Submitted:
19 May 2023
Posted:
23 May 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
3.1. Participant Charicteristics
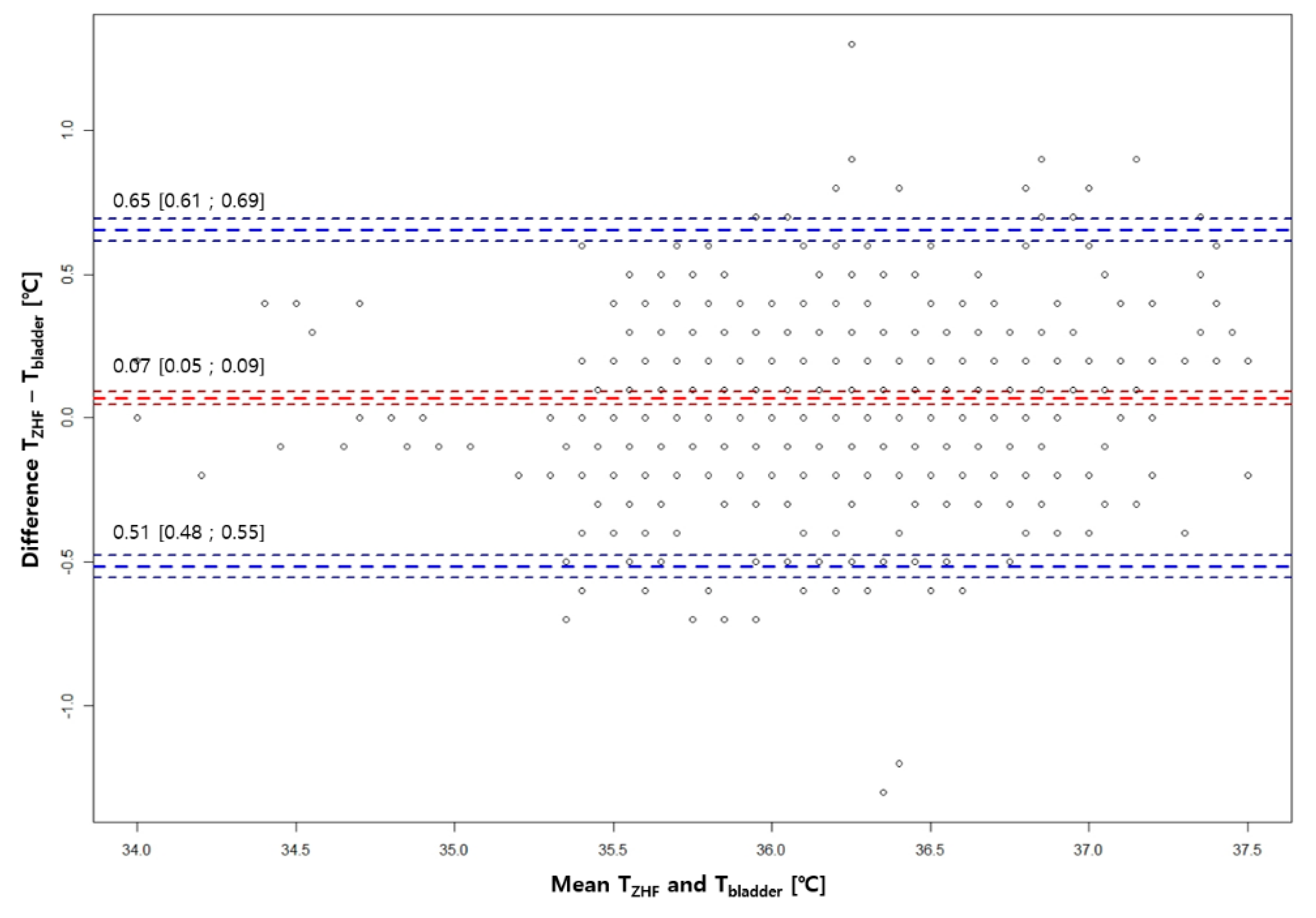
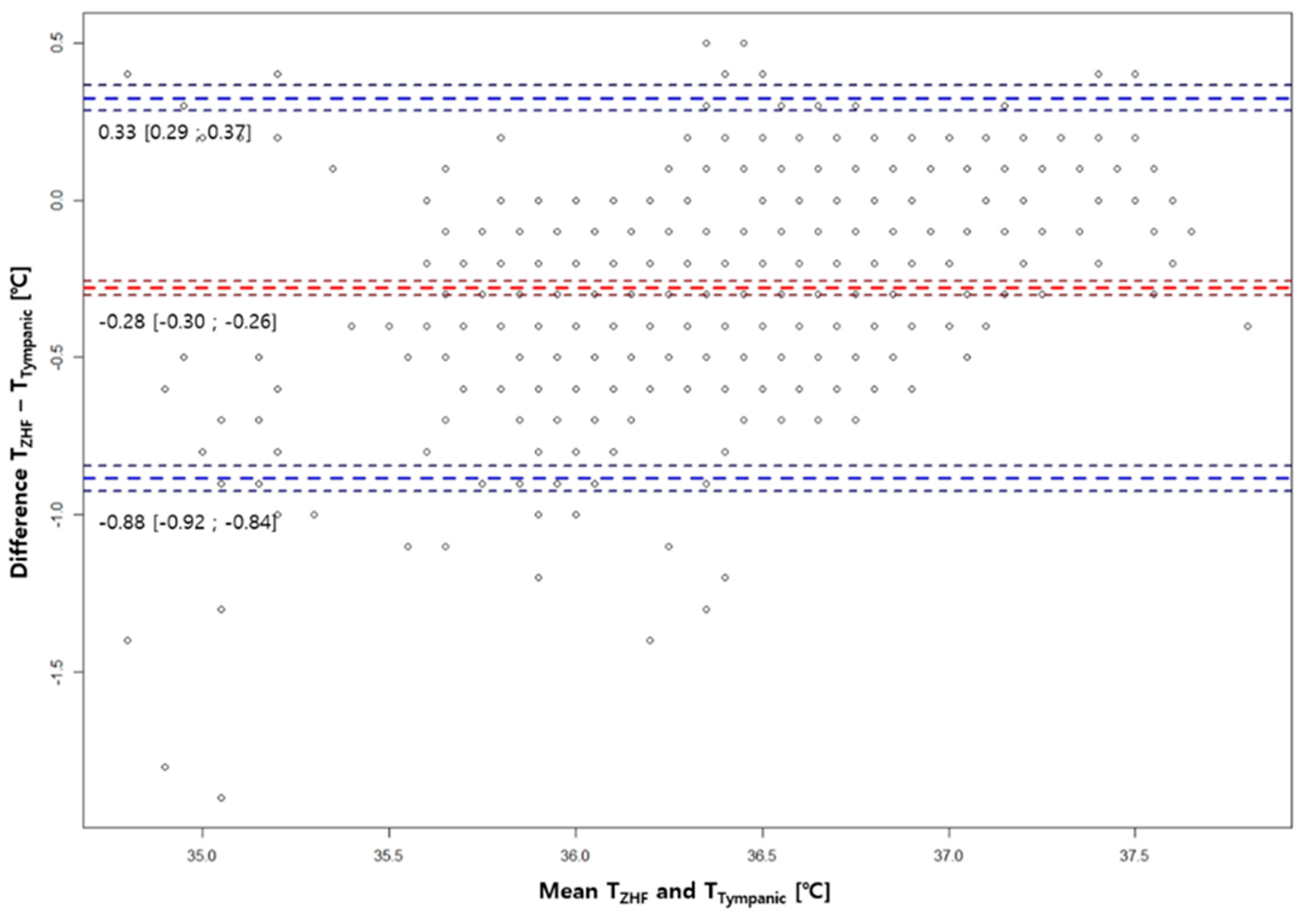
3.2. Bland-Altman Analysis Between ZHF(SpotOn®) Sensor and the Other Two Methods
3.3. Absolute Differences Between ZHF(SpotOn®) Sensor and the Other Two Methods
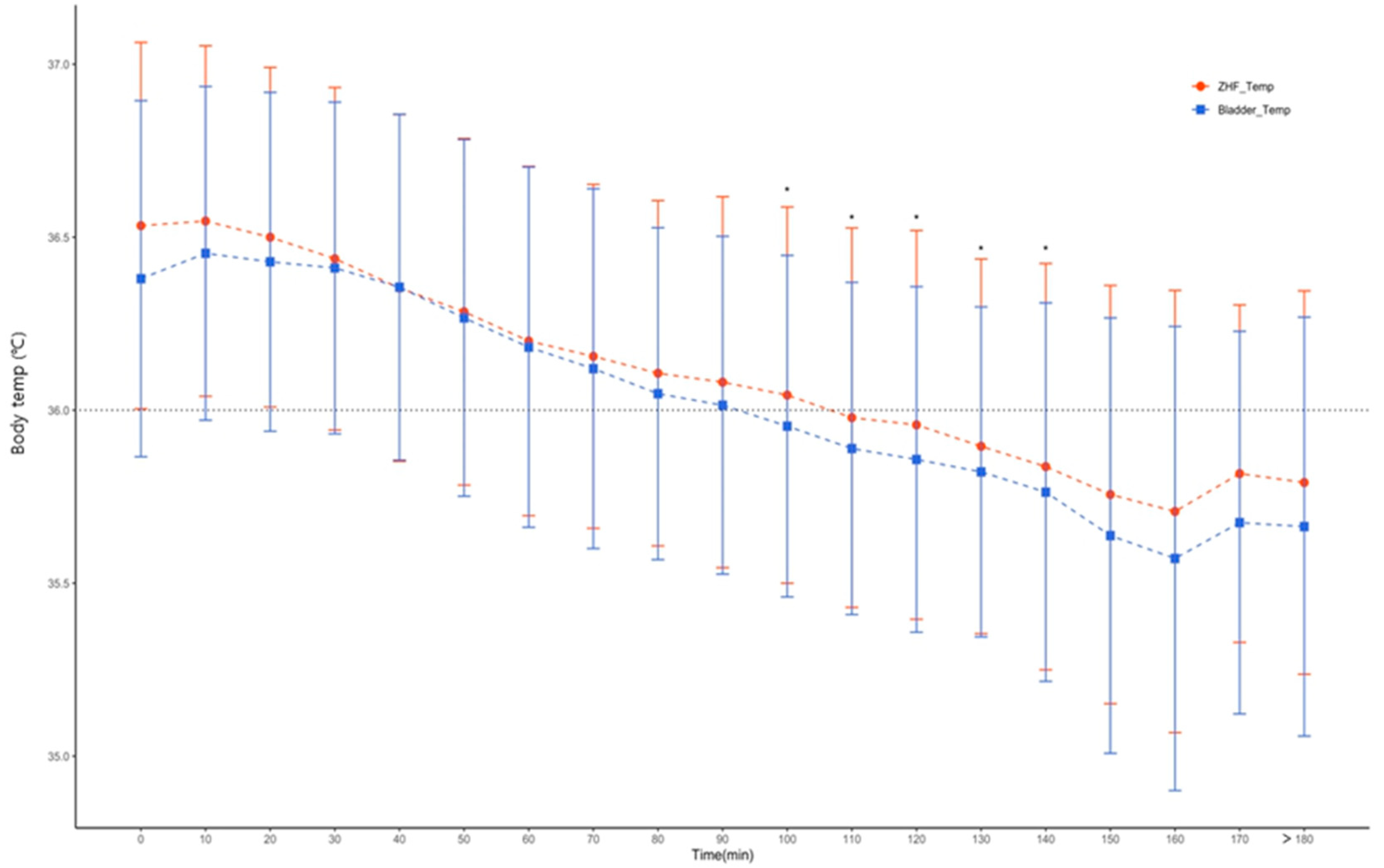
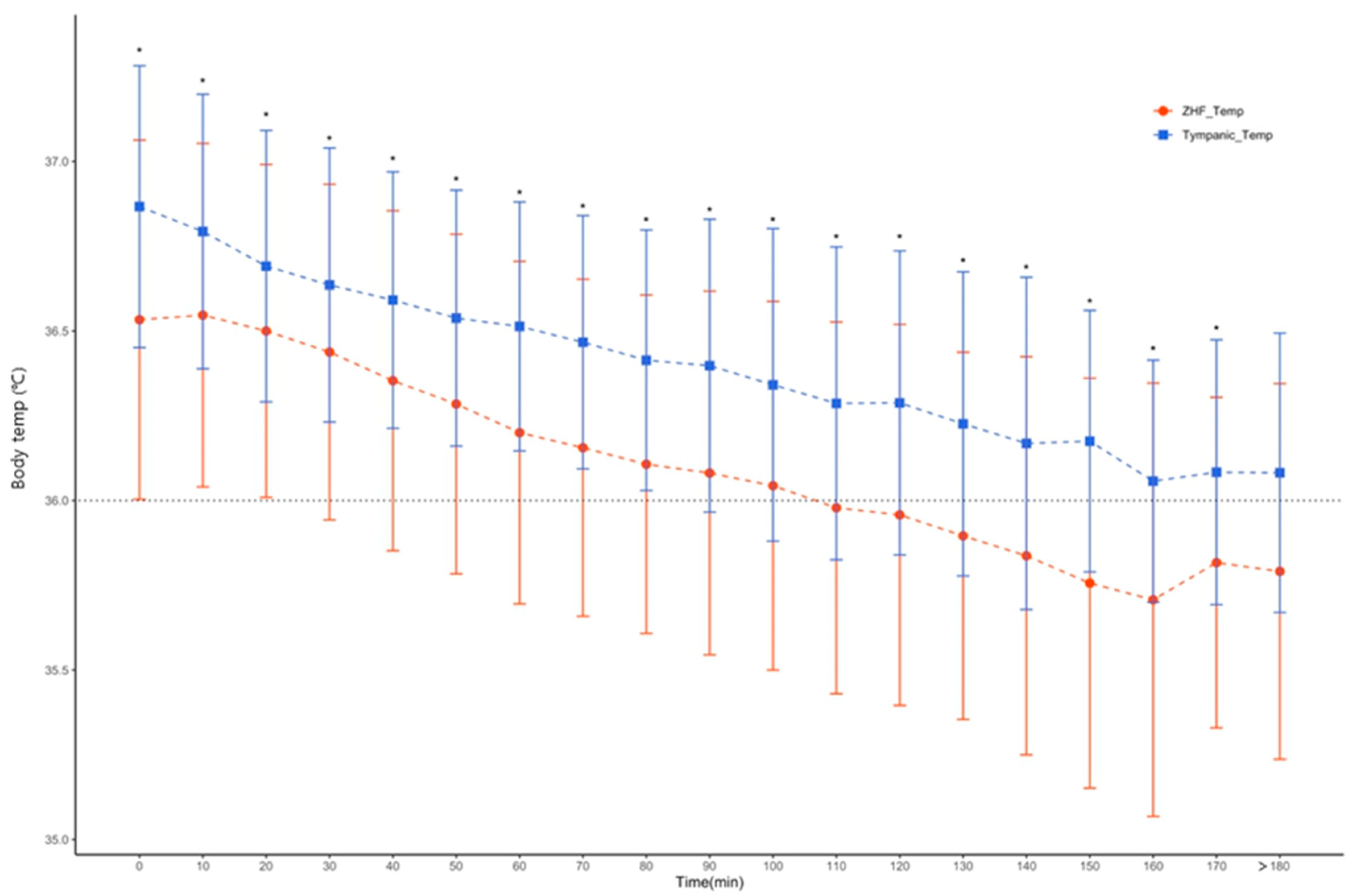
3.4. Sensitivity to detect hypothermia during lower extremity orthopedic surgery over aged 80 years
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Sessler, D.I. Perioperative thermoregulation and heat balance. Lancet. 2016, 387, 2655–2664. [Google Scholar] [CrossRef] [PubMed]
- Kurz, A.; Sessler, D.I.; Lenhardt, R. Perioperative normothermia to reduce the incidence of surgical-wound infection and shorten hospitalization. Study of Wound Infection and Temperature Group. N Engl J Med. 1996, 334, 1209–1215. [Google Scholar] [CrossRef] [PubMed]
- Lenhardt, R.; Marker, E.; Goll, V.; Tschernich, H.; Kurz, A.; Sessler, D.I.; Narzt, E.; Lackner, F. Mild intraoperative hypothermia prolongs postanesthetic recovery. Anesthesiology. 1997, 87, 1318–1323. [Google Scholar] [CrossRef] [PubMed]
