Submitted:
08 January 2024
Posted:
08 January 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
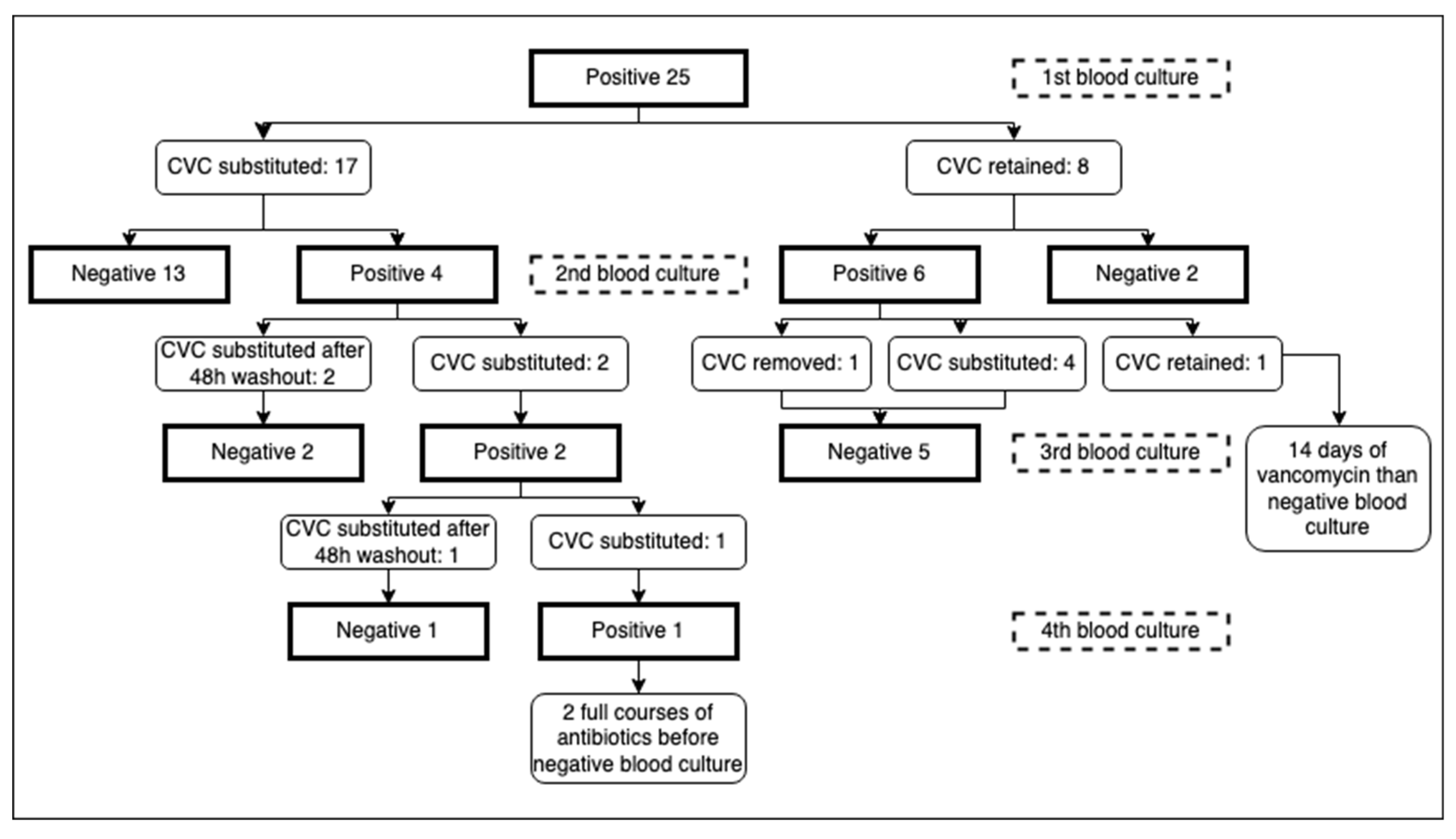
3.1. Catheter Removal
3.2. Clinical Presentation
3.3. Antimicrobial Therapy and Antibiogram
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bizzarro, M.J. Health Care–Associated Infections in the Neonatal Intensive Care Unit: Barriers to Continued Success. Seminars in Perinatology 2012, 36, 437–444. [Google Scholar] [CrossRef] [PubMed]
- Puopolo, K.M.; Benitz, W.E.; Zaoutis, T.E.; COMMITTEE ON FETUS AND NEWBORN; COMMITTEE ON INFECTIOUS DISEASES; Cummings, J.; Juul, S.; Hand, I.; Eichenwald, E.; Poindexter, B.; et al. Management of Neonates Born at ≥35 0/7 Weeks’ Gestation With Suspected or Proven Early-Onset Bacterial Sepsis. Pediatrics 2018, 142, e20182894. [Google Scholar] [CrossRef] [PubMed]
- Boghossian, N.S.; Page, G.P.; Bell, E.F.; Stoll, B.J.; Murray, J.C.; Cotten, C.M.; Shankaran, S.; Walsh, M.C.; Laptook, A.R.; Newman, N.S.; et al. Late-Onset Sepsis in Very Low Birth Weight Infants from Singleton and Multiple-Gestation Births. The Journal of Pediatrics 2013, 162, 1120–1124.e1. [Google Scholar] [CrossRef] [PubMed]
- Fanaroff, A.A.; Korones, S.B.; Wright, L.L.; Verter, J.; Poland, R.L.; Bauer, C.R.; Tyson, J.E.; Philips, J.B.; Edwards, W.; Lucey, J.F.; et al. Incidence, Presenting Features, Risk Factors and Significance of Late Onset Septicemia in Very Low Birth Weight Infants. The National Institute of Child Health and Human Development Neonatal Research Network. Pediatr Infect Dis J 1998, 17, 593–598. [Google Scholar] [CrossRef] [PubMed]
- Flannery, D.D.; Edwards, E.M.; Coggins, S.A.; Horbar, J.D.; Puopolo, K.M. Late-Onset Sepsis Among Very Preterm Infants. Pediatrics 2022, 150, e2022058813. [Google Scholar] [CrossRef] [PubMed]
- Glaser, M.A.; Hughes, L.M.; Jnah, A.; Newberry, D. Neonatal Sepsis: A Review of Pathophysiology and Current Management Strategies. Advances in Neonatal Care 2021, 21, 49–60. [Google Scholar] [CrossRef] [PubMed]
- Manzoni, P.; Luca, D.D.; Stronati, M.; Jacqz-Aigrain, E.; Ruffinazzi, G.; Luparia, M.; Tavella, E.; Boano, E.; Castagnola, E.; Mostert, M.; et al. Prevention of Nosocomial Infections in Neonatal Intensive Care Units. Am J Perinatol 2013, 30, 81–88. [Google Scholar] [CrossRef]
- Dong, Y.; Speer, C.P. Late-Onset Neonatal Sepsis: Recent Developments. Arch Dis Child Fetal Neonatal Ed 2015, 100, F257–263. [Google Scholar] [CrossRef]
- Dong, Y.; Speer, C.P. The Role of Staphylococcus Epidermidis in Neonatal Sepsis: Guarding Angel or Pathogenic Devil? International Journal of Medical Microbiology 2014, 304, 513–520. [Google Scholar] [CrossRef]
