Submitted:
04 February 2024
Posted:
06 February 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Material and Methods
3. Results
4. Discussion
5. Conclusion
Supplementary Materials
Author Contributions
Funding source
Institutional Review Board Statement
Informed Consent Statement
Declaration of Conflicting Interests
References
- Bozkurt, B.; Ahmad, T.; Alexander, K.M.; Baker, W.L.; Bosak, K.; Breathett, K.; Fonarow, G.C.; Heidenreich, P.; Ho, J.E.; Hsich, E.; Ibrahim, N.E.; Jones, L.M.; Khan, S.S.; Khazanie, P.; Koelling, T.; Krumholz, H.M.; Khush, K.K.; Lee, C.; Morris, A.A.; Page, R.L. 2nd.; Pandey, A., Piano, M.R., Stehlik, J., Stevenson, L.W., Teerlink, J.R., Vaduganathan, M., Eds.; Ziaeian, B. Writing Committee Members. Heart Failure Epidemiology and Outcomes Statistics: A Report of the Heart Failure Society of America. J. Card. Fail. 2023, 29, 1412-1451. [Google Scholar] [CrossRef]
- Sulo, G.; Igland, J.; Vollset, S.E.; Nygård, O.; Ebbing, M.; Sulo, E.; Egeland, G.M.; Tell, G.S. Heart Failure Complicating Acute Myocardial Infarction; Burden and Timing of Occurrence: A Nation-wide Analysis Including 86 771 Patients From the Cardiovascular Disease in Norway (CVDNOR) Project. J. Am. Heart Assoc. 2016, 5. [Google Scholar] [CrossRef] [PubMed]
- Krikunov, P.V.; Vasyuk, Yu.A.; Krikunova, O.V. Predictive value of echocardiography in post myocardial infarction setting. Part 1. Russ. J. Cardiol. 2017, 12, 120–128. [Google Scholar] [CrossRef]
- Hamilton, E.; Desta, L.; Lundberg, A.; Alfredsson, J.; Christersson, C.; Erlinge, D.; Kellerth, T.; Lindmark, K.; Omerovic, E.; Reitan, C.; Jernberg, T. Prevalence and prognostic impact of left ventricular systolic dysfunction or pulmonary congestion after acute myocardial infarction. ESC Heart Fail. 2023, 10, 1347–1357. [Google Scholar] [CrossRef] [PubMed]
