Submitted:
23 March 2024
Posted:
25 March 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Characterization of the Sample
2.3. Instruments
2.4. Tasks, Procedures, and Protocols
2.5. Variables
- - Clinical Data: Comorbidities associated with obesity (diabetes, hypertension, dyslipidemia and OSAS);
- - Questionnaires: Quality of life, satisfaction with telemedicine monitoring and perception of sleep quality;
- - Other variables: Gender, age, weight, body mass index.
2.6. Statistical Treatment
2.7. Ethical Considerations
3. Results
4. Discussion
5. Limitation
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Public Involvement Statement
Guidelines and Standards Statement
Conflicts of Interest
References
- Perez-Campos, E.; Mayoral, L.P.-C.; Andrade, G.M.; Mayoral, E.P.-C.; Huerta, T.H.; Canseco, S.P.; Canales, F.J.R.; Cabrera-Fuentes, H.A.; Cruz, M.M.; Santiago, A.D.P.; et al. Obesity subtypes, related biomarkers & heterogeneity. Indian J. Med Res. 2020, 151, 11–21. [Google Scholar] [CrossRef]
- Mechanick, J.I.; Youdim, A.; Jones, D.B.; Garvey, W.T.; Hurley, D.L.; McMahon, M.M.; Heinberg, L.J.; Kushner, R.; Adams, T.D.; Shikora, S.; et al. Clinical Practice Guidelines for the Perioperative Nutritional, Metabolic, and Nonsurgical Support of the Bariatric Surgery Patient—2013 Update: Cosponsored by American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic & Bariatric Surgery. Surg. Obes. Relat. Dis. 2013, 9, 159–191. [Google Scholar] [CrossRef]
- Hruby, A.; Manson, J.E.; Qi, L.; Malik, V.S.; Rimm, E.B.; Sun, Q.; Willett, W.C.; Hu, F.B. Determinants and Consequences of Obesity. Am. J. Public Health 2016, 106, 1656–1662. [Google Scholar] [CrossRef]
- Rozier, M.D.; Ghaferi, A.A.; Rose, A.; Simon, N.-J.; Birkmeyer, N.; Prosser, L.A. Patient Preferences for Bariatric Surgery: Findings From a Survey Using Discrete Choice Experiment Methodology. JAMA Surg. 2019, 154, e184375–e184375. [Google Scholar] [CrossRef]
- Spaniolas, K.; Kasten, K.R.; Celio, A.; Burruss, M.B.; Pories, W.J. Postoperative Follow-up After Bariatric Surgery: Effect on Weight Loss. Obes. Surg. 2016, 26, 900–903. [Google Scholar] [CrossRef] [PubMed]
- Mechanick, J.I.; Apovian, C.; Brethauer, S.; Garvey, W.T.; Joffe, A.M.; Kim, J.; Kushner, R.F.; Lindquist, R.; Pessah-Pollack, R.; Seger, J.; et al. Clinical practice guidelines for the perioperative nutrition, metabolic, and nonsurgical support of patients undergoing bariatric procedures – 2019 update: cosponsored by American Association of Clinical Endocrinologists/American College of Endocrinology, The Obesity Society, American Society for Metabolic & Bariatric Surgery, Obesity Medicine Association, and American Society of Anesthesiologists. Surg. Obes. Relat. Dis. 2019, 16, 175–247. [Google Scholar] [CrossRef]
