Submitted:
06 March 2024
Posted:
08 March 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction:
2. Methods:
2.1. Setting:
2.2. Participants:
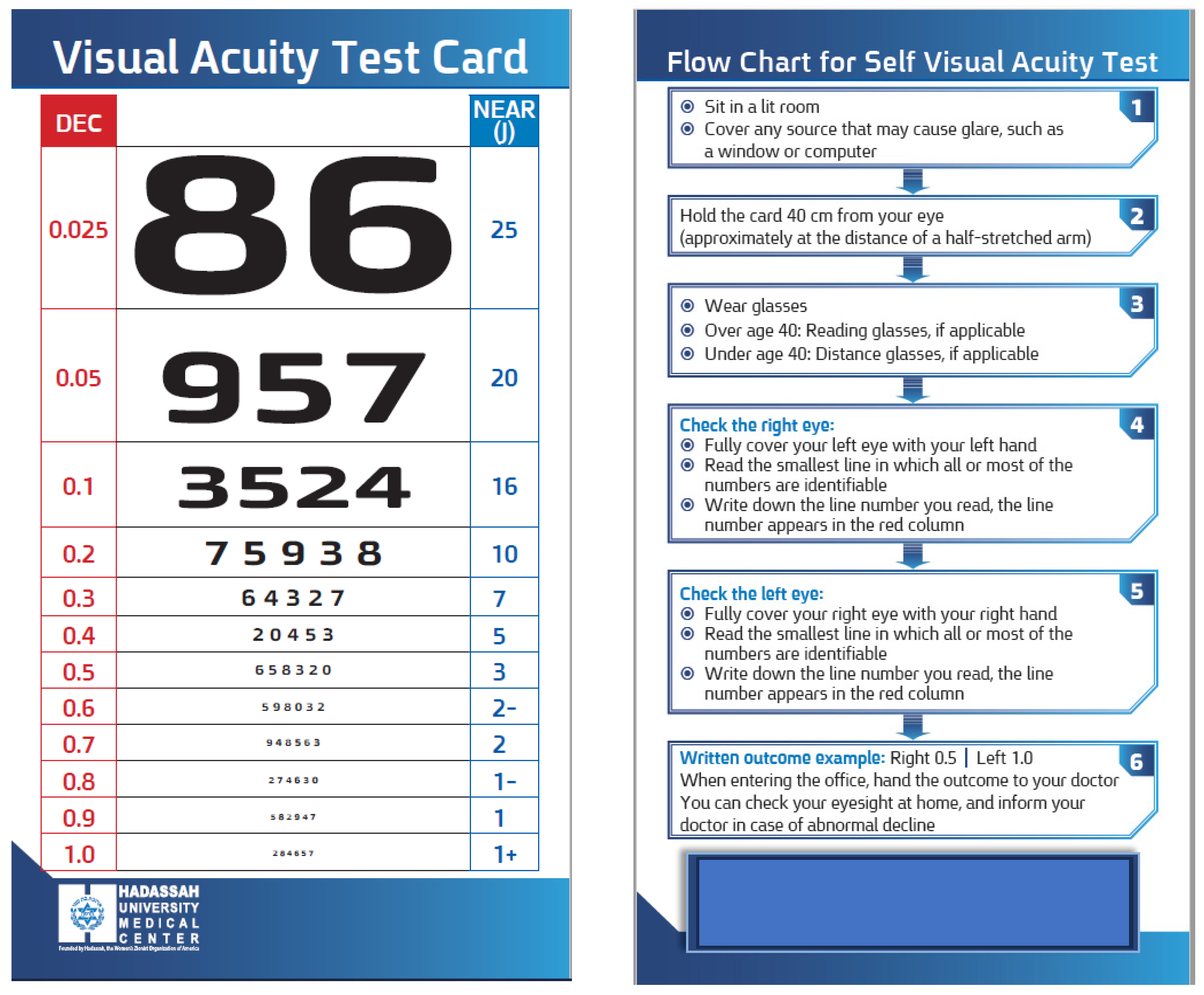
2.3. Development of the visual acuity near chart
2.3.1. Procedure
2.4. Outcome measures
2.5. Sample Size Calculation
2.6. Statistical analysis
2.7. Power Analysis
3. Results
3.1. Test-retest reliability:
3.2. Accuracy:
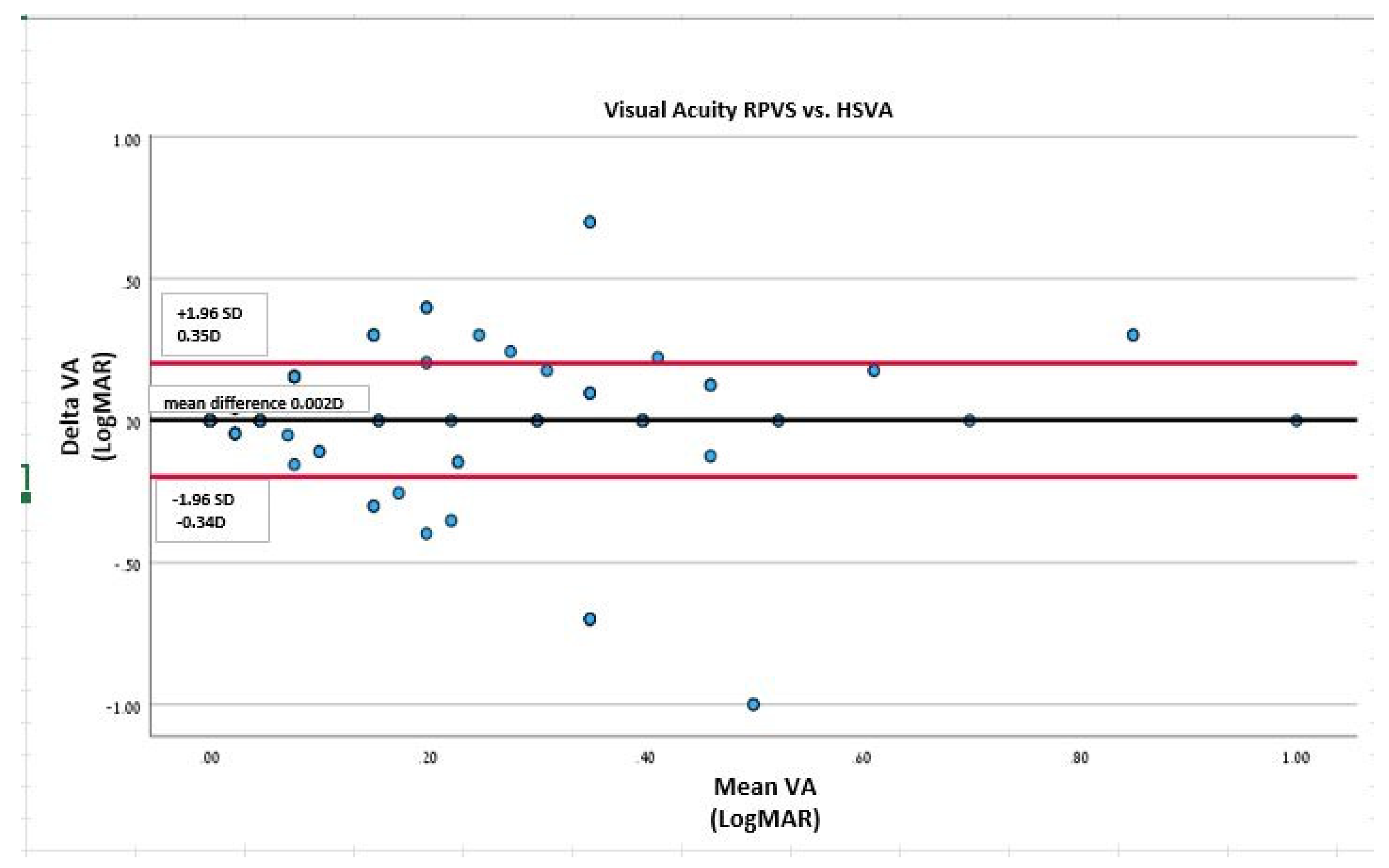
3.3. Agreement between HSVA and RPVS charts:
3.4. Self-test HSVA:
3.5. Self-test vs. electronic medical records:
3.6. Prediction analysis:
4. Discussion:
5. Conclusions:
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations:
References
- E. Silverstein, J. S. Williams, J. R. Brown, E. Bylykbashi, and S. S. Stinnett, “Teleophthalmology: Evaluation of Phone-based Visual Acuity in a Pediatric Population,” Am J Ophthalmol, vol. 221, pp. 199–206, 2021. [CrossRef]
- J. Siktberg et al., “Validation of a Standardized Home Visual Acuity Test for Teleophthalmology,” Ophthalmology Science, vol. 1, no. 1, p. 100007, 2021. [CrossRef]
- E. P. Chen et al., “Remote vision testing of central retinal acuity and comparison with clinic-based Snellen acuity testing in patients followed for retinal conditions,” Digit Health, vol. 9, pp. 1–7, 2023. [CrossRef]
- N. M. Holekamp, “Moving from Clinic to Home: What the Future Holds for Ophthalmic Telemedicine,” Am J Ophthalmol, vol. 187, pp. xxviii–xxxv, 2018. [CrossRef]
- A. Arditi and R. Cagenello, “On the Statistical Reliability of Letter-Chart Visual Acuity Measurements,” Invest Ophthalmol Vis Sci, vol. 34, no. 1, pp. 120–129, 1993.
