Submitted:
29 February 2024
Posted:
01 March 2024
You are already at the latest version
Abstract
In the pursuit of effective pain management, non-pharmacological interventions are gaining prominence within the medical community. Techniques like cognitive-behavioral therapy, physiotherapy, and relaxation methods are integral parts of modern treatment strategies. Among these, aromatherapy stands out for its drug-free approach and potential to utilize the body's sensory pathways for pain relief. Here we have introduced a Modified Olfactory Rehabilitation Protocol (mORP) and assessed its effectiveness in 34 chronic pain patients. Contrasted with a Control Group, which did not undergo olfactory rehabilitation, our novel protocol incorporates enhanced strategies to overcome conventional limitations. Initial results show significant pain reduction in the mORP group, supported by fMRI analyses revealing alterations in brain activation patterns associated with pain perception and emotional processing. These changes, particularly in olfactory-related regions, highlight mORP's ability to modulate pain pathways. These findings suggest mORP could revolutionize non-pharmacological pain therapy, emphasizing the potential of sensory-based approaches in reshaping chronic pain experiences. Further research is warranted to validate these findings and elucidate underlying mechanisms, guiding future advancements in sensory interventions against chronic pain.
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
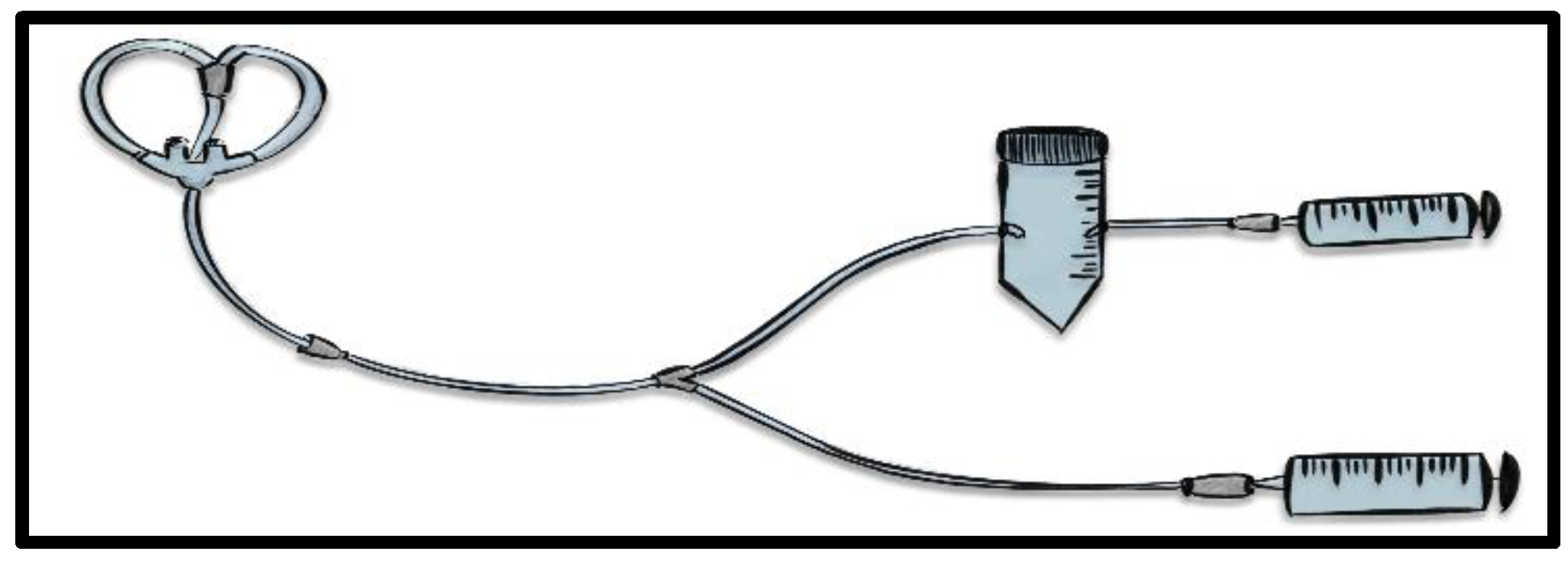
2.2. The modified Olfactory Rehabilitation Protocol (mORP)
2.3. fMRI BOLD 3 Tesla Measurements
2.4. Statistical Analysis
3. Results
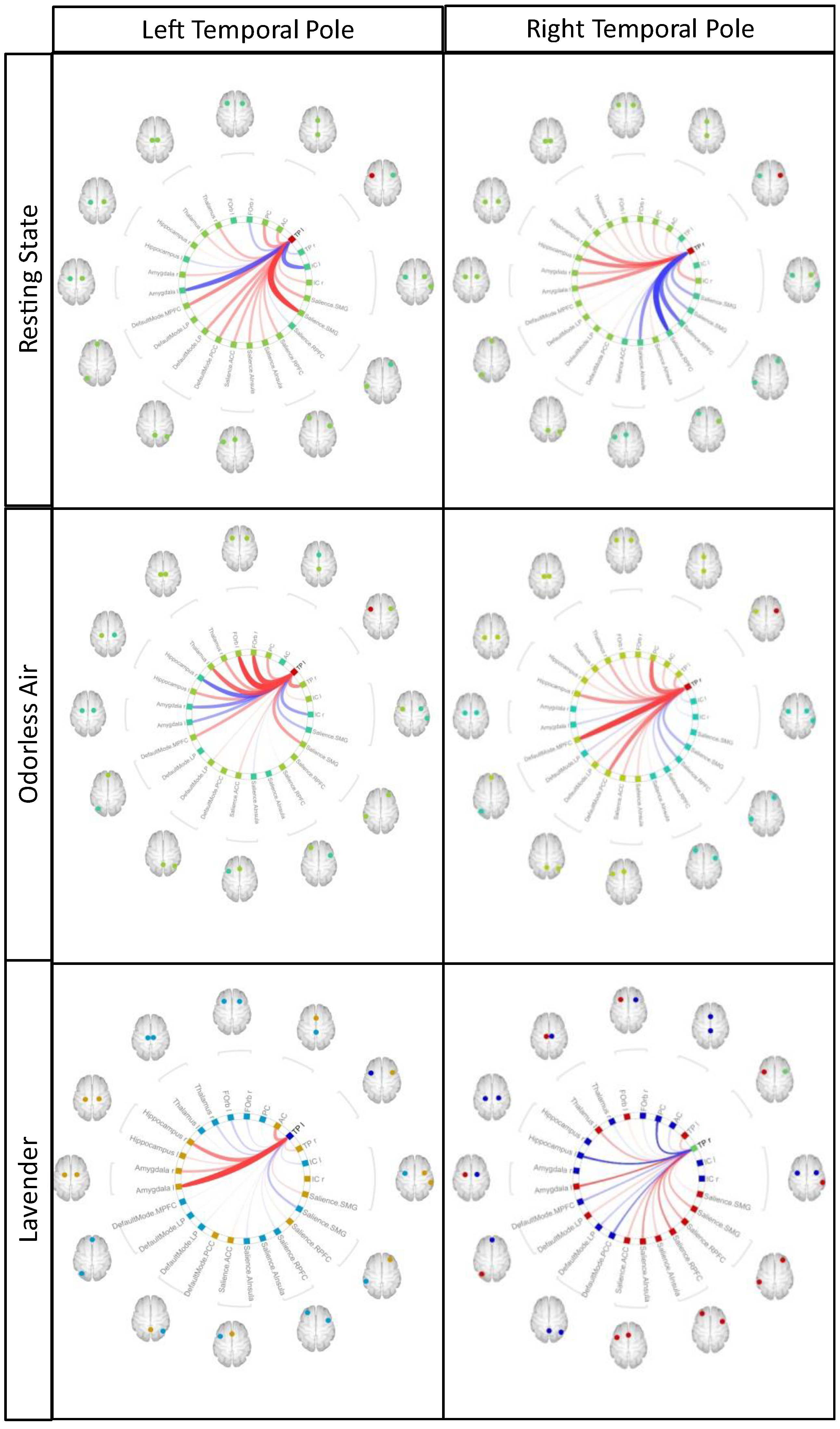
