Submitted:
18 November 2025
Posted:
19 November 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results

- 1. General characteristics
| Total (n=273) | Male (n=149) | Female (n=124) | |
| Anthropology, Clinical | |||
| Age (years) | 69 (55-76) | 64 (52-74) | 71 (62-78) |
| Height (m) | 1.60 (1.55-1.65) | 1.65 (1.60-1.67) | 1.55 (1.50-1.58) |
| Weight (kg) | 58 (50-65) | 60 (55-66) | 53 (48.5-60) |
| BMI (kg/m2) | 22.5 (20.7-24.1) | 23.1 (20.9-24.2) | 22.0 (20.0-23.4) |
| Systolic BP (mmHg) | 130 (120-140) | 125 (120-140) | 130 (120-140) |
| Diastolic BP (mmHg) | 74 (70-80) | 75 (70-80) | 78 (70-80) |
| Laboratory Tests | |||
| HGB (g/L) | 128 (115-138) | 134 (126-144) | 119 (109-129) |
| HCT (%) | 38.3 (35.0-41.3) | 40.1 (37.6-42.8) | 35.6 (30.0-38.6) |
| WBC (G/L) | 8.0 (6.7-10.0) | 8.2 (6.9-9.8) | 7.8 (6.2-10.0) |
| PLT (G/L) | 188 (137-233) | 173 (141-214) | 200 (128-269) |
| INR | 1.05 (1.01-1.13) | 1.06 (1.02-1.14) | 1.04 (1.00-1.11) |
| Creatinine (mg/dL) | 0.89 (0.76-1.10) | 0.96 (0.82-1.16) | 0.81 (0.67-0.97) |
| eGFR (mL/min/1.73m2) | 80.6 (62.3-93.6) | 84.5 (64.5-97.8) | 73.3 (57.7-90.3) |
| Free T4 (pg/mL) | 12.4 (11.2-13.7) | 12.4 (11.2-13.9) | 12.4 (11.2-13.6) |
| TSH (mIU/L) | 1.41 (0.79-2.25) | 1.24 (0.70-2.07) | 1.48 (0.88-2.30) |
| Echocardiography | |||
| EF (%) | 65 (57-71) | 63 (53-71) | 66 (58-71) |
| EDV (mL) | 102 (84-129) | 108 (89-135) | 97 (78-118) |
| ESV (mL) | 36 (27-52) | 38 (29-61) | 32 (26-43) |
| LVEDD (mm) | 47 (43-52) | 48 (44-53) | 46 (42-50) |
| LVESD (mm) | 30 (27-34) | 31 (28-37) | 29 (26-32) |
- 2.
- hs-cTnI Levels
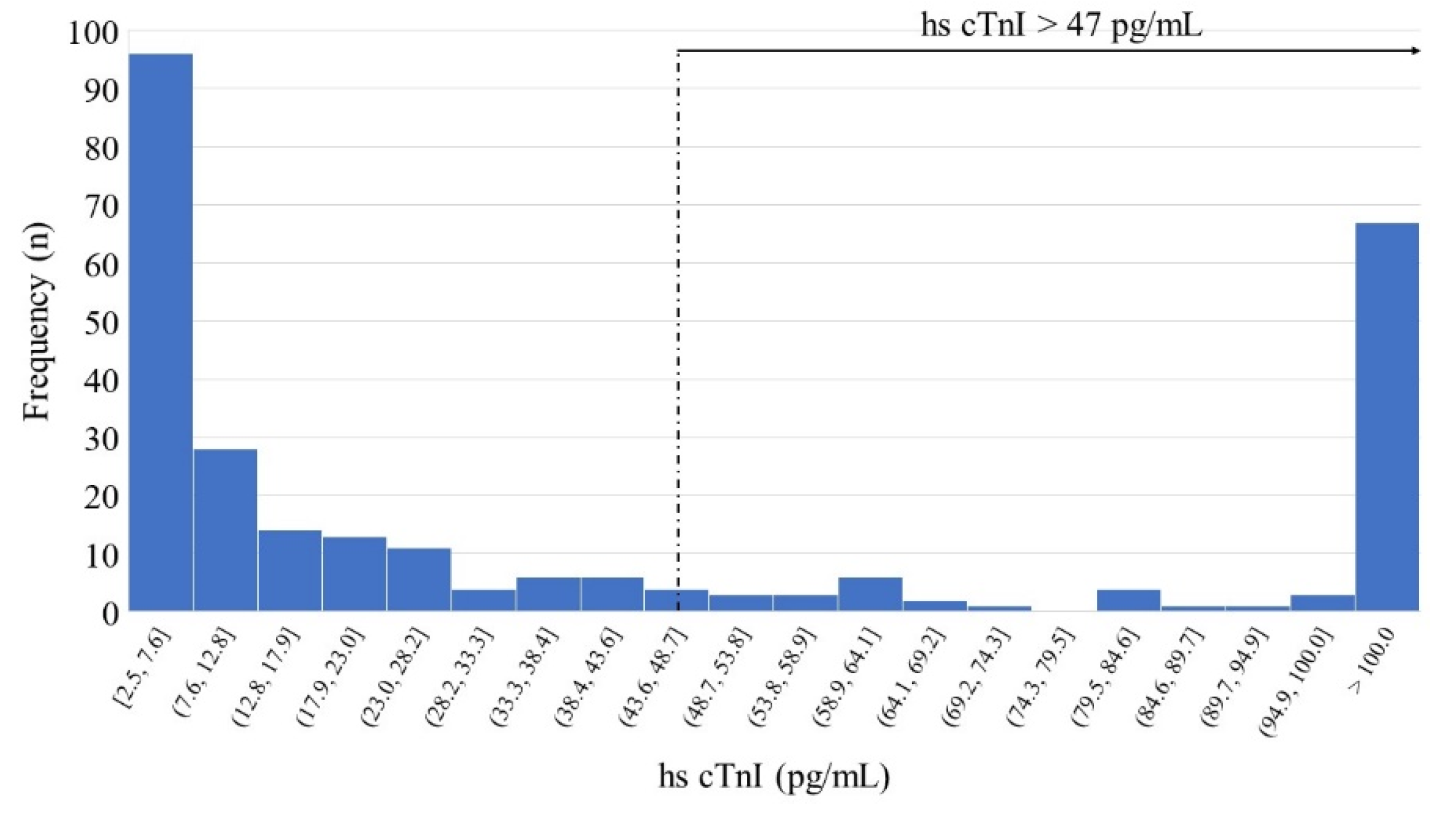
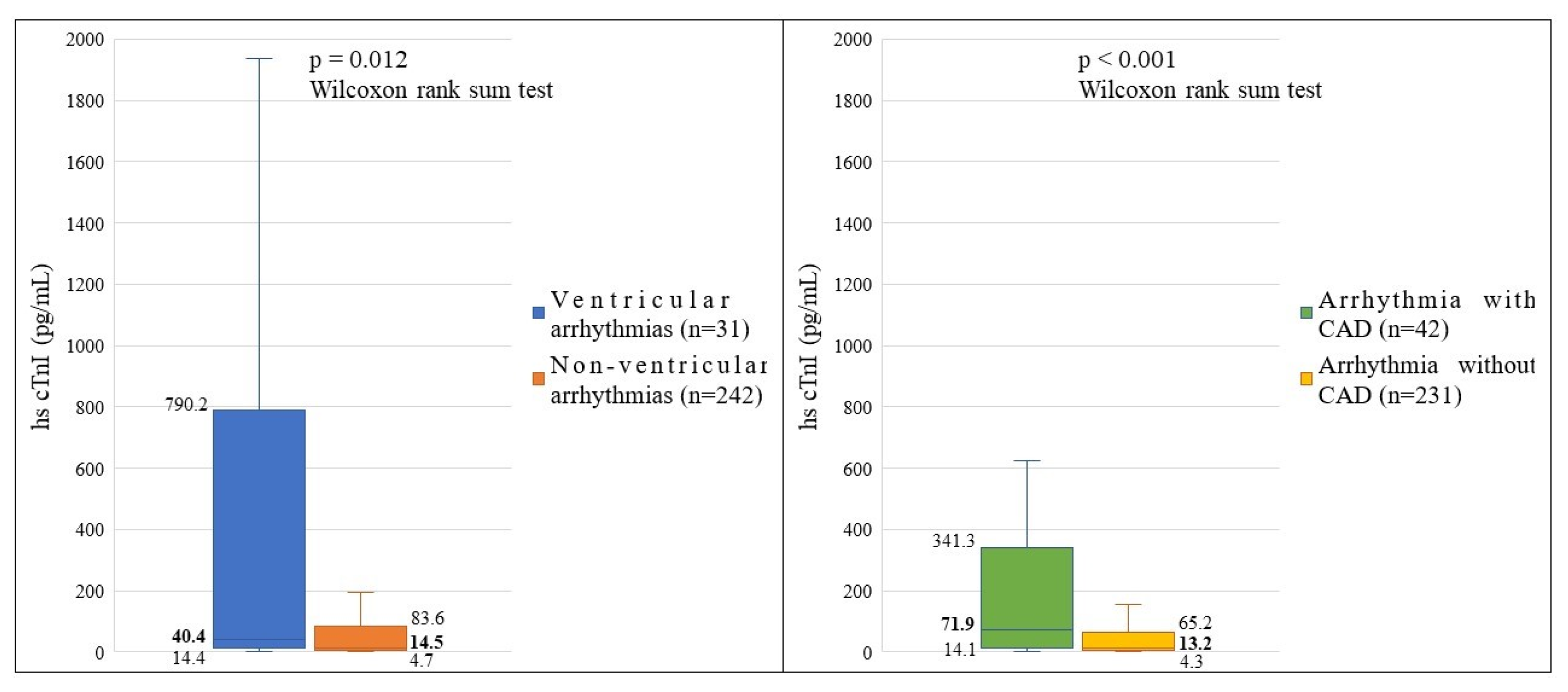
- 3.
