Submitted:
02 October 2024
Posted:
03 October 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
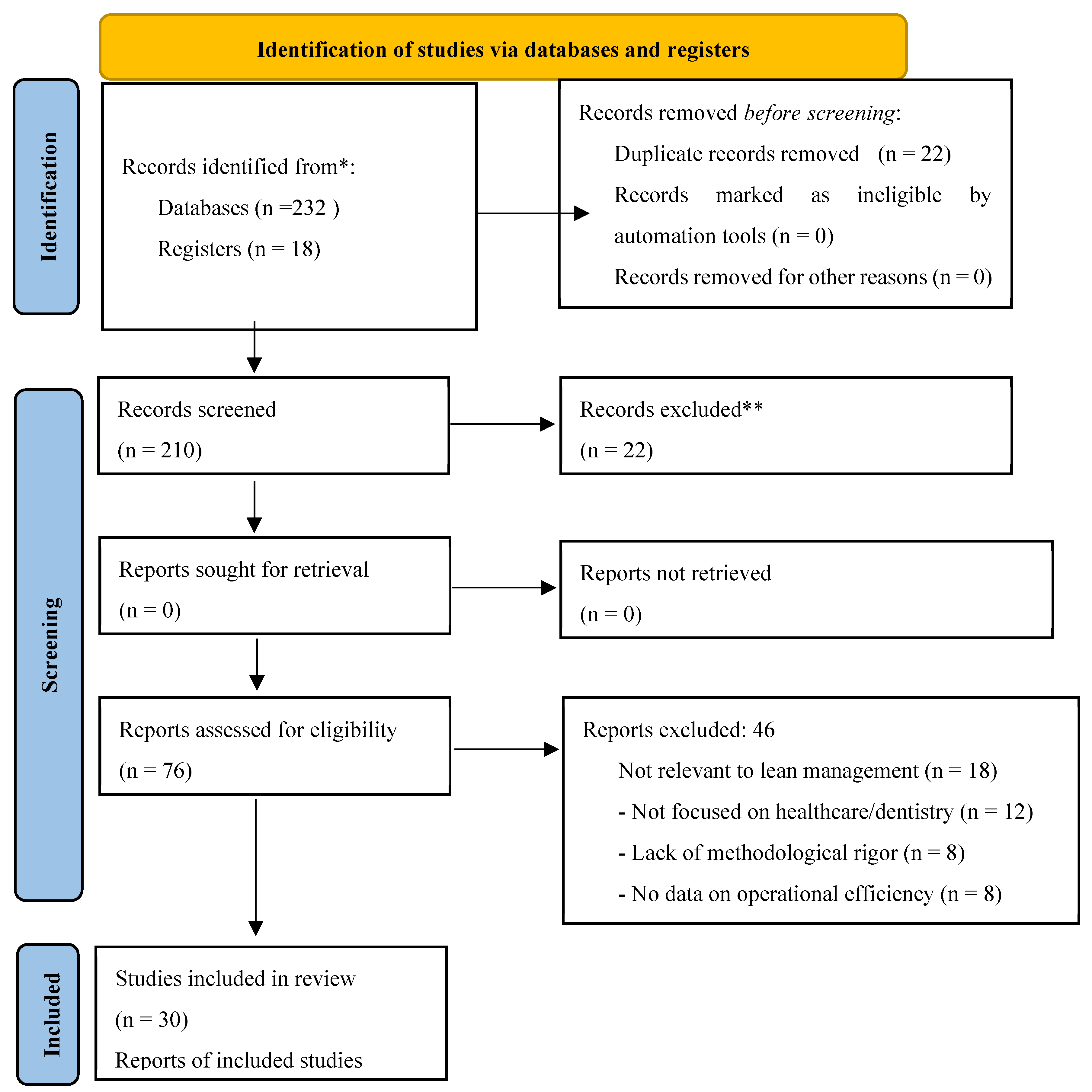
2. Materials and Methods
3. Results
Percentage of Different Issues Explored in the Articles
General Applications of Lean in Healthcare and Transferability to Dentistry
Lean Applications in Dentistry
Lean Tools, Application, Outcomes, and Impact on Patient Satisfaction in Dentistry
Lean Tools, Circular Economy Principles and Outcomes in Dentistry
Supply Chain and Waste Management
Types of Waste and Lean Tools
Sustainability of Lean Practices in Dentistry
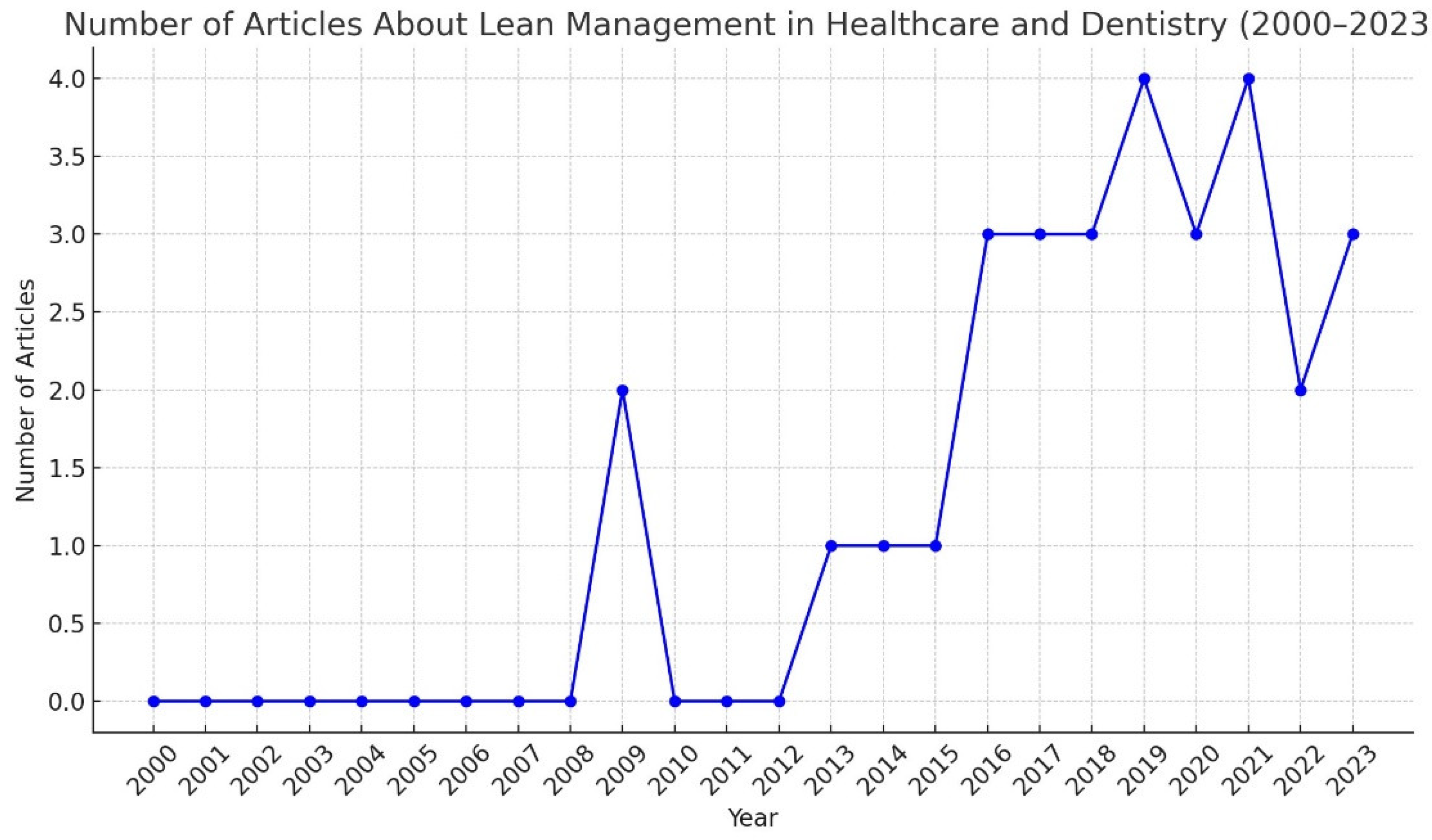
Increasing Interest Over Time for the Research Theme
Educational Activities Suggested for Lean Management in Healthcare and Dentistry
4. Discussion
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Abubakar, I.R.; Maniruzzaman, K.M.; Dano, U.L.; AlShihri, F.S.; AlShammari, M.S.; Ahmed, S.M.S.; Al-Gehlani, W.A.G.; Alrawaf, T.I. Environmental Sustainability Impacts of Solid Waste Management Practices in the Global South. Int. J. Environ. Res. Public Heal. 2022, 19, 12717. [Google Scholar] [CrossRef]
- Antoniadou, M.; Varzakas, T.; Tzoutzas, I. Circular Economy in Conjunction with Treatment Methodologies in the Biomedical and Dental Waste Sectors. Circ. Econ. Sustain. 2021, 1, 563–592. [Google Scholar] [CrossRef]
- Debrah, J.K.; Teye, G.K.; Dinis, M.A.P. Barriers and Challenges to Waste Management Hindering the Circular Economy in Sub-Saharan Africa. Urban Sci. 2022, 6, 57. [Google Scholar] [CrossRef]
- Hariram, N.P.; Mekha, K.B.; Suganthan, V.; Sudhakar, K. Sustainalism: An Integrated Socio-Economic-Environmental Model to Address Sustainable Development and Sustainability. Sustainability 2023, 15, 10682. [Google Scholar] [CrossRef]
