1. Introduction
Bicuspid aortic valve (BAV) is the most common congenital heart disease with a prevalence ranging from 0.5% to 1.4% in the population and is associated with severe complications including aortopathy and is mostly asymptomatic in childhood. [
1,
2]. On the other hand, calcineurin signal pathway genes participating in intrauterine valvulogenesis and hypertrophic reactions after birth [
3,
4]. The role of calcineurin pathway biomarkers in early myocardial changes in children with BAV has been demonstrated in our previous study. [
5]. Basic genes regulating these reactions belong to the nuclear factor-activated T-cell family (NFATC) with highest expression in adipocytes, chondrocytes and during morphogenesis of veins and heart valves, and also in myocardial hypertrophy [
6,
7]. In addition, the recruitment of T cells in myocardial remodeling and heart failure has been demonstrated [
8,
9]. Homozygous alleles with conservative sequences of the NFATC1 gene were found in 1 out of 4 patients with BAV. [
10,
11]. It has been shown in animal models that overproduction of calcineurin is the cause of hypertrophic responses and the development of heart failure but overproduction of calcineurin inhibitors may have a protective effect. [
12,
13].
In phenotypes of BAV also demonstrated the heterogeneity in relation to subsequent aortic complications with the prevalence of BAV-RL and BAV with raphe corresponding to the development of aortic regurgitation and BAV-RN corresponding to aortic stenosis but theses studies mostly included adolescents and adults. [
14,
15]. These data indicate that aortic complications most commonly develop after pediatric age. It should also be noted the different characteristics of BAV in children compared to adults with the predominance of type 0 and type 1 morphology according to Sievers and no significant relationships with myocardial remodeling in asymptomatic patients. [
16]. At the same time, in children with BAV the left ventricle (LV) changes such as increased LV mass mainly combined with significant aortic stenosis and regurgitation were demonstrated but aortal dilation were associated with older age [
17,
18].
In line with the above studies and the importance of calcineurin signaling pathway genes in both valve development and myocardial remodeling, these factors could also be implicated in myocardial changes in children with BAV. In this connection, detecting the significance of NFATC1 and NFATC4 expression in early myocardial remodeling in BAV children seems relevant.
The aim of the study is to determine the association of NFATC1 and NFATC4 genes expression with myocardial remodeling and changes in intracardiac hemodynamics in children with BAV.
2. Materials and Methods
2.1. Patient Selection
The study was conducted at Zaporizhzhya Regional Clinical Children’s Hospital. In the study participated 112 patients in whom the diagnosis of BAV was established by general clinical investigation and standard Doppler echocardiography. The control group included 20 healthy children without pathology of the cardiovascular system as well as heart anomalies by their clinical exam and heart ultrasound. Criteria for inclusion in the main study group were the age of patients from 9 to 15, the diagnosis of BAV, absence of complaints at presentation, no ultrasound and clinical signs of aortopathies or heart complications, informed consent of children or their parents to conduct the study.
The exclusion criteria were the age of children younger than 9 and older than 15 years old, sports, the presence of clinical signs of heart failure, congenital malformations of other organs and systems, sports, established chromosomal abnormalities, chronic diseases in the stage of decompensation or acute infectious diseases. After inclusion and exclusion criteria were applied there were 47 patients with BAV in the main group without significant differences in age, BMI, and gender distribution to control (
Table 1).
2.2. Doppler Echocardiography
Doppler echocardiography was performed using the “Xario 100” scanner (Toshiba, Japan) with 2.5 MHz sensor and detection of standard parameters. Relative left ventricular posterior wall thickness (RPWT) detected by A. Ganau. Left ventricular mass (LVM) detected by Devereux R.B. Left ventricular myocardium mass index (LVMMI) detected by P. Gosse.
2.3. Genetic Study
The expression level of NFATC1 and NFATC4 genes in the blood cells of patients detected by total RNA extraction and obtaining of cDNA by reverse transcription with CFX96™ Real-Time PCR Detection Systems amplifier (Bio-Rad Laboratories, Inc., USA) and the Maxima SYBR Green/ROX qPCR Master Mix (2X) reagent kit (Thermo Scientific, USA). Statistical analysis of PCR data was performed using CFX Manager ™ software (Bio-Rad, USA). The obtained values were presented in units of relative normalized expression compared to the expression in the control group was taken as the 1 unit of expression (e.u).