- Santos, C.; Carvalho, M.; Oliveira, L.; Palmeira, A.; Rodrigues, L.M.; Gregório, J. The Long-Term Association between Physical Activity and Weight Regain, Metabolic Risk Factors, Quality of Life and Sleep after Bariatric Surgery. Int. J. Environ. Res. Public Heal. 2022, 19, 8328. [Google Scholar] [CrossRef]
- Raoof, M.; Näslund, I.; Rask, E.; Karlsson, J.; Sundbom, M.; Edholm, D.; Karlsson, F.A.; Svensson, F.; Szabo, E. Health-Related Quality-of-Life (HRQoL) on an Average of 12 Years After Gastric Bypass Surgery. Obes. Surg. 2015, 25, 1119–1127. [Google Scholar] [CrossRef] [PubMed]
- Mead, N.; Bower, P. Patient-centredness: a conceptual framework and review of the empirical literature. Soc. Sci. Med. 2000, 51, 1087–1110. [Google Scholar] [CrossRef] [PubMed]
- Kwame, A.; Petrucka, P.M. A literature-based study of patient-centered care and communication in nurse-patient interactions: barriers, facilitators, and the way forward. BMC Nurs. 2021, 20, 1–10. [Google Scholar] [CrossRef]
- Camolas, J.; Santos, O.; Moreira, P.; Carmo, I.D. INDIVIDUO: Results from a patient-centered lifestyle intervention for obesity surgery candidates. Obes. Res. Clin. Pr. 2017, 11, 475–488. [Google Scholar] [CrossRef]
- Goretti, G.; Marinari, G.M.; Vanni, E.; Ferrari, C. Value-Based Healthcare and Enhanced Recovery After Surgery Implementation in a High-Volume Bariatric Center in Italy. Obes. Surg. 2020, 30, 2519–2527. [Google Scholar] [CrossRef]
- Fastenau, J.; Kolotkin, R.L.; Fujioka, K.; Alba, M.; Canovatchel, W.; Traina, S. A call to action to inform patient-centred approaches to obesity management: Development of a disease-illness model. Clin. Obes. 2019, 9, e12309. [Google Scholar] [CrossRef] [PubMed]
- Das, A.; Faxvaag, A.; Svanæs, D. The Impact of an eHealth Portal on Health Care Professionals’ Interaction with Patients: Qualitative Study. J. Med Internet Res. 2015, 17, e267. [Google Scholar] [CrossRef]
- Wright, C.; Mutsekwa, R.N.; Hamilton, K.; Campbell, K.L.; Kelly, J. Are eHealth interventions for adults who are scheduled for or have undergone bariatric surgery as effective as usual care? A systematic review. Surg. Obes. Relat. Dis. 2021, 17, 2065–2080. [Google Scholar] [CrossRef] [PubMed]
- Mangieri, C.W.; Johnson, R.J.; Sweeney, L.B.; Choi, Y.U.; Wood, J.C. Mobile health applications enhance weight loss efficacy following bariatric surgery. Obes. Res. Clin. Pr. 2019, 13, 176–179. [Google Scholar] [CrossRef] [PubMed]