3.2. fMRI-BOLD Results and Data Analysis with CONN
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Cohen, S.P.; Vase, L.; Hooten, W.M. Chronic pain: an update on burden, best practices, and new advances. Lancet. 2021, 397, 2082–2097. [Google Scholar] [CrossRef] [PubMed]
- Gossrau, G.; Zaranek, L.; Klimova, A.; Sabatowski, R.; Koch, T.; Richter, M.; Haehner, A. Olfactory training reduces pain sensitivity in children and adolescents with primary headaches. Front Pain Res (Lausanne). 2023, 4, 1091984, PMID: 36860330; PMCID: PMC9968932. [Google Scholar] [CrossRef]
- Garland, E.L. Pain processing in the human nervous system: a selective review of nociceptive and biobehavioral pathways. Prim Care. 2012, 39, 561–571, Epub 2012 Jul 24. PMID: 22958566; PMCID: PMC3438523. [Google Scholar] [CrossRef]
- Hummel, T.; Rissom, K.; Reden, J.; Hähner, A.; Weidenbecher, M.; Hüttenbrink, K.B. Effects of olfactory training in patients with olfactory loss. Laryngoscope. 2009, 119, 496–499. [Google Scholar] [CrossRef] [PubMed]
- Kronenbuerger, M.; Pilgramm, M. Olfactory Training. 2022 Oct 24. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan–. [PubMed]
- Gossrau, G.; Baum, D.; Koch, T.; Sabatowski, R.; Hummel, T.; Haehner, A. Exposure to Odors Increases Pain Threshold in Chronic Low Back Pain Patients. Pain Med. 2020, 21, 2546–2551. [Google Scholar] [CrossRef] [PubMed]
- Yalcinkaya, G.; Sengul, Y.S. Can olfactory training change the psychosocial aspects of chronic pain? Explore (NY). 2023, 19, 561–564, Epub 2022 Oct 23. PMID: 36307317. [Google Scholar] [CrossRef]