- Rajagopalan, S.; Mascha, E.; Na, J.; Sessler, D.I. The effects of mild perioperative hypothermia on blood loss and transfusion requirement. Anesthesiology. 2008, 108, 71–77. [Google Scholar] [CrossRef] [PubMed]
- Frank, S.M.; Fleisher, L.A.; Breslow, M.J.; Higgins, M.S.; Olson, K.F.; Kelly, S.; Beattie, C. Perioperative maintenance of normothermia reduces the incidence of morbid cardiac events. A randomized clinical trial. JAMA. 1997, 277, 1127–1134. [Google Scholar] [CrossRef] [PubMed]
- Forbes, Shawn S.; Eskicioglu, Cagia.; Nathens, Avery B.; Fenech, Darlene S.; Laflamme, Claude; McLean, Richard F.; McLeod, *!!! REPLACE !!!*; Robin, S.; Best Practice in General Surgery Committee, University of Toronto. Evidence-based guidelines for prevention of perioperative hypothermia. J Am Coll Surg. 2009, 209, 492–503.e1. [Google Scholar] [CrossRef]
- Horn EP,; Torossian A. [Prevention of perioperative hypothermia]. Anasthesiol Intensivmed Notfallmed Schmerzther. 2010, 45, 160–167. [Google Scholar]
- Fox, R.H.; Solman, A.J.; Isaacs, R.; Fry, A.J.; MacDonald, I.C. A new method for monitoring deep body temperature from the skin surface. Clin Sci. 1973, 44, 81–86. [Google Scholar] [CrossRef]
