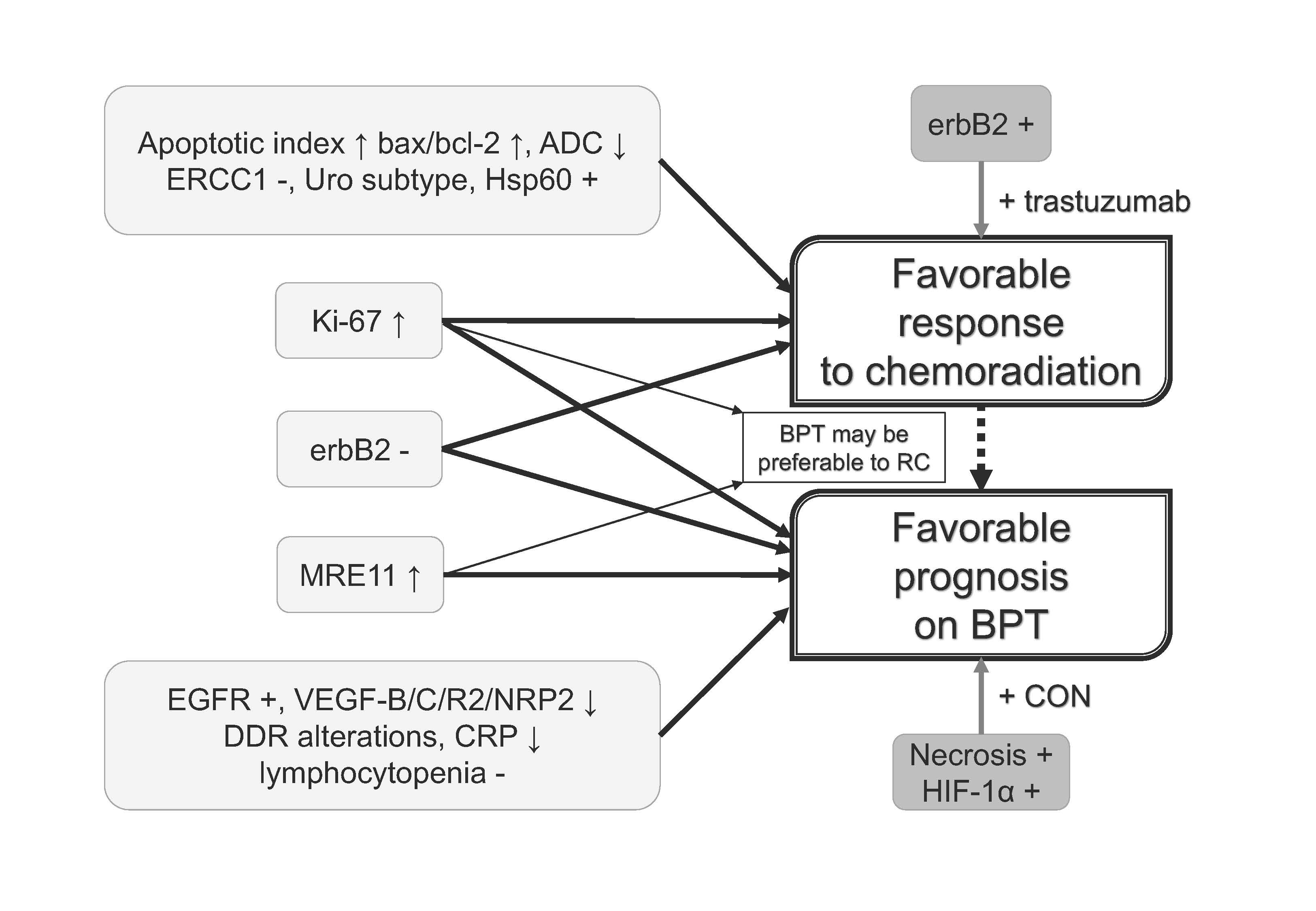
Chemoradiation-based bladder preservation therapy (BPT) is currently a curative option for non-metastatic muscle-invasive bladder cancer (MIBC) patients at favorable risk or an alternative to radical cystectomy (RC) for those who are unfit for RC. In BPT, only patients who achieve complete response (CR) after chemoradiation have favorable prognosis and quality of life with preserved functional bladder. Thus, predicting CR and favorable prognosis is important for optimal patient selection for BPT. We reviewed biomarkers for predicting clinical outcomes of chemoradiation-based BPT. Biomarkers studied were categorized into those related to apoptosis, cell proliferation, receptor tyrosine kinases, DNA damage response genes, hypoxia, molecular subtype, and others. Among these biomarkers, Ki-67 labeling index (Ki-67 LI) and meiotic recombination 11 may be used for selecting BPT or RC. Ki-67 LI and erythroblastic leukemia viral oncogene homolog 2 (erbB2) may be used for predicting both chemoradiation response and prognosis of patients on BPT. Concurrent use of trastuzumab and a combination of carbogen and nicotinamide can overcome chemoradiation resistance conferred by erbB2 overexpression and tumor hypoxia. Further studies are needed to confirm the practical utility of these biomarkers for progress on biomarker-directed personalized management of MIBC patients.