- Kandić, M.; Moliadze, V.; Andoh, J.; Flor, H.; Nees, F. Brain Circuits Involved in the Development of Chronic Musculoskeletal Pain: Evidence From Non-invasive Brain Stimulation. Front Neurol. 2021, 12, 732034, PMID: 34531819, PMCID: PMC8438114. [Google Scholar] [CrossRef]
- Caston, R.M.; Smith, E.H.; Davis, T.S.; Rolston, J.D. The Cerebral Localization of Pain: Anatomical and Functional Considerations for Targeted Electrical Therapies. J Clin Med. 2020, 9, 1945, PMID: 32580436, PMCID: PMC7355617. [Google Scholar] [CrossRef]
- Apkarian, A.V.; Bushnell, M.C.; Treede, R.D.; Zubieta, J.K. Human brain mechanisms of pain perception and regulation in health and disease. Eur J Pain. 2005, 9, 463–484, Epub 2005 Jan 21. PMID: 15979027. [Google Scholar] [CrossRef]
- Mueller, S.; Wang, D.; Fox, M.D.; Yeo, B.T.; Sepulcre, J.; Sabuncu, M.R.; Shafee, R.; Lu, J.; Liu, H. Individual variability in functional connectivity architecture of the human brain. Neuron. 2013, 77, 586–595, PMID: 23395382, PMCID: PMC3746075. [Google Scholar] [CrossRef]
- Hinz, A.; Luck, T.; Riedel-Heller, S.G.; Herzberg, P.Y.; Rolffs, C.; Wirkner, K.; Engel, C. Olfactory dysfunction: properties of the Sniffin' Sticks Screening 12 test and associations with quality of life. Eur Arch Otorhinolaryngol. 2019, 276, 389–395, Epub 2018 Nov 20. PMID: 30456541. [Google Scholar] [CrossRef]
- Haefeli, M.; Elfering, A. Pain assessment. Eur Spine J. 2006, 15 (Suppl 1), S17–24, Epub 2005 Dec 1. PMID: 16320034; PMCID: PMC3454549. [Google Scholar] [CrossRef]
- Shibasaki, H. Central mechanisms of pain perception. Suppl Clin Neurophysiol. 2004, 57, 39–49. [Google Scholar] [CrossRef] [PubMed]
- Blanco, S.; Sanromán, L.; Pérez-Calvo, S.; Velasco, L.; Peñacoba, C. Olfactory and cognitive functioning in patients with fibromyalgia. Psychol Health Med. 2019, 24, 530–541, Epub 2018 Nov 19. PMID: 30453770. [Google Scholar] [CrossRef]