- Correlations Between hs-cTnI Levels and Other Variables
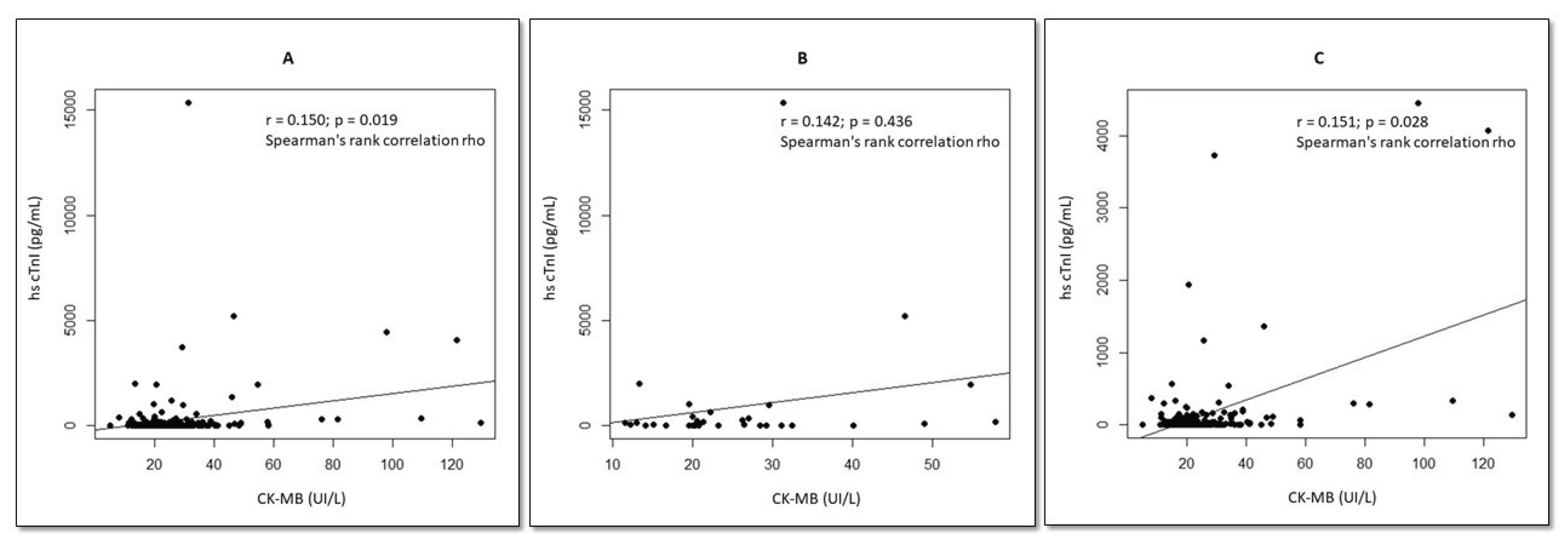
| Variable | Spearman's Rank Correlation rho | P |
| Age (years) | 0.016 | 0.929 |
| BMI (kg/m2) | 0.305 | 0.094 |
| Creatinine (mg/dL) | 0.161 | 0.384 |
| eGFR (mL/min/1.73m2) | -0,051 | 0.782 |
| NT-proBNP (pg/mL) | 0.509 | 0.003 |
| TSH (mIU/L) | -0.129 | 0.504 |
| HGB (g/L) | 0.154 | 0.407 |
| WBC (G/L) | 0.548 | 0.001 |
| PLT(G/L) | 0.271 | 0.139 |
| EF (%) | -0.280 | 0.126 |
| EDV (mL) | 0.336 | 0.068 |
| ESV (mL) | 0.269 | 0.142 |
| LVEDD (mm) | 0.302 | 0.104 |
| LVESD (mm) | 0.353 | 0.059 |
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AHA | American Heart Association |
| AMI | Acute Myocardial Infarction |
| CAD | Coronary Artery Disease |
| CBC | Complete Blood Count |
| CK-MB | Creatine Kinase-MB |
| EDV | End Diastolic Volume |
| EF | Ejection Fraction |
| ESV | End Systolic Volume |
| hs-cTnI | High-sensitivity Cardiac Troponin I |
| LVEDD | Left Ventricular End Diastolic Diameter |
| LVESD | Left Ventricular End Systolic Diameter |
| NVAs | Non-ventricular Arrhythmias |
| VAs | Ventricular Arrhythmias |
| VT | Ventricular Tachycardia |
References
- Srinivasan, N.T.; Schilling, R.J. Sudden Cardiac Death and Arrhythmias. Arrhythm Electrophysiol Rev 2018, 7, 111–117. [Google Scholar] [CrossRef] [PubMed]
- Hayashi, M.; Shimizu, W.; Albert, C.M. The spectrum of epidemiology underlying sudden cardiac death. Circ Res 2015, 116, 1887–1906. [Google Scholar] [CrossRef] [PubMed]
- Desai, D.S.; Hajouli, S. Arrhythmias. In StatPearls; Treasure Island (FL) ineligible companies. Disclosure: Said Hajouli declares no relevant financial relationships with ineligible companies., 2024.