- Teunissen, L.P.; Klewer, J.; de Haan, A.; de Koning, J.J.; Daanen, H.A. Non-invasive continuous core temperature measurement by zero heat flux. Physiol Meas. 2011, 32, 559–570. [Google Scholar] [CrossRef]
- Conway, A.; Bittner, M.; Phan, D.; Chang, K.; Kamboj, N.; Tipton, E.; Parotto, M. Accuracy and precision of zero-heat-flux temperature measurements with the 3M™ Bair Hugger™ Temperature Monitoring System: a systematic review and meta-analysis. J Clin Monit Comput. 2021, 35, 39–49. [Google Scholar] [CrossRef]
- Inoue, Y.; Nakao, M.; Araki, T.; Ueda, H. Thermoregulatory responses of young and older men to cold exposure. Eur J Appl Physiol Occup Physiol. 1992, 65, 492–498. [Google Scholar] [CrossRef] [PubMed]
- Watts, A.J. Hypothermia in the aged: a study of the role of cold-sensitivity. Environ Res. 1972, 5, 119–126. [Google Scholar] [CrossRef] [PubMed]
- Bone, M.E.; Feneck, R.O. Bladder temperature as an estimate of body temperature during cardiopulmonary bypass. Anaesthesia. 1988, 43, 181–185. [Google Scholar] [CrossRef] [PubMed]
- Bräuer, A.; Fazliu, A.; Perl, T.; Heise, D.; Meissner, K.; Brandes, I.F. Accuracy of zero-heat-flux thermometry and bladder temperature measurement in critically ill patients. Sci Rep. 2020, 10, 21746. [Google Scholar] [CrossRef]
