2. Case Report
Written informed consent was obtained from the patient for the publication of this case report.
We report a case of a 33-year-old pregnant woman (height, 153 cm; weight, 61 kg) at 13 weeks gestation. She had been experiencing hoarseness and bilateral granuloma, requiring surgical intervention.
Six month ago, she was admitted to Korea University Guro Hospital’s emergency room with unstable mental condition. She experienced severe vomiting and diarrhea prior to admission, and shortly after the urgent admission, she suffered a cardiac arrest with pulseless electrical activity. Cardiac compressions were initiated right away, and she was intubated with a 7.5 inner diameter tube. After three cycles of cardiopulmonary resuscitation, spontaneous circulation was restored. Computed tomography revealed the hemoperitonium that was caused by ovarian cyst rupture. Her vital sign and hypovolemic condition were managed in the emergency room. Her mental conditions improved with the recovery of vital signs. However, four hours after intubation, she accidently removed the intubated tube. Shortly after this incident, the patient was transferred to the operating room for emergency laparoscopic exploration. Intubation was reperformed before the surgery in operating room. The surgery lasted one hour. After the surgery,she was transferred to the intensive care unit and her endotracheal tube was maintained due to the possibility of unstable vital signs. Fifteen hours after the surgery, extubation was performed, and she was able to breathe spontaneously without discomfort. After spending two days in the ICU, she recovered well and resumed her daily life.
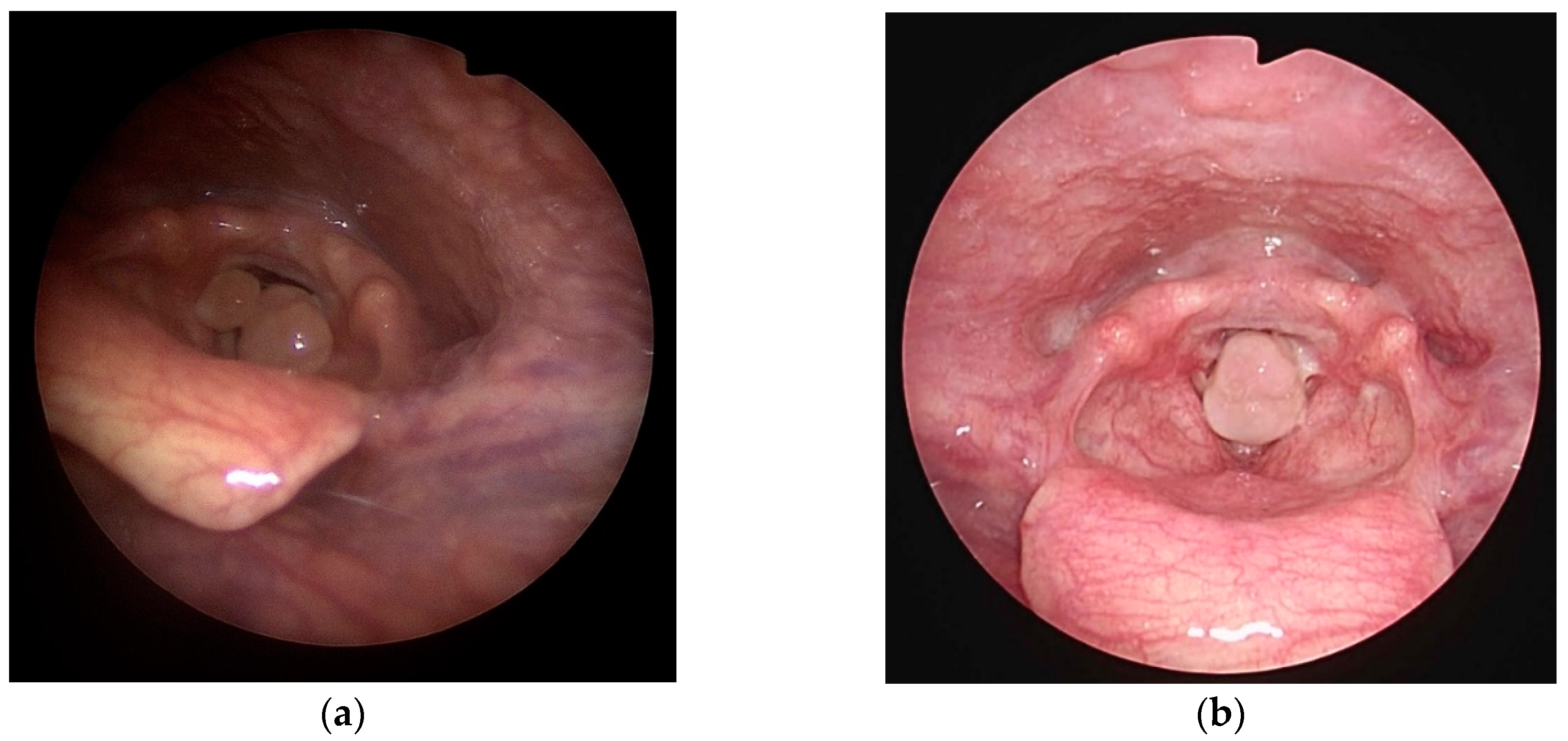
Approximately three months later, she became pregnant. At 11 weeks gestation, she returned to Korea University Guro Hospital’s emergency room with complaints of hoarseness and dyspnea. During medical examination, she mentioned that mild hoarseness had persisted since her last admission, but it worsened three days prior, accompanied by dyspnea and sore throat. She was referred to the otolaryngology department, where an examination of her glottis with indirect laryngoscopy revealed bilateral large vocal process granulomas that almost completely obstructed her glottis. (
Figure 1a) Initially, oral steroid and proton pump inhibitor were prescribed for treatment, despite the teratogenic risks. Her symptoms improved with oral medication. However, upon discontinuation of the medications after one week, her symptoms recurred. Due to the progression in size of granuloma and the burden of continuing steroid treatment, surgical intervention was deemed necessary. (
