Submitted:
26 July 2025
Posted:
30 July 2025
You are already at the latest version
Abstract
Keywords:
Introduction
Methodology
Study Area and Period
Study Design
Study Population and Eligibility
Sample Size Determination and Sampling Technique
Data Collection Methods
Anthropometric Measurements
Data Collection Process
Study Variables
- Dependent Variable: Nutritional status (MNA-SF score: 0–7 = malnourished, 8–11 = at risk, 12–14 = normal) 17,23.
- Independent Variables: Socio-demographic characteristics, health conditions (e.g., chronic illness, recent illness, medication use), functional status, dietary diversity, feeding practices, and food insecurity.
Operational Definitions
- Dietary Diversity: Low (≤3 food groups), medium (4–5), or high (≥6) based on HDDS classification24.
- Feeding Practices: Good (≥3 meals/day), moderate (2 meals/day), or poor (≤1 meal/day)25–27.
- Food Insecurity: Categorized as food secure (0–1), mildly (2–8), moderately (9–16), or severely (17–27) food insecure per HFIAS21.
- Age Grouping: 65–74 = young-old, 75–84 = middle-old, ≥85 = very old28.
Data Quality Assurance
Data Processing and Analysis
Ethical Considerations
Results
Socio-Demographic Characteristics
Co-Morbidities and Health-Related Factors
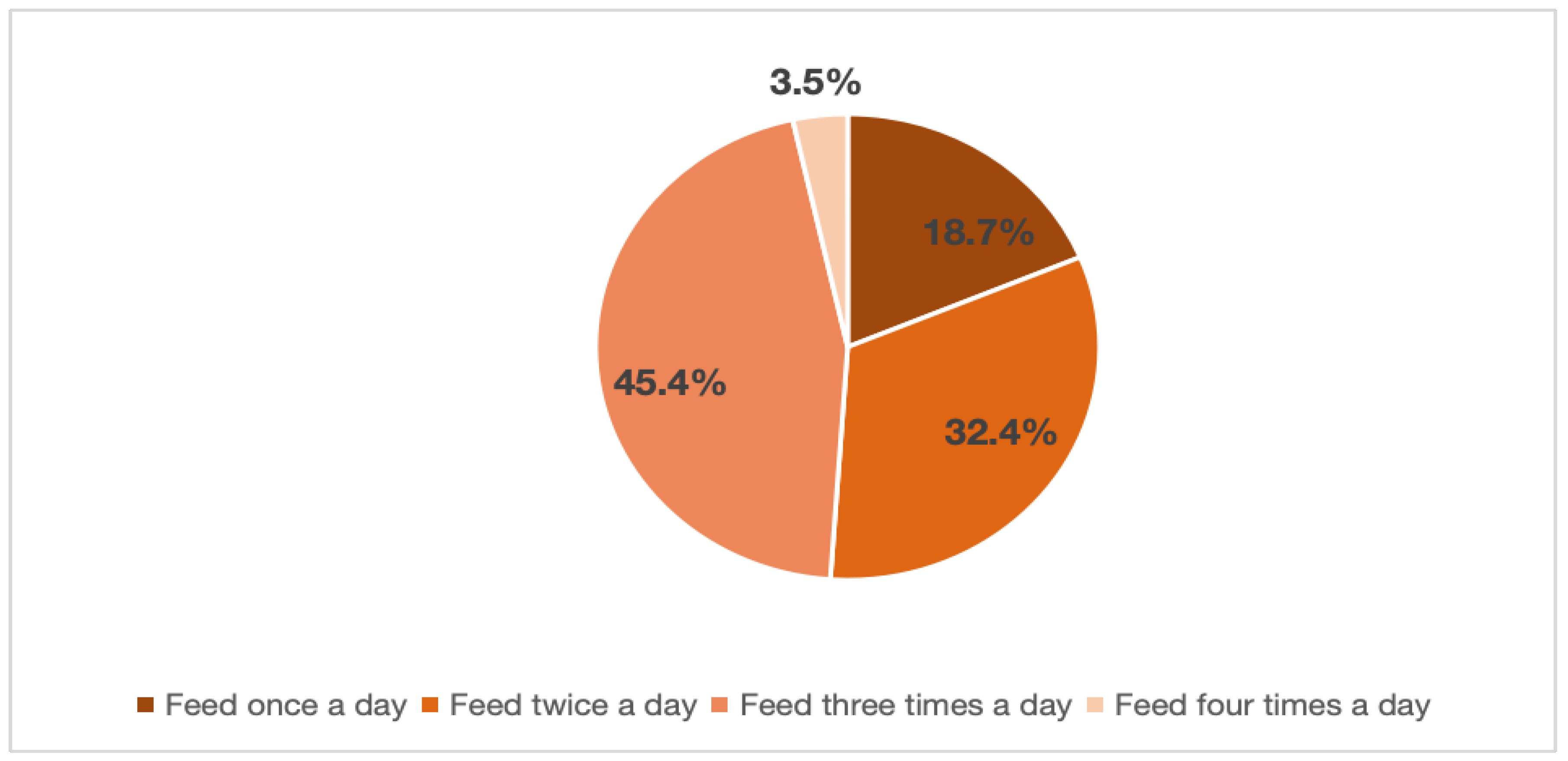
Feeding Practice
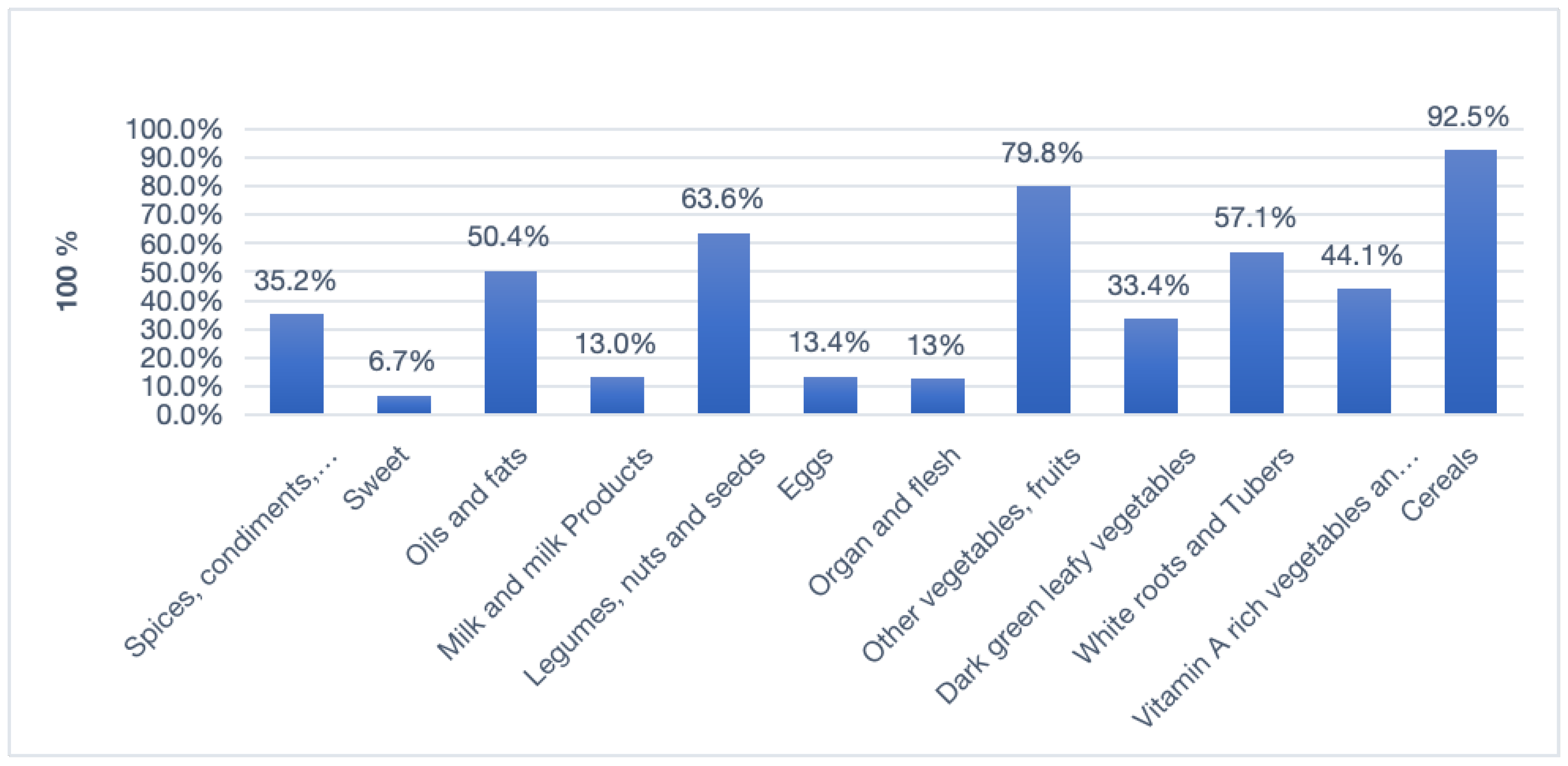
Dietary Diversity Score
Food Security with Household Food Insecurity Access Scale (HFIAS)
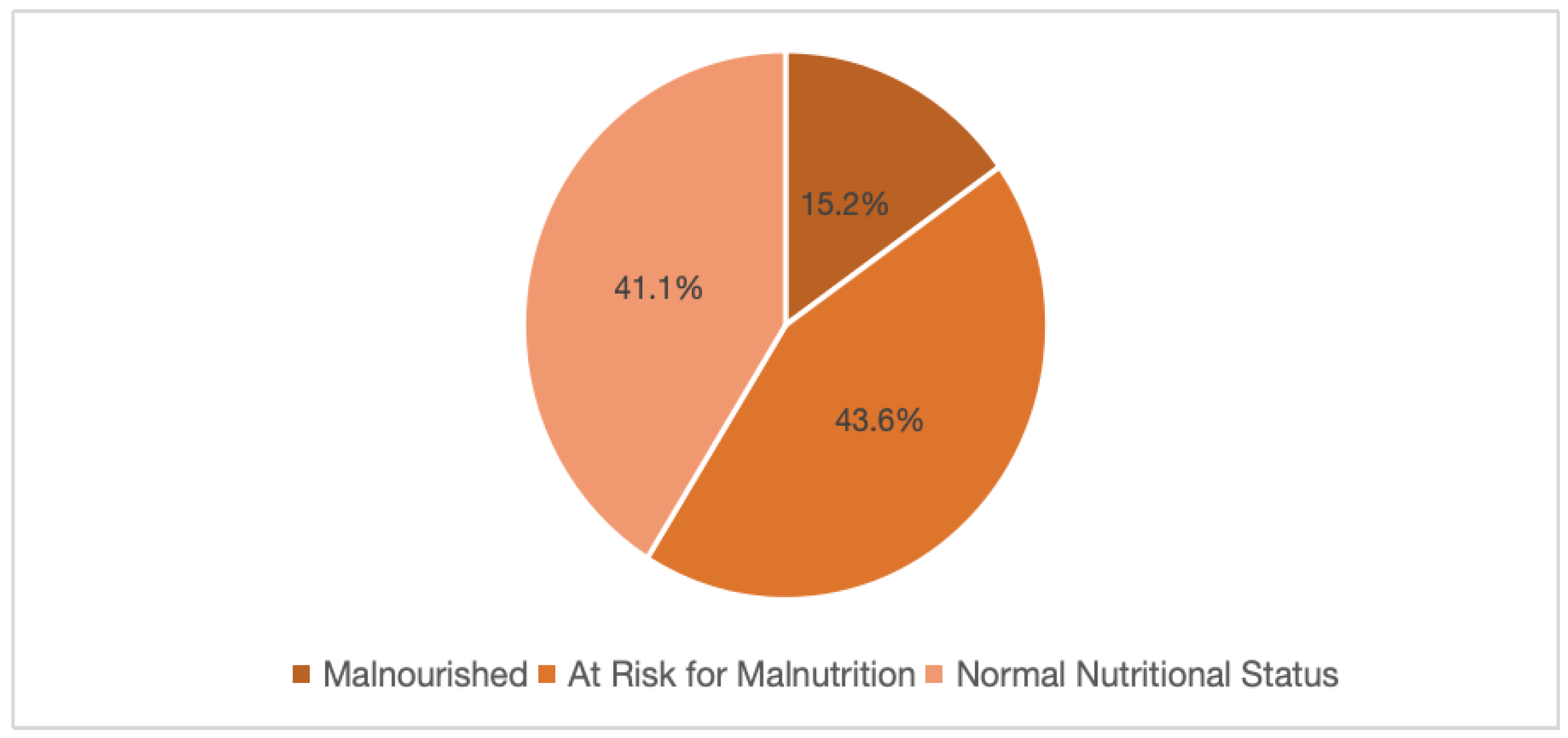
Nutritional Status of Older Adults Above 65 Years
Factors Associated with Nutritional Status
Discussion
Conclusions and Recommendation
Strengths and Limitations of the Study
Author Contributions
Funding
Ethics Approval
Consent to Participate
Data Availability
Acknowledgments
Competing Interests
Abbreviations
| BMI: Body Mass Index |
| CI: Confidence Interval |
| COPD: Chronic Obstructive Pulmonary Disease |
| DDS: Dietary Diversity score |
| DM: Diabetes Mellitus |
| HFIAS: Household Food Insecurity Access Scale |
| IHERC: Institutional Health Ethics Review Committee |
| MNA: Mini Nutritional Assessment |
| MNA-SF: Mini Nutritional Assessment Short-Form |
| NGOs: Non-governmental organizations |
| SPSS: Statistical Package for the Social Sciences |
References
- Ageing and health. https://www.who.int/news-room/fact-sheets/detail/ageing-and-health.
