Anaemia among Children Aged 6–59 Months in Nigeria. Public Health Pract. 2022, 3, 100229. [Google Scholar] [CrossRef] [PubMed]
- Obasohan, P.E.; Walters, S.J.; Jacques, R.; Khatab, K. Individual and Contextual Factors Associated with Malaria among Children 6–59 Months in Nigeria: A Multilevel Mixed Effect Logistic Model Approach. Int. J. Environ. Res. Public. Health 2021, 18, 11234. [Google Scholar] [CrossRef] [PubMed]
- Obasohan, P.E.; Walters, S.J.; Jacques, R.; Khatab, K. Socio-Economic, Demographic, and Contextual Predictors of Malnutrition among Children Aged 6–59 Months in Nigeria | BMC Nutrition | Full Text. BMC Nutr. 2024, 10. [Google Scholar] [CrossRef] [PubMed]
- Hailu, B.A.; Bogale, G.G.; Beyene, J. Spatial Heterogeneity and Factors Influencing Stunting and Severe Stunting among Under-5 Children in Ethiopia: Spatial and Multilevel Analysis. Sci. Rep. 2020, 10, 16427. [Google Scholar] [CrossRef]
- Kassie, G.W.; Workie, D.L. Determinants of Under-Nutrition among Children under Five Years of Age in Ethiopia. BMC Public Health 2020, 20, 399. [Google Scholar] [CrossRef] [PubMed]
- Khamis, A.G.; Mwanri, A.W.; Kreppel, K.; Kwesigabo, G. The Burden and Correlates of Childhood Undernutrition in Tanzania According to Composite Index of Anthropometric Failure. BMC Nutr. 2020, 6, 39. [Google Scholar] [CrossRef]
- Douglas, A.C. Influence of Malaria on Anemia Levels among Children Less than 60 Months of Age. Int. J. Adv. Res. Dev. 2, 5.
- Dwumoh, D.; Essuman, E.E.; Afagbedzi, S.K. Determinant of Factors Associated with Child Health Outcomes and Service Utilization in Ghana: Multiple Indicator Cluster Survey Conducted in 2011 | Archives of Public Health | Full Text. Available online: https://archpublichealth.biomedcentral.com/articles/10.1186/2049-3258-72-42 (accessed on 22 March 2024).
- Mohammed, S.H.; Habtewold, T.D.; Esmaillzadeh, A. Household, Maternal, and Child Related Determinants of Hemoglobin Levels of Ethiopian Children: Hierarchical Regression Analysis. BMC Pediatr. 2019, 19, 113. [Google Scholar] [CrossRef]
- Moschovis, P.P.; Wiens, M.O.; Arlington, L.; Antsygina, O.; Hayden, D.; Dzik, W.; Kiwanuka, J.P.; Christiani, D.C.; Hibberd, P.L. Individual, Maternal and Household Risk Factors for Anaemia among Young Children in Sub-Saharan Africa: A Cross-Sectional Study. BMJ Open 2018, 8, e019654. [Google Scholar] [CrossRef]
- Ntenda, P.A.M.; Chilumpha, S.; Mwenyenkulu, E.T.; Kazambwe, J.F.; El-Meidany, W. Clinical Malaria and the Potential Risk of Anaemia among Preschool-Aged Children: A Population-Based Study of the 2015–2016 Malawi Micronutrient Survey | Infectious Diseases of Poverty | Full Text. Available online: https://idpjournal.biomedcentral.com/articles/10.1186/s40249-019-0607-8 (accessed on 22 March 2024).
- Ojoniyi, O.O.; Odimegwu, C.O.; Olamijuwon, E.O.; Akinyemi, J.O. Does Education Offset the Effect of Maternal Disadvantage on Childhood Anaemia in Tanzania? Evidence from a Nationally Representative Cross-Sectional Study. BMC Pediatr. 2019, 19, N.PAG-N.PAG. [Google Scholar] [CrossRef]
- Ngnie-Teta, I.; Receveur, O.; Kuate-Defo, B. Risk Factors for Moderate to Severe Anemia among Children in Benin and Mali: Insights from a Multilevel Analysis. Food Nutr. Bull. 2007, 28, 76–89. [Google Scholar] [CrossRef] [PubMed]
- Austin, A.M.; Fawzi, W.; Hill, A.G. Anaemia among Egyptian Children between 2000 and 2005: Trends and Predictors. Matern. Child. Nutr. 2011, 8, 522–532. [Google Scholar] [CrossRef]
- Wanzira, H.; Katamba, H.; Okullo, A.E.; Agaba, B.; Kasule, M.; Rubahika, D. Factors Associated with Malaria Parasitaemia among Children under 5 Years in Uganda: A Secondary Data Analysis of the 2014 Malaria Indicator Survey Dataset. Malar. J. 2017, 16, 191. [Google Scholar] [CrossRef]
- Zgambo, M.; Mbakaya, B.C.; Kalembo, F.W. Prevalence and Factors Associated with Malaria Parasitaemia in Children under the Age of Five Years in Malawi: A Comparison Study of the 2012 and 2014 Malaria Indicator Surveys (MISs) | PLOS ONE. Available online: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0175537 (accessed on 22 March 2024).
