Submitted:
04 December 2023
Posted:
05 December 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Study Population and Sample Size
2.3. Ethical Considerations
2.4. Diabetes Self-Management Questionnaire (DSMQ)
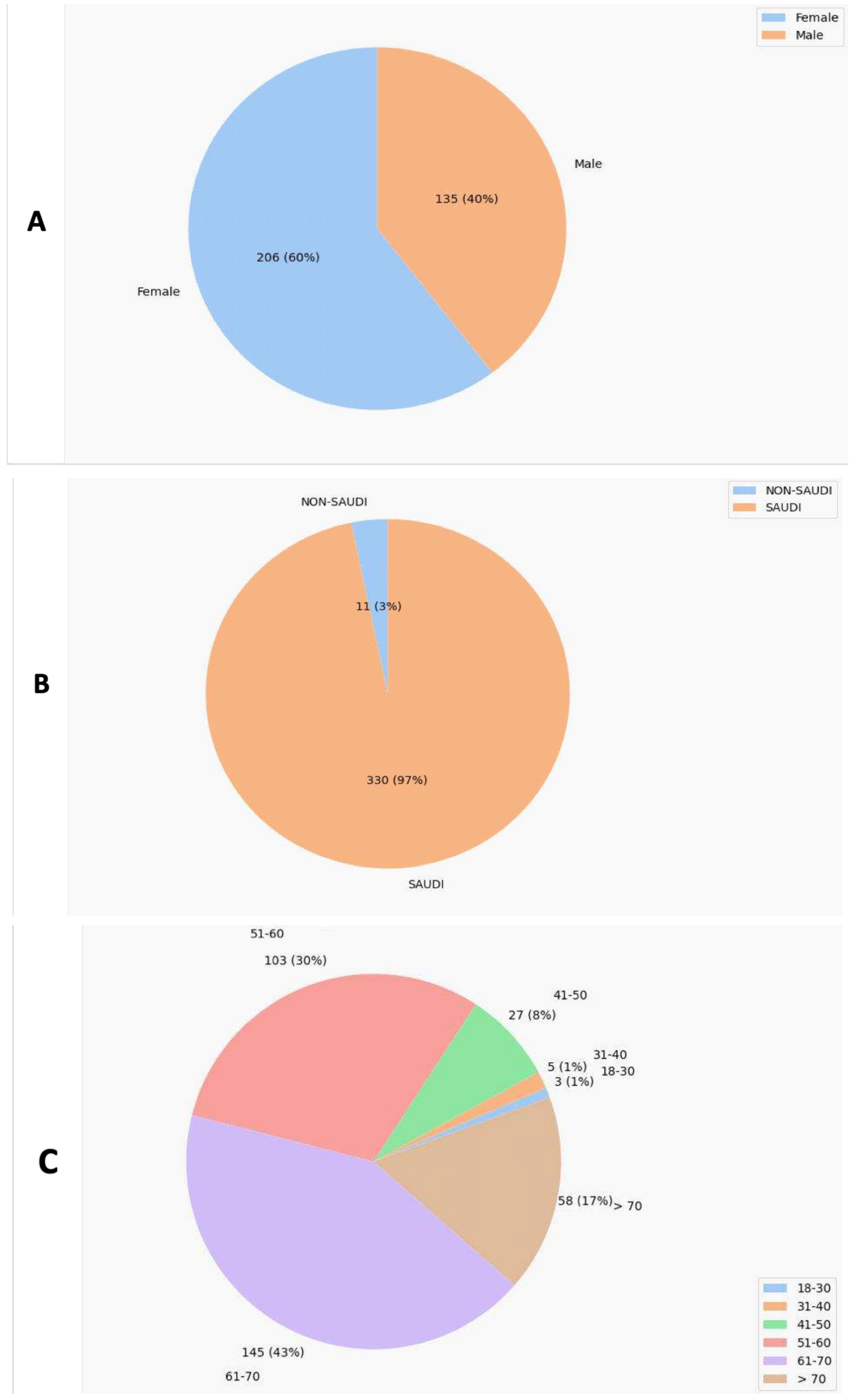
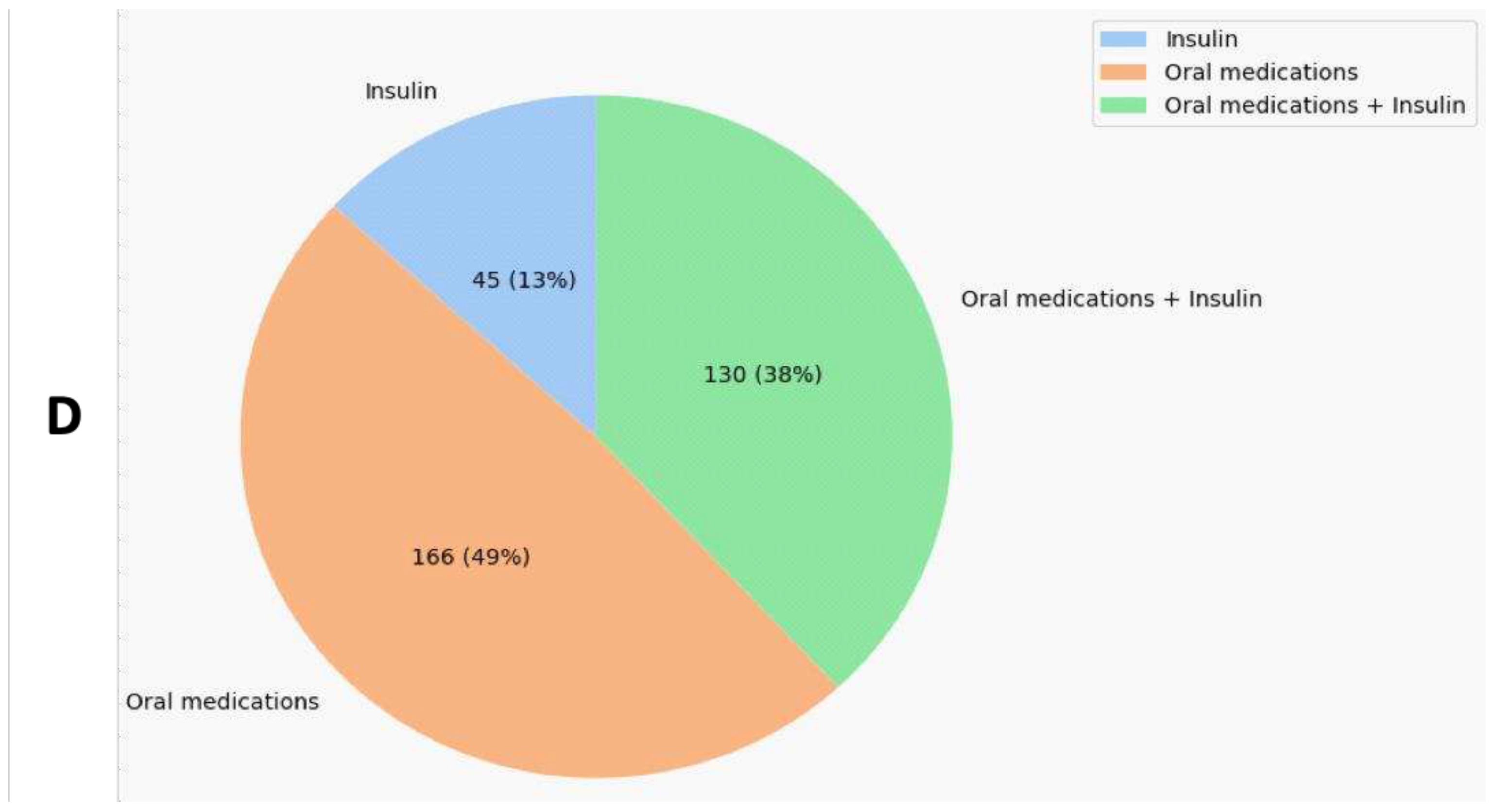
2.5. Participant Demographics
- 129 responses had missing/incomplete values on important questionnaire items.
- 36 patients gave their responses twice or three times. Upon examining these duplicates, some responses had discrepancies in demographic information such as gender, age, nationality, how long they had diabetes, and the type of medications they are currently taking for diabetes. Accordingly, these duplicates were filtered by selecting the earliest response and correcting the demographic information according to the hospital system and physician/patient notes.
2.6. Data Analysis
2.7. Software
2.8. Statistical Analysis
3. Results
3.1. Study Overview
3.2. Study Findings in Comparison with Relevant Previous Studies
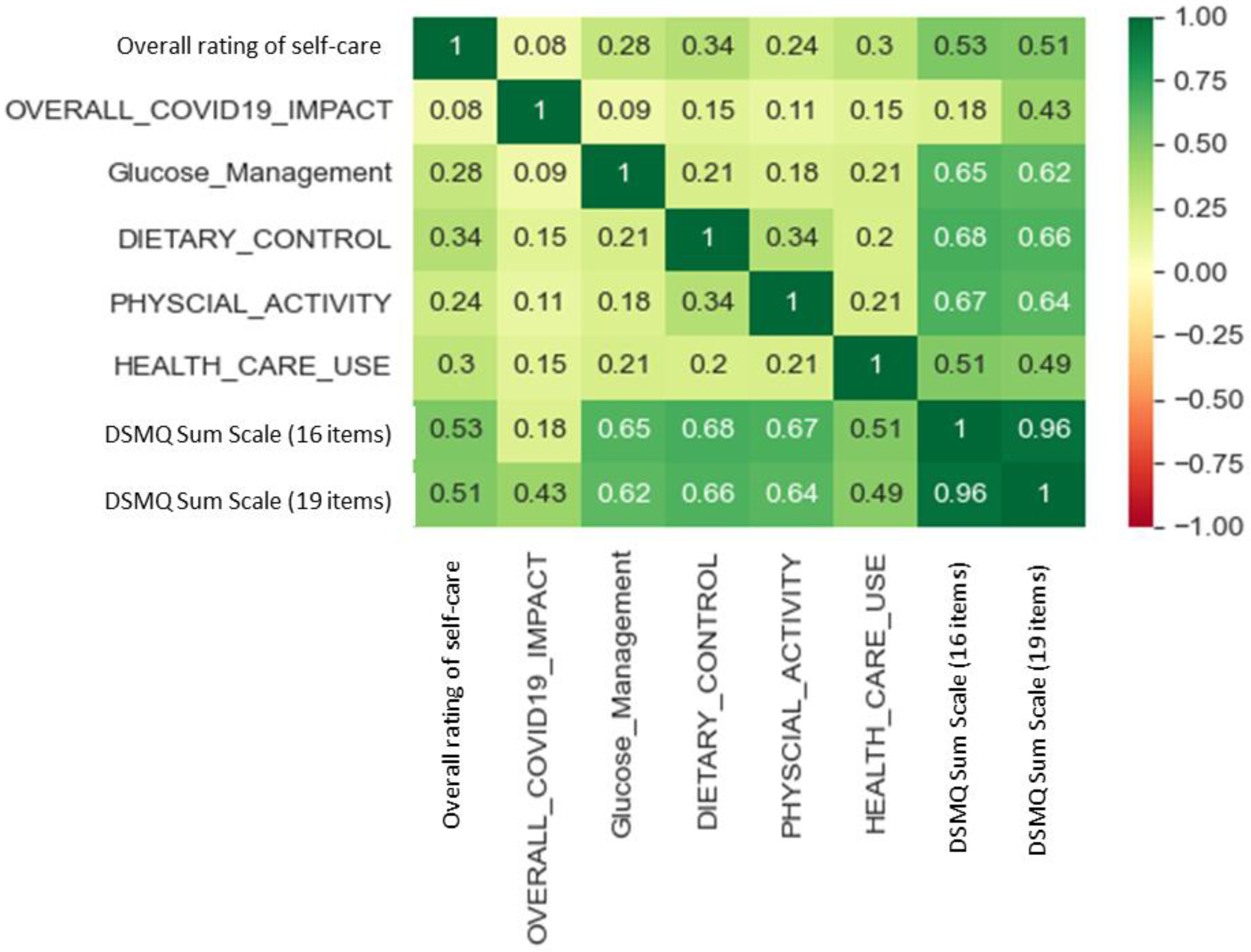
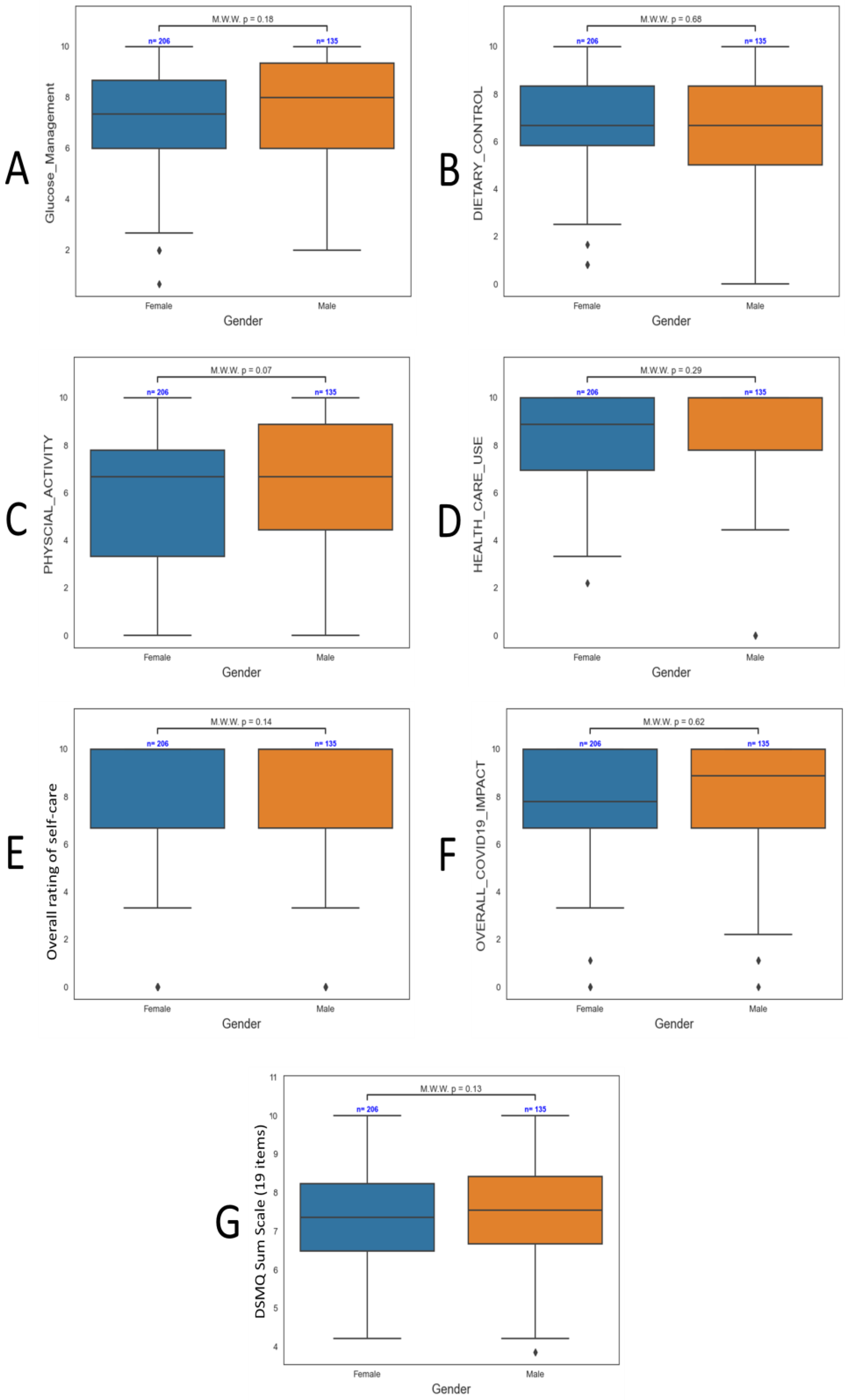
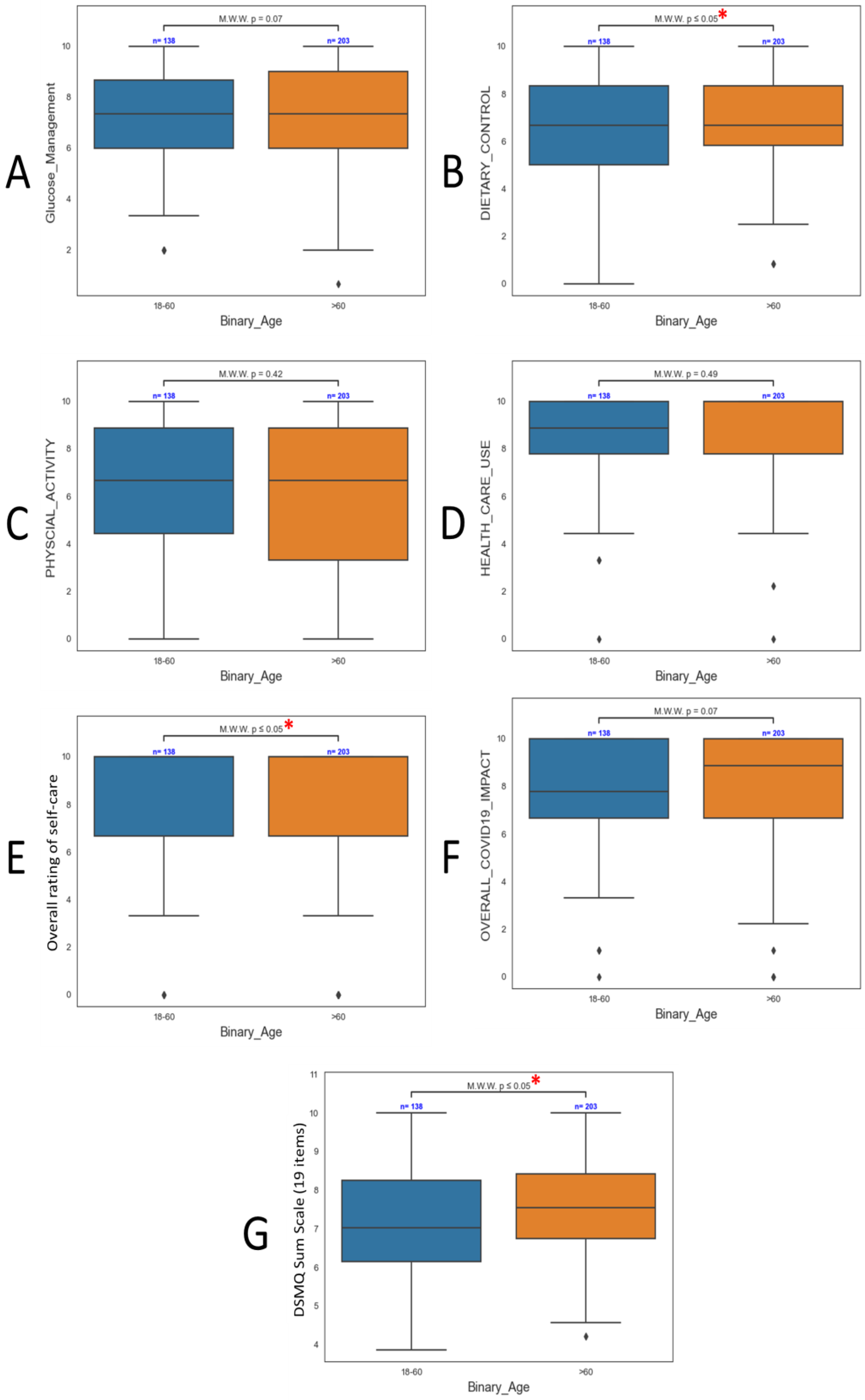
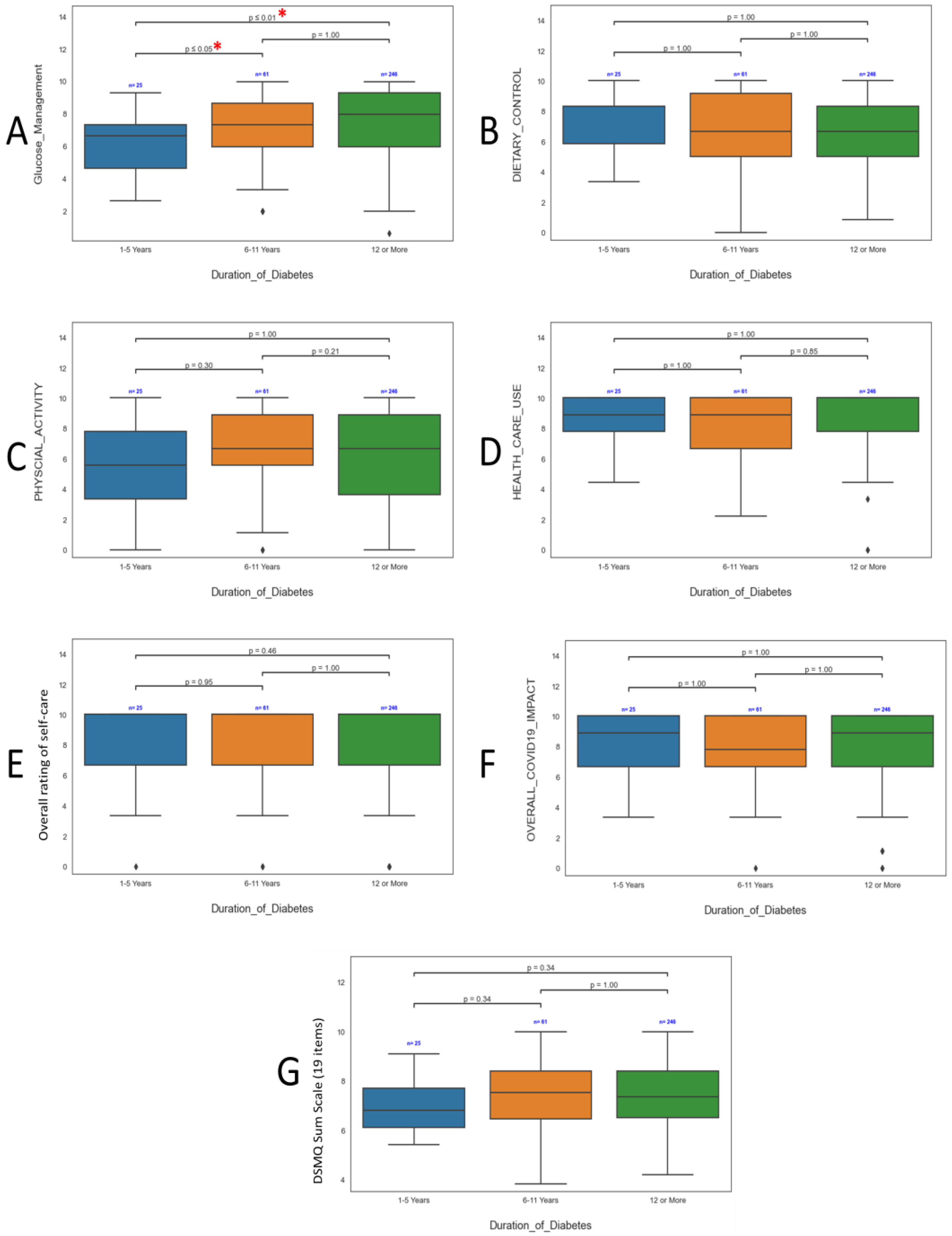
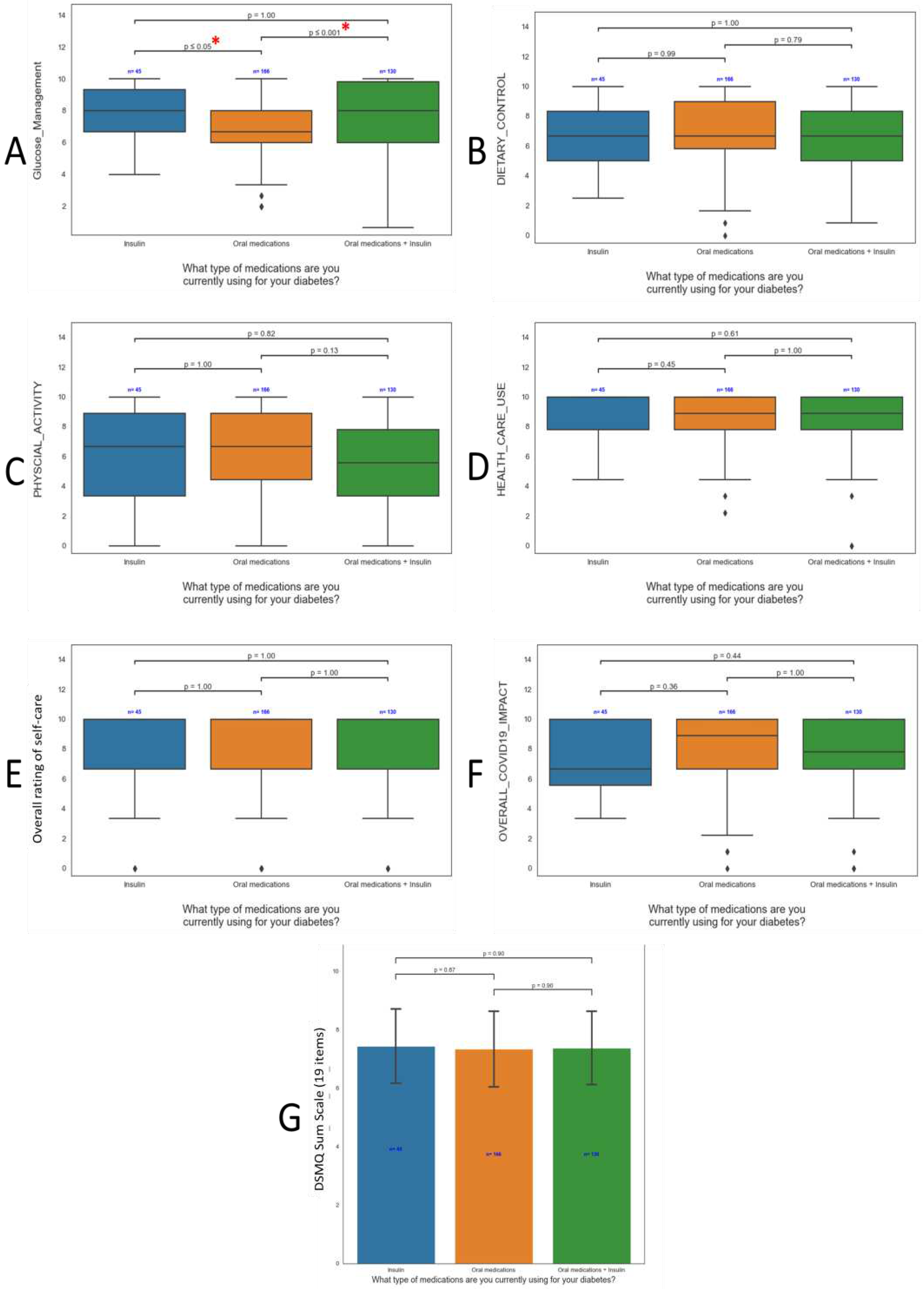
3.3. Influence of Patient Demographics on DSMQ Findings