- Upadhayay, S.; Alqassimi, O.; Khashadourian, E.; Sherm, A.; Prajapati, D. Development in the Circular Economy Concept: Systematic Review in Context of an Umbrella Framework. Sustainability 2024, 16, 1500. [Google Scholar] [CrossRef]
- Vogiantzi, C.; Tserpes, K. On the Definition, Assessment, and Enhancement of Circular Economy across Various Industrial Sectors: A Literature Review and Recent Findings. Sustainability 2023, 15, 16532. [Google Scholar] [CrossRef]
- Bharsakade, R.S.; Acharya, P.; Ganapathy, L.; Tiwari, M.K. A lean approach to healthcare management using multi criteria decision making. OPSEARCH 2021, 58, 610–635. [Google Scholar] [CrossRef]
- Khurshid, Z. Digital Dentistry: Transformation of Oral Health and Dental Education with Technology. Eur. J. Dent. 2023, 17, 943–944. [Google Scholar] [CrossRef]
- Kirchherr, J.; Yang, N.-H.N.; Schulze-Spüntrup, F.; Heerink, M.J.; Hartley, K. Conceptualizing the Circular Economy (Revisited): An Analysis of 221 Definitions. Resour. Conserv. Recycl. 2023, 194. [Google Scholar] [CrossRef]
- Martin, N.; Sheppard, M.; Gorasia, G.; Arora, P.; Cooper, M.; Mulligan, S. Drivers, opportunities and best practice for sustainability in dentistry: A scoping review. J. Dent. 2021, 112, 103737. [Google Scholar] [CrossRef]
- Kenny, C.; Priyadarshini, A. Review of Current Healthcare Waste Management Methods and Their Effect on Global Health. Healthcare 2021, 9, 284. [Google Scholar] [CrossRef]
- Olawade, D.B.; Fapohunda, O.; Wada, O.Z.; Usman, S.O.; Ige, A.O.; Ajisafe, O.; Oladapo, B.I. Smart waste management: A paradigm shift enabled by artificial intelligence. Waste Manag. Bull. 2024, 2, 244–263. [Google Scholar] [CrossRef]
- Iranmanesh, M.; Zailani, S.; Hyun, S.S.; Ali, M.H.; Kim, K. Impact of Lean Manufacturing Practices on Firms’ Sustainable Performance: Lean Culture as a Moderator. Sustainability 2019, 11, 1112. [Google Scholar] [CrossRef]