- Amare, Z.Y.; Ahmed, M.E.; Mehari, A.B. Determinants of Nutritional Status among Children under Age 5 in Ethiopia: Further Analysis of the 2016 Ethiopia Demographic and Health Survey. Glob. Health 2019, 15, 62. [Google Scholar] [CrossRef] [PubMed]
- Fantay Gebru, K.; Mekonnen Haileselassie, W.; Haftom Temesgen, A.; Oumer Seid, A.; Afework Mulugeta, B. Determinants of Stunting among Under-Five Children in Ethiopia: A Multilevel Mixed-Effects Analysis of 2016 Ethiopian Demographic and Health Survey Data. BMC Pediatr. 2019, 19, 176. [Google Scholar] [CrossRef] [PubMed]
- Geda, N.R.; Feng, C.X.; Henry, C.J.; Lepnurm, R.; Janzen, B.; Whiting, S.J. Multiple Anthropometric and Nutritional Deficiencies in Young Children in Ethiopia: A Multi-Level Analysis Based on a Nationally Representative Data. BMC Pediatr. 2021, 21, 11. [Google Scholar] [CrossRef]
- Tran, T.D.; Biggs, B.-A.; Holton, S.; Nguyen, H.T.M.; Hanieh, S.; Fisher, J. Co-Morbid Anaemia and Stunting among Children of Pre-School Age in Low- and Middle-Income Countries: A Syndemic. Public Health Nutr. 2019, 22, 35–43. [Google Scholar] [CrossRef]
- Chitunhu, S.; Musenge, E. Direct and Indirect Determinants of Childhood Malaria Morbidity in Malawi: A Survey Cross-Sectional Analysis Based on Malaria Indicator Survey Data for 2012. Malar. J. 2015, 14, 265. [Google Scholar] [CrossRef] [PubMed]
- Adekanmbi, V.T.; Kayode, G.A.; Uthman, O.A. Individual and Contextual Factors Associated with Childhood Stunting in Nigeria: A Multilevel Analysis. Matern. Child. Nutr. 2011, 9, 244–259. [Google Scholar] [CrossRef]
- Machisa, M.; Wichmann, J.; Nyasulu, P.S. Biomass Fuel Use for Household Cooking in Swaziland: Is There an Association with Anaemia and Stunting in Children Aged 6-36 Months? Trans. R. Soc. Trop. Med. Hyg. 2013, 107, 535–544. [Google Scholar] [CrossRef]
- Mulatya, D.M.; Mutuku, F.W. Assessing Comorbidity of Diarrhea and Acute Respiratory Infections in Children Under 5 Years: Evidence From Kenya’s Demographic Health Survey 2014. J. Prim. Care Community Health 2020, 11, 2150132720925190. [Google Scholar] [CrossRef] [PubMed]
- Hartnell, S.J. Intersections of Gender, Ethnicity, and Socioeconomic Position in Health in England: A Mixed Methods Study Available online: https://etheses.whiterose.ac.uk/cgi/search/simple?q=ScHARR&_action_search=&_order=bytitle&basic_srchtype=ALL&_satisfyall=ALL.
- Dawson, J.F. Moderation in Management Research: What, Why, When, and How. J. Bus. Psychol. 2014, 29, 1–19. [Google Scholar] [CrossRef]
- Adedokun, S.T. Correlates of Childhood Morbidity in Nigeria: Evidence from Ordinal Analysis of Cross-Sectional Data. PLOS ONE 2020, 15, e0233259. [Google Scholar] [CrossRef] [PubMed]
- National Population Commission (NPC)[Nigeria]; ICF Nigeria Demographic and Health Survey 2018 2019.
- TheCable Rescuing the Nigerian Middle Class. Available online: https://www.thecable.ng/rescuing-the-nigerian-middle-class (accessed on 10 March 2024).
- The Stata Forum Interpretation of Interaction Term Coefficients of an Ordinal Logistic Regression. - Statalist. Available online: https://www.statalist.org/forums/forum/general-stata-discussion/general/1409237-interpretation-of-interaction-term-coefficients-of-an-ordinal-logistic-regression (accessed on 22 March 2024).
- Williams, R. Adjusted Predictions & Marginal Effects for Multiple Outcome Models & Commands (Including Ologit, Mlogit, Oglm, & Gologit2). 2021, 10.
- Williams, R. Interpreting Interaction Effects; Interaction Effects and Centering. 2021, available at: https://www3.nd.edu/~rwilliam/, 8.