- Berardi, A.; Sforza, F.; Baroni, L.; Spada, C.; Ambretti, S.; Biasucci, G.; Bolognesi, S.; Capretti, M.; Carretto, E.; Ciccia, M.; et al. Epidemiology and Complications of Late-Onset Sepsis: An Italian Area-Based Study. PLoS One 2019, 14, e0225407. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, A.; Sousa, E.; Freitas, J.; Viana, M.; Miranda, F.; Silva, F.P. da Positive Blood Culture and Neonatal Sepsis – A Five-Year Study. NASCER E CRESCER - BIRTH AND GROWTH MEDICAL JOURNAL 2022, 31, 106–114. [Google Scholar] [CrossRef]
- Størdal, E.H.; Solevåg, A.L.; Bjørnholt, J.V.; Rønnestad, A.; Stensvold, H.J. Sepsis Treatment Options Identified by 10-Year Study of Microbial Isolates and Antibiotic Susceptibility in a Level-Four Neonatal Intensive Care Unit. Acta Paediatr 2022, 111, 519–526. [Google Scholar] [CrossRef] [PubMed]
- Sands, K.; Carvalho, M.J.; Spiller, O.B.; Portal, E.A.R.; Thomson, K.; Watkins, W.J.; Mathias, J.; Dyer, C.; Akpulu, C.; Andrews, R.; et al. Characterisation of Staphylococci Species from Neonatal Blood Cultures in Low- and Middle-Income Countries. BMC Infect Dis 2022, 22, 593. [Google Scholar] [CrossRef]
- Okomo, U.; Akpalu, E.N.K.; Le Doare, K.; Roca, A.; Cousens, S.; Jarde, A.; Sharland, M.; Kampmann, B.; Lawn, J.E. Aetiology of Invasive Bacterial Infection and Antimicrobial Resistance in Neonates in Sub-Saharan Africa: A Systematic Review and Meta-Analysis in Line with the STROBE-NI Reporting Guidelines. Lancet Infect Dis 2019, 19, 1219–1234. [Google Scholar] [CrossRef]
- Medugu, N.; Iregbu, K.; Tam, P.-Y.I.; Obaro, S. Aetiology of Neonatal Sepsis in Nigeria, and Relevance of Group b Streptococcus: A Systematic Review. PLOS ONE 2018, 13, e0200350. [Google Scholar] [CrossRef] [PubMed]
- Freeman, J.; Platt, R.; Sidebottom, D.G.; Leclair, J.M.; Epstein, M.F.; Goldmann, D.A. Coagulase-Negative Staphylococcal Bacteremia in the Changing Neonatal Intensive Care Unit Population. Is There an Epidemic? JAMA 1987, 258, 2548–2552. [Google Scholar] [CrossRef]
- Healy, C.M.; Baker, C.J.; Palazzi, D.L.; Campbell, J.R.; Edwards, M.S. Distinguishing True Coagulase-Negative Staphylococcus Infections from Contaminants in the Neonatal Intensive Care Unit. J Perinatol 2013, 33, 52–58. [Google Scholar] [CrossRef]
- Ben Said, M.; Hays, S.; Bonfils, M.; Jourdes, E.; Rasigade, J.-P.; Laurent, F.; Picaud, J.-C. Late-Onset Sepsis Due to Staphylococcus Capitis ‘Neonatalis’ in Low-Birthweight Infants: A New Entity? Journal of Hospital Infection 2016, 94, 95–98. [Google Scholar] [CrossRef] [PubMed]