- Salman, S.; Morshed, S.M.; Karim, R.; Rahman, R.; Hasanat, S.; Ahsan, A. Exploring lean manufacturing drivers for enhancing circular economy performance in the pharmaceutical industry: a Bayesian best–worst approach. Int. J. Ind. Eng. Oper. Manag. [CrossRef]
- Romanos, G.E.; Gupta, S. Applied lean principles in dental practice. 53. [CrossRef]
- Mahmoud, Z.; Angelé-Halgand, N.; Churruca, K.; Ellis, L.A.; Braithwaite, J. The impact of lean management on frontline healthcare professionals: a scoping review of the literature. BMC Heal. Serv. Res. 2021, 21, 1–11. [Google Scholar] [CrossRef]
- Mitsika, I.; Chanioti, M.; Antoniadou, M. Dental Solid Waste Analysis: A Scoping Review and Research Model Proposal. Appl. Sci. 2024, 14, 2026. [Google Scholar] [CrossRef]
- EPA. National Service Center for Environmental Publications (NSCEP). https://nepis.epa.gov/EPA/html/pubs/pubtitleOW.
- Covernment of Canada. Canadian Biosafety Handbook, Second Edition Chapter 11-15. https://www.canada.ca/en/public-health/services/canadian-biosafety-standards-guidelines/handbook-second-edition/chapter-11-15.
- European Commision. Circular economy Action Plan. https://environment.ec.europa.eu/strategy/circular-economy-action-plan_en#:~:text=The%20new%20action%20plan%20announces,for%20as%20long%20as%20possible.
- European Commision. Waste framework Directive (2008/98/EC). https://environment.ec.europa.
- European Parliament. Circular economy: definition, importance and benefits. Topics. https://www.europarl.europa. 2015.
- Dental waste management Innovative Solutions for Dental Waste Management: A Guide for Entrepreneurs. Updated: 20 Jun 2024. https://fastercapital.com/content/Dental-waste-management-Innovative-Solutions-for-Dental-Waste-Management--A-Guide-for-Entrepreneurs.