- Functional bold MRI: advantages of the 3 T vs. the 1.5 T, Reyes García-Eulate, David García-García, Pablo D Dominguez, Jose J Noguera, Esther De Luis, María C Rodriguez-Oroz, Jose L Zubieta. Clinical Imaging 2011, 35, 236–241. [CrossRef]
- Livshits, I.; Hussein, S.; Kennedy, C.; Weinstock-Guttman, B.; Hojnacki, D.; Zivadinov, R. Comparison of a 1.5T standard vs. 3T optimized protocols in multiple sclerosis patients. Minerva Med. 2012, 103, 97–102. [Google Scholar] [CrossRef] [PubMed]
- Willinek, W.A.; Schild, H.H. Clinical advantages of 3. 0 T MRI over 1.5 T. Eur J Radiol. 2008, 65, 2–14, Epub 2007 Dec 26. PMID: 18162354. [Google Scholar] [CrossRef]
- Whitfield-Gabrieli, S.; Nieto-Castanon, A. Conn: a functional connectivity toolbox for correlated and anticorrelated brain networks. Brain Connect. 2012, 2, 125–141, Epub 2012 Jul 19. PMID: 22642651. [Google Scholar] [CrossRef]
- Zhong, Y.; Wang, H.; Lu, G.; Zhang, Z.; Jiao, Q.; Liu, Y. Detecting functional connectivity in fMRI using PCA and regression analysis. Brain Topogr. 2009, 22, 134–144, Epub 2009 May 1. PMID: 19408112. [Google Scholar] [CrossRef]
- Chen, G.; Chen, G.; Xie, C.; Li, S.J. Negative functional connectivity and its dependence on the shortest path length of positive network in the resting-state human brain. Brain Connect. 2011, 1, 195–206, PMID: 22433048, PMCID: PMC3572722. [Google Scholar] [CrossRef]
- Churchill, N.W.; Madsen, K.; Mørup, M. The Functional Segregation and Integration Model: Mixture Model Representations of Consistent and Variable Group-Level Connectivity in fMRI. Neural Comput. 2016, 28, 2250–2290, Epub 2016 Aug 24. PMID: 27557105. [Google Scholar] [CrossRef]