- World Bank Open Data. World Bank Open Data https://data.worldbank.org.
- Skirbekk, V. F., Staudinger, U. M. & Cohen, J. E. How to Measure Population Aging? The Answer Is Less than Obvious: A Review. Gerontology 65, 136–144 (2019). [CrossRef]
- Takele, A. M., Kotecho, M. G. & Adamek, M. E. ‘Hunger would kill us instead of COVID-19 ’: Elders’ response to the pandemic in Debre Markos Town, Ethiopia. Health Soc. Care Community 30, 2250–2258 (2022).
- Li, L. et al. Global patterns of change in the burden of malnutrition in older adults from 1990 to 2021 and the forecast for the next 25 years. Front. Nutr. 12, (2025).
- Salari, N. et al. Global prevalence of malnutrition in older adults: A comprehensive systematic review and meta-analysis. Public Health Pract. 9, 100583 (2025). [CrossRef]
- Kaur, D. et al. Nutritional Interventions for the Elderly and Considerations for the Development of Geriatric Foods. Curr. Aging Sci. 12, 15–27 (2019). [CrossRef]
- Cawood, A. L., Elia, M. & Stratton, R. J. Systematic review and meta-analysis of the effects of high protein oral nutritional supplements. Ageing Res. Rev. 11, 278–296 (2012). [CrossRef]
- Leslie, W. & Hankey, C. Aging, Nutritional Status and Health. Healthcare 3, 648–658 (2015).
- Telila, H. F. & Sima, E. A. Quantifying food insecurity in Ethiopia: Prevalence, drivers, and policy implications. Cogent Soc. Sci. 10, (2024).
- Mezemir, Y., Egata, G., Geset, D. & Lambebo, A. Nutritional Status and Associated Factors Among the Community-Dwelling Elderly Population in Debre Berhan Town, North Shewa Zone, Ethiopia. Nutr. Diet. Suppl. Volume 12, 289–299 (2020). [CrossRef]
- Seid, A. M. & Babbel, N. F. Prevalence of malnutrition among old age people in Africa. Front. Aging 3, (2022). [CrossRef]
- Yisak, H. et al. Determinants of undernutrition among older adults in South Gondar Zone, Ethiopia: a community-based study. BMJ Open 12, e056966 (2022). [CrossRef]
- Abdu, A. O., Yimamu, I. D. & Kahsay, A. A. Predictors of malnutrition among older adults aged above 65 years in eastern Ethiopia: neglected public health concern. BMC Geriatr. 20, (2020).
- Harar Regional Health Bureau | MINISTRY OF HEALTH - Ethiopia. https://www.moh.gov.et/am/node/222.
- Yisak, H. et al. Undernutrition and associated factors among older adults in Ethiopia: systematic review and meta-analysis. BMJ Open 13, e062845 (2023).
- Vellas, B. et al. Overview of the MNA – Its history and challenges. J. Nutr. Health Aging 10, 456–63; discussion 463 (2005).