- Khaled, S.; Shalaby, G. Severe Left Ventricular Dysfunction Earlier after Acute Myocardial Infarction Treated with Primary Percutaneous Coronary Intervention: Predictors and In-Hospital Outcome- A Middle Eastern Tertiary Center Experience. J. Saudi Heart Assoc. 2023, 34, 257–263. [Google Scholar] [CrossRef] [PubMed]
- Im, M.S.; Kim, H.L.; Kim, S.H.; Lim, W.H.; Seo, J.B.; Chung, W.Y.; Zo, J.H.; Kim, M.A.; Park, K.W.; Koo, B.K.; Kim, H.S.; Chae, I.H.; Cho, D.J. ; Ahn, Y; Jeong, M.H. Other Korea Acute Myocardial Infarction Registry (KAMIR) and Korea Working Group on Myocardial Infarction (KorMI) Investigators. Different prognostic factors according to left ventricular systolic function in patients with acute myocardial infarction. Int. J. Cardiol. [CrossRef]
- Pozo, E.; Sanz, J. Imaging techniques in the evaluation of post-infarction function and scar. Rev. Esp. Cardiol (Engl Ed). [CrossRef]
- Souto, A.L.M.; Souto, R.M.; Teixeira, I.C.R.; Nacif, M.S. Myocardial Viability on Cardiac Magnetic Resonance. Arq. Bras. Cardiol. 2017, 108, 458–469. [Google Scholar] [CrossRef] [PubMed]
- Mochula, O.V.; Sulejmanova, A.S.; Sukhareva, A.E.; Ryabov, V.V.; Zavadovsky, K.V. Relationship between the degree of myocardial damage according to contrast-enhanced cardiac magnetic resonance imaging and laboratory data in patients with acute myocardial infarction. Russ. J. Cardiol. 2022, 27, 5226. [Google Scholar] [CrossRef]
- Bulluck, H.; Dharmakumar, R.; Arai, A.E.; Berry, C.; Hausenloy, D.J. Cardiovascular Magnetic Resonance in Acute ST-Segment-Elevation Myocardial Infarction: Recent Advances, Controversies, and Future Directions. Circulation. 2018, 137, 1949–1964. [Google Scholar] [CrossRef]
- Locca, D.; Bucciarelli-Ducci, C.; Ferrante, G.; La Manna, A.; Keenan, N.G.; Grasso, A.; Barlis, P.; Del Furia, F.; Prasad, S.K.; Kaski, J.C.; Pennell, D.J.; Di Mario, C. New universal definition of myocardial infarction applicable after complex percutaneous coronary interventions? JACC Cardiovasc. Interv. 2010, 3, 950–8. [Google Scholar] [CrossRef] [PubMed]