- Hayashi, M.; Haapasalo, M.; Imazato, S.; Lee, J.I.; Momoi, Y.; Murakami, S.; Whelton, H.; Wilson, N. Dentistry in the 21st century: challenges of a globalising world. Int. Dent. J. 2014, 64, 333–342. [Google Scholar] [CrossRef]
- Allan, J.; Belz, S.; Hoeveler, A.; Hugas, M.; Okuda, H.; Patri, A.; Rauscher, H.; Silva, P.; Slikker, W.; Sokull-Kluettgen, B.; et al. Regulatory landscape of nanotechnology and nanoplastics from a global perspective. Regul. Toxicol. Pharmacol. 2021, 122, 104885. [Google Scholar] [CrossRef]
- Concari, A.; Kok, G.; Martens, P. A Systematic Literature Review of Concepts and Factors Related to Pro-Environmental Consumer Behaviour in Relation to Waste Management Through an Interdisciplinary Approach. Sustainability 2020, 12, 4452. [Google Scholar] [CrossRef]
- Khanna, R.; Konyukhov, Y.; Maslennikov, N.; Kolesnikov, E.; Burmistrov, I. An Overview of Dental Solid Waste Management and Associated Environmental Impacts: A Materials Perspective. Sustainability 2023, 15, 15953. [Google Scholar] [CrossRef]
- Yogesh, M.J.; Karthikeyan, J. Health Informatics: Engaging Modern Healthcare Units: A Brief Overview. Front. Public Heal. 2022, 10, 854688. [Google Scholar] [CrossRef]
- Roopa, M.; Siriram, R.; Coetzee, R. Exploring Industrial Engineering Knowledge and Environmental Sustainability. Sustainability 2024, 16, 7392. [Google Scholar] [CrossRef]
- Taelman, S.E.; Tonini, D.; Wandl, A.; Dewulf, J. A Holistic Sustainability Framework for Waste Management in European Cities: Concept Development. Sustainability 2018, 10, 2184. [Google Scholar] [CrossRef]
- Thakar, S.; Kinariwala, N.; Pandya, D.; Parekh, N.H.; Patel, N.K.; Patel, A. Awareness and Constraints towards the Implementation of Green Dentistry amongst Dental Students and Private Practitioners of West India. J. Pharm. Bioallied Sci. 2023, 15, S1287–S1290. [Google Scholar] [CrossRef]
- Antoniadou, M.; Chrysochoou, G.; Tzanetopoulos, R.; Riza, E. Green Dental Environmentalism among Students and Dentists in Greece. Sustainability 2023, 15, 9508. [Google Scholar] [CrossRef]
- Munn, Z.; Peters, M.D.J.; Stern, C.; Tufanaru, C.; McArthur, A.; Aromataris, E. Systematic Review or Scoping Review? Guidance for Authors When Choosing between a Systematic or Scoping Review Approach. BMC Med. Res. Methodol. 2018, 18, 143. [Google Scholar] [CrossRef]
- Womack, J. P. , & Jones, D. T. (1996). Lean Thinking: Banish Waste and Create Wealth in Your Corporation. Simon & Schuster.
- Kolaski, K.; Logan, L.R.; Ioannidis, J.P.A. Guidance to best tools and practices for systematic reviews. Syst. Rev. 2023, 12, 1–29. [Google Scholar] [CrossRef]
- Tierney, A.A.B.; Shortell, S.M.P.; Rundall, T.G.; Blodgett, J.C.M.; Reponen, E. Examining the Relationship Between the Lean Management System and Quality Improvement Care Management Processes. Qual. Manag. Heal. Care 2021, 31, 1–6. [Google Scholar] [CrossRef]
- Bektas, G.; Kiper, F. Applications of lean in human resources management in healthcare. J. Pak. Med Assoc. 2021, 72, 532–536. [Google Scholar] [CrossRef]
- van Rossum, L.; Aij, K.H.; Simons, F.E.; van der Eng, N.; Have, W.D.T. Lean healthcare from a change management perspective. J. Heal. Organ. Manag. 2016, 30, 475–493. [Google Scholar] [CrossRef]
- Sloan, T.; Fitzgerald, A.; Hayes, K.J.; Radnor, Z.; Sohal, S.R.A.A. Lean in healthcare – history and recent developments. J. Heal. Organ. Manag. 2014, 28, 130–4. [Google Scholar] [CrossRef]
- Bowe, C.; Gurney, B.; Sloane, J.; Newlands, C. Process mapping and Lean principles applied to orthognathic surgery. Br. J. Oral Maxillofac. Surg. 2020, 59, 157–162. [Google Scholar] [CrossRef]