Figure 1b)
Due to the severe airway obstruction, intubation and ventilation were not deemed feasible. The medical team, including the anesthesiologist and otolaryngologist, discussed potential surgical options in advance. Tracheostomy was considered but deemed excessive for the patient's condition. Jet ventilation was considered as an option, but the healthcare providers in our center did not frequently practice it. Considering the anticipated short duration of the surgical procedure, the anesthetic plan focused on preoxygenation and maintaining adequate oxygen reserves to sustain any potential apneic period. HFNC oxygenation was chosen to ensure sufficient oxygen supply before anesthesia, and ORi monitoring was utilized as a tool to predict oxygen reserve and decreases of oxygen saturation during general anesthesia.
The essential laboratory data, including CBC, electrolytes, and blood coagulation, were within normal range. Due to dyspnea, the patient underwent chest x-ray and pulmonary function test. The chest x-ray showed no abnormalities, but the pulmonary function test revealed an extra-thoracic obstruction pattern, causing difficulty with inhalation. Due to her history of cardiac arrest, she underwent echocardiography. The echocardiography revealed grade 1 impairment of left ventricle diastolic function and normal left ventricle systolic function with an ejection fraction of 60-65%. A pre-anesthetic physical examination was conducted. Her Mallampati grade was 2, and she had unrestricted neck extension with full range of motion. Although she experienced hoarseness and dyspnea, there were no apparent neck or mandible swelling issues that could hinder mask bagging.
In the operating room, standard monitoring was implemented, including pulse oximetry, non-invasive blood pressure, and electrocardiography. Bispectorial index (BISTM, Medtronic, Minneapolis, USA) was used to estimate anesthetic depth, and electromyography (EMG, TwitchView®, Blink, Seattle, USA) was used for evaluate the degree of muscle relaxation. In addition, ORi was continuously monitored using a sensor attached to the patient’s finger through pulse oximetry (Radical-7™, Masimo Corp., Irvine, CA, USA), allowing for ongoing assessment of oxygen reserve. Following the placement of monitoring, pulse oximetry displayed a stable SpO2 of 100% along with consistent vital signs.
