Submitted:
26 October 2023
Posted:
26 October 2023
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
3.1. Sample demographic profile
3.2. Demographic profile of SARS-CoV-2 cases and predicting asymptomatic infection
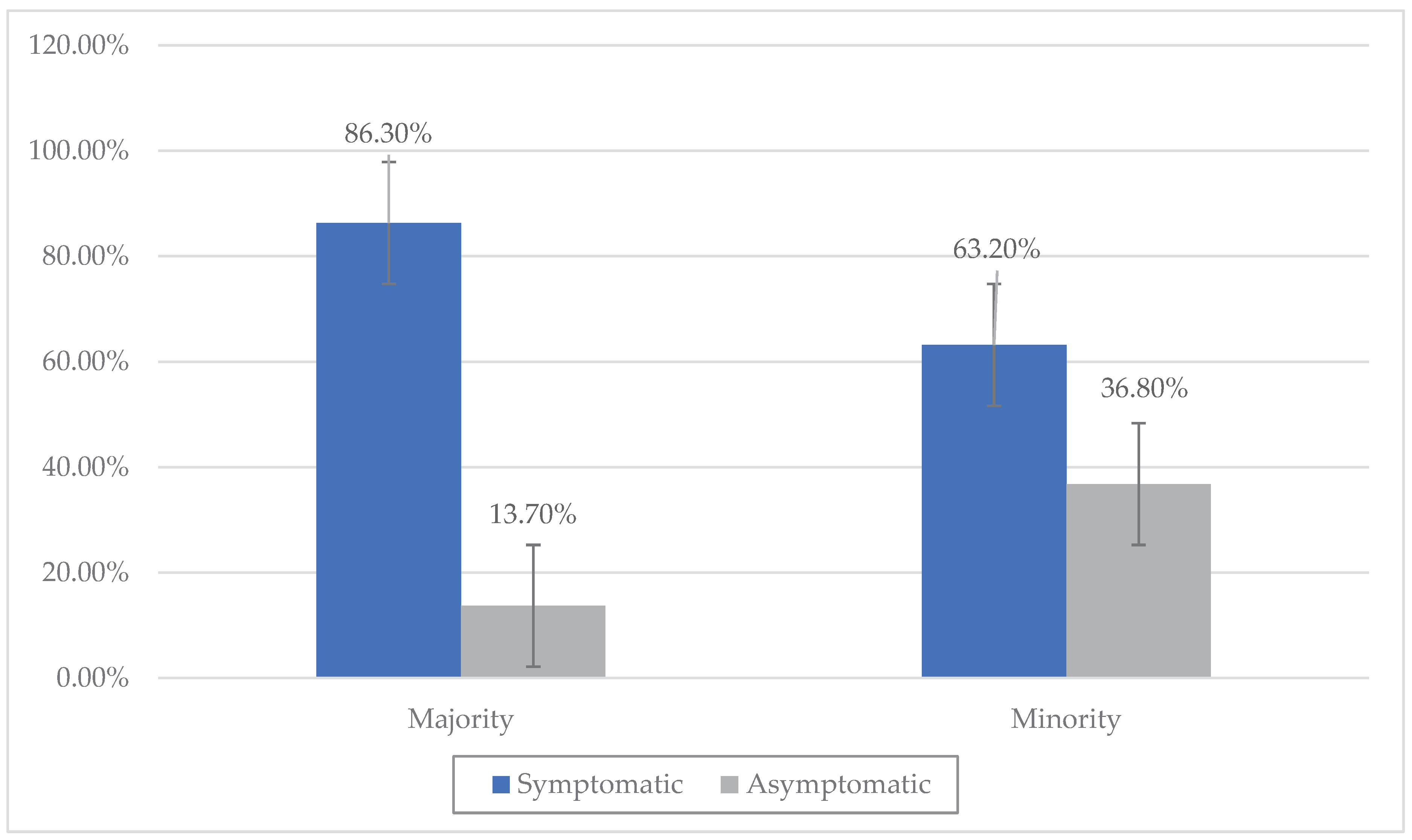
3.3. Ethnicity and asymptomatic infection
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organisation Managing epidemics: Key facts about major deadly disease. WHO. Available online: https://www.who.int/publications/i/item/managing-epidemics-key-facts-about-major-deadly-diseases (accessed on 12 October 2023).
- Cheng, H.Y.; Jian, S.W.; Liu, D.P.; Ng, T.C.; Huang, W.T.; Lin, H.H.; Taiwan COVID-19 Outbreak Investigation Team. Contact Tracing Assessment of COVID-19 Transmission Dynamics in Taiwan and Risk at Different Exposure Periods Before and After Symptom Onset. JAMA internal medicine 2020, 9, 1156–1163. [Google Scholar] [CrossRef] [PubMed]
- World Health Organisation Coronavirus disease. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019 (accessed on 12 October 2023).