- Fallis, W.M. Monitoring bladder temperatures in the OR. Aorn j 2002, 76, 467–476, 81-6, 88-9. [Google Scholar] [CrossRef]
- Klein, D.G.; Mitchell, C.; Petrinec, A.; Monroe, M.K.; Oblak, M.; Ross, B.; Youngblut, J.M. A comparison of pulmonary artery, rectal, and tympanic membrane temperature measurement in the ICU. Heart Lung. 1993, 22, 435–441. [Google Scholar]
- Boisson, M.; Alaux, A.; Kerforne, T.; Mimoz, O.; Debaene, B.; Dahyot-Fizelier, C.; Frasca, D. Intra-operative cutaneous temperature monitoring with zero-heat-flux technique (3M SpotOn) in comparison with oesophageal and arterial temperature: A prospective observational study. Eur J Anaesthesiol. 2018, 35, 825–830. [Google Scholar] [CrossRef]
- Kollmann Camaiora, A.; Brogly, N.; Alsina, E.; de Celis, I.; Huercio, I.; Gilsanz, F. Validation of the Zero-Heat-Flux thermometer (SpotOn®) in major gynecological surgery to monitor intraoperative core temperature: a comparative study with esophageal core temperature. Minerva Anestesiol. 2019, 85, 351–357. [Google Scholar] [CrossRef]
- Eshraghi, Y.; Nasr, V.; Parra-Sanchez, I.; Van Duren, A.; Botham, M.; Santoscoy, T.; Sessler, D.I. An evaluation of a zero-heat-flux cutaneous thermometer in cardiac surgical patients. Anesth Analg. 2014, 119, 543–549. [Google Scholar] [CrossRef]