2.4. Statistical Analysis
Statistical analysis was performed using the Statiatica 13.0 program. The normality of distribution was assessed by the Shapiro-Wilk test. The data were presented in the form M ± m where M is the sample mean, m is the error of mean in the case of a normal distribution and in the form of Median (min-max) in the case when distribution deviated from normal. In assessing the significance between groups with normal distribution the Student’s t-test was scored, for the presence of the difference between groups, in not normal distribution the Mann-Whitney nonparametric criterion for small samples was scored. The relationship between parameters assessed by Spearman correlations.
2.5. Ethics
All procedures performed in studies involving human participants were in accordance with the ethical standards according to the principles of the Declaration of Helsinki and this study was approved by Zaporizhzhya State Medical University Clinical Research Ethical Committee (Protocol Number 5 from 17.04.2019).
3. Results
In children with BAV, significant differences in Doppler echocardiographic parameters were observed between groups (
Table 2).
These included increased SWTd and PWTd, AoPPG, LVM, LVMMI and RPWT, acceleration of the AVV (p<0,05), which clearly reflected the morphological and functional characteristics of this defect. At the same time, there were no significant differences in other Doppler echocardiographic data between the groups. Noteworthy is that RPWT and LVMMI were significantly higher in 29 (61.7%) of the children with BAV with PWTd >8mm compared to those with PWTd <8mm (p<0,05), as shown in
Table 3. Thus, in two-thirds of the patients the LV enlargement is according to PWTd, LVMMI, and RPWT parameters which correspond to concentric hypertrophy of the LV myocardium. In another 18 patients with BAV (38.3%) LV geometry remained unchanged.
Evaluation of NFATC1 and NFATC4 gene expression in children with BAV has revealed a significantly higher expression of NFATC1 gene (NFATC1 median (min-max) 70,88 (8,79-106,51) e.u. vs 7,72 (1,74-22,67) e.u., respectively p<0,05), although the expression of both genes was 71-fold and 8-fold higher compared to control, respectively.
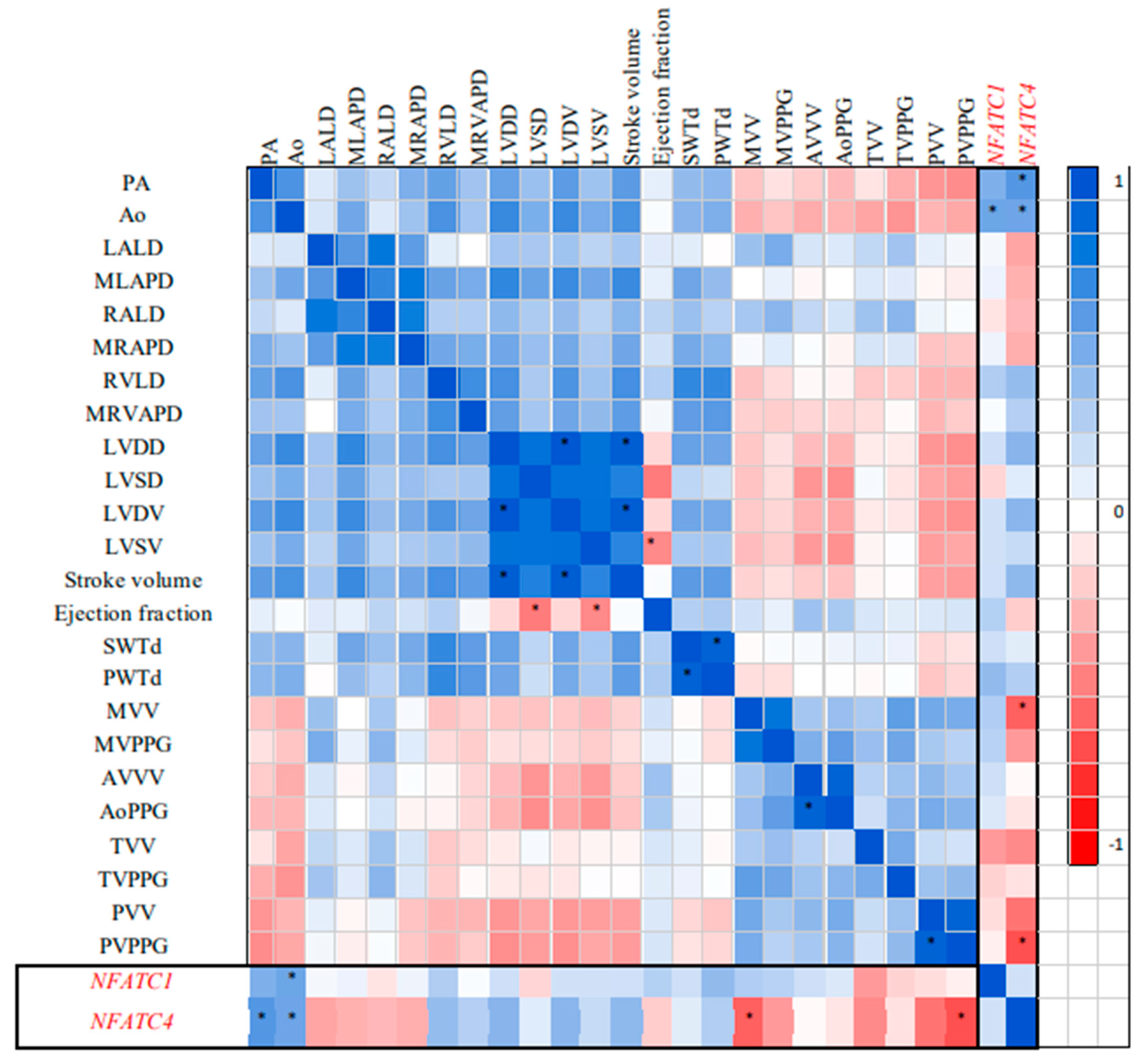
Correlation analysis of NFATC1 and NFATC4 with Doppler echocardiographic parameters (
Figure 1). showed a significant correlation of NFATC1 and NFATC4 with Ao (R=+0,53 and R=+0,54 respectively, p<0,05) and NFATC4 with MVV and PVPPG (R=-0.62 and R=-0.68, respectively, p<0,05). Other significant correlations reflected interactions in functional Doppler echocardiographic parameters of BAV children (LVDD with LVSD and LVDV (R=+0,84 and R=+0,98 respectively, p<0,05), stroke volume with LVDD and LVSD (R=+0,95 and R=+0,74 respectively, p<0,05), ejection fraction with LVSD and LVSV (R=-0,52 and R=-0,46 respectively, p<0,05), MLAPD to LALD (R=+0,61, p<0,05).