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Mohseni, M., et al., Challenges of routine diabetes care during COVID-19 era: A systematic search and narrative review. Prim Care Diabetes, 2021. 15(6): p. 918-922. https://doi.org/10.1016/j.pcd.2021.07.017. [CrossRef]
- Vamos, E.P. and K. Khunti, Indirect effects of the COVID-19 pandemic on people with type 2 diabetes: time to urgently move into a recovery phase. BMJ Qual Saf, 2022. 31(7): p. 483-485. https://doi.org/10.1136/bmjqs-2021-014079. [CrossRef]
- Mafi, J.N., et al., Trends in US Ambulatory Care Patterns During the COVID-19 Pandemic, 2019-2021. JAMA, 2022. 327(3): p. 237-247. https://doi.org/10.1001/jama.2021.24294. [CrossRef]
- Molina, M., et al., Analysis of Emergency Department Encounters Among High Users of Health Care and Social Service Systems Before and During the COVID-19 Pandemic. JAMA Netw Open, 2022. 5(10): p. e2239076. https://doi.org/10.1001/jamanetworkopen.2022.39076. [CrossRef]
- Zachrison, K.S., Z. Yan, and L.H. Schwamm, Changes in Virtual and In-Person Health Care Utilization in a Large Health System During the COVID-19 Pandemic. JAMA Netw Open, 2021. 4(10): p. e2129973. https://doi.org/10.1001/jamanetworkopen.2021.29973. [CrossRef]
- Khunti, K., et al., The impact of the COVID-19 pandemic on diabetes services: planning for a global recovery. Lancet Diabetes Endocrinol, 2022. 10(12): p. 890-900. https://doi.org/10.1016/S2213-8587(22)00278-9. [CrossRef]