- Atisook, R.; Euasobhon, P.; Saengsanon, A.; Jensen, M.P. Validity and Utility of Four Pain Intensity Measures for Use in International Research. J Pain Res. 2021, 14, 1129–1139, PMID: 33907460; PMCID: PMC8071079. [Google Scholar] [CrossRef]
- Faria, V.; Dulheuer, J.; Joshi, A.; Wahl, H.; Klimova, A.; Haehner, A.; Gossrau, G. Impact of a 12-week olfactory training programme in women with migraine with aura: protocol for a double-blind, randomised, placebo-controlled trial. BMJ Open. 2023, 13, e071443, PMID: 37419649, PMCID: PMC10335595. [Google Scholar] [CrossRef]
- Zhou, G.; Lane, G.; Cooper, S.L.; Kahnt, T.; Zelano, C. Characterizing functional pathways of the human olfactory system. Elife. 2019, 8, e47177, PMID: 31339489, PMCID: PMC6656430. [Google Scholar] [CrossRef]
- Philpott, C.M.; Bennett, A.; Murty, G.E. A brief history of olfaction and olfactometry. J Laryngol Otol. 2008, 122, 657–662, Epub 2008 Jan 18. PMID: 18201391. [Google Scholar] [CrossRef]
- Weismann, M.; Yousry, I.; Heuberger, E.; Nolte, A.; Ilmberger, J.; Kobal, G.; Yousry, T.A.; Kettenmann, B.; Naidich, T.P. Functional magnetic resonance imaging of human olfaction. Neuroimaging Clin N Am. 2001, 11, 237–250. [Google Scholar] [PubMed]
- Grady, C.L. Meta-analytic and functional connectivity evidence from functional magnetic resonance imaging for an anterior to posterior gradient of function along the hippocampal axis. Hippocampus. 2020, 30, 456–471, Epub 2019 Oct 7. PMID: 31589003. [Google Scholar] [CrossRef]
- Kastrup, A.; Baudewig, J.; Schnaudigel, S.; et al. Behavioral correlates of negative BOLD signal changes in the primary somatosensory cortex. Neuroimage. 2008, 41, 1364–1371. [Google Scholar] [CrossRef]