- Dahyot-Fizelier, C.; Lamarche, S.; Kerforne, T.; Bénard, T.; Giraud, B.; Bellier, R.; Carise, E.; Frasca, D.; Mimoz, O. Accuracy of Zero-Heat-Flux Cutaneous Temperature in Intensive Care Adults. Crit Care Med. 2017, 45, e715–e717. [Google Scholar] [CrossRef]
- Sang, B.H.; Lee, C.; Lee, D.Y. Prospective comparative analysis of noninvasive body temperature monitoring using zero heat flux technology (SpotOn sensor) compared with esophageal temperature monitoring during pediatric surgery. PLoS One. 2022, 17, e0272720. [Google Scholar] [CrossRef] [PubMed]
- Pesonen, E.; Silvasti-Lundell, M.; Niemi, T.T.; Kivisaari, R.; Hernesniemi, J.; Mäkinen, M.T. The focus of temperature monitoring with zero-heat-flux technology (3M Bair-Hugger): a clinical study with patients undergoing craniotomy. J Clin Monit Comput. 2019, 33, 917–923. [Google Scholar] [CrossRef] [PubMed]
- Niven, D.J.; Gaudet, J.E.; Laupland, K.B.; Mrklas, K.J.; Roberts, D.J.; Stelfox, H.T. Accuracy of peripheral thermometers for estimating temperature: a systematic review and meta-analysis. Ann Intern Med. 2015, 163, 768–777. [Google Scholar] [CrossRef]
- Verheyden, C.; Neyrinck, A.; Laenen, A.; Rex, S.; Van Gerven, E. Clinical evaluation of a cutaneous zero-heat-flux thermometer during cardiac surgery. J Clin Monit Comput. 2022, 36, 1279–1287. [Google Scholar] [CrossRef] [PubMed]