- Distaso, W., et al., Diabetes self-management during the COVID-19 pandemic and its associations with COVID-19 anxiety syndrome, depression and health anxiety. Diabet Med, 2022. 39(10): p. e14911. doi: 10.1111/dme.14911. [CrossRef]
- Zupa, M.F., et al., Changes in Self-management During the COVID-19 Pandemic Among Adults with Type 2 Diabetes at a Federally Qualified Health Center. J Immigr Minor Health, 2022. 24(5): p. 1375-1378. https://doi.org/10.1007/s10903-022-01351-7. [CrossRef]
- Alkhormi, A.H., et al., Psychological Health and Diabetes Self-Management among Patients with Type 2 Diabetes during COVID-19 in the Southwest of Saudi Arabia. Medicina (Kaunas), 2022. 58(5). https://doi.org/10.3390/medicina58050675. [CrossRef]
- Fatani, B., et al., Behavioral Changes in Patients With Diabetes During the COVID-19 Pandemic in Saudi Arabia: A Cross-Sectional Study. Cureus, 2023. 15(2): p. e34956. https://doi.org/10.7759/cureus.34956. [CrossRef]
- Al-Daghri, N.M., et al., COVID-19 Lockdown and Lifestyle Changes in Saudi Adults With Types 1 and 2 Diabetes. Front Public Health, 2022. 10: p. 912816. https://doi.org/10.3389/fpubh.2022.912816. [CrossRef]