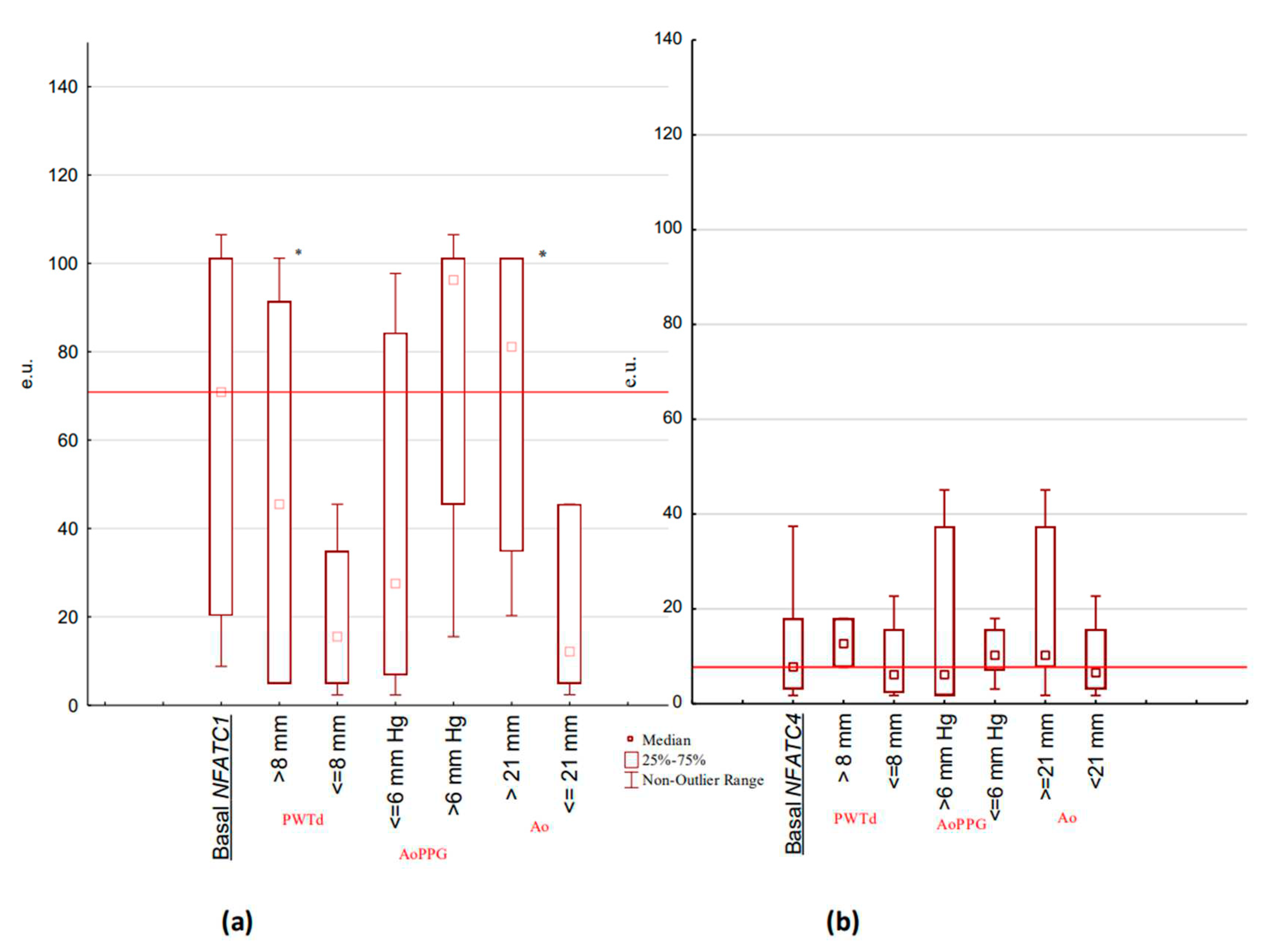
Expressive levels of NFATC1 and NFATC4 genes in the change of defect-associated parameters of Doppler echocardiography in children with BAV (
Figure 2) showed significant differences.
In children with increased PWTd more than 8 mm compared to BAV children with PWTd less than or equal to 8 mm, the level of NFATC1 expression was significantly higher (NFATC1 median (min-max) 45,49 (5,01-101,52) e.u. vs 15,53 (2,36-44,40) e.u., p<0.05) with respect to NFATC4 insignificant differences by this parameter (NFATC4 median (min-max) 12,60 (7,72-37,41) e.u. vs 6,31(1,74-45,09) e.u., p>0.05). For both NFATC1 and NFATC4 expression in AoPPG more than 6 mm Hg compared to value less than or equal to 6 mm Hg there is no significance was detected (NFATC1 median (min-max) 96.25 (15.50-106.50) e.u. vs 27.53 (2.36-91.54) e.u.), p>0.05 and NFATC4 median (min-max) 6.24 (1.74-45.09) e.u. vs 10.16 (3.08-17.96) e.u., p>0.05). The parameter of Ao related to the value of 21 mm was found to be significantly increased for NFATC1 expression (NFATC1 median (min-max) 81.11 (20.27-101.10) e.u. at Ao >= 21 mm vs 12.16 (2,40-45.49) e.u., at Ao < 21 mm p<0.05) and was not significant for NFATC4 expression (NFATC4 median (min-max) 10,16 (1,45-45,09) e.u. at Ao >= 21 vs 6,38(1,74-22,67) e.u. at Ao < 21 mm p>0.05).