- Newell, S.; Jordan, Z. The patient experience of patient-centered communication with nurses in the hospital setting: a qualitative systematic review protocol. JBI Évid. Synth. 2015, 13, 76–87. [Google Scholar] [CrossRef] [PubMed]
- S. André and P. Ribeiro, “E-health: as TIC como mecanismo de evolução em saúde,” Gestão e Desenvolvimento, vol. 28, no. 28, pp. 95–116, Jul. 2020. [CrossRef]
- de Queiroz, C.; Sallet, J.A.; Silva, P.G.M.D.B.E.; Queiroz, L.d.G.P.d.S.; Pimentel, J.A.; Sallet, P.C. Application of BAROS’ questionnaire in obese patients undergoing bariatric surgery with 2 years of evolution. Arq. de Gastroenterol. 2017, 54, 60–64. [Google Scholar] [CrossRef]
- Maciel, J.; Infante, P.; Ribeiro, S.; Ferreira, A.; Silva, A.C.; Caravana, J.; Carvalho, M.G. Translation, Adaptation and Validation of a Portuguese Version of the Moorehead-Ardelt Quality of Life Questionnaire II. Obes. Surg. 2014, 24, 1940–1946. [Google Scholar] [CrossRef]
- João, K.A.D.R.; Becker, N.B.; Jesus, S.d.N.; Martins, R.I.S. Validation of the Portuguese version of the Pittsburgh Sleep Quality Index (PSQI-PT). Psychiatry Res. 2017, 247, 225–229. [Google Scholar] [CrossRef]
- Abecasis, F.; Interna, H.G.d.O.S.d.M. Consulta Telefónica em Contexto Pandémico: Avaliação da Satisfação dos Doentes. Med. Interna 2021, 28, 250–256. [Google Scholar] [CrossRef]
- Jassil, F.C.; Richards, R.; Carnemolla, A.; Lewis, N.; Montagut-Pino, G.; Kingett, H.; Doyle, J.; Kirk, A.; Brown, A.; Chaiyasoot, K.; et al. Patients' views and experiences of live supervised tele-exercise classes following bariatric surgery during the COVID-19 pandemic: The BARI-LIFESTYLE qualitative study. Clin. Obes. 2021, 12, e12499. [Google Scholar] [CrossRef]
- Sockalingam, S.; Leung, S.E.; Ma, C.; Hawa, R.; Wnuk, S.; Dash, S.; Jackson, T.; Cassin, S.E. The Impact of Telephone-Based Cognitive Behavioral Therapy on Mental Health Distress and Disordered Eating Among Bariatric Surgery Patients During COVID-19: Preliminary Results from a Multisite Randomized Controlled Trial. Obes. Surg. 2022, 32, 1884–1894. [Google Scholar] [CrossRef]
- Wang, C.D.; Rajaratnam, T.; Stall, B.; Hawa, R.; Sockalingam, S. Exploring the Effects of Telemedicine on Bariatric Surgery Follow-up: a Matched Case Control Study. Obes. Surg. 2019, 29, 2704–2706. [Google Scholar] [CrossRef]
- Baillot, A.; Boissy, P.; Tousignant, M.; Langlois, M.-F. Feasibility and effect of in-home physical exercise training delivered via telehealth before bariatric surgery. J. Telemed. Telecare 2016, 23, 529–535. [Google Scholar] [CrossRef] [PubMed]