- Stevens, J.S.; Hamann, S. Sex differences in brain activation to emotional stimuli: a meta-analysis of neuroimaging studies. Neuropsychologia. 2012, 50, 1578–1593. [Google Scholar] [CrossRef]
- Minnix, J.A.; Versace, F.; Robinson, J.D.; et al. The late positive potential (LPP) in response to varying types of emotional and cigarette stimuli in smokers: a content comparison. Int J Psychophysiol. 2013, 89, 18–25. [Google Scholar] [CrossRef]
- Yalcinkaya, G.; Sengul, Y.S. Can olfactory training change the psychosocial aspects of chronic pain? Explore (NY). 2023, 19, 561–564, Epub 2022 Oct 23. PMID: 36307317. [Google Scholar] [CrossRef]
- Gottfried, J.A. Smell: central nervous processing. Adv Otorhinolaryngol. 2006, 63, 44–69. [Google Scholar] [CrossRef] [PubMed]
| Sex distribution | Sniffin Sticks Score | Chronic Pain | |
|---|---|---|---|
| Control Group | 25 females; 8 males | Mean Score: 13.7 | Fibromyalgia: 14 |
| SD: 1.38 | Lumbar pain: 10 | ||
| Other*: 9 | |||
| Test Group | 24 females; 10 males | Mean score: 13.1 | Fibromyalgia: 14 |
| SD: 1.34 | Lumbar Pain: 12 | ||
| Other*: 8 |
| Variable | Control Group Mean (SD) | Test Group Mean (SD) | p-value | t-statistic |
|---|---|---|---|---|
| Age (years) | 52.76 (11.86) | 54.32 (14.89) | 0.6362 | 0.25 |
| Sex | 25 females; 8 males | 24 females; 10 males | 0.8402 | |
| SS Score | 13.7 (1.38) | 13.1 (1.34) | 0.076 | 1.806 |
| NRS at t0 | 8.67 (0.92) | 8.68 (0.77) | 0.9624 | -0.44 |
| NRS at t1 | 6.33 (1.53) | 5.30 (1.33) | 0.00495 | 2.91 |
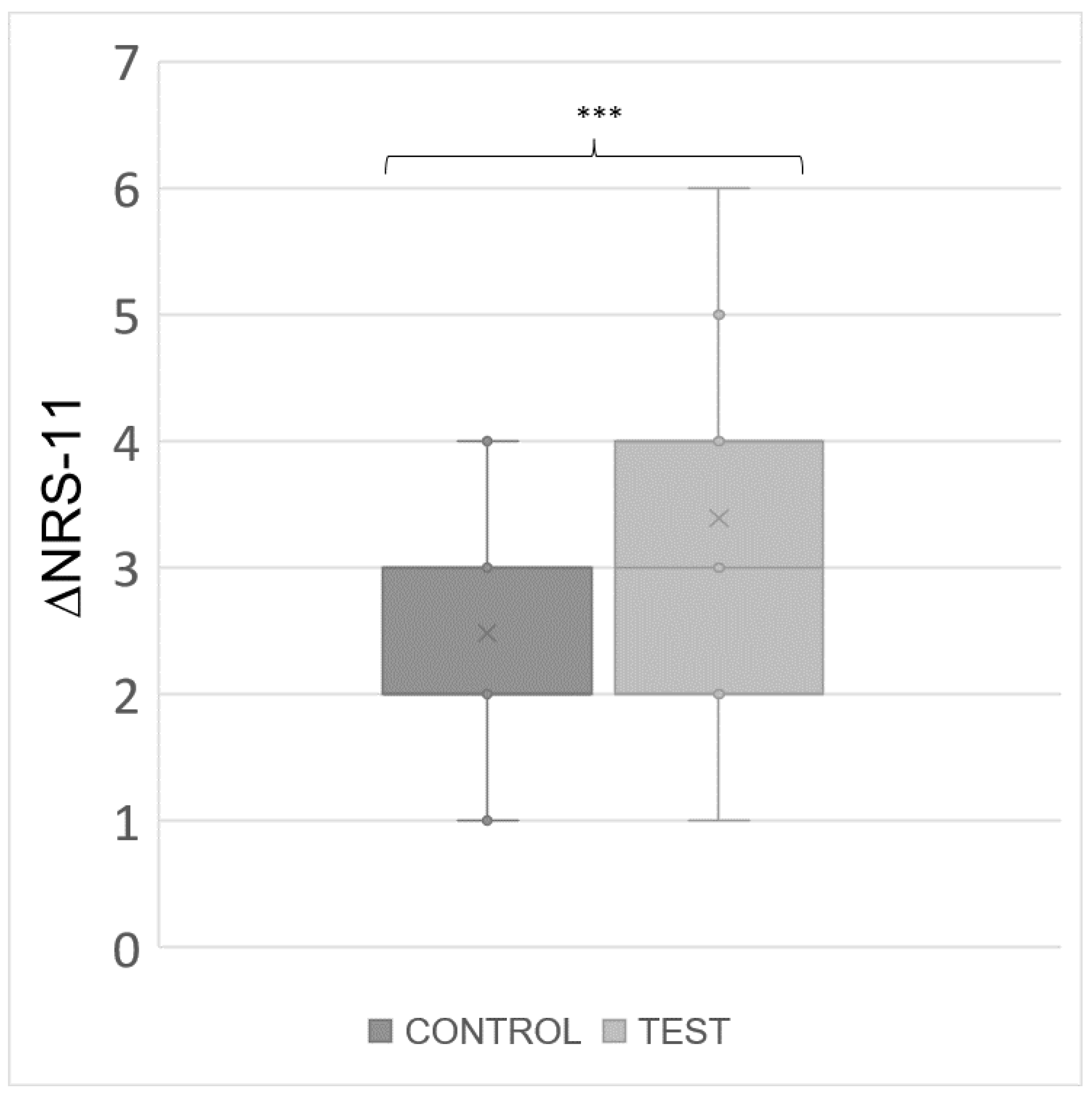
| ΔNRS-11 | 2.33 (1.14) | 3.53 (1.46) | 0.0004 | -3.73 |
| Smoke | 15 - no ; 18 - yes | 20 - no; 14 - yes | 0.395 | 0.724 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