- Alshareef, R., et al., Impact of the COVID-19 lockdown on diabetes patients in Jeddah, Saudi Arabia. Diabetes Metab Syndr, 2020. 14(5): p. 1583-1587. https://doi.org/10.1016/j.dsx.2020.07.051. [CrossRef]
- Schmitt, A., et al., The Diabetes Self-Management Questionnaire (DSMQ): development and evaluation of an instrument to assess diabetes self-care activities associated with glycaemic control. Health Qual Life Outcomes, 2013. 11: p. 138. https://doi.org/10.1186/1477-7525-11-138. [CrossRef]
- Almigbal, T.H., et al., Association of health literacy and self-management practices and psychological factor among patients with type 2 diabetes mellitus in Saudi Arabia. Saudi Med J, 2019. 40(11): p. 1158-1166. https://doi.org/10.15537/smj.2019.11.24585. [CrossRef]
- Schmitt, A., et al., A Self-Report Measure of Diabetes Self-Management for Type 1 and Type 2 Diabetes: The Diabetes Self-Management Questionnaire-Revised (DSMQ-R) - Clinimetric Evidence From Five Studies. Front Clin Diabetes Healthc, 2021. 2: p. 823046. https://doi.org/10.3389/fcdhc.2021.823046. [CrossRef]
- Al-Qahtani, A.M., Frequency and factors associated with inadequate self-care behaviors in patients with type 2 diabetes mellitus in Najran, Saudi Arabia. Based on diabetes self-management questionnaire. Saudi Med J, 2020. 41(9): p. 955-964. doi: 10.15537/smj.2020.9.25339. [CrossRef]