- Lozoya, R. M., Martínez-Alzamora, N., Marín, G. C., Guirao-Goris, S. J. A. & Ferrer-Diego, R. M. Predictive ability of the Mini Nutritional Assessment Short Form (MNA-SF) in a free-living elderly population: a cross-sectional study. PeerJ 5, e3345 (2017). [CrossRef]
- Harris, D. & Haboubi, N. Malnutrition screening in the elderly population. J. R. Soc. Med. 98, 411–414 (2005).
- Hussein, F. M., Ahmed, A. Y. & Muhammed, O. S. Household food insecurity access scale and dietary diversity score as a proxy indicator of nutritional status among people living with HIV/AIDS, Bahir Dar, Ethiopia, 2017. PLOS ONE 13, e0199511 (2018).
- Coates, J., Swindale, A. & Bilinsky, P. Household Food Insecurity Access Scale (HFIAS) for Measurement of Food Access: Indicator Guide: Version 3: (576842013-001). American Psychological Association (APA) https://doi.org/10.1037/e576842013-001 (2007). [CrossRef]
- McDowell, M. A., Fryar, C. D., Ogden, C. L. & Flegal, K. M. Anthropometric Reference Data for Children and Adults: United States, 2003-2006: (623932009-001). American Psychological Association (APA) https://doi.org/10.1037/e623932009-001 (2008). [CrossRef]
- Liu, H. et al. Nutritional Status According to the Short-Form Mini Nutritional Assessment (MNA-SF) and Clinical Characteristics as Predictors of Length of Stay, Mortality, and Readmissions Among Older Inpatients in China: A National Study. Front. Nutr. 9, (2022).
- Household Dietary Diversity Score (HDDS) | INDDEX Project. https://inddex.nutrition.tufts.edu/data4diets/indicator/household-dietary-diversity-score-hdds.
- Motadi, S. A., Khorommbi, T., Maluleke, L., Mugware, A. & Mushaphi, L. Nutritional status and dietary pattern of the elderly in Thulamela Municipality of Vhembe District. Afr. J. Prim. Health Care Fam. Med. 14, (2022). [CrossRef]
- Ortega, R. M. et al. [Relationship between the number of daily meals and the energy and nutrient intake in the elderly. Effect on various cardiovascular risk factors]. Nutr. Hosp. 13, 186–192 (1998).
- Paoli, A., Tinsley, G., Bianco, A. & Moro, T. The Influence of Meal Frequency and Timing on Health in Humans: The Role of Fasting. Nutrients 11, 719 (2019). [CrossRef]
- Mesele, M. High Prevalence of Undernutrition among Elderly People in Northwest Ethiopia: A Cross Sectional Study. J. Nutr. Health Food Sci. 2, (2014).
- Bursac, Z., Gauss, C. H., Williams, D. K. & Hosmer, D. W. Purposeful selection of variables in logistic regression. Source Code Biol. Med. 3, 17 (2008).
- Gemeda, B. H. et al. Magnitude and Associated Factors of Undernutrition among elderly people in Shashemene District, West Arsi Zone, Oromia Region, South Ethiopia. Preprint at https://doi.org/10.21203/rs.3.rs-3147066/v1 (2023). [CrossRef]
- Wondiye, K., Asseffa, N. A., Gemebo, T. D. & Astawesegn, F. H. Predictors of undernutrition among the elderly in Sodo zuriya district Wolaita zone, Ethiopia. BMC Nutr. 5, (2019).
- Adhana, Z. K., Tessema, G. H. & Getie, G. A. PREVALENCE OF UNDER NUTRITION AND ASSOCIATED FACTORS AMONG PEOPLE OF OLD AGE IN DEBRE MARKOS TOWN, NORTHWEST ETHIOPIA, 2015. J. Aging Res. Lifestyle 1–7 (2019). [CrossRef]
- Hailemariam, H., Singh, P. & Fekadu, T. Evaluation of mini nutrition assessment (MNA) tool among community dwelling elderly in urban community of Hawassa city, Southern Ethiopia. BMC Nutr. 2, (2016). [CrossRef]
- Ferede, Y. M., Derso, T. & Sisay, M. Prevalence of malnutrition and associated factors among older adults from urban and rural residences of Metu district, Southwest Ethiopia. BMC Nutr. 8, (2022). [CrossRef]
- Abate, T., Mengistu, B., Atnafu, A. & Derso, T. Malnutrition and its determinants among older adults people in Addis Ababa, Ethiopia. BMC Geriatr. 20, (2020).