- Robbers, L.F.H.J.; Delewi, R.; Nijveldt, R.; Hirsch, A.; Beek, A.M.; Kemme, M.J.B.; van Beurden, Y.; van der Laan, A.M.; van der Vleuten, P.A.; Tio, R.A.; Zijlstra, F.; Piek, J.J.; van Rossum, A.C. Myocardial infarct heterogeneity assessment by late gadolinium enhancement cardiovascular magnetic resonance imaging shows predictive value for ventricular arrhythmia development after acute myocardial infarction. Eur. Heart J. Cardiovasc. Imaging. 2013, 14, 1150–1158. [Google Scholar] [CrossRef]
- Jensch, P.J.; Stiermaier, T.; Reinstadler, S.J.; Feistritzer, H.J.; Desch, S.; Fuernau, G.; de Waha-Thiele, S.; Thiele, H.; Eitel, I. Prognostic relevance of peri-infarct zone measured by cardiovascular magnetic resonance in patients with ST-segment elevation myocardial infarction. Int. J. Cardiol. 2022, 347, 83–88. [Google Scholar] [CrossRef] [PubMed]
- Jones, R.E.; Zaidi, H.A.; Hammersley, D.J.; Hatipoglu, S.; Owen, R.; Balaban, G.; de Marvao, A.; Simard, F.; Lota, A.S.; Mahon, C.; Almogheer, B.; Mach, L.; Musella, F.; Chen, X.; Gregson, J.; Lazzari, L.; Ravendren, A.; Leyva, F.; Zhao, S.; Vazir, A.; Lamata, P.; Halliday, B.P.; Pennell, D.J.; Bishop, M.J.; Prasad, S.K. Comprehensive Phenotypic Characterization of Late Gadolinium Enhancement Predicts Sudden Cardiac Death in Coronary Artery Disease. JACC Cardiovasc. Imaging. 2023, 16, 628–638. [Google Scholar] [CrossRef] [PubMed]
- Galea, N.; Dacquino, G.M.; Ammendola, R.M.; Coco, S.; Agati, L.; De Luca, L.; Carbone, I.; Fedele, F.; Catalano, C.; Francone, M. Microvascular obstruction extent predicts major adverse cardiovascular events in patients with acute myocardial infarction and preserved ejection fraction. Eur. Radiol. 2019, 29, 2369–2377. [Google Scholar] [CrossRef] [PubMed]
