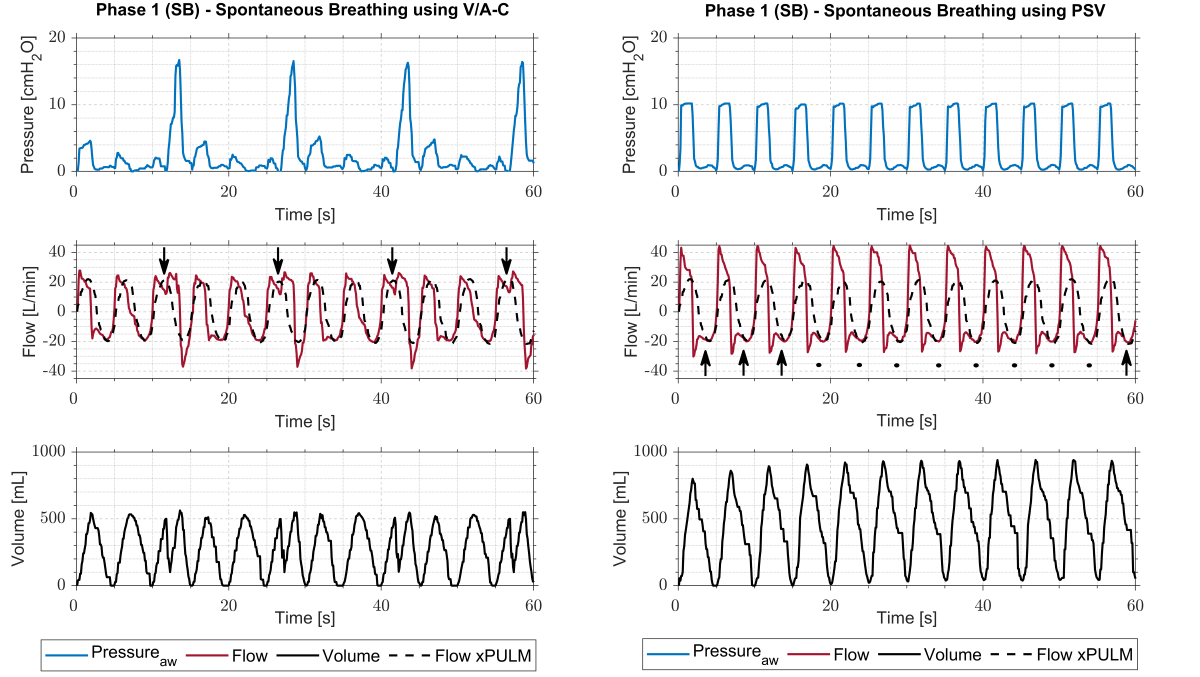
During mechanical ventilation, a disparity between flow, pressure or volume demands of the patient and the assistance delivered by the mechanical ventilator often occurs. Asynchrony effect and ventilator performance are frequently studied from ICU datasets or using commercially available lung simulators and test lungs. This paper introduces an alternative approach of simulating and evaluating patient-ventilator interactions with high fidelity using the electro-mechanical lung simulator xPULM™ under selected conditions. The xPULM™ approximates respiratory activities of a patient during alternating phases of spontaneous breathing and apnoea intervals while connected to a mechanical ventilator. Focusing on different triggering events, volume assist-controlled (V/A-C) and pressure support ventilation (PSV) modes were chosen to test patient-ventilator interactions. In V/A-C mode a double-triggering was detected every third breathing cycle leading to an asynchrony index of 16.67%, being classified as severe. This asynchrony causes a major increase of Peak Inspiratory Pressure PIP = 12.80 ± 1.39 cmH2O and Peak Expiratory Flow PEF = -18.33 ± 1.13 L/min when compared to synchronous phases of the breathing simulation. Additionally, events of premature cycling were observed during PSV mode. In this mode, the peak delivered volume during simulated spontaneous breathing phases almost doubles compared to apnoea phases. The presented approach demonstrates the possibility of simulating and evaluating disparities in fundamental ventilation characteristics caused by double-triggering and premature cycling under V/A-C and PSV ventilation modes. Various dynamic clinical situations can be approximated and could help to identify undesired patient-ventilation interactions in the future. Rapidly manufactured ventilator systems could also be tested using this approach.