- Cattaneo, C.G.; Frank, S.M.; Hesel, T.W.; El-Rahmany, H.K.; Kim, L.J.; Tran, K.M. The accuracy and precision of body temperature monitoring methods during regional and general anesthesia. Anesth Analg. 2000, 90, 938–945. [Google Scholar] [CrossRef]
- Frank, S.M.; Shir, Y.; Raja, S.N.; Fleisher, L.A.; Beattie, C. Core hypothermia and skin-surface temperature gradients. Epidural versus general anesthesia and the effects of age. Anesthesiology. 1994, 80, 502–508. [Google Scholar] [CrossRef]
| General | |
|---|---|
| Sex (M/F) | 9(20%)/36(80%) |
| Age (year) | 85.2 ± 4.7 |
| BMI (kg/m2) | 22.4 ± 3.69 |
| ASA physical status | |
| ASA 1 | 0 |
| ASA 2 | 32(71%) |
| ASA 3 | 13(29%) |
| Type of surgery | |
| Hip surgery | 34(76%) |
| Knee surgery | 11(24%) |
| Type of anesthesia | |
| General | 9(20%) |
| Spinal | 36(80%) |
| Duration of the operation | 116 ± 40 |
| Total Input | 1496 ± 702 |
| Total Output | 632 ± 490 |
| ZHF vs. Bladder thermometer | ZHF vs. Tympanic thermometer | |
| ≤±0.3℃ | 526/679(77.5%) | 405/679(59.6%) |
| ≤±0.5℃ | 635/679(93.5%) | 588/679(86.6%) |
| ≤±0.8℃ | 671/679(98.8%) | 650/679(95.7%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