- Symons, R.; Pontone, G.; Schwitter, J.; Francone, M.; Iglesias, J.F.; Barison, A.; Zalewski, J.; de Luca, L.; Degrauwe, S.; Claus, P.; Guglielmo, M.; Nessler, J.; Carbone, I.; Ferro, G.; Durak, M.; Magistrelli, P.; Lo Presti, A.; Aquaro, G.D.; Eeckhout, E.; Roguelov, C.; Andreini, D.; Vogt, P.; Guaricci, A.I.; Mushtaq, S.; Lorenzoni, V.; Muller, O.; Desmet, W.; Agati, L.; Janssens, S.; Bogaert, J.; Masci, P.G. Long-Term Incremental Prognostic Value of Cardiovascular Magnetic Resonance After ST-Segment Elevation Myocardial Infarction: A Study of the Collaborative Registry on CMR in STEMI. JACC Cardiovasc. Imaging. 2018, 11, 813–825. [Google Scholar] [CrossRef] [PubMed]
- Alekseeva, Ya.V.; Vyshlov, E.V.; Mochula, O.V.; Ussov, V.Yu.; Ryabov, V.V. Effect of intramyocardial haemorrhage on structural and functional echocardiographic parameters of myocardium after ST-segment elevation myocardial infarction with. Russ. J. Cardiol. 2020, 25, 4032. [Google Scholar] [CrossRef]
- Kontsevaya, A.V.; Myrzamatova, A.О.; Drapkina, O.M. Biomarkers in predicting cardiovascular risk: new prospects of troponin I. Cardiovascular Therapy and Prevention. 2020, 19, 2584. [Google Scholar] [CrossRef]
- Salatzki, J.; Giannitsis, E.; Hegenbarth, A.; Mueller-Hennessen, M.; André, F.; Katus, H.A.; Frey, N.; Biener, M. Correlation of serial high-sensitivity cardiac Troponin T values to infarct mass determined by cardiac magnetic resonance imaging: a validation study. Eur. Heart J. Acute Cardiovasc. Care. 2022, 11, 826–833. [Google Scholar] [CrossRef] [PubMed]
- Rahsepar, A.A.; Bluemke, D.A.; Habibi, M.; Liu, K.; Kawel-Boehm, N.; Ambale-Venkatesh, B.; Fernandes, V.R.S.; Rosen, B.D.; Lima, J.A.C.; Carr, J.C. Association of Pro-B-Type Natriuretic Peptide With Cardiac Magnetic Resonance-Measured Global and Regional Cardiac Function and Structure Over 10 Years: The MESA Study. J. Am. Heart Assoc. 2021, 10. [Google Scholar] [CrossRef] [PubMed]