- Zainal, H. Understanding Troponin as a Biomarker of Myocardial Injury: Where the Path Crosses with Cardiac Imaging. Cardiology 2023, 148, 228–229. [Google Scholar] [CrossRef] [PubMed]
- Mariathas, M.; Gemmell, C.; Olechowski, B.; Nicholas, Z.; Mahmoudi, M.; Curzen, N. High sensitivity troponin in the management of tachyarrhythmias. Cardiovasc Revasc Med 2018, 19, 487–492. [Google Scholar] [CrossRef]
- McCarthy, C.P.; Yousuf, O.; Alonso, A.; Selvin, E.; Calkins, H.; McEvoy, J.W. High-Sensitivity Troponin as a Biomarker in Heart Rhythm Disease. Am J Cardiol 2017, 119, 1407–1413. [Google Scholar] [CrossRef]
- Virani, S.S.; Newby, L.K.; Arnold, S.V.; Bittner, V.; Brewer, L.C.; Demeter, S.H.; Dixon, D.L.; Fearon, W.F.; Hess, B.; Johnson, H.M.; et al. 2023 AHA/ACC/ACCP/ASPC/NLA/PCNA Guideline for the Management of Patients With Chronic Coronary Disease: A Report of the American Heart Association/American College of Cardiology Joint Committee on Clinical Practice Guidelines. Circulation 2023, 148, e9–e119. [Google Scholar] [CrossRef]
- Stark, M.; Kerndt, C.C.; Sharma, S. Troponin. In StatPearls; Treasure Island (FL) ineligible companies. Disclosure: Connor Kerndt declares no relevant financial relationships with ineligible companies. Disclosure: Sandeep Sharma declares no relevant financial relationships with ineligible companies., 2024.
- Kumar, D.A.; Muneer, D.K.; Qureshi, D.N. Relationship between high sensitivity troponin I and clinical outcomes in non-acute coronary syndrome (non-ACS) acute heart failure patients - a one-year follow-up study. Indian Heart J 2024, 76, 139–145. [Google Scholar] [CrossRef]
- Ramasamy, I. Highly sensitive troponin I assay in the diagnosis of coronary artery disease in patients with suspected stable angina. World J Cardiol 2021, 13, 745–757. [Google Scholar] [CrossRef]
- Bandorski, D.; Holtgen, R.; Wieczorek, M.; Ghofrani, H.A.; Bogossian, H.; Iliodromitis, K. Evaluation of troponin I serum levels in patients with arrhythmias with and without coronary artery disease. Med Klin Intensivmed Notfmed 2024, 119, 39–45. [Google Scholar] [CrossRef]
- Schmalstieg-Bahr, K.; Gladstone, D.J.; Hummers, E.; Suerbaum, J.; Healey, J.S.; Zapf, A.; Koster, D.; Werhahn, S.M.; Wachter, R. Biomarkers for predicting atrial fibrillation: An explorative sub-analysis of the randomised SCREEN-AF trial. Eur J Gen Pract 2024, 30, 2327367. [Google Scholar] [CrossRef]
- Moore, J.P.; Arcilla, L.; Wang, S.; Lee, M.S.; Shannon, K.M. Characterization of Cardiac Troponin Elevation in the Setting of Pediatric Supraventricular Tachycardia. Pediatr Cardiol 2016, 37, 392–398. [Google Scholar] [CrossRef] [PubMed]
- White, H.D. Higher sensitivity troponin levels in the community: what do they mean and how will the diagnosis of myocardial infarction be made? Am Heart J 2010, 159, 933–936. [Google Scholar] [CrossRef] [PubMed]