- Borges, G.A.; Tortorella, G.; Rossini, M.; Portioli-Staudacher, A. Lean implementation in healthcare supply chain: a scoping review. J. Heal. Organ. Manag. 2019, 33, 304–322. [Google Scholar] [CrossRef]
- Crema, M.; Verbano, C. Lean Management to support Choosing Wisely in healthcare: the first evidence from a systematic literature review. Int. J. Qual. Heal. Care 2017, 29, 889–895. [Google Scholar] [CrossRef]
- Burgess, N.; Radnor, Z. Evaluating Lean in healthcare. Int. J. Heal. Care Qual. Assur. 2013, 26, 220–235. [Google Scholar] [CrossRef]
- Prado-Prado, J.C.; García-Arca, J.; Fernández-González, A.J.; Mosteiro-Añón, M. Increasing Competitiveness through the Implementation of Lean Management in Healthcare. Int. J. Environ. Res. Public Heal. 2020, 17, 4981. [Google Scholar] [CrossRef]
- Nazarali, S.; Rayat, J.; Salmonson, H.; Moss, T.; Mathura, P.; Damji, K.F. The application of a “6S Lean” initiative to improve workflow for emergency eye examination rooms. Can. J. Ophthalmol. 2017, 52, 435–440. [Google Scholar] [CrossRef]
- de Barros, L.B.; Bassi, L.d.C.; Caldas, L.P.; Sarantopoulos, A.; Zeferino, E.B.B.; Minatogawa, V.; Gasparino, R.C. Lean Healthcare Tools for Processes Evaluation: An Integrative Review. Int. J. Environ. Res. Public Heal. 2021, 18, 7389. [Google Scholar] [CrossRef]
- Flynn, R.; Newton, A.S.; Rotter, T.; Hartfield, D.; Walton, S.; Fiander, M.; Scott, S.D. The sustainability of Lean in pediatric healthcare: a realist review. Syst. Rev. 2018, 7, 1–17. [Google Scholar] [CrossRef]
- Morales-Contreras, M.F.; Chana-Valero, P.; Suárez-Barraza, M.F.; Díaz, A.S.; García, E.G. Applying Lean in Process Innovation in Healthcare: The Case of Hip Fracture. Int. J. Environ. Res. Public Heal. 2020, 17, 5273. [Google Scholar] [CrossRef]
- de Freitas, P.S.; de Mendonça, G.S.; Resende, E.S. Implementation of the Lean Healthcare System in the Emergency Room of the Clinical Hospital of the Federal University of Uberlândia: A Case Study. Int. J. Environ. Res. Public Heal. 2023, 20, 7184. [Google Scholar] [CrossRef]
- Milstein, B. , and J. Homer. 2006. Background on system dynamics simulation modeling with a summary of major public health studies. Atlanta, GA: CDC. http://www.caldiabetes.org/get_file.cfm?contentID=501&ContentFilesID=389 (accessed , 2024). 3 September.
- Robinson, F.G.; Fischbach, H.; Salisbury, J.; Stefanik, D.; Kearney, R.; Fields, H.W. Clinical Integration in a Dental School Clinic Through an Enhanced Patient Intake Process. J. Dent. Educ. 2019, 83, 1030–1038. [Google Scholar] [CrossRef]
- Robinson FG, Cunningham LL, Turner SP, Lindroth J, Ray D, Khan T, Yates A. Improving a Dental School’s Clinic Operations Using Lean Process Improvement. J Dent Educ. 2016, 80(10), 1170-1179. 2769.
- Isfahani, H.M.; Tourani, S.; Seyedin, H. Lean management approach in hospitals: a systematic review. Int. J. Lean Six Sigma 2019, 10, 161–188. [Google Scholar] [CrossRef]
- Radnor, Z. Implementing Lean in Health Care: Making the Link Between the Approach, Readiness and Sustainability. Vol12 - Issue 1 2011, 2, 1–12. [Google Scholar] [CrossRef]
- Mistri, I.U.; Badge, A.; Shahu, S. Enhancing Patient Safety Culture in Hospitals. Cureus 2023, 15, e51159. [Google Scholar] [CrossRef]
- Shortell, S.; Blodgett, J.; Rundall, T.; Henke, RM.; Reponen, E. Lean Management and Hospital Performance: Adoption vs. Implementation. The Joint Commission Journal on Quality and Patient Safety 2021; 000:1–10. https://clear.berkeley.edu/sites/default/files/lean_management_and_hp.