| Parameter | LVEF ≥50 % (n=74) | LVEF 40-49 % (n=27) | LVEF <40 % (n=8) |
р |
| group 1 | group 2 | group 3 | ||
|---|---|---|---|---|
| Age, years | 57 (50; 61) | 58 (54; 62) | 61.8±6.0 | р1-3=0.013 |
| Male/female, n (%) | 62/12 (84/16) | 27/0 (100/0) | 8/0 (100/0) | р1-2=0.026 |
| Body mass index, kg/m2 | 27.9±3.9 | 27.5±3.9 | 26.5 (23.3; 29.2) | ns |
| Systolic blood pressure, mm Hg | 130 (122; 135) | 131.5±15.4 | 129.3±24.8 | ns |
| Diastolic blood pressure, mm Hg | 80 (78; 90) | 79.8±9.4 | 82.7±14.7 | ns |
| Anamnesis of CAD, n (%) | 19 (25.7) | 8 (29.6) | 2 (25.0) | ns |
| Arterial hypertension, n (%) | 62 (83.8) | 24 (88.9) | 6 (75.0) | ns |
| SYNTAX score, points | 15.3±7.1 | 19.7±10.3 | 21.0±9.9 |
р1-2=0.017 р1-3=0.042 |
| Infarct-related artery: ADA, n (%) RCA, n (%) Other artery, n (%) |
32 (43.2) 28 (37.8) 14 (19.0) |
15 (55.6) 7 (25.9) 5 (18.5) |
7 (87.5) 0 (0) 1 (12.5) |
р1-3=0.017 р1-3=0.032 ns |
| Pharmaco-invasive revascularization/Primary PCI, n (%) | 27/47 (36.5/63.5) | 8/19 (29.6/70.4) | 6/2 (75.0/25.0) |
р1-3=0.035 р2-3=0.021 |
| Pain-to-needle time, min | 90 (50; 120) | 135.0±79.3 | 200.0 (120; 270) | р1-3=0.004 |
| Pain-to-balloon time, min | 223 (145; 330) | 305 (210; 560) | 305.0 (227.5; 432.5) | р1-2=0.019 |
| Parameter | LVEF ≥50 % (n=74) |
LVEF 40-49 % (n=27) |
LVEF <40 % (n=8) |
р1-2 | р1-3 | р2-3 |
|---|---|---|---|---|---|---|
| group 1 | group 2 | group 3 | ||||
| Standard cardiacMRI indicators | ||||||
| EDVI, mL/m2 | 76.8 (67.0; 86.0) | 79.6±14.8 | 90.7±24.0 | 0.620 | 0.169 | 0.069 |
| ESVI, mL/m2 | 33.4 (28.3; 38.3) | 41.6±10.1 | 58.8±18.8 | <0.001 | <0.001 | 0.002 |
| LVMI, g/m2 | 57.9 (51.9; 69.5) | 60.1 (56.1; 71.8) | 73.9±17.6 | 0.0936 | 0.018 | 0.121 |
| LVEF, % | 55.5 (52.6; 59.2) | 47.0 (44.1; 49.0) | 37.4 (34.7; 38.3) | <0.001 | <0.001 | <0.001 |
| LCI | 1.4 (1.1; 1.6) | 1.9±0.4 | 2.6±0.4 | <0.001 | <0.001 | <0.001 |