- Al-Khaledi, M., et al., Diabetes Self-Management: A Key to Better Health-Related Quality of Life in Patients with Diabetes. Med Princ Pract, 2018. 27(4): p. 323-331. https://doi.org/10.1159/000489310. [CrossRef]
- Al-Hadhrami, R., O. Al-Rawajfah, and J. Muliira, Diabetes Self-Management and the Associated Factors Among Adult Omanis with Type 1 Diabetes. Sultan Qaboos Univ Med J, 2020. 20(4): p. e339-e345. https://doi.org/10.18295/squmj.2020.20.04.010. [CrossRef]
- Mishra, P., et al., Descriptive statistics and normality tests for statistical data. Ann Card Anaesth, 2019. 22(1): p. 67-72. doi: 10.4103/aca.ACA_157_18. [CrossRef]
- McHugh, M.L., The chi-square test of independence. Biochem Med (Zagreb), 2013. 23(2): p. 143-9. doi:10.11613/bm.2013.018. [CrossRef]
- Anderson, M.R., et al., Determining Success or Failure After Foot and Ankle Surgery Using Patient Acceptable Symptom State (PASS) and Patient Reported Outcome Information System (PROMIS). Foot Ankle Int, 2018. 39(8): p. 894-902. https://doi.org/10.1177/1071100718769666. [CrossRef]
- Nahm, F.S., Nonparametric statistical tests for the continuous data: the basic concept and the practical use. Korean J Anesthesiol, 2016. 69(1): p. 8-14. https://doi.org/10.4097/kjae.2016.69.1.8. [CrossRef]
- Schober, P., C. Boer, and L.A. Schwarte, Correlation Coefficients: Appropriate Use and Interpretation. Anesth Analg, 2018. 126(5): p. 1763-1768. doi:10.1213/ane.0000000000002864. [CrossRef]