- Isfahani, H.M.; Tourani, S.; Seyedin, H. Features and Results of Conducted Studies Using a Lean Management Approach in Emergency Department in Hospital: A Systematic Review. Bull. Emerg. Trauma 2019, 7, 9–20. [Google Scholar] [CrossRef]
- Wannemuehler, T.J.; Elghouche, A.N.; Kokoska, M.S.; Ba, C.R.D.; Matt, B.H. Impact of Lean on surgical instrument reduction: Less is more. Laryngoscope 2015, 125, 2810–2815. [Google Scholar] [CrossRef]
- Karstoft, J.; Tarp, L. Is Lean Management implementable in a department of radiology? Insights into Imaging 2011, 2, 267–273. [Google Scholar] [CrossRef]
- Montesarchio, V.; Grimaldi, A.M.; A Fox, B.; Rea, A.; Marincola, F.M.; A Ascierto, P. Lean oncology: a new model for oncologists. J. Transl. Med. 2012, 10, 74–74. [Google Scholar] [CrossRef]
- Tay, HL. Adapting Lean for process redesign in senior day care services. Journal of hospital management and health policy, 2022, 6. https://jhmhp.amegroups. 6817. [Google Scholar]
- Hayward, L.M. How applicable is lean in mental health? International Journal of Clinical Leadership 2010, 17(3), 165–173. [Google Scholar]
- Boom-Cárcamo, E.; Peñabaena-Niebles, R. Analysis of the Development of Industrial Symbiosis in Emerging and Frontier Market Countries: Barriers and Drivers. Sustainability 2022, 14, 4223. [Google Scholar] [CrossRef]
- Salik I, Ashurst JV. Closed Loop Communication Training in Medical Simulation. [Updated 2023 Jan 23]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih. 5498.
- Nazir, A.; Gokcekaya, O.; Billah, K.M.M.; Ertugrul, O.; Jiang, J.; Sun, J.; Hussain, S. Multi-material additive manufacturing: A systematic review of design, properties, applications, challenges, and 3D printing of materials and cellular metamaterials. Mater. Des. 2023, 226. [Google Scholar] [CrossRef]
- Blum, I.R.; Özcan, M. Reparative Dentistry: Possibilities and Limitations. Curr. Oral Heal. Rep. 2018, 5, 264–269. [Google Scholar] [CrossRef]
- Petre, A.E.; Pantea, M.; Drafta, S.; Imre, M.; Țâncu, A.M.C.; Liciu, E.M.; Didilescu, A.C.; Pițuru, S.M. Modular Digital and 3D-Printed Dental Models with Applicability in Dental Education. Medicina 2023, 59, 116. [Google Scholar] [CrossRef]
- Benedettini, O. Green Servitization in the Single-Use Medical Device Industry: How Device OEMs Create Supply Chain Circularity through Reprocessing. Sustainability 2022, 14, 12670. [Google Scholar] [CrossRef]
- Fontana, A.; Barni, A.; Leone, D.; Spirito, M.; Tringale, A.; Ferraris, M.; Reis, J.; Goncalves, G. Circular Economy Strategies for Equipment Lifetime Extension: A Systematic Review. Sustainability 2021, 13, 1117. [Google Scholar] [CrossRef]
- Alkhoraif, A.; Rashid, H.; McLaughlin, P. Lean implementation in small and medium enterprises: Literature review. Oper. Res. Perspect. 2018, 6, 100089. [Google Scholar] [CrossRef]
- Gnepp, J.; Klayman, J.; Williamson, I.O.; Barlas, S. The future of feedback: Motivating performance improvement through future-focused feedback. PLOS ONE 2020, 15, e0234444. [Google Scholar] [CrossRef]
- Shujaat, S.; Bornstein, M.M.; Price, J.B.; Jacobs, R. Integration of imaging modalities in digital dental workflows - possibilities, limitations, and potential future developments. Dentomaxillofacial Radiol. 2021, 50. [Google Scholar] [CrossRef]
- Al-Balushi, S.; Sohal, A.; Singh, P.; Al Hajri, A.; Al Farsi, Y.; Al Abri, R. Readiness factors for lean implementation in healthcare settings – a literature review. J. Heal. Organ. Manag. 2014, 28, 135–153. [Google Scholar] [CrossRef]
- Schultz SR, Ruter RL, Tibor LC. Lean Management Systems in Radiology: Elements for Success. Radiol Manage. 2016, 38(2), 23-30; quiz 32. 2717.
- Magalhães, A.L.P.; Erdmann, A.L.; da Silva, E.L.; dos Santos, J.L.G. Lean thinking in health and nursing: an integrative literature review. Rev. Latino-Americana de Enferm. 2016, 24, e2734. [Google Scholar] [CrossRef]
- Mazzocato, P.; Savage, C.; Brommels, M.; Aronsson, H.; Thor, J. Lean thinking in healthcare: a realist review of the literature. BMJ Qual. Saf. 2010, 19, 376–382. [Google Scholar] [CrossRef]
- Rees, G.H.; Gauld, R. Can lean contribute to work intensification in healthcare? J. Heal. Organ. Manag. 2017, 31, 369–384. [Google Scholar] [CrossRef]
- Drotz, E.; Poksinska, B. Lean in healthcare from employees’ perspectives. J. Heal. Organ. Manag. 2014, 28, 177–195. [Google Scholar] [CrossRef]
- The Importance of Adopting a Lean Mindset and Culture for Health Care Organizations. Trends in Medicine. 2020. Harvard medical review. https://postgraduateeducation.hms.harvard. 13 November.