- [COVID19 Barwon Health and Deakin University COVID-19 Research Task Force and Cohort Study] Barwon Health Geelong. 2020. COVID-19 Second Wave; unpublished data; 20/56 14/05/2020 & 21/91 14/10/2021.
- Gao, Z.; Xu, Y.; Sun, C.; Wang, X.; Guo, Y.; Qiu, S.; Ma, K. A systematic review of asymptomatic infections with COVID-19. Journal of microbiology, immunology 2021, 1, 12–16. [Google Scholar] [CrossRef] [PubMed]
- Kronbichler, A.; Kresse, D.; Yoon, S.; Lee, K.H.; Effenberger, M.; Shin, J.I. Asymptomatic patients as a source of COVID-19 infections: A systematic review and meta-analysis. IJID 2020, 98, 180–186. [Google Scholar] [CrossRef] [PubMed]
- Syangtan, G; Bista, S.; Dawadi, P. Asymptomatic SARs-COV-2 Carriers: A Systematic Review and Meta-Analysis. Frontiers in Public Health 2020, 8, 58–74. [Google Scholar] [CrossRef] [PubMed]
- Roder, C.; Maggs, C.; McNamara, B.; O’Brien, D.; Wade, A.J.; Bennett, C.; Pascol, J.A.; Athan, E. Area-level social and economic factors and the local incidence of SARS-CoV-2 infections in Victoria during. Medical Journal of Aust 2020, 7, 349–356. [Google Scholar] [CrossRef]
- Voysey, M.; Costa Clemens, S.A.; Madhi, S.A.; Weckx, L.Y.; Folegatti, P.M.; Aley, P.K.; Angus, B.; Baillie, V.L.; Barnabas, S.L.; Bhorat, Q.E.; et al. Single-dose administration and the influence of the timing of the booster dose on immunogenicity and efficacy of ChAdOx1 nCoV-19 (AZD1222) vaccine: a pooled analysis of four randomised trials. Lancet 2021, 397, 881–891. [Google Scholar] [CrossRef] [PubMed]
- Murdolo, D.; L Chatzileontiadou, D. A common allele of HLA is associated with asymptomatic SARS-CoV-2 infection. Nature 2023, 620, 128–136. [Google Scholar] [CrossRef]
- StataCorp Stata Statistical Software Release 17. Available online: https://www.stata.com/ (accessed on 15 July 2021).
- World Health Organisation Life course. Available online: https://www.who.int/our-work/life-course (accessed on 17 July 2021).
- Ranganathan, P.; Pramesh, C.S.; Aggarwal, R. Common pitfalls in statistical analysis: Logistic regression. Perspect Clin Res. 2017, 8, 148–151. [Google Scholar] [CrossRef]
- Wang, H.; Peng, J.; Wang, B. Inconsistency Between Univariate and Multiple Logistic Regressions. Shanghai Arch Psychiatry. 2017, 29, 124–128. [Google Scholar] [CrossRef]
- Kang, H. The prevention and handling of the missing data. Korean journal of anesthesiology 2016, 45, 402–406. [Google Scholar] [CrossRef]
- Rentsch, C.T.; Kidwai-Khan, F.; Tate, J.P.; Park, L.S.; King, J.T., Jr; Skanderson, M.; Hauser, R.G.; Schultze, A.; Jarvis, C.I.; Holodniy, M.; et al. Patterns of COVID-19 testing and mortality by race and ethnicity among United States veterans: A nationwide cohort study. PLoS medicine 2020, 17, e1003379. [Google Scholar] [CrossRef] [PubMed]
- Byambasuren, O.; Cardona, M.; Bell, K.; Clark, J.; McLaws, M.L.; Glasziou, P. Estimating the extent of asymptomatic COVID-19 and its potential for community transmission: Systematic review and meta-analysis. JAMMI 2020, 5, 223–234. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Han, Z.G.; Qin, P.Z.; Liu, W.H.; Yang, Z.; Chen, Z.Q.; Li, K.; Xie, C.J.; Ma, Y.; Wang, H.; et al. Transmission and containment of the SARS-CoV-2 Delta variant of concern in Guangzhou, China: A population-based study. PLoS neglected tropical diseases 2022, 16, e0010048. [Google Scholar] [CrossRef] [PubMed]