- Costabel, J.P.; Burgos, L.M.; Trivi, M. The Significance Of Troponin Elevation In Atrial Fibrillation. J Atr Fibrillation 2017, 9, 1530. [Google Scholar] [CrossRef] [PubMed]
- Chow, G.V.; Hirsch, G.A.; Spragg, D.D.; Cai, J.X.; Cheng, A.; Ziegelstein, R.C.; Marine, J.E. Prognostic significance of cardiac troponin I levels in hospitalized patients presenting with supraventricular tachycardia. Medicine (Baltimore) 2010, 89, 141–148. [Google Scholar] [CrossRef]
- Eggers, K.M.; Johnston, N.; Lind, L.; Venge, P.; Lindahl, B. Cardiac troponin I levels in an elderly population from the community--The implications of sex. Clin Biochem 2015, 48, 751–756. [Google Scholar] [CrossRef]
- Liu, L.; Liu, S.; Shen, L.; Tu, B.; Hu, Z.; Hu, F.; Zheng, L.; Ding, L.; Fan, X.; Yao, Y. Correlations between cardiac troponin I and nonsustained ventricular tachycardia in hypertrophic obstructive cardiomyopathy. Clin Cardiol 2020, 43, 1150–1159. [Google Scholar] [CrossRef]
- Ocak, T.; Erdem, A.; Duran, A.; Tekelioglu, U.Y.; Ozturk, S.; Ayhan, S.S.; Ozlu, M.F.; Tosun, M.; Kocoglu, H.; Yazici, M. The diagnostic significance of NT-proBNP and troponin I in emergency department patients presenting with palpitations. Clinics (Sao Paulo) 2013, 68, 543–547. [Google Scholar] [CrossRef]
- Mohebi, R.; Jackson, L.; McCarthy, C.P.; Murtagh, G.; Murphy, S.P.; Abboud, A.; Miksenas, H.; Gaggin, H.K.; Januzzi, J.L., Jr. Relation of High-Sensitivity Cardiac Troponin I and Obstructive Coronary Artery Disease in Patients Without Acute Myocardial Infarction. Am J Cardiol 2022, 173, 16–24. [Google Scholar] [CrossRef]
- Horjen, A.W.; Ulimoen, S.R.; Norseth, J.; Svendsen, J.H.; Smith, P.; Arnesen, H.; Seljeflot, I.; Tveit, A. High-sensitivity troponin I in persistent atrial fibrillation - relation to NT-proBNP and markers of inflammation and haemostasis. Scand J Clin Lab Invest 2018, 78, 386–392. [Google Scholar] [CrossRef]
- Horjen, A.W.; Ulimoen, S.R.; Enger, S.; Norseth, J.; Seljeflot, I.; Arnesen, H.; Tveit, A. Troponin I levels in permanent atrial fibrillation-impact of rate control and exercise testing. BMC Cardiovasc Disord 2016, 16, 79. [Google Scholar] [CrossRef]
- Lebedeva, V.K.; Klitcenko, O.A.; Lebedev, D.S.; Lyubimtseva, T.A. Ventricular tachycardia prediction in patients with implantable cardioverter-defibrillators for primary prevention of sudden cardiac death. Indian Pacing Electrophysiol J 2019, 19, 57–62. [Google Scholar] [CrossRef]
- Chugh, S.S.; Reinier, K.; Uy-Evanado, A.; Chugh, H.S.; Elashoff, D.; Young, C.; Salvucci, A.; Jui, J. Prediction of Sudden Cardiac Death Manifesting With Documented Ventricular Fibrillation or Pulseless Ventricular Tachycardia. JACC Clin Electrophysiol 2022, 8, 411–423. [Google Scholar] [CrossRef]