- Shuremu, M., Belachew, T. & Hassen, K. Nutritional status and its associated factors among elderly people in Ilu Aba Bor Zone, Southwest Ethiopia: a community-based cross-sectional study. BMJ Open 13, e067787 (2023). [CrossRef]
- Tesfaye, B. T., Yizengaw, M. A., Birhanu, T. E. & Bosho, D. D. Nutritional status of hospitalized elderly patients in Ethiopia: a cross-sectional study of an important yet neglected problem in clinical practice. Front. Nutr. 10, (2024). [CrossRef]
- Zewdu, E., Daniel, L., Derso, T. & Ferede, Y. M. Level of malnutrition and associated factors among community-dwelling rural older adults in Fogera Zuriya district, Northwest Ethiopia. Nutrition 113, 112085 (2023). [CrossRef]
- Grammatikopoulou, M. G. et al. Food insecurity increases the risk of malnutrition among community-dwelling older adults. Maturitas 119, 8–13 (2019).
- Tari Selcuk, K., Atan, R. M., Arslan, S. & Sahin, N. Relationship between food insecurity and geriatric syndromes in older adults: A multicenter study in Turkey. Exp. Gerontol. 172, 112054 (2023). [CrossRef]
| Characteristics | Categories | Frequency | Percentage (%) |
|---|---|---|---|
| Age | Young old (65 to 74 years of age) | 219 | 54.6% |
| Middle old (75 to 84 years of age) | 116 | 28.9 | |
| Old Old (>85 years of age) | 66 | 16.5 | |
| Educational status | Unable to read and write | 125 | 31.7 |
| Able to read and write | 73 | 18.2 | |
| Primary school (grades 1-8) | 58 | 14.5 | |
| Secondary school (grade 9-12) | 85 | 21.2 | |
| college and above | 60 | 15.0 | |
| Occupation of the respondent | Merchant | 65 | 16.2 |
| Government employee | 71 | 17.7 | |
| Daily laborer | 18 | 4.5 | |
| Housewife | 45 | 11.2 | |
| Farmer | 8 | 2.0 | |
| Retired | 184 | 45.9 | |
| Living condition | With partner | 213 | 53.1 |
| With Children’s | 106 | 26.4 | |
| Lives alone | 63 | 15.7 | |
| Other | 19 | 4.7 | |
| Source of household food | From market | 397 | 99.0 |
| From agriculture | 2 | 0.5 | |
| Household family size? | 0 to 5 people | 326 | 81.3 |
| 6 to 15 people | 71 | 17.7 | |
| Any use of the following substances | Khat | 88 | 21.9 |
| Cigarette | 20 | 5.0 | |
| Alcohol | 37 | 9.2 |
| DDS Cat | |||||||
| Low dietary diversity score | Medium dietary diversity score | High dietary diversity score | |||||
| Count | Column N % | Count | Column N % | Count | Column N % | ||
| Eaten Cereals | No | 7 | 8.3% | 14 | 8.1% | 9 | 6.3% |
| Yes | 77 | 91.7% | 159 | 91.9% | 135 | 93.8% | |
| Vitamin A-rich vegetables and fruits | No | 73 | 86.9% | 94 | 54.3% | 57 | 39.6% |
| Yes | 11 | 13.1% | 79 | 45.7% | 87 | 60.4% | |
| White roots and Tubers | No | 38 | 45.2% | 77 | 44.5% | 57 | 39.6% |
| Yes | 46 | 54.8% | 96 | 55.5% | 87 | 60.4% | |
| Dark green leafy vegetables | No | 78 | 92.9% | 119 | 68.8% | 70 | 48.6% |