- Runfola, M.; Fantola, G.; Pintus, S.; Iafrancesco, M.; Moroni, R. Telemedicine Implementation on a Bariatric Outpatient Clinic During COVID-19 Pandemic in Italy: an Unexpected Hill-Start. Obes. Surg. 2020, 30, 5145–5149. [Google Scholar] [CrossRef] [PubMed]
- Wolf, D.M.; Lehman, L.; Quinlin, R.; Zullo, T.; Hoffman, L. Effect of Patient-Centered Care on Patient Satisfaction and Quality of Care. J. Nurs. Care Qual. 2008, 23, 316–321. [Google Scholar] [CrossRef]
- Parnell, K.E.; Philip, J.; Billmeier, S.E.; Trus, T.L. The effects of using telemedicine for introductory bariatric surgery seminars during the COVID-19 pandemic. Surg. Endosc. 2022, 37, 5509–5515. [Google Scholar] [CrossRef] [PubMed]
- Güven, B.; Akyolcu, N. Effects of Nurse-Led Education on Quality of Life and Weight Loss in Patients Undergoing Bariatric Surgery. Bariatr. Surg. Pr. Patient Care 2020, 15, 81–87. [Google Scholar] [CrossRef]
- Sarkhosh, K.; Switzer, N.J.; El-Hadi, M.; Birch, D.W.; Shi, X.; Karmali, S. The Impact of Bariatric Surgery on Obstructive Sleep Apnea: A Systematic Review. Obes. Surg. 2013, 23, 414–423. [Google Scholar] [CrossRef]
- Pinto, T.F.; de Bruin, P.F.C.; de Bruin, V.M.S.; Lopes, P.M.; Lemos, F.N. Obesity, Hypersomnolence, and Quality of Sleep: the Impact of Bariatric Surgery. Obes. Surg. 2017, 27, 1775–1779. [Google Scholar] [CrossRef] [PubMed]
- Baillot, A.; Romain, A.J.; Boisvert-Vigneault, K.; Audet, M.; Baillargeon, J.P.; Dionne, I.J.; Valiquette, L.; Chakra, C.N.A.; Avignon, A.; Langlois, M.-F. Effects of Lifestyle Interventions That Include a Physical Activity Component in Class II and III Obese Individuals: A Systematic Review and Meta-Analysis. PLOS ONE 2015, 10, e0119017–e0119017. [Google Scholar] [CrossRef]
- dos Santos, C.A. Asociación a largo plazo entre la actividad física, el aumento de peso, los factores de riesgo metabólicos y la calidad de vida en pacientes sometidos a cirugía bariátrica – Revisión de la literatura sistemática (Long-term association between physical activity, weight gain, metabolic risk factors and quality of life in patients undergoing bariatric surgery - Systematic Literature Review) (Associação no longo-termo entre a prática de atividade física, o reganho de peso, fatores de risco metabólic. Retos 2022, 46, 622–630. [Google Scholar] [CrossRef]