- Frampton, J.; Ortengren, A.R.; Zeitler, E.P. Arrhythmias After Acute Myocardial Infarction. Yale J Biol Med 2023, 96, 83–94. [Google Scholar] [CrossRef]
- Vazquez-Calvo, S.; Roca-Luque, I.; Althoff, T.F. Management of Ventricular Arrhythmias in Heart Failure. Curr Heart Fail Rep 2023, 20, 237–253. [Google Scholar] [CrossRef] [PubMed]
- Khanal, R.R.; Gajurel, R.M.; Shah, S.; Poudel, C.M.; Shrestha, H.; Devkota, S.; Thapa, S. Arrhythmias: Its Occurrence, Risk Factors, Therapy, and Prognosis in Acute Coronary Syndrome. J Nepal Health Res Counc 2023, 21, 8–14. [Google Scholar] [CrossRef] [PubMed]
- Severino, P.; D'Amato, A.; Pucci, M.; Infusino, F.; Adamo, F.; Birtolo, L.I.; Netti, L.; Montefusco, G.; Chimenti, C.; Lavalle, C.; et al. Ischemic Heart Disease Pathophysiology Paradigms Overview: From Plaque Activation to Microvascular Dysfunction. Int J Mol Sci 2020, 21. [Google Scholar] [CrossRef] [PubMed]
- Bessiere, F.; Mondesert, B.; Chaix, M.A.; Khairy, P. Arrhythmias in adults with congenital heart disease and heart failure. Heart Rhythm O2 2021, 2, 744–753. [Google Scholar] [CrossRef]
- Shoureshi, P.; Tan, A.Y.; Koneru, J.; Ellenbogen, K.A.; Kaszala, K.; Huizar, J.F. Arrhythmia-Induced Cardiomyopathy: JACC State-of-the-Art Review. J Am Coll Cardiol 2024, 83, 2214–2232. [Google Scholar] [CrossRef]
- Raymond-Paquin, A.; Nattel, S.; Wakili, R.; Tadros, R. Mechanisms and Clinical Significance of Arrhythmia-Induced Cardiomyopathy. Can J Cardiol 2018, 34, 1449–1460. [Google Scholar] [CrossRef]
- Lazar, D.R.; Lazar, F.L.; Homorodean, C.; Cainap, C.; Focsan, M.; Cainap, S.; Olinic, D.M. High-Sensitivity Troponin: A Review on Characteristics, Assessment, and Clinical Implications. Dis Markers 2022, 2022, 9713326. [Google Scholar] [CrossRef]
- Shomanova, Z.; Ohnewein, B.; Schernthaner, C.; Hofer, K.; Pogoda, C.A.; Frommeyer, G.; Wernly, B.; Brandt, M.C.; Dieplinger, A.M.; Reinecke, H.; et al. Classic and Novel Biomarkers as Potential Predictors of Ventricular Arrhythmias and Sudden Cardiac Death. J Clin Med 2020, 9. [Google Scholar] [CrossRef] [PubMed]
- Novack, M.L.; Zubair, M. Natriuretic Peptide B Type Test. In StatPearls; Treasure Island (FL) ineligible companies. Disclosure: Muhammad Zubair declares no relevant financial relationships with ineligible companies., 2024.
- Sandoval, Y.; Jaffe, A.S. The Evolving Role of Cardiac Troponin: From Acute to Chronic Coronary Syndromes. J Am Coll Cardiol 2023, 82, 486–488. [Google Scholar] [CrossRef] [PubMed]
- Lazzerini, P.E.; Abbate, A.; Boutjdir, M.; Capecchi, P.L. Fir(e)ing the Rhythm: Inflammatory Cytokines and Cardiac Arrhythmias. JACC Basic Transl Sci 2023, 8, 728–750. [Google Scholar] [CrossRef]
- Chen, M.; Li, X.; Wang, S.; Yu, L.; Tang, J.; Zhou, S. The Role of Cardiac Macrophage and Cytokines on Ventricular Arrhythmias. Front Physiol 2020, 11, 1113. [Google Scholar] [CrossRef]