- Butin, M.; Rasigade, J.-P.; Subtil, F.; Martins-Simões, P.; Pralong, C.; Freydière, A.-M.; Vandenesch, F.; Tigaud, S.; Picaud, J.-C.; Laurent, F. Vancomycin Treatment Is a Risk Factor for Vancomycin-Nonsusceptible Staphylococcus Capitis Sepsis in Preterm Neonates. Clinical Microbiology and Infection 2017, 23, 839–844. [Google Scholar] [CrossRef]
- Butin, M.; Rasigade, J.-P.; Martins-Simões, P.; Meugnier, H.; Lemriss, H.; Goering, R.V.; Kearns, A.; Deighton, M.A.; Denis, O.; Ibrahimi, A.; et al. Wide Geographical Dissemination of the Multiresistant Staphylococcus Capitis NRCS-A Clone in Neonatal Intensive-Care Units. Clinical Microbiology and Infection 2016, 22, 46–52. [Google Scholar] [CrossRef]
- Moore, G.; Barry, A.; Carter, J.; Ready, J.; Wan, Y.; Elsayed, M.; Haill, C.; Khashu, M.; Williams, O.M.; Brown, C.S.; et al. Detection, Survival, and Persistence of Staphylococcus Capitis NRCS-A in Neonatal Units in England. J Hosp Infect 2023, 140, 8–14. [Google Scholar] [CrossRef]
- Gras-Le Guen, C.; Fournier, S.; Andre-Richet, B.; Caillon, J.; Chamoux, C.; Espaze, E.; Richet, H.; Roze, J.C.; Lepelletier, D. Almond Oil Implicated in a Staphylococcus Capitis Outbreak in a Neonatal Intensive Care Unit. J Perinatol 2007, 27, 713–717. [Google Scholar] [CrossRef]
- Carter, G.P.; Ussher, J.E.; Da Silva, A.G.; Baines, S.L.; Heffernan, H.; Riley, T.V.; Broadbent, R.; van der Linden, A.; Lee, J.; Monk, I.R.; et al. Genomic Analysis of Multiresistant Staphylococcus Capitis Associated with Neonatal Sepsis. Antimicrob Agents Chemother 2018, 62, e00898-18. [Google Scholar] [CrossRef]
- Lepainteur, M.; Royer, G.; Bourrel, A.S.; Romain, O.; Duport, C.; Doucet-Populaire, F.; Decousser, J.-W. Prevalence of Resistance to Antiseptics and Mupirocin among Invasive Coagulase-Negative Staphylococci from Very Preterm Neonates in NICU: The Creeping Threat? J Hosp Infect 2013, 83, 333–336. [Google Scholar] [CrossRef]
- Butin, M.; Dumont, Y.; Monteix, A.; Raphard, A.; Roques, C.; Martins Simoes, P.; Picaud, J.-C.; Laurent, F. Sources and Reservoirs of Staphylococcus Capitis NRCS-A inside a NICU. Antimicrob Resist Infect Control 2019, 8, 157. [Google Scholar] [CrossRef] [PubMed]
- D’mello, D.; Daley, A.J.; Rahman, M.S.; Qu, Y.; Garland, S.; Pearce, C.; Deighton, M.A. Vancomycin Heteroresistance in Bloodstream Isolates of Staphylococcus Capitis. Journal of Clinical Microbiology 2008, 46, 3124–3126. [Google Scholar] [CrossRef]