- Pujol-Rafols, J.; Al Abbas, A.I.; Devriendt, S.; Guerra, A.; Herrera, M.F.; Himpens, J.; Pardina, E.; Pouwels, S.; Ramos, A.; Ribeiro, R.J.; et al. Conversion of Adjustable Gastric Banding to Roux-en-Y Gastric Bypass in One or Two Steps: What Is the Best Approach? Analysis of a Multicenter Database Concerning 832 Patients. Obes. Surg. 2020, 30, 5026–5032. [Google Scholar] [CrossRef] [PubMed]
- Rubino, F.; Nathan, D.M.; Eckel, R.H.; Schauer, P.R.; Alberti, K.G.M.; Zimmet, P.Z.; Del Prato, S.; Ji, L.; Sadikot, S.M.; Herman, W.H.; et al. Metabolic Surgery in the Treatment Algorithm for Type 2 Diabetes: A Joint Statement by International Diabetes Organizations. Surg. Obes. Relat. Dis. 2016, 12, 1144–1162. [Google Scholar] [CrossRef] [PubMed]
- Rubino, F.; Gagner, M. Potential of Surgery for Curing Type 2 Diabetes Mellitus. Ann. Surg. 2002, 236, 554–559. [Google Scholar] [CrossRef]
- Mendes, C.; Carvalho, M.; Oliveira, L.; Rodrigues, L.M.; Gregório, J. Nurse-led intervention for the management of bariatric surgery patients: A systematic review. Obes. Rev. 2023, 24, e13614. [Google Scholar] [CrossRef]
| Female | Male | Total | |
|---|---|---|---|
| Sex | 68 (85%) | 12 (15%) | 80 (100%) |
| Age | 42,3±9,86 | 45±10,3 | 42,7±9,91 |
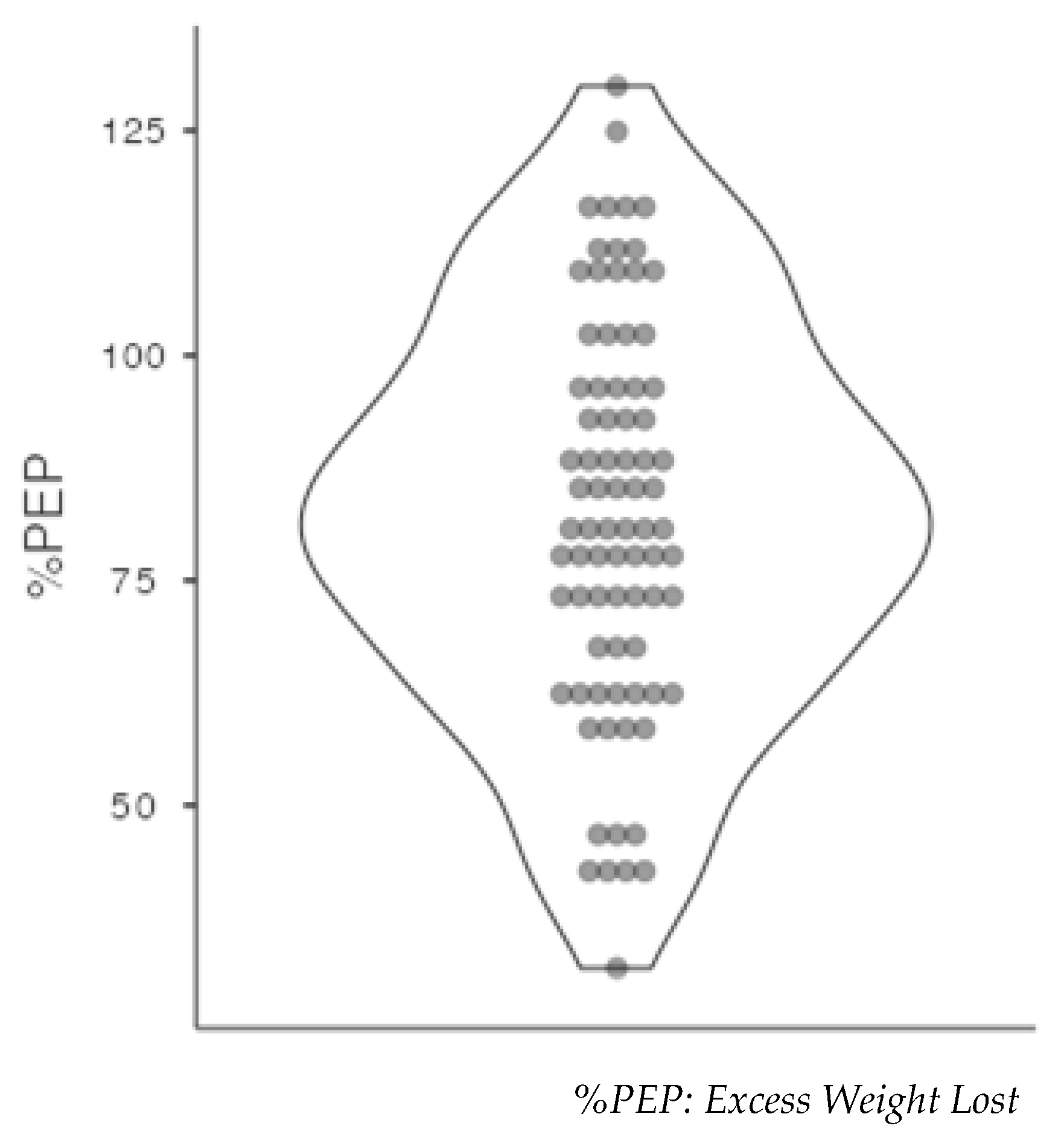
| %PEP | 83,6±22,6 | 74,2±14 | 82,2±21,7 |
| Total subjects | n=80 |
|---|---|
| Gender (Female %) | 85% |
| Age (years) | 42,7 (±9,91) |
| Marital status | |
| Single | 13,8% |
| Married | 60,0% |
| Divorced | 23,8% |
| Widower | 2,5% |
| Initial weight (kg) | 114 (±15,4) |
| Initial BMI (kg/m2) | 42,8 (±4,37) |
| PP (%) | 53,1 (±22,8) |
| PEP (%) | 82,2 (±21,7) |
| Dyslipidemia (initial prevalence) | 82,5% |
| Diabetes (initial prevalence) | 78,8% |
| Hypertension (initial prevalence) | 83,8% |
| OSAS (initial prevalence) | 17,5% |
| Variables | Baseline | 3 years | Sig. |
|---|---|---|---|
| Weight (Kg) | 114±15,4 | 75,6±13,4 | p=< 0,001 * |
| BMI (Kg/m2) | 42,8±4,37 | 28,4±4,28 | p=< 0,001 * |
| Dyslipidemia (%) | 82,5% | 6,3% | p=< 0,001 + |
| Diabetes (%) | 78,8% | 11,3% | p=< 0,001 + |
| HTA (%) | 83,8% | 5% | p=< 0,001 + |
| OSAS (%) | 17,5% | 2,5% | p=< 0,001 + |
| Associated diseases | Time* QoL | Time* QoS | |
|---|---|---|---|
|
Dislipidemia |
baseline | p= 0,250 | p= 0,654 |
| 3 years | |||
| Diabetes | baseline | p= 0,888 | p= 0,786 |
| 3 years | |||
|
HTA |
baseline | p= 0,657 | p= 0,877 |
| 3 years | |||
| OSAS | baseline | p= 0,318 | p= 0,476 |
| 3 years | |||
| Level of Satisfaction | Sig. | ||
|---|---|---|---|
| Satisfied | Not Satisfied | ||
| % Excess Loss Weight | 88,5±17,8 | 66,7±23 | P<0,001* |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