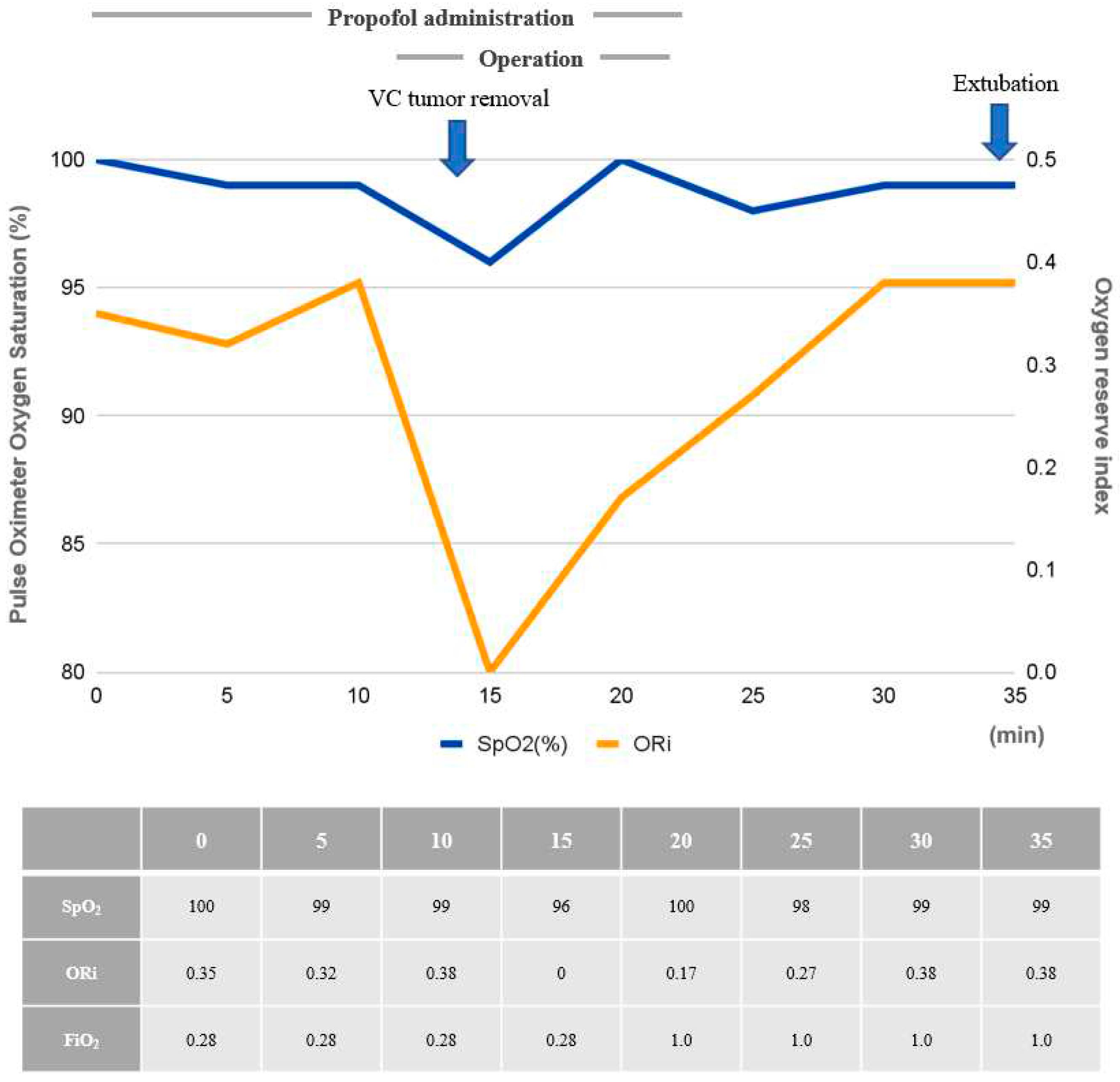
Prior to surgical mass removal, the patient received sufficient oxygen through HFNC oxygenation for five minutesHFNC was then used continuously untilbilateral granuloma excision, at which pointmask bagging became possible. After confirming the patient’s oxygen status through ORi monitoring of 0.35, total intravenous anesthesia with 2% propofol and remifentanil was initiated with the target-controlled infusion of propofol (Ce, 3-4 ng/ml) and remifentanil (Ce, 3-4 ng/kg), targeting the BIS under 60. Loss of consciousness was induced, but mask bagging was impeded by the mass. Twenty mg of rocuronium was immediately administered to facilitate laryngo-microscopic surgery and prevent movement, at which point the ORi was 0.32. After confirming muscle relaxation using train of four count (TOF) monitoring with the count of 0, the operation commenced. During surgery, anesthesia was maintained with a combination of propofol and remifentanil, targeting a BIS value under 60. Larynx was exposed with suspension laryngoscope after the patient lied in Boyce position. The bilateral granuloma was successfully removed with cup-head forcep and scissors. At that moment the ORi decreased to 0, and SpO2 was 96% and the surgical procedure was on hold for a minute. Mask ventilation was performed without difficulty and adequate mask bagging followed by HFNC oxygenation restored an ORi of 0.38 and SpO2 of 99% before completing the surgery. (
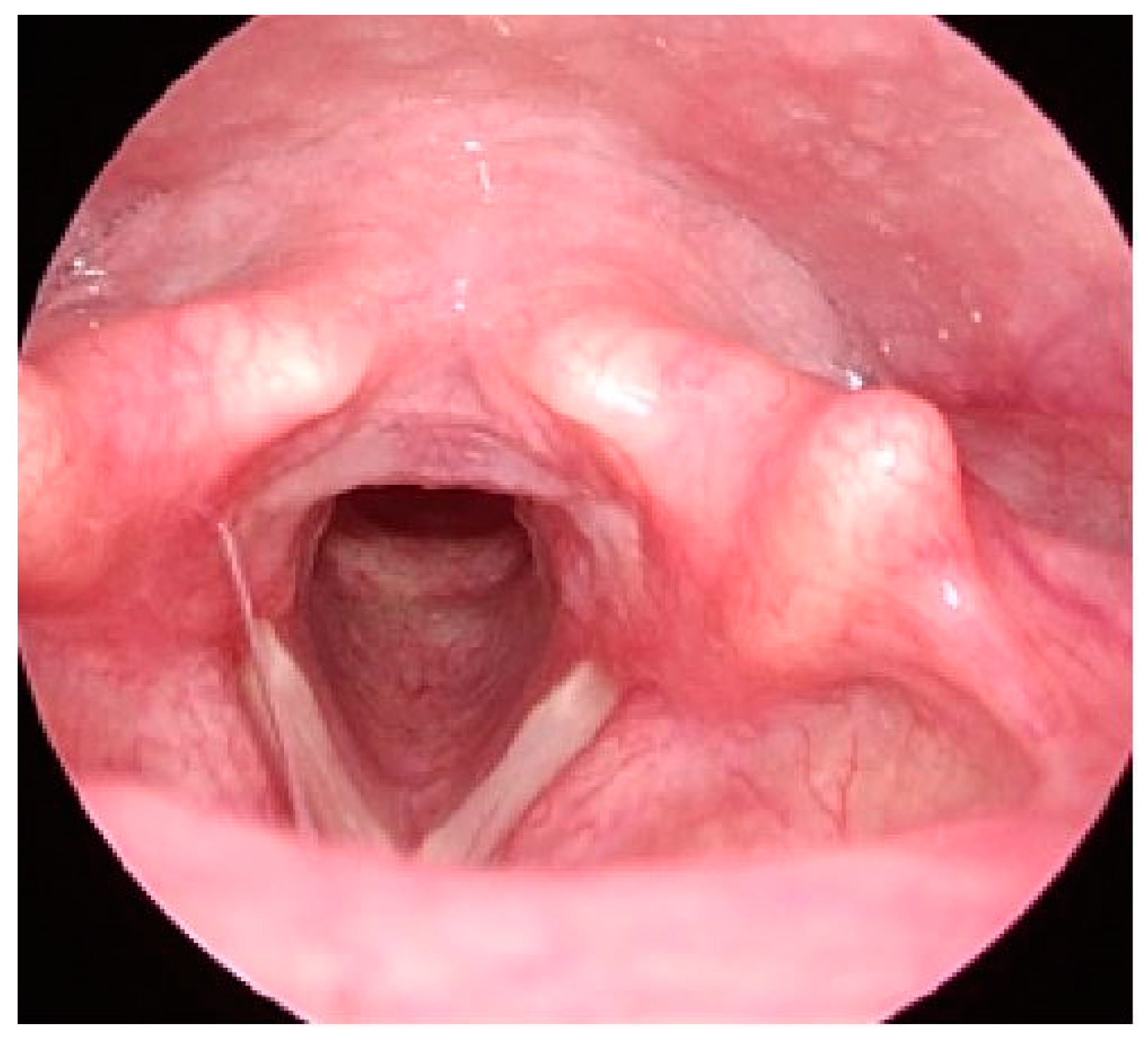
Figure 2) At the end of the procedure, anesthetic agents were discontinued, and the patient regained self-respiration after receiving sugammadex 120 mg. After confirming stable vital signs and spontaneous respiration, she was transferred to the post-anesthetic care unit (PACU). She experienced no complications in the PACU. On post-operative day (POD) 1, her follow-upindirect laryngoscope showed absence of granuloma on the vocal cords. (