- Van Der Zwet, W.C.; Debets-Ossenkopp, Y.J.; Reinders, E.; Kapi, M.; Savelkoul, P.H.M.; Van Elburg, R.M.; Hiramatsu, K.; Vandenbroucke-Grauls, C.M.J.E. Nosocomial Spread of a Staphylococcus Capitis Strain with Heteroresistance to Vancomycin in a Neonatal Intensive Care Unit. Journal of Clinical Microbiology 2002, 40, 2520–2525. [Google Scholar] [CrossRef] [PubMed]
- Decalonne, M.; Dos Santos, S.; Gimenes, R.; Goube, F.; Abadie, G.; Aberrane, S.; Ambrogi, V.; Baron, R.; Barthelemy, P.; Bauvin, I.; et al. Staphylococcus Capitis Isolated from Bloodstream Infections: A Nationwide 3-Month Survey in 38 Neonatal Intensive Care Units. Eur J Clin Microbiol Infect Dis 2020, 39, 2185–2194. [Google Scholar] [CrossRef]
- Rasigade, J.-P.; Raulin, O.; Picaud, J.-C.; Tellini, C.; Bes, M.; Grando, J.; Said, M.B.; Claris, O.; Etienne, J.; Tigaud, S.; et al. Methicillin-Resistant Staphylococcus Capitis with Reduced Vancomycin Susceptibility Causes Late-Onset Sepsis in Intensive Care Neonates. PLoS ONE 2012, 7, e31548–e31548. [Google Scholar] [CrossRef] [PubMed]
- Qu, Y.; Daley, A.J.; Istivan, T.S.; Garland, S.M.; Deighton, M.A. Antibiotic Susceptibility of Coagulase-Negative Staphylococci Isolated from Very Low Birth Weight Babies: Comprehensive Comparisons of Bacteria at Different Stages of Biofilm Formation. Ann Clin Microbiol Antimicrob 2010, 9, 1–12. [Google Scholar] [CrossRef]
- Cui, B.; Smooker, P.M.; Rouch, D.A.; Daley, A.J.; Deighton, M.A. Differences between Two Clinical Staphylococcus Capitis Subspecies as Revealed by Biofilm, Antibiotic Resistance, and Pulsed-Field Gel Electrophoresis Profiling. J Clin Microbiol 2013, 51, 9–14. [Google Scholar] [CrossRef]
- França, A. The Role of Coagulase-Negative Staphylococci Biofilms on Late-Onset Sepsis: Current Challenges and Emerging Diagnostics and Therapies. Antibiotics (Basel) 2023, 12, 554. [Google Scholar] [CrossRef]
- Hocevar, S.N.; Edwards, J.R.; Horan, T.C.; Morrell, G.C.; Iwamoto, M.; Lessa, F.C. Device-Associated Infections among Neonatal Intensive Care Unit Patients: Incidence and Associated Pathogens Reported to the National Healthcare Safety Network, 2006-2008. Infect Control Hosp Epidemiol 2012, 33, 1200–1206. [Google Scholar] [CrossRef]
- Horan, T.C.; Andrus, M.; Dudeck, M.A. CDC/NHSN Surveillance Definition of Health Care-Associated Infection and Criteria for Specific Types of Infections in the Acute Care Setting. Am J Infect Control 2008, 36, 309–332. [Google Scholar] [CrossRef]
- Mermel, L.A.; Allon, M.; Bouza, E.; Craven, D.E.; Flynn, P.; O’Grady, N.P.; Raad, I.I.; Rijnders, B.J.A.; Sherertz, R.J.; Warren, D.K. Clinical Practice Guidelines for the Diagnosis and Management of Intravascular Catheter-Related Infection: 2009 Update by the Infectious Diseases Society of America. Clinical Infectious Diseases 2009, 49, 1–45. [Google Scholar] [CrossRef]