4. Discussion
Authors
Genes of NFATC family as transcription factors play an essential role in many pathological processes such as myocardial hypertrophy tumorigenesis and immune response. The study of the expression of these genes in children with BAV has both diagnostic and prognostic value because of involvement in valvulogenesis and the presence of polymorphisms that could influence the development of this anomaly. Our previous investigation showed the predominance of rs11665469 homozygous TT genotype of NFATC1 in children with BAV [
19] and in the current study we found an increased expression activity of this gene. It was also found that there was a significant correlation between the expression of NFATC1 and the diameter of the aortic root in children with BAV and its absence for PWTd, although the expression level was significantly increased at elevated values of both parameters. This may indicate an earlier involvement of aortic changes in the pathological process influenced by NFATC1 expression. This is indirectly confirmed by the highest levels of expression of NFATC1 in relation to the other parameters studied and by exceeding the overall level of expression of this gene in children with BAV. Nevertheless, the elevated expression of NFATC1 could also be related to an advanced adaptive change of the LV marked in the BAV patients. Our results are consistent with studies showing high levels of transcriptionally active mutated gene expression that are involved in heart development [
20] and may also contribute to autonomous LV remodeling in some children with BAV.
The established association of NFATC1 gene expression levels with LV and aortic changes in children with BAV allows us to define the risk stratification strategy regarding complications and future cardiovascular events in these patients who are experiencing increasing aortic diameter. High NFATC1 expression in association with changes in PWTd and Ao in children with BAV is indicative of intense and progressive myocardial changes and requires closer follow-up with clinical evaluation and Doppler echocardiography.
4.1. Limitations
This study has some limitations due to overlap in the parameters studied. Some patients appeared to have both elevated PWTd and Ao, or Ao with elevated AoPPG. Another limitation concerns some phenotypic heterogenicity in BAV anatomy that could affect AV hemodynamics and was not included in this study, However, the association of LV and aortic changes with the level of NFATC1 expression, but not with AV haemodynamics, was found to reflect a predominant remodeling caused by a possible increased expression of mutant genes of the transcriptional cascade associated with BAV. In addition, the results obtained on the expression of NFATC1 in children with BAV could be the basis for a therapeutic approach based on expressive activity regulation.
5. Conclusions
In children with BAV the high expression of the NFATC1 calcineurin signalling pathway gene is associated with elevated PWTd and Ao.
Author Contributions
Conceptualization, An.K., M.G. Methodology, Al.K., V.O., Validation, An.K., M.G. V.O., Formal analysis, An.K., O.K. Investigation: Al.K., V.O. Writing original draft, An.K, M.G., Writing-review and editing, M.G, V.O. Project administration An.K. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
All procedures performed in studies involving human participants were in accordance with the ethical standards according to the principles of the Declaration of Helsinki and this study was approved by Zaporizhzhya State Medical University Clinical Research Ethical Committee (Protocol # 5 from 17.04.2019).
Informed Consent Statement
Informed consent was obtained from all subjects included in the study.
Acknowledgments
This article is based on the doctoral study of Andrii Kamenshchyk. The authors are grateful to Zaporizhzhya State Medical and Pharmaceutical University for supporting the research and laboratory environment.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Mubarik, A.; Sharma, S.; Law, M.A. Bicuspid Aortic Valve. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023. Available online: https://www.ncbi.nlm.nih.gov/books/NBK534214/ (accessed on 21 January 2023).