- Pluijmert, N.J.; Atsma, D.E.; Quax, P.H.A. Post-ischemic Myocardial Inflammatory Response: A Complex and Dynamic Process Susceptible to Immunomodulatory Therapies. Front Cardiovasc Med 2021, 8, 647785. [Google Scholar] [CrossRef]
- Castillo, E.C.; Vazquez-Garza, E.; Yee-Trejo, D.; Garcia-Rivas, G.; Torre-Amione, G. What Is the Role of the Inflammation in the Pathogenesis of Heart Failure? Curr Cardiol Rep 2020, 22, 139. [Google Scholar] [CrossRef]
- Zahid, M.; Sonel, A.F.; Kelley, M.E.; Wall, L.; Whittle, J.; Fine, M.J.; Good, C.B. Effect of both elevated troponin-I and peripheral white blood cell count on prognosis in patients with suspected myocardial injury. Am J Cardiol 2005, 95, 970–972. [Google Scholar] [CrossRef]
- Cheng, M.L.; Chen, C.M.; Gu, P.W.; Ho, H.Y.; Chiu, D.T. Elevated levels of myeloperoxidase, white blood cell count and 3-chlorotyrosine in Taiwanese patients with acute myocardial infarction. Clin Biochem 2008, 41, 554–560. [Google Scholar] [CrossRef] [PubMed]
|
Ventricular Arrhythmias (n = 31) |
Non-Ventricular Arrhythmias (n = 242) |
Arrhythmia with CAD n = 42) |
Arrhythmia without CAD (n = 231) |
|
| Anthropology, Clinical | ||||
| Age (years) | 67 (55-72) | 69 (55-76) | 71 (61-76) | 67 (55-76) |
| Height (m) | 1.60 (1.55-1.63) | 1.60 (1.55-1.65) | 1.60 (1.55-1.65) | 1.60 (1.55-1.65) |
| Weight (kg) | 60 (49-65) | 57 (50-65) | 58 (54-65) | 57 (50-65) |
| BMI (kg/m2) | 22.8 (20.3-24.3) | 22.2 (20.7-24.0) | 22.8 (21.2-25.0) | 22.2 (20.6-24.0) |
| Systolic BP (mmHg) | 120 (110-138) | 130 (120-140) | 120 (110-137) | 130 (120-140) |
| Diastolic BP (mmHg) | 76 (70-80) | 73 (70-80) | 72 (70-80) | 75 (70-80) |
| Laboratory Tests | ||||
| HGB (g/L) | 131 (127-141) | 128 (114-137) | 130 (117-139) | 128 (115-138) |
| HCT (%) | 40 (37-42) | 38 (34-41) | 39 (35-41) | 38 (35-41) |
| WBC (G/L) | 9.1 (6.9-11.8) | 7.8 (6.6-9.8) | 7.8 (6.7-10.3) | 8.0 (6.6-9.8) |
| PLT (G/L) | 216 (145-298) | 183 (134-227) | 162 (131-220) | 191 (138-235) |
| INR | 1.05 (1.04-1.16) | 1.05 (1.01-1.12) | 1.05 (1.00-1.20) | 1.05 (1.02-1.12) |
| Creatinine (mg/dL) | 0.87 (0.70-1.03) | 0.89 (0.77-1.11) | 0.98 (0.82-1.23) | 0.87 (0.75-1.08) |
| eGFR (mL/min/1.73m2) | 83.9 (70.4-95.9) | 78.9 (62.1-93.4) | 69.9 (51.2-89.1) | 81.8 (63.5-94.2) |
| Free T4 (pg/mL) | 12.4 (12.0-13.6) | 12.4 (11.2-13.8) | 12.9 (12.2-14.5) | 12.3 (11.1-13.6) |
| TSH (mIU/L) | 1.57 (1.16-2.55) | 1.37 (0.78-2.23) | 1.48 (0.67-2.67) | 1.31 (0.80-2.12) |
| Echocardiography | ||||
| EF (%) | 55 (36-63) | 66 (58-72) | 45 (35-59) | 66 (59-72) |
| EDV (mL) | 101 (88-157) | 102 (83-127) | 126 (91-171) | 99 (84-120) |
| ESV (mL) | 43 (31-98) | 35 (27-47) | 58 (35-101) | 34 (27-44) |
| LVEDD (mm) | 46 (44-59) | 47 (43-52) | 53 (47-61) | 46 (43-50) |
| LVESD (mm) | 31 (28-46) | 30 (26-33) | 38 (29-50) | 29 (26-32) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