- Vasudevan, C.; Oddie, S.J.; McGuire, W. Early Removal versus Expectant Management of Central Venous Catheters in Neonates with Bloodstream Infection. Cochrane Database of Systematic Reviews 2016, 2016. [Google Scholar] [CrossRef] [PubMed]
- Benjamin, D.K., Jr.; Miller, W.; Garges, H.; Benjamin, D.K.; McKinney, R.E., Jr.; Cotton, M.; Fisher, R.G.; Alexander, K.A. Bacteremia, Central Catheters, and Neonates: When to Pull the Line. Pediatrics 2001, 107, 1272–1276. [Google Scholar] [CrossRef] [PubMed]
- Ng, P.C.; Chow, V.C.Y.; Lee, C.H.; Ling, J.M.L.; Wong, H.L.; Chan, R.C.Y. PERSISTENT STAPHYLOCOCCUS CAPITIS SEPTICEMIA IN A PRETERM INFANT. Pediatric Infectious Disease Journal 2006, 25, 652–654. [Google Scholar] [CrossRef]
- Karlowicz, M.G.; Hashimoto, L.N.; Kelly, R.E.; Buescher, E.S. Should Central Venous Catheters Be Removed as Soon as Candidemia Is Detected in Neonates? Pediatrics 2000, 106, E63. [Google Scholar] [CrossRef] [PubMed]
- Nazemi, K.J.; Buescher, E.S.; Kelly, R.E.; Karlowicz, M.G. Central Venous Catheter Removal versus in Situ Treatment in Neonates with Enterobacteriaceae Bacteremia. Pediatrics 2003, 111, e269–274. [Google Scholar] [CrossRef] [PubMed]
- Sc, E.; Jl, T.; Lt, G. Outcome of Treatment of Candidemia in Children Whose Central Catheters Were Removed or Retained. The Pediatric infectious disease journal 1989, 8. [Google Scholar]
- Boussamet, L.; Launay, E.; Thomas, E.; Leguen, C.G.; Lepelletier, D. Should Central Venous Catheters Be Rapidly Removed to Treat Staphylococcus Aureus Related-Catheter Bloodstream Infection (CR-BSI) in Neonates and Children? An 8-Year Period (2010–2017) Retrospective Analysis in a French University Hospital. Journal of Hospital Infection 2019, 103, 97–100. [Google Scholar] [CrossRef] [PubMed]
- Rubin, L.G.; Sánchez, P.J.; Siegel, J.; Levine, G.; Saiman, L.; Jarvis, W.R.; the Pediatric Prevention Network. Evaluation and Treatment of Neonates With Suspected Late-Onset Sepsis: A Survey of Neonatologists’ Practices. Pediatrics 2002, 110, e42. [Google Scholar] [CrossRef]
- Karlowicz, M.G.; Furigay, P.J.; Croitoru, D.P.; Buescher, E.S. Central Venous Catheter Removal versus in Situ Treatment in Neonates with Coagulase-Negative Staphylococcal Bacteremia. Pediatr Infect Dis J 2002, 21, 22–27. [Google Scholar] [CrossRef] [PubMed]