- Utli, H. and B. Vural Doğru, The effect of the COVID-19 pandemic on self-management in patients with type 2 diabetics. Prim Care Diabetes, 2021. 15(5): p. 799-805. https://doi.org/10.1016/j.pcd.2021.07.009. [CrossRef]
- Alhussein, N.A., et al., Diabetes Self-Management Among Healthcare Providers in King Abdulaziz Medical City, Riyadh: A Cross-Sectional Pilot Study. Cureus, 2021. 13(9): p. e18155. https://doi.org/10.7759/cureus.18155. [CrossRef]
- Alodhayani, A., et al., Association between self-care management practices and glycemic control of patients with type 2 diabetes mellitus in Saud Arabia: A cross -sectional study. Saudi J Biol Sci, 2021. 28(4): p. 2460-2465. https://doi.org/10.1016/j.sjbs.2021.01.047. [CrossRef]
- Alruhaim, H.Y., et al., The association between diabetes numeracy and diabetes self-management among Saudi adults with insulin-treated diabetes. Saudi Med J, 2021. 42(5): p. 517-525. https://doi.org/10.15537/smj.2021.42.5.20200422. [CrossRef]
- Shi, C., et al., Barriers to Self-Management of Type 2 Diabetes During COVID-19 Medical Isolation: A Qualitative Study. Diabetes Metab Syndr Obes, 2020. 13: p. 3713-3725. https://doi.org/10.2147/dmso.s268481. [CrossRef]