- Moran, M. Statistical Interaction: More than the Sum of Its Parts. Available online: https://www.statisticssolutions.com/statistical-interaction-more-than-the-sum-of-its-parts/ (accessed on 17 August 2022).
- Obasohan, P. Religion, Ethnicity and Contraceptive Use among Reproductive Age Women in Nigeria. Int. J. MCH AIDS IJMA 2014, 3. [Google Scholar] [CrossRef]
- Academy of Medical Science Multimorbidity: A Priority for Global Health Research Overview and Key Messages 2018.
| Multimorbidity | Chi-square | ||||
|---|---|---|---|---|---|
| Variables | Total | None of the diseases | One disease only | Two or more the diseases | |
| n(%) | n(%) | n(%) | n(%) | ||
| Child’s sex | χ2 (2) = 25.03, p=0.0002 | ||||
| Male | 5217(51.23) | 841(16.13) | 1734(33.25) | 2641(50.62) | |
| Female | 4967(48.77) | 926(18.64) | 1764(35.52) | 2277(45.84) | |
| Child’s age in group | χ2 (8) = 205.55, p<0.0001 | ||||
| 6-11 months | 1232(12.1) | 165(13.35) | 566(45.91) | 502(40.74) | |
| 12-23 months | 2422(23.78) | 289(11.95) | 888(36.66) | 1245(51.39) | |
| 24-35 months | 2160(21.21) | 363(16.82) | 694(32.13) | 1102(51.05) | |
| 36-47 months | 2227(21.87) | 452(20.32) | 664(29.83) | 1110(49.85) | |
| 48-59 months | 2143(21.04) | 498(23.23) | 687(32.06) | 958(44.71) | |
| Household wealth index | χ2 (8) = 1635.53, P<0.0001 | ||||
| Poorest | 1893(18.59) | 109(5.73) | 392(20.7) | 1393(73.57) | |
| Poorer | 1989(19.53) | 166(8.33) | 555(27.9) | 1268(63.77) | |
| Middle | 2139(21) | 328(15.35) | 753(35.19) | 1058(49.46) | |
| Richer | 2144(21.05) | 445(20.75) | 876(40.85) | 823(38.4) | |
| Richest | 2019(19.83) | 720(35.66) | 924(45.75) | 376(18.6) | |
| MAMM status | 10184(100) | 1767(17.35) | 3499(34.36) | 4918(48.29) | |
| Model | Number of covariates | Log-likelihood | AIC | BIC |
|---|---|---|---|---|
| Model 1 | Child’s sex * wealth status + all the covariates | -6933.6 | 14015.1 | 14530.2 |
| Model 2 | Child’s sex * age + all the covariates | -6933.4 | 14014.8 | 14529.9 |
| Model 3 | Child’s age * wealth status + all the covariates | -6902.6 | 13977.3 | 14575.9 |
| Model 4 | Child’s sex * wealth status + child’s sex * age + child’s age * wealth status + all the covariates | -6898.5 | 13985.03 | 14639.4 |
| Model 5 | Child’s sex * age * wealth status + all the covariates | -6890.8 | 14001.6 | 14767.4 |
| Disease classification | Age (Months) | Household wealth status | ||||
| Poorest | Poorer | Middle | Richer | Richest | ||
| None of the disease | 06-11 | 0.162 | 0.196 | 0.166 | 0.187 | 0.17 |
| 11-23 | 0.116 | 0.111 | 0.129 | 0.153 | 0.172 | |
| 23-35 | 0.094 | 0.11 | 0.138 | 0.161 | 0.22 | |
| 35-47 | 0.092 | 0.104 | 0.144 | 0.185 | 0.296 | |
| 47-59 | 0.119 | 0.143 | 0.182 | 0.201 | 0.305 | |
| One disease only | 06-11 | 0.372 | 0.392 | 0.375 | 0.387 | 0.377 |
| 11-23 | 0.328 | 0.322 | 0.343 | 0.365 | 0.378 | |
| 23-35 | 0.299 | 0.321 | 0.352 | 0.371 | 0.401 | |
| 35-47 | 0.296 | 0.313 | 0.357 | 0.386 | 0.412 | |
| 47-59 | 0.331 | 0.356 | 0.385 | 0.394 | 0.412 | |
| Two or more diseases | 06-11 | 0.466 | 0.412 | 0.459 | 0.426 | 0.454 |
| 11-23 | 0.557 | 0.568 | 0.528 | 0.482 | 0.45 | |
| 23-35 | 0.607 | 0.569 | 0.509 | 0.468 | 0.378 | |
| 35-47 | 0.612 | 0.583 | 0.499 | 0.429 | 0.292 | |
| 47-59 | 0.55 | 0.501 | 0.433 | 0.406 | 0.283 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