- J. W. H. H Kenneth Walker, W Dallas Hall, Clinical Methods: The History, Physical, and Laboratory Examinations - PubMed, 3rd editio. Boston: Butterworths, 1990.
- D. M. G. Harrison F. Daiber, Visual Acuity. Treasure Island (FL): StatPearls Publishing, 2023.
- R. Hetherinton, “The Shellen Chart as a test of visual acuity,” Psychol Forsch, vol. 357, pp. 349–357, 1954. [CrossRef]
- D. Caltrider, A. Gupta, and K. Tripathy, Evaluation Of Visual Acuity. StatPearls Publishing, Treasure Island (FL), 2021.
- R. R. A. Bourne et al., “Magnitude, temporal trends, and projections of the global prevalence of blindness and distance and near vision impairment : a systematic review and meta-analysis,” Lancet Glob Health, vol. 5, no. (9), pp. e888–e897, 2017. [CrossRef]
- A. L. C. J S Wolffsohn, “The practical near acuity chart (PNAC) and prediction of visual ability at near.” 2000. [CrossRef]
- A. L. C. J S Wolffsohn, “The practical near acuity chart (PNAC) and prediction of visual ability at near - PubMed,” Ophthalmic & physiological optics, vol. 20, no. 2, pp. 90–7, 2000. [CrossRef]
- A. J. Thirunavukarasu, R. Hassan, A. Limonard, and S. V. Savant, “Accuracy and reliability of self-administered visual acuity tests: Systematic review of pragmatic trials,” PLoS One, vol. 18, no. 6, p. e0281847, Jun. 2023. [CrossRef]
- X. Han et al., “Development and Validation of a Smartphone-Based Visual Acuity Test (Vision at Home),” vol. 8, no. 4, 2019. [CrossRef]
- A. Bastawrous et al., “Development and Validation of a Smartphone-Based Visual Acuity Test (Peek Acuity) for Clinical Practice and Community-Based Fieldwork,” JAMA Ophthalmol, vol. 133, no. (8), pp. 930–7, 2015. [CrossRef]
- D. M. Do Gyun Kim, Aaron D Webel, Mark S Blumenkranz, Yonguk Kim, Ji Ho Yang, Seung Young Yu, Hyung Woo Kwak, Daniel Palanker, Brian Toy, “A Smartphone-Based Near-Vision Testing System: Design, Accuracy, and Reproducibility Compared With Standard Clinical Measures,” Ophthalmic Surg Lasers Imaging Retina, vol. 53, no. 2, pp. 79–84, 2022. [CrossRef]
- E. Racano, G. Malfatti, R. Pertile, R. D. Site, F. Romanelli, and A. Nicolini, “A novel smartphone App to support the clinical practice of pediatric ophthalmology and strabismus: the validation of visual acuity tests,” Eur J Pediatr, 2023. [CrossRef]
- J. Claessens, J. Van Egmond, J. Wanten, N. Bauer, R. Nuijts, and R. Wisse, “The Accuracy of a Web-Based Visual Acuity Self-assessment Tool Performed Independently by Eye Care Patients at Home: Method Comparison Study,” JMIR Form Res, vol. 7, 2023. [CrossRef]
- M. Raja, D. Ramamurthy, K. Srinivasan, and L. S. Varadharajan, “Development of Pocket Vision Screener and its effectiveness at screening visual acuity deficits,” Indian J Ophthalmol, vol. 62, no. (12), pp. 1152–5, 2014. [CrossRef]
- E. P. Chen et al., “Remote vision testing of central retinal acuity and comparison with clinic-based Snellen acuity testing in patients followed for retinal conditions,” Digit Health, vol. 9, Jan. 2023. [CrossRef]
- G. Labiris et al., “Development and Validation of the First Smart TV-Based Visual Acuity Test: A Prospective Study,” Healthcare (Basel), vol. 10, no. 11, 2022. [CrossRef]
- J. L. J. Claessens, J. R. Geuvers, S. M. Imhof, and R. P. L. Wisse, “Digital Tools for the Self-Assessment of Visual Acuity: A Systematic Review,” Ophthalmol Ther, vol. 10, no. 4, pp. 715–730, 2021. [CrossRef]
- M. L. Rubin and C. Horton, “Warning on inaccurate Rosenbaum cards for testing near vision,” Surv Ophthalmol, vol. 42, no. 2, 1997. [CrossRef]