- Yanes-Lane, M.; Winters, N.; Fregonese, F.; Bastos, M.; Perlman-Arrow, S.; Campbell, J.R.; Menzies, D. Proportion of asymptomatic infection among COVID-19 positive persons and their transmission potential: A systematic review and meta-analysis. PloS one 2020, 15, e0241536. [Google Scholar] [CrossRef] [PubMed]
- Kumar, N.; Shahul Hameed, S.K.; Babu, G.R.; Venkataswamy, M.M.; Dinesh, P.; Kumar Bg, P.; John, D.A.; Desai, A.; Ravi, V. Descriptive epidemiology of SARS-CoV-2 infection in Karnataka state, South India: Transmission dynamics of symptomatic vs. asymptomatic infections. EClinicalMedicine 2021, 32, 100717. [Google Scholar] [CrossRef] [PubMed]
- Niedzwiedz, C.L.; O'Donnell, C.A.; Jani, B.D.; Demou, E.; Ho, F.K.; Celis-Morales, C.; Nicholl, B.I.; Mair, F.S.; Welsh, P.; Sattar, N.; et al. Ethnic and socioeconomic differences in SARS-CoV-2 infection: prospective cohort study using UK Biobank. BMC medicine 2020, 18, 160. [Google Scholar] [CrossRef] [PubMed]
- Sze, S.; Pan, D.; Nevill, C.R.; Gray, L.J.; Martin, C.A.; Nazareth, J.; Minhas, J.S.; Divall, P.; Khunti, K.; Abrams, K.R.; Nellums, L.B.; et al. Ethnicity and clinical outcomes in COVID-19: A systematic review and meta-analysis. EClinicalMedicine 2020, 29, 100630. [Google Scholar] [CrossRef] [PubMed]
- Treibel, T.A.; Manisty, C.; Burton, M.; McKnight, Á.; Lambourne, J.; Augusto, J.B.; Couto-Parada, X.; Cutino-Moguel, T.; Noursadeghi, M.; Moon, J.C. COVID-19: PCR screening of asymptomatic health-care workers at London hospital. Lancet 2020, 395, 1608–1610. [Google Scholar] [CrossRef] [PubMed]
- Olmos, C.; Campaña, G.; Monreal, V.; Pidal, P.; Sanchez, N.; Airola, C.; Sanhueza, D.; Tapia, P.; Muñoz, A.M.; et al. SARS-CoV-2 infection in asymptomatic healthcare workers at a clinic in Chile. PloS one 2021, 16, e0245913. [Google Scholar] [CrossRef]
- Yoon, S.; Li, H.; Lee, K.H.; Hong, S.H.; Kim, D.; Im, H.; Rah, W.; Kim, E.; Cha, S.; Yang, J.; et al. Clinical Characteristics of Asymptomatic and Symptomatic Pediatric Coronavirus Disease 2019 (COVID-19): A Systematic Review. Medicina 2020, 56, 474. [Google Scholar] [CrossRef]
- Griffith, G.; Morris, T.; Tudball, M. Collider bias undermines our understanding of COVID-19 disease risk and severity. Nature Communications 2020, 11, 11. [Google Scholar] [CrossRef] [PubMed]
- Le, T.Q.M.; Takemura, T.; Moi, M.L.; Nabeshima, T.; Nguyen, L.K.H.; Hoang, V.M.P.; Ung, T.H.T.; Le, T.T.; Nguyen, V.S.; Pham, H.Q.A.; Duong, T.N.; et al. Severe Acute Respiratory Syndrome Coronavirus 2 Shedding by Travelers, Vietnam. Emerging infectious diseases 2020, 26, 1624–1626. [Google Scholar] [CrossRef] [PubMed]
| Demographics | Count | % (95% CI) | |||
|---|---|---|---|---|---|
| S | A | Total | S | A | |
| Total | 265 | 63 | 328 | 80.8% | 19.2% |
| Age (mean years) | 38.1 | 37.8 | |||
|
Age (years) (S=265) (A=63) Youth (18-24) Young adult (25-44) Adult (45-64) Senior (65+) |
56 114 87 8 |
7 44 8 4 |
63 158 95 12 |
21.1% (16.6 – 26.5) 43.0% (37.2 – 49.1) 32.8% (27.4 – 38.7) 3.1% (1.5 – 5.9) |
11.1% (5.4 – 21.6) 69.8% (57.4 – 79.9) 12.7% (6.5 – 23.4) 6.4% (2.4 – 15.8) |
|
Sex (S=265) (A=63) Male Female |
138 127 |
37 26 |