- Masri, A.; Svensson, L.G.; Griffin, B.P.; Desai, M.Y. Contemporary natural history of bicuspid aortic valve disease: a systematic review. Heart. 2017, 103, 1323–1330. [Google Scholar] [CrossRef] [PubMed]
- Gunawan, F.; Gentile, A.; Gauvrit, S.; Didier YRBensimon-Brito SBensimon-Brito, A. NFATC1 Promotes Interstitial Cell Formation During Cardiac Valve Development in Zebrafish. Circulation Research. 2020, 126, 968. [Google Scholar] [CrossRef] [PubMed]
- Shaw, R.M.; Nikolova, A.P. A Surprising Noncanonical Role for Calcineurin in Pressure-Induced Cardiac Hypertrophy. J Am Coll Cardiol. 2018, 71, 668–669. [Google Scholar] [CrossRef] [PubMed]
- Kamenshchyk, A.V. Determination of signal calcineurin pathway biomarkers significance in early myocardial changes in children with bicuspid aortic valve. Science Rise: Medical Science. 2017, 11, 22–27. [Google Scholar] [CrossRef]
- Mognol, G.; Carneiro, F.; Robbs, B.K.; Faget, B.V.; Viola, J.P.B. Cell cycle and apoptosis regulation by NFAT transcription factors: new roles for an old player. Cell Death Dis 2016, 7, e2199. [Google Scholar] [CrossRef] [PubMed]
- Chaklader, M.; Rothermel, B.A. Calcineurin in the heart: New horizons for an old friend. Cellular Signalling 2021, 87, 110134. [Google Scholar] [CrossRef] [PubMed]
- Blanton, R.M.; Carrillo-Salinas, F.J.; Alcaide, P. T-cell recruitment to the heart: friendly guests or unwelcome visitors? Am J Physiol Heart Circ Physiol. 2019, 317, H124–H140. [Google Scholar] [CrossRef] [PubMed]
- Liu., Hu J, Lei H,. Quin H., Wang Ch., et al. Regulatory T Cells in Pathological Cardiac Hypertrophy: Mechanisms and Therapeutic Potential. Cardiovasc Drugs Ther. 2023. [CrossRef]
- Xue, Z.X.; Zhi, G.B.Z. Association between nuclear factor of activated T cells 1 gene mutation and simple congenital heart disease in children. Chin Med J. 2010, 38, 621–624. [Google Scholar]
- Zhao, W.; Niu, G.; Shen, B.; Zheng, Y.; Gong, F.; Wang, X.; et al. High-resolution analysis of copy number variants in adults with simple-to-moderate congenital heart disease. Am J Med Genet A. 2013, 161, 3087–94. [Google Scholar] [CrossRef] [PubMed]
- Li, S.J.; Wang, J.; Ma, L.; Lu, C.; Wang, J.; Wu, J.W.; et al. Cooperative autoinhibition and multi-level activation mechanisms of calcineurin. Cell Res. 2016, 26, 336–49. [Google Scholar] [CrossRef] [PubMed]
- Parra, V.; Rothermel, B.A. Calcineurin signaling in the heart: The importance of time and place. J Mol Cell Cardiol. 2017, 103, 121–136. [Google Scholar] [CrossRef] [PubMed]
- Toufan Tabrizi, M.; Rahimi Asl, R.; Nazarnia, S.; Pourafkari, L. Evaluation of relationship between bicuspid aortic valve phenotype with valve dysfunction and associated aortopathy. J Cardiovasc Thorac Res. 2018, 10, 236–242. [Google Scholar] [CrossRef] [PubMed]
- Mai, Z.; Guan, L.; Mu, Y. Association between bicuspid aortic valve phenotype and patterns of valvular dysfunction: A meta-analysis. Clin Cardiol. 2021, 44, 1683–1691. [Google Scholar] [CrossRef] [PubMed]
- Liu, T.; Xie, M.; Lv, Q.; Li, Y.; Fang, L.; Zhang, L.; Deng, W.; Wang, J. Bicuspid Aortic Valve: An Update in Morphology, Genetics, Biomarker, Complications, Imaging Diagnosis and Treatment. Front. Physiol. 1921, 9. [Google Scholar] [CrossRef] [PubMed]
- Stefek, H.A.; Berhane, H.; Robinson, J.D.; Reilly, B.; Ruh, A.; et al. Comprehensive MR Analysis of Cardiac Function, Aortic Hemodynamics and Left Ventricular Strain in Pediatric Cohort with Isolated Bicuspid Aortic Valve. Pediatr Cardiol 2019, 40, 1450–1459. [Google Scholar] [CrossRef] [PubMed]
- Grattan, M.; Prince, A.; Rumman, R.K.; Morgan, C.; Petrovic, M.; et al. Predictors of Bicuspid Aortic Valve-Associated Aortopathy in Childhood: A Report From the MIBAVA Consortium. Circ Cardiovasc Imaging. 2020, 13, e009717. [Google Scholar] [CrossRef] [PubMed]
- Kamenshchyk, A.V. RS11665469, RS724256, RS754505 single nucleotide polymorphisms of NFATC1 gene and RS2229309 of NFATC4 gene in children with bicuspid aortic valve. Actual problems of Pediatrics, Obstetrics and Gynecology. 2017, 2, 5–9. [Google Scholar] [CrossRef]
- Zaidi, S.; Choi, M.; Wakimoto, H.; Lijiang Ma Jiang, J.; et al. De novo mutations in histone-modifying genes in congenital heart diseases. Nature 2013, 498, 220–223. [Google Scholar] [CrossRef]
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).