- Olesen, K., et al., How has the COVID-19 Pandemic Affected Diabetes Self-Management in People With Diabetes? - A One-Year Follow-Up Study. Front Clin Diabetes Healthc, 2022. 3: p. 867025. https://doi.org/10.3389/fcdhc.2022.867025. [CrossRef]
- Oraibi, O., et al., Impact of COVID-19 on Patients with Diabetes Standard of Care in the Jazan Region, Saudi Arabia. Mater Sociomed, 2022. 34(4): p. 272-277. https://doi.org/10.5455/msm.2022.34.272-277. [CrossRef]
- ElSayed, N.A., et al., 5. Facilitating Positive Health Behaviors and Well-being to Improve Health Outcomes: Standards of Care in Diabetes—2023. Diabetes Care, 2022. 46(Supplement_1): p. S68-S96. https://doi.org/10.2337/dc24-s005. [CrossRef]
- Boulé, N.G., et al., Effects of exercise on glycemic control and body mass in type 2 diabetes mellitus: a meta-analysis of controlled clinical trials. Jama, 2001. 286(10): p. 1218-27. https://doi.org/10.1034/j.1600-0838.2002.120111_3.x. [CrossRef]
- Franz, M.J., et al., Academy of Nutrition and Dietetics Nutrition Practice Guideline for Type 1 and Type 2 Diabetes in Adults: Systematic Review of Evidence for Medical Nutrition Therapy Effectiveness and Recommendations for Integration into the Nutrition Care Process. J Acad Nutr Diet, 2017. 117(10): p. 1659-1679. https://doi.org/10.1016/j.jand.2017.03.022. [CrossRef]
- Vision, K., 2030 Strategic Objectives and Vision Realization Programs. 2021.