- R. A. Armstrong, “Statistical guidelines for the analysis of data obtained from one or both eyes,” Ophthalmic & physiological optics, pp. 7–14, 2013. [CrossRef]
- L. J. Briones, J. P. Gomez, and E. F. Leuenberger, “The Philippine Peso Bill as an Alternative Near Visual Acuity Chart in Filipino Eyes: A Pilot Study,” Clin Ophthalmol, vol. 16, pp. 3437–3445, 2022. [CrossRef]
- P. Cho and G. C. Woo, “Repeatability of the Waterloo Four-Contrast LogMAR Visual Acuity chart and Near Vision Test card on a group of normal young adults,” Ophthalmic & physiological optics, vol. 24, no. 5, pp. 427–435, 2004. [CrossRef]
- T. A. Chen, J. Li, J. M. Schallhorn, and C. Q. Sun, “Comparing a Home Vision Self-Assessment Test to Office-Based Snellen Visual Acuity,” Clinical ophthalmology, vol. 15, pp. 3205–3211, 2021. [CrossRef]
- Y. Xian, Y. Ye, F. Liu, X. Zhou, and J. Zhao, “Agreement between a mobile applet-based visual acuity self-test program and the conventional method for distance and near visual acuity tests,” Clin Exp Ophthalmol, vol. 51, no. 2, pp. 112–121, 2023. [CrossRef]
- D. A. Rosser, D. A. H. Laidlaw, and I. E. Murdoch, “The development of a ‘reduced logMAR’ visual acuity chart for use in routine clinical practice,” Br J Ophthalmol, vol. 85, no. 4, pp. 432–436, 2001. [CrossRef]
- C. J. Brady, A. O. Eghrari, and A. B. Labrique, “Smartphone-Based Visual Acuity Measurement for Screening and Clinical Assessment,” JAMA, vol. 314, no. 24, pp. 2682–2683, 2015. [CrossRef]
- M. D. Cooke et al., “An innovative visual acuity chart for urgent and primary care settings: validation of the Runge near vision card,” Eye (Lond), vol. 33, no. 7, pp. 1104–1110, 2019. [CrossRef]
- “The Jaeger Notation Debate - Precision Vision.” Accessed: Feb. 23, 2024. [Online]. Available: https://precision-vision.com/the-jaeger-notation-debate/.

| Visual Acuity Chart | Mean | Median | SD | P* | Spearman (Rs) | P |
|---|---|---|---|---|---|---|
| Snellen -1st test | 0.06 | 0.0 | 0.19 | 0.14 | 0.99 | <0.001 |
| Snellen – 2nd test | 0.04 | 0.0 | 0.14 | |||
| RPVSb -1st test | 0.02 | 0.0 | 0.11 | 1.0 | 1.0 | <0.001 |
| RPVSb – 2nd test | 0.02 | 0.0 | 0.11 | |||
| HSVAc -1st test | 0.02 | 0.0 | 0.11 | 1.0 | 1.0 | <0.001 |
| HSVAc – 2nd test | 0.02 | 0.0 | 0.11 |
| Visual Acuity Chart | Mean | Median | SD | P* |
|---|---|---|---|---|
| Snellen | 0.15 | 0.1 | 0.22 | Snellen-RPVS: 0.001 |
| RPVSb | 0.10 | 0.0 | 0.19 | Snellen-HSVA: 0.001 |
| HSVAc | 0.09 | 0.0 | 0.20 | RPVS-HSVA: 0.10 |
| Test method | Mean | Median | SD | P* | Spearman (Rs) | P | ICC |
|---|---|---|---|---|---|---|---|
| Self-test | 0.10 | 0.0 | 0.20 | 0.17 | |||
| Masked examiner | 0.09 | 0.0 | 0.19 | 0.87 | <0.001 | 0.96 |
| Visual Acuity Chart | Mean | Median | SD | P* | P* |
|---|---|---|---|---|---|
| Snellen (medical records) | 0.24 | 0.1 | 0.31 | 0.12 | |
| HSVA by examiner | 0.18 | 0.0 | 0.27 | 0.04 | |
| Self-test HSVA (N=26) | 0.19 | 0.05 | 0.27 |
| Near RPVS VA | Distance Snellen VA | ||||||
|---|---|---|---|---|---|---|---|
| B (SEB) | β | P | B(SEB) | β | P | ||
| Model I | age | 0.004 (0.001) | 0.35 | 0.003 | 0.011 (0.07) | 0.26 | 0.02 |
| F | 9.5 | 0.003 | 5.1 | 0.02 | |||
| R² | 0.13 | 0.07 | |||||
| Model II | age | 0.001 (0.00) | 0.08 | 0.06 | 0.001 (0.001) | 0.09 | 0.37 |
| HSVA by examiner | 0.13 (0.18) | 0.91 | 0.001 | -0.50(0.45) | -0.40 | 0.27 | |
| HSVA Self-test | -0.24(0.17) | -0.22 | 0.15 | 1.10(0.43) | 0.93 | 0.01 | |
| F | 156.9 | 0.001 | 11.6 | 0.001 | |||
| R² | 0.88 | 0.36 | |||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