| Yes | 6 | 7.1% | 54 | 31.2% | 74 | 51.4% | |
| Other Vegetables and Fruit | No | 31 | 36.9% | 28 | 16.2% | 22 | 15.3% |
| Yes | 53 | 63.1% | 145 | 83.8% | 122 | 84.7% | |
| Organ and flesh | No | 83 | 98.8% | 156 | 90.2% | 112 | 77.8% |
| Yes | 1 | 1.2% | 17 | 9.8% | 32 | 22.2% | |
| Eaten Eggs | No | 83 | 98.8% | 157 | 90.8% | 107 | 74.3% |
| Yes | 1 | 1.2% | 16 | 9.2% | 37 | 25.7% | |
| legumes, nuts, and seeds? | No | 34 | 40.5% | 69 | 39.9% | 40 | 27.8% |
| Yes | 50 | 59.5% | 104 | 60.1% | 104 | 72.2% | |
| Milk and milk Products | No | 83 | 98.8% | 161 | 93.1% | 105 | 72.9% |
| Yes | 1 | 1.2% | 12 | 6.9% | 39 | 27.1% | |
| Oils and fats | No | 81 | 96.4% | 104 | 60.1% | 14 | 9.7% |
| Yes | 3 | 3.6% | 69 | 39.9% | 130 | 90.3% | |
| Eaten Sweet | No | 81 | 96.4% | 169 | 97.7% | 124 | 86.1% |
| Yes | 3 | 3.6% | 4 | 2.3% | 20 | 13.9% | |
| Spices, condiments, beverages | No | 84 | 100.0% | 134 | 77.5% | 42 | 29.2% |
| Yes | 0 | 0.0% | 39 | 22.5% | 102 | 70.8% | |
| HFIAS | No | Yes |
Rarely Once or twice in the past four weeks |
Sometimes Three to ten times in the past four weeks |
Often More than ten times in the past four weeks |
| 1. Worry about food | 35.2% 141 |
64.8% 260 |
|||
| 1a. how often | 28.7% 115 |
29.7% 119 |
6.7% 27 |
||
| 2. Not able to eat | 40.6% 163 |
59.4% 238 |
|||
| 2a. How often | 28.2% 113 |
19.0% 76 |
12.2% 49 |
||
| 3. Eat limited variety. | 38.7% 155 |
61.3% 246 |
|||
| 3a. How often | 21.7% 87 |
27.4% 110 |
12.5% 50 |
||
| 4. Have you eaten foods you really didn’t want? | 37.4% 150 |
62.6% 251 |
|||
| 4a. How often | 29.4% 118 |
26.2% 105 |
6.7% 27 |
||
| 5. Eaten smaller meal | 45.6% 183 |
54.4% 218 |
|||
| 5a. How often | 21.9% 88 |
18.7% 75 |
2.5% 10 |
||
| 6. Eaten Fewer meals | 50.9% 204 |
48.9% 196 |
|||
| 6a. How often | 26.4% 106 |
18.7% 75 |
2.5% 10 |
||
| 7. No food of any kind | 66.6% 267 |
33.4% 134 |
|||
| 7a. How often | 15.2% 61 |
14.0% 56 |
2.0% 8 |
||
| 8. Slept hungry | 82.3% 330 |
17.7% 71 |
|||
| 8a. How often | 9.2% 37 |
5.5% 22 |
2.2% 9 |
||
| 9. Whole day and night without food | 98.0% 394 |
2.0% 8 |
|||
| 9a. How often | 2.0% 8 |
0.0% 0 |
0% 0 |
| Variable and Categories |
Nutritional status | Crude odds ratio With CI |
Adjusted Odds Ratio |
P-value | |
|---|---|---|---|---|---|
| Malnourished or at risk | Normal nutritional status | ||||
| Age | |||||
| 65-74 | 96 (23.9%) | 123 (30.7%) | 1 | 1 | 1 |
| 75-84 | 64 (16.0%) | 52 (13.0%) | 1.57(1.00-2.48) | 2.58(1.26-5.31) | 0.010* |
| 85-95 | 43 (10.7%) | 23 (5.7) | 2.39 (1.35-4.24) | 2.90(1.20-6.99) | 0.017* |
| Marital status | |||||
| Single | 28 (7.0%) | 16 (4.0%) | 1 | 1 | 1 |
| Married | 68 (17.0%) | 135 (33.7%) | 0.28 (0.14-0.56) | 0.19(0.07-0.52) | 0.001* |
| Divorced | 25 (6.2%) | 27 (6.7%) | 0.52 (0.23-1.20) | 0.30(0.09-1.01) | 0.06 |