- Safavi, S.; Tabibi, S.; Riahi, L.; Farahani, M. Factors Affecting Lean Management: Designing a Model for Teaching Hospitals. J. Intercult. Ethnopharmacol. 2021, 12, 74–81. [Google Scholar] [CrossRef]
- Hihnala, S.; Kettunen, L.; Suhonen, M.; Tiirinki, H. The Finnish healthcare services lean management. Leadersh. Heal. Serv. 2017, 31, 17–32. [Google Scholar] [CrossRef]
- Abuzied, Y. A Practical Guide to the Kaizen Approach as a Quality Improvement Tool. Glob. J. Qual. Saf. Heal. 2022, 5, 79–81. [Google Scholar] [CrossRef]
- Babiker, A.; El Husseini, M.; Al Nemri, A.; Al Frayh, A.; Al Juryyan, N.; O Faki, M.; Assiri, A.; Al Saadi, M.; Shaikh, F.; Al Zamil, F. Health care professional development: Working as a team to improve patient care. . 2014, 14, 9–16. [Google Scholar]
- Buljac-Samardzic, M.; Doekhie, K.D.; van Wijngaarden, J.D.H. Interventions to improve team effectiveness within health care: a systematic review of the past decade. Hum. Resour. Heal. 2020, 18, 1–42. [Google Scholar] [CrossRef]
- Lawal, A.K.; Rotter, T.; Kinsman, L.; Sari, N.; Harrison, L.; Jeffery, C.; Kutz, M.; Khan, M.F.; Flynn, R. Lean management in health care: definition, concepts, methodology and effects reported (systematic review protocol). Syst. Rev. 2014, 3, 103–103. [Google Scholar] [CrossRef]
- Morell-Santandreu, O.; Santandreu-Mascarell, C.; Garcia-Sabater, J.J. A Model for the Implementation of Lean Improvements in Healthcare Environments as Applied in a Primary Care Center. Int. J. Environ. Res. Public Heal. 2021, 18, 2876. [Google Scholar] [CrossRef]
- Nowak, M.; Pfaff, H.; Karbach, U. Does Value Stream Mapping affect the structure, process, and outcome quality in care facilities? A systematic review. Syst. Rev. 2017, 6, 1–11. [Google Scholar] [CrossRef]
- Barnabè, F.; Giorgino, M.C.; Guercini, J.; Bianciardi, C.; Mezzatesta, V. Management simulations for Lean healthcare: exploiting the potentials of role-playing. J. Heal. Organ. Manag. 2018, 32, 298–320. [Google Scholar] [CrossRef]
- Souza, D.L.; Korzenowski, A.L.; Alvarado, M.M.; Sperafico, J.H.; Ackermann, A.E.F.; Mareth, T.; Scavarda, A.J. A Systematic Review on Lean Applications’ in Emergency Departments. Healthcare 2021, 9, 763. [Google Scholar] [CrossRef]
- Zepeda-Lugo, C.; Tlapa, D.; Baez-Lopez, Y.; Limon-Romero, J.; Ontiveros, S.; Perez-Sanchez, A.; Tortorella, G. Assessing the Impact of Lean Healthcare on Inpatient Care: A Systematic Review. Int. J. Environ. Res. Public Heal. 2020, 17, 5609. [Google Scholar] [CrossRef]
- Rotter, T.; Plishka, C.; Lawal, A.; Harrison, L.; Sari, N.; Goodridge, D.; Flynn, R.; Chan, J.; Fiander, M.; Poksinska, B.; et al. What Is Lean Management in Health Care? Development of an Operational Definition for a Cochrane Systematic Review. Evaluation Heal. Prof. 2018, 42, 366–390. [Google Scholar] [CrossRef]
- Charns, M.P.; Lerner, B.; Yakovchenko, V.; Urech, T.H.; Shin, M.H.; Kim, B.; Engle, R.L.; Vashi, A.A. Achieving transformation to lean management systems in health care. Heal. Serv. Res. 2022, 58, 343–355. [Google Scholar] [CrossRef]
- K, V.K.; K, S.; Kandasamy, J.; Venkat, V.; Mani, R.S. Barriers to the adoption of digital technologies in a functional circular economy network. Oper. Manag. Res. 2023, 16, 1541–1561. [Google Scholar] [CrossRef]
- Smith, I.; Hicks, C.; McGovern, T. Adapting Lean methods to facilitate stakeholder engagement and co-design in healthcare. BMJ 2020, 368, m35. [Google Scholar] [CrossRef]
- U.S. Environmental Protection Agency (EPA), “Effluent Limitations Guidelines and Standards for the Dental Office Category. https://www.federalregister. 2017.