- Deshpande, P.; Jain, A.; Shah, P.S. Outcomes Associated with Early Removal versus Retention of Peripherally Inserted Central Catheters after Diagnosis of Catheter-Associated Infections in Neonates. The Journal of Maternal-Fetal & Neonatal Medicine 2016, 29, 4082–4087. [Google Scholar] [CrossRef]
- İşgüder, R.; Devrim, İ.; Ceylan, G.; Kara, A.; Gülfidan, G.; Ağın, H. Risk Factors for Recurrent Central Line-Associated Bloodstream Infections in a Pediatric Intensive Care Unit. Turk J Med Sci 2017, 47, 1128–1136. [Google Scholar] [CrossRef]
- Zhong, Y.; Deng, L.; Zhou, L.; Liao, S.; Yue, L.; Wen, S.W.; Xie, R.; Lu, Y.; Zhang, L.; Tang, J.; et al. Association of Immediate Reinsertion of New Catheters with Subsequent Mortality among Patients with Suspected Catheter Infection: A Cohort Study. Annals of Intensive Care 2022, 12, 38. [Google Scholar] [CrossRef]
- Chin, B.S.; Han, S.H.; Lee, H.S.; Jeong, S.J.; Choi, H.; Kim, C.O.; Choi, J.Y.; Song, Y.G.; Kim, J.M. Risk Factors for Recurrent Catheter-Related Infections after Catheter-Related Bloodstream Infections. Int J Infect Dis 2010, 14, e16–21. [Google Scholar] [CrossRef]
- Lee, Y.-M.; Ryu, B.-H.; Hong, S.I.; Cho, O.-H.; Hong, K.-W.; Bae, I.-G.; Kwack, W.G.; Kim, Y.J.; Chung, E.K.; Kim, D.Y.; et al. Clinical Impact of Early Reinsertion of a Central Venous Catheter after Catheter Removal in Patients with Catheter-Related Bloodstream Infections. Infection Control & Hospital Epidemiology 2021, 42, 162–168. [Google Scholar] [CrossRef]
- Stoll, B.J.; Hansen, N.; Fanaroff, A.A.; Wright, L.L.; Carlo, W.A.; Ehrenkranz, R.A.; Lemons, J.A.; Donovan, E.F.; Stark, A.R.; Tyson, J.E.; et al. Late-Onset Sepsis in Very Low Birth Weight Neonates: The Experience of the NICHD Neonatal Research Network. Pediatrics 2002, 110, 285–291. [Google Scholar] [CrossRef]
- Laurent, F.; Butin, M. Staphylococcus Capitis and NRCS-A Clone: The Story of an Unrecognized Pathogen in Neonatal Intensive Care Units. Clinical Microbiology and Infection 2019, 25, 1081–1085. [Google Scholar] [CrossRef] [PubMed]
| 2019 | 2020 | 2021 | 2022 | |
|---|---|---|---|---|
| n. of S. capitis CLABSI (% of total) | 5 (33,3) | 5 (20,8) | 9 (36) | 6 (42,9) |
| n. of CoNS CLABSI | 9 | 18 | 16 | 11 |
| Total n. of CLABSI | 15 | 24 | 25 | 14 |
| n. tot = 25 | |
|---|---|
| F (%) | 10 (40) |
| M (%) | 15 (60) |
| Gestational age (range) | 28 (24+1 – 38+6) |
| < 28 wks (%) | 11 (44) |
| 28-32 wks (%) | 9 (36) |
| 32-35 wks (%) | 1 (4) |
| 35.37 wks (%) | 2 (8) |
| > 37 wks (%) | 2 (8) |
| Weight (range) | 885 (491-2950) |
| < 1000 gr (%) | 14 (56) |
| 1000 – 1500 gr (%) | 6 (24) |
| >1500 gr (%) | 5 (20) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