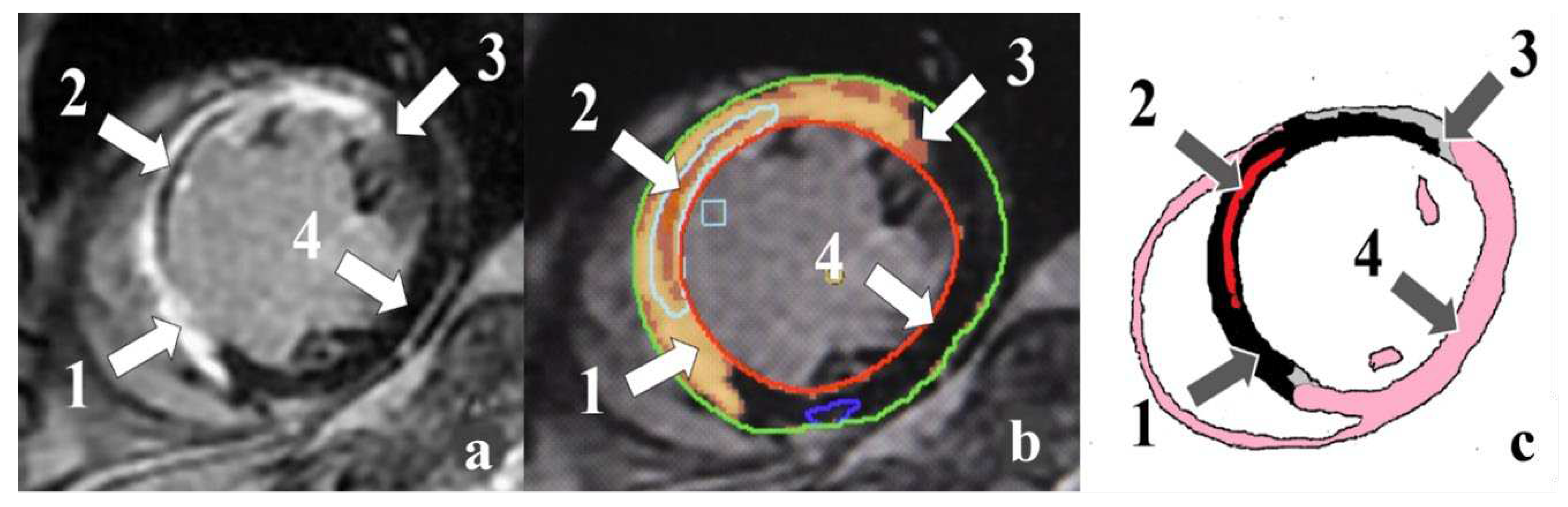
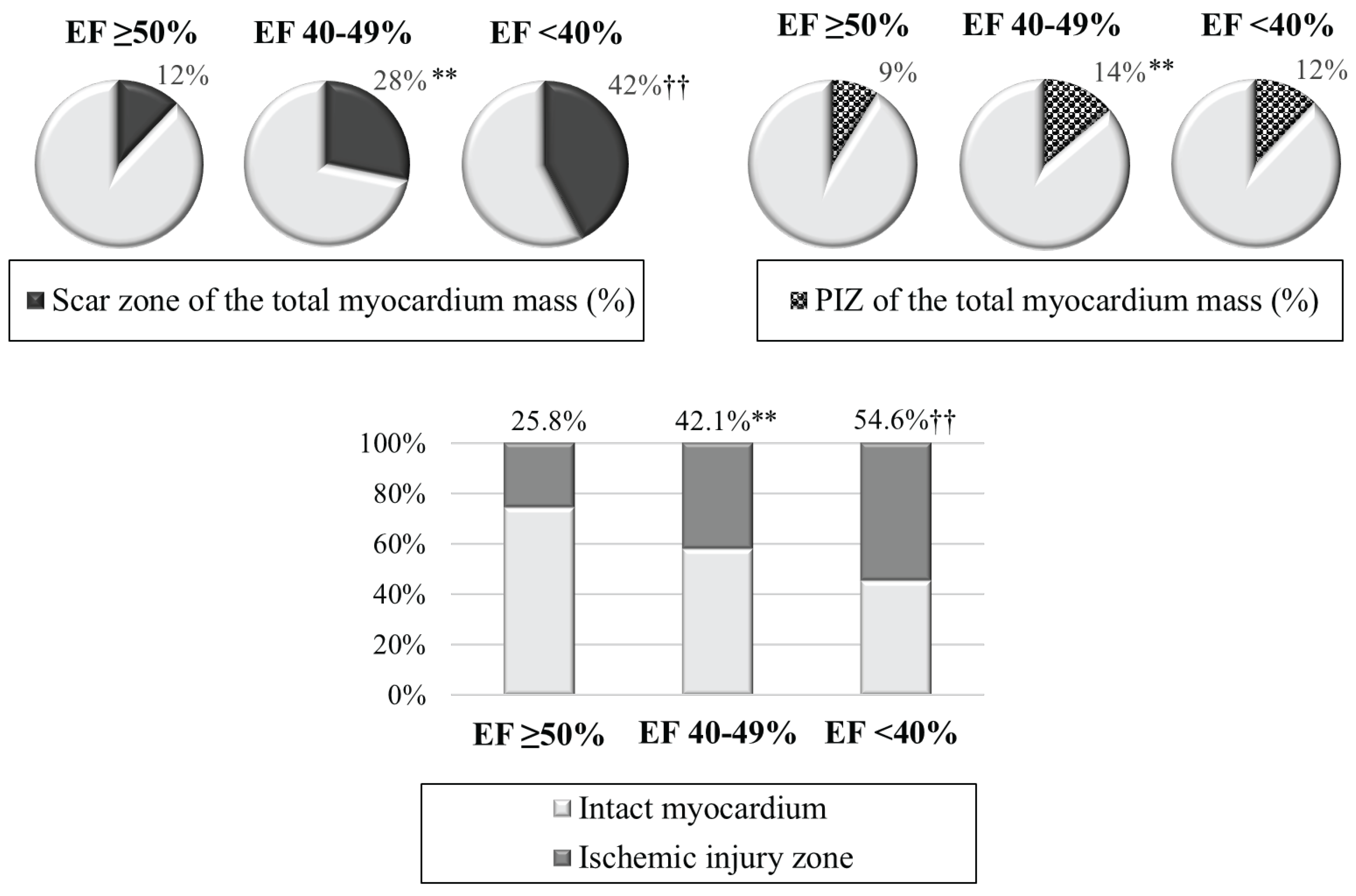
| Cardiac MRI-based parameters of ischemic injury | ||||||
| Scar tissue mass, g | 15.7 (5.6; 24.7) | 41.1 (13.6; 56.4) | 62.5±35.9 | <0.001 | <0.001 | 0.036 |
| PIZ mass, g | 10.4 (5.8; 16.5) | 17.6±7.7 | 17.0±8.0 | <0.001 | 0.089 | 0.839 |
| Ischemic injury mass, g | 27.8 (10.8; 39.8) | 53.9±24.4 | 79.5±35.1 | <0.001 | <0.001 | 0.025 |
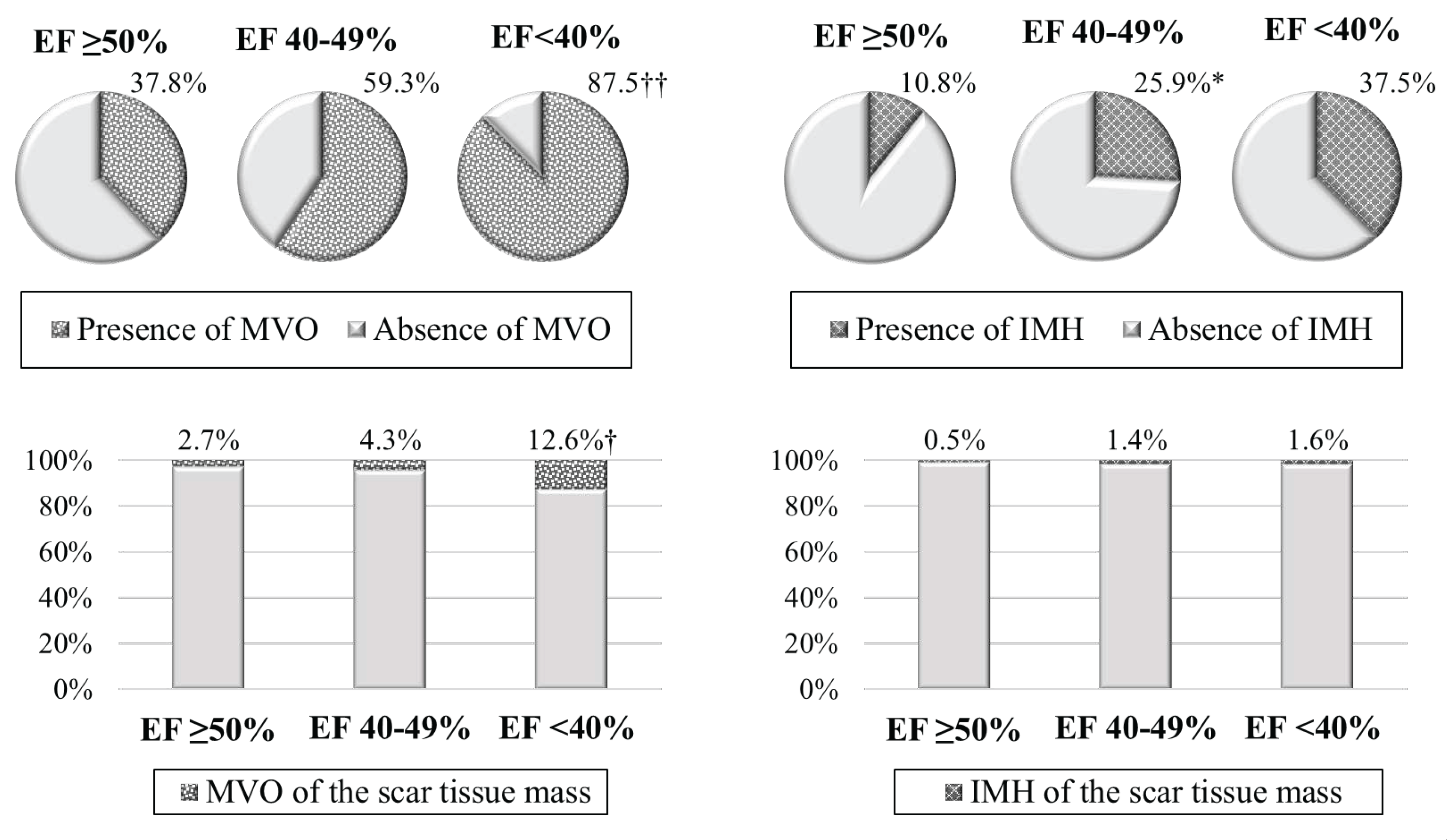
| MVO mass, g | 0.0 (0.0; 1.0) | 1.0 (0.0; 3.1) | 7.3±6.8 | 0.028 | <0.001 | 0.011 |
| IMH mass, g | 0.0 (0.0; 0,1) | 0.0 (0.0; 0.5) | 0.0 (0.0; 3.5) | 0.221 | 0.167 | 0.421 |
| GCI, % | 17.7 (11.8; 29.4) | 34.2±12.2 | 64.0 (41.2; 66.9) | <0.001 | <0.001 | 0.007 |
| Parameter | β | b | p |
|---|---|---|---|
| Gender | 0.242 | 0.361 | 0.011 |
| Pain-to-needle time, min | 0.482 | 0.003 | 0.002 |
| Pain-to-balloon time, min | 0.195 | 0.001 | 0.042 |
| SYNTAX score, points | 0.262 | 0.015 | 0.006 |
| Lesion of ADA, RCA, or any other artery as infarct-related one | 0.197 | 0.104 | 0.039 |
| ESVI, mL/m2 | 0.417 | 0.016 | <0.001 |
| LVMI, g/m2 | 0.230 | 0.008 | 0.016 |
| LCI | 0.574 | 0.017 | <0.001 |
| Scar tissue mass, g | 0.549 | 0.012 | <0.001 |
| Scar zone of the total myocardium mass, % | 0.547 | 0.017 | <0.001 |
| PIZ mass, g | 0.329 | 0.019 | <0.001 |
| PIZ of the total myocardium mass, % | 0.282 | 0.022 | 0.003 |
| Ischemic injury mass, g | 0.548 | 0.009 | <0.001 |
| Ischemic injury of the total myocardium mass, % | 0.529 | 0.013 | <0.001 |
| Presence of MVO | 0.261 | 0.244 | 0.006 |
| MVO mass, g | 0.382 | 0.065 | <0.001 |
| MVO of the scar tissue mass, % | 0.259 | 0.019 | 0.006 |
| IMH mass, g | 0.266 | 0.120 | 0.005 |
| Global contrast index, % | 0.664 | 0.628 | <0.001 |
| HsTI, pg/mL | 0.237 | 0.001 | 0.006 |
| NT-proBNP, pg/mL | 0.325 | 0.001 | 0.013 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