Figure 3) Also, she had no symptom of dyspnea. She was discharged on POD 1 since she had no complications after the surgery.
Due to the patient’s increased risk of bleeding resulting from partial placental previa, a condition in which the placenta partially covers the cervix, a decision was made to schedule a cesarean section. This surgical procedure, aimed at ensuring the safety of both the mother and the baby, was scheduled to take place 5 months after the vocal surgery. She underwent an indirect laryngoscope prior to the surgery, revealing clear vocal cords without any granuloma. In addition to the clear findings on the indirect laryngoscope, the patient provided reassurance by reporting the absence of any recurring symptoms that were experienced prior to the development of bilateral granuloma. Specifically, she did not complain of dyspnea, hoarseness, or any discomfort in her throat. These reassuring reports further indicated the positive outcome of the procedure and her overall improved vocal health. To ensure a comprehensive evaluation, an otolaryngologic consultation was conducted to assess the condition of her vocal cords. During the consultation, the clinician carefully examined the patient’s vocal cord movement and observed no abnormal or irregular patterns. This further confirmed the successful outcome of the surgery and provided additional reassurance regarding the patient’s vocal cord health. As a result, it was deemed feasible for her to undergo general anesthesia with endotracheal intubation. Despite undergoing surgery under spinal anesthesia, she experienced no complications, and the neonate showed no signs ofdistress perioperatively.