| Widowed | 82 (20.4%) | 20 (5.0%) | 2.34 (1.06-5.13) | 1.83(0.63-5.34) | 0.20 |
| Educational status | |||||
| Unable to read and write | 66 (16.5%) | 59 (14.7%) | 3.67 (1.57-6.02) | 1.51(0.57-4.02) | 0.40 |
| Able to read and write | 55 (13.7%) | 18 (4.5%) | 8.40 (3.8-18.4) | 4.17(1.43-12.1) | 0.01* |
| Primary education | 27 (6.7%) | 31 (7.7%) | 2.39 (1.1-5.2) | 1.06(0.35-3.12) | 0.91 |
| Secondary education | 39 (9.7%) | 46 (11.5%) | 2.33 (1.1-4.76) | 2.28(0.82-6.34) | 0.11 |
| College and above | 16 (4.0%) | 44 (11.0%) | 1 | 1 | 1 |
| Substance use | |||||
| Yes | 105 (26.3%) | 37 (9.3%) | 0.21 (0.13-0.33) | 0.18 (0.09-0.34) | <0.001* |
| No | 98 (24.5%) | 160 (40.0%) | 1 | 1 | 1 |
| illness in the past 3 month | |||||
| Yes | 127 (31.7%) | 62 (15.5%) | 3.66 (2.42-5.54) | 2.77 (1.49-5.14) | 0.001* |
| No | 76 (19.0%) | 136 (33.9%) | 1 | 1 | 1 |
| History of chronic illness | |||||
| Yes | 111 (27.7%) | 64 (16.0%) | 2.52 (1.68-3.79) | 0.59 (0.32-1.06) | 0.07 |
| No | 92 (22.9%) | 134 (33.4%) | 1 | 1 | 1 |
| Illness in the past 2 weeks | |||||
| Yes | 97 (24.2%) | 62 (15.5%) | 2.00 (1.33-3.01) | 0.56 (0.30-1.04) | 0.06 |
| No | 106 (26.4%) | 136 (33.9%) | 1 | 1 | 1 |
| Ability to feed by him/herself | |||||
| By oneself | 163 (40.6%) | 189 (47.1%) | 1 | 1 | 1 |
| Help from others | 40 (10.0%) | 9 (2.2%) | 4.54 (1.94-10.6) | 1.77 (0.63-4.99) | 0.27 |
| With whom are you feeding | |||||
| Always alone | 56 (14.0%) | 34 (8.5%) | 1 | 1 | 1 |
| Sometimes alone | 78 (19.5%) | 65 (16.2%) | 0.72 (0.42-1.24) | 2.25 (0.97-5.20) | 0.06 |
| Always with family | 42 (10.5%) | 74 (18.5%) | 0.34 (0.19-0.61) | 1.43 (0.55-3.72) | 0.45 |
| Time to have a meal | |||||
| Regular | 122 (30.4%) | 161 (40.1%) | 1 | 1 | 1 |
| Irregular | 81 (20.2%) | 35 (9.2%) | 2.88 (1.83-4.55) | 1.75 (0.85-3.61) | 0.12 |
| Feeding habit | |||||
| Poor feeding habits | 60 (15.0%) | 15 (3.7%) | 7.9 (4.19-15.03) | 4.77 (1.79-12.46) | 0.001* |
| Moderate feeding habit | 77 (19.2%) | 52 (13.0%) | 2.93 (1.85-4.65) | 2.83 (1.44-5.56) | 0.003* |
| Good feeding habit | 66 (16.5%) | 131 (32.7%) | 1 | 1 | 1 |
| Dietary diversity | |||||
| Low DDS | 58 (14.5%) | 26 (6.5%) | 5.24 (2.29-9.39) | 4.0 (1.82-12.46) | 0.002* |
| Medium DDS | 102 (25.4%) | 71 (17.7%) | 3.37 (2.11-5.38) | 2.83 (1.44-5.56) | 0.002* |
| High DDS | 43 (10.7%) | 101 (25.2%) | 1 | 1 | 1 |
| HFIAS | |||||
| Food secured | 32 (8.0%) | 98 (24.4%) | 1 | 1 | 1 |
| Mild food insecurity | 63 (15.7%) | 48 (12.0%) | 4.02 (2.32-6.95) | 2.82(1.29-6.17) | 0.009* |
| Moderate food insecurity | 73 (18.2%) | 42 (10.5%) | 5.32 (3.06-9.23) | 5.57(2.45-12.6) | <0.001* |
| Food insecure | 35 (8.7%) | 10 (2.7%) | 10.7 (4.77-24.1) | 6.33(2.07-19.3) | 0.001* |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