- Chowdhury, S., D. Mok, and L. Leenen, Transformation of health care and the new model of care in Saudi Arabia: Kingdom's Vision 2030. J Med Life, 2021. 14(3): p. 347-354. https://doi.org/10.25122/jml-2021-0070. [CrossRef]
- Alshaya, O.A., et al., Ambulatory care pharmacy in Saudi Arabia; definition, history, present, future potentials, and expected challenges. JACCP: JOURNAL OF THE AMERICAN COLLEGE OF CLINICAL PHARMACY, 2022. 5(3): p. 332-341. https://doi.org/10.1002/jac5.1577. [CrossRef]
| Item code* | Item statement |
| Q1 | I check my blood sugar levels with care and attention. |
| Q2 | The food I choose to eat makes it easy to achieve optimal blood sugar levels. |
| Q3 | I keep all doctors’ appointments recommended for my diabetes treatment. |
| Q4 | I take my diabetes medication (e. g. insulin, tablets) as prescribed. |
| rQ5 | Occasionally I eat lots of sweets or other foods rich in carbohydrates. |
| Q6 | I record my blood sugar levels regularly (or analyze the value chart with my blood glucose meter). |
| rQ7 | I tend to avoid diabetes-related doctors’ appointments. |
| Q8 | I do regular physical activity to achieve optimal blood sugar levels. |
| Q9 | I strictly follow the dietary recommendations given by my doctor or diabetes specialist. |
| rQ10 | I do not check my blood sugar levels frequently enough as would be required for achieving good blood glucose control. |
| rQ11 | I avoid physical activity, although it would improve my diabetes.', |
| rQ12 | I tend to forget to take or skip my diabetes medication (e. g. insulin, tablets). |
| rQ13 | Sometimes I have real ‘food binges’ (not triggered by low blood sugar)', |
| rQ14 | Regarding my diabetes care, I should see my medical practitioner(s) more often. |
| rQ15 | I tend to skip planned physical activity. |
| rQ16 | My diabetes self-care is poor. |
| rQ17 | The COVID-19 pandemic negatively affected my diabetes control. |
| rQ18 | The COVID-19 pandemic negatively affected my exercise regimen. |
| rQ19 | The COVID-19 pandemic negatively affected my ability to follow a diet (for my Diabetes). |
| parameters | Q1 | Q2 | rQ3 | Q4 | Q5 | Q6 | rQ7 | Q8 | Q9 | rQ10 | rQ11 | rQ12 | rQ13 | rQ14 | rQ15 | rQ16 | rQ17 | rQ18 | rQ19 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| mean | 1.98 | 1.76 | 2.68 | 2.77 | 2.24 | 1.30 | 2.83 | 1.33 | 1.77 | 2.36 | 2.13 | 2.61 | 2.40 | 2.23 | 2.04 | 2.53 | 2.40 | 2.21 | 2.42 |
| std | 1.08 | 1.00 | 0.74 | 0.59 | 0.91 | 1.26 | 0.61 | 1.12 | 1.06 | 0.90 | 1.04 | 0.81 | 0.93 | 1.08 | 1.06 | 0.79 | 0.89 | 0.96 | 0.83 |
| min | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 |
| 25% | 1.00 | 1.00 | 3.00 | 3.00 | 2.00 | 0.00 | 3.00 | 0.00 | 1.00 | 2.00 | 2.00 | 3.00 | 2.00 | 2.00 | 1.00 | 2.00 | 2.00 | 2.00 | 2.00 |
| 50% | 2.00 | 2.00 | 3.00 | 3.00 | 2.00 | 1.00 | 3.00 | 1.00 | 2.00 | 3.00 | 2.00 | 3.00 | 3.00 | 3.00 | 2.00 | 3.00 | 3.00 | 3.00 | 3.00 |
| 75% | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 2.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 |
| max | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 | 3.00 |
| Parameters | Items* | n | Cronbach's alpha |
|---|---|---|---|
| Glucose Management | Q1, Q4, Q6, rQ10, rQ12 | 5 | 0.577 |
| Dietary Control | Q2, rQ5, Q9, rQ13 | 4 | 0.578 |
| Physical Activity | Q8, rQ11, rQ15 | 3 | 0.758 |
| Health Care Use | Q3, rQ7, rQ14 | 3 | 0.262 |
| Overall rating of self-care | rQ16 | 1 | NA |
| DSMQ Sum Scale (16 items) | Q1, Q2, Q3, Q4, rQ5, Q6, rQ7, Q8, Q9, rQ10, rQ11, rQ12rQ13, rQ14, rQ15, rQ16 | 16 | 0.720 |
| Overall COVID-19 Impact | rQ17,rQ18,rQ19 | 3 | 0.708 |
| DSMQ Sum Scale (19 items) | Q1, Q2, Q3, Q4, rQ5, Q6, rQ7, Q8, Q9, rQ10, rQ11, rQ12, rQ13, rQ14, rQ15, rQ16,rQ17,rQ18,rQ19 | 19 | 0.719 |
| Parameters | DMSQ score | ||
| Turkish population POST-COVID (adapted from [8]) n = 378 |
Saudi population POST-COVID (current study) n = 341 |
Saudi population BEFORE COVID (adapted from [7]) n = 352 |
|
| Glucose Management | 5.18 ± 0.24 | 7.35 ± 1.94 | 7.8 ± 2.3 |
| Dietary Control | 5.20 ± 1.15 | 6.82 ± 2.17 | 6.5 ± 1.5 |
| Physical Activity | 5.10 ± 0.22 | 6.12 ± 2.95 | 5.8 ± 1.1 |
| Health Care Use | 5.24 ± 0.56 | 8.6 ± 1.77 | 4.8 ± 1.2 |
| Overall rating of self-care | NA | 8.45 ± 2.65 | NA |
| DSMQ Sum Scale (16 items) | 5.25 ± 1.04 | 7.29 ± 1.4 | NA |
| Overall COVID-19 Impact | NA | 7.81 ± 2.37 | NA |
| DSMQ Sum Scale (19 items) | NA | 7.37 ± 1.28 | NA |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