175 153 |
52.1% (46.0 – 58.1) 47.9% (41.9 – 54.0) |
58.7% (45.5 – 69.7) 41.3% (30.3 – 54.5) |
|
Ethnicity (S=199) (A=60) Majority Minority |
132 67 |
21 39 |
153 106 |
66.3% (59.5 – 72.6) 33.7% (27.4 – 40.5) |
35.0% (24.0 – 47.9) 65.0% (52.2 – 76.0) |
|
Occupation (S=222) (A=58) Healthcare worker Essential service worker Residential age care worker Other working Other not working Other unknown |
34 55 15 67 13 38 |
2 14 2 9 5 26 |
36 69 17 76 18 64 |
15.3% (11.1 – 20.7) 24.8% (19.5 – 30.9) 6.7% (4.1 – 10.9) 30.2% (24.5 – 36.6) 5.9% (3.4 – 9.8) 17.1% (12.7 – 22.7) |
3.5% (0.9 – 12.8) 24.1% (14.8 – 36.8) 3.5% (0.9 – 12.8) 15.5% (8.3 – 27.3) 8.6% (3.6 – 19.2) 44.8% (32.6 – 57.7) |
|
Living (S=254) (A=63) Family Friends/housemates Alone |
197 46 11 |
36 24 3 |
233 70 14 |
77.6% (72.0 – 82.3) 18.1% (13.8 – 23.4) 4.3% (2.4 – 7.7) |
57.1% (44.7 – 68.8) 38.1% (27.0 – 50.6) 4.8% (1.5 – 13.8) |
|
Comorbidity (S=265) (A=63) Yes None reported |
33 232 |
7 56 |
40 288 |
12.5% (9.0 – 17.0) 87.5% (83.0 – 91.0) |
11.1% (5.4 – 21.6) 88.9% (78.4 – 94.6) |
|
Smoker status (S=99) (A=11) Never Current Former |
55 12 32 |
10 1 0 |
65 13 32 |
55.6% (45.6 – 65.1) 12.1% (7.0 – 20.3) 32.3% (23.8 – 42.2) |
90.9% (55.6 – 98.8) 9.1% (1.2 – 44.4) 0.0% |
|
Exposure type (S=183) (A=47) Household Workplace Other |
95 65 23 |
22 16 9 |
117 81 32 |
51.9% (44.6 – 59.1) 35.5% (28.9 – 42.8) 12.6% (8.5 – 18.2) |
46.8% (33.1 – 61.0) 34.0% (22.0 – 48.6) 19.2% (10.2 – 33.0) |
| Unadjusted | Adjusted (n=179) | |||
|---|---|---|---|---|
| Demographics | Odds Ratio | 95% CI | Odds Ratio | 95% CI |
| Age (years) (S=265) (A=63) | ||||
| Youth 18 – 24 (RC) Young Adults 25 – 44 Adults 45 – 64 Seniors 65+ |
1.0 3.1** 0.7 4.0 |
1.3 – 7.3 0.3 – 2.1 1.0 – 16.8 |
2.1 0.6 7.3* |
0.7 – 5.9 0.2 – 2.2 1.0 – 50.5 |
| Sex (S=265) (A=63) | ||||
| Male (RC) Female |
1.0 0.8 |
0.8 – 2.3 |
1.4 |
0.7 – 2.8 |
| Ethnicity (S=199) (A=60) | ||||
| Majority (RC) Minority |
1.0 3.7*** |
2.0 – 6.7 |
3.2** |
1.5 – 6.7 |
| Occupation (S=222) (A=58) | ||||
| Healthcare worker (RC) Essential service worker Residential age care worker Other working Other not working Other unknown |
1.0 4.3 2.3 2.3 6.5* 11.6*** |
0.9 – 20.2 0.3 – 17.6 0.5 – 11.2 1.1 – 38.0 2.6 – 52.7 |
2.4 1.1 1.5 4.6 7.3* |
0.4 – 12.5 0.1 – 9.2 0.3 – 8.6 0.6 – 34.4 1.5 – 34.6 |
| Living situation (S=254) (A=63) | ||||
| Alone (RC) With Family With Friends/Housemates |
1.0 0.7 1.9 |
0.2 – 2.5 0.5 – 7.5 |
||
| Comorbidity (S=265) (A=63) | ||||
| None reported (RC) Yes |
1.0 0.9 |
0.3 – 2.1 |
||
| Smoker status (S=99) (A=11) | ||||
| Never (RC) Current Former |
1.0 0.5 1.0 |
0.1 – 3.9 | ||
| Exposure type (S=183) (A=47) | ||||
| Other (RC) Household Workplace |
1.0 0.6 0.6 |
0.2 – 1.5 0.2 – 1.6 |
||
| Symptom Profile n (%) | |||
|---|---|---|---|
| Ethnicity | Asymptomatic | Symptomatic | Total |
| Caucasian | 21 (13.7%) | 132 (86.3%) | 153 |
| Southeast Asian | 7 (28.0%) | 18 (72.0%) | 25 |
| Northeast Asian | 7 (41.2%) | 10 (58.8%) | 17 |
| Southern and Central Asian | 2 (28.6%) | 5 (71.4%) | 7 |
| African | 3 (33.3%) | 6 (66.7%) | 9 |
| Middle Eastern | 2 (33.3%) | 4 (66.7%) | 6 |
| Other minorities | 18 (42.9%) | 24 (57.1%) | 42 |
| Total | 60 | 199 | 259 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