- Simonsen, E.M.; Herrera, R.F.; Atencio, E. Benefits and Difficulties of the Implementation of Lean Construction in the Public Sector: A Systematic Review. Sustainability 2023, 15, 6161. [Google Scholar] [CrossRef]
- Tlapa, D.; Tortorella, G.; Fogliatto, F.; Kumar, M.; Mac Cawley, A.; Vassolo, R.; Enberg, L.; Baez-Lopez, Y. Effects of Lean Interventions Supported by Digital Technologies on Healthcare Services: A Systematic Review. Int. J. Environ. Res. Public Heal. 2022, 19, 9018. [Google Scholar] [CrossRef]
- Tsai, C.H.; Eghdam, A.; Davoody, N.; Wright, G.; Flowerday, S.; Koch, S. Effects of Electronic Health Record Implementation and Barriers to Adoption and Use: A Scoping Review and Qualitative Analysis of the Content. Life 2020, 10, 327. [Google Scholar] [CrossRef]
- Boronat, F.; Budia, A.; Broseta, E.; Ruiz-Cerdá, J.; Vivas-Consuelo, D. Aplicación de la metodología Lean healthcare en un servicio de urología de un hospital terciario como herramienta de mejora de la eficiencia. Actas Urol Esp 2018, 42, 42–48. [Google Scholar] [CrossRef]
- La Forgia, D.; Paparella, G.; Signorile, R.; Arezzo, F.; Comes, M.C.; Cormio, G.; Daniele, A.; Fanizzi, A.; Fioretti, A.M.; Gatta, G.; et al. Lean Perspectives in an Organizational Change in a Scientific Direction of an Italian Research Institute: Experience of the Cancer Institute of Bari. Int. J. Environ. Res. Public Heal. 2022, 20, 239. [Google Scholar] [CrossRef]
- Maware, C.; Parsley, D.M. The Challenges of Lean Transformation and Implementation in the Manufacturing Sector. Sustainability 2022, 14, 6287. [Google Scholar] [CrossRef]
- Rehman, N.; Mahmood, A.; Ibtasam, M.; Murtaza, S.A.; Iqbal, N.; Molnár, E. The Psychology of Resistance to Change: The Antidotal Effect of Organizational Justice, Support and Leader-Member Exchange. Front. Psychol. 2021, 12, 678952. [Google Scholar] [CrossRef]
- FDI. Consensus on Environmentally Sustainable Oral Healthcare: A Joint Stakeholder Statement. https://www.fdiworlddental.org/sites/default/files/2022-03/Consensus%20Statement%20-%20FDI.
- Shoplogix. Guide to Lean Continuous Improvement: Boost Efficiency and Growth. , 2024. https://shoplogix. 13 June.
- Raza, AH. Lean Continuous Improvement – What It is and Why You Should Implement It? , 2023. https://throughput. 19 December.
- Aziz, R.F.; Hafez, S.M. Applying lean thinking in construction and performance improvement. Alex. Eng. J. 2013, 52, 679–695. [Google Scholar] [CrossRef]
- Costa, L.B.M.; Filho, M.G.; Rentes, A.F.; Bertani, T.M.; Mardegan, R. Lean healthcare in developing countries: evidence from Brazilian hospitals. Int. J. Heal. Plan. Manag. 2015, 32, e99–e120. [Google Scholar] [CrossRef]
- García-Cutrín, J.; Rodríguez-García, C. Enhancing Corporate Sustainability through Just-In-Time (JIT) Practices: A Meta-Analytic Examination of Financial Performance Outcomes. Sustainability 2024, 16, 4025. [Google Scholar] [CrossRef]
- Antoniadou, M.; Intzes, A.; Kladouchas, C.; Christou, I.; Chatzigeorgiou, S.; Plexida, M.; Stefanidakis, V.; Tzoutzas, I. Factors Affecting Water Quality and Sustainability in Dental Practices in Greece. Sustainability 2023, 15, 9115. [Google Scholar] [CrossRef]
- Silver, S.A.; Harel, Z.; McQuillan, R.; Weizman, A.V.; Thomas, A.; Chertow, G.M.; Nesrallah, G.; Bell, C.M.; Chan, C.T. How to Begin a Quality Improvement Project. Clin. J. Am. Soc. Nephrol. 2016, 11, 893–900. [Google Scholar] [CrossRef]
- Patalas-Maliszewska, J.; Szmołda, M.; Łosyk, H. Integrating Artificial Intelligence into the Supply Chain in Order to Enhance Sustainable Production—A Systematic Literature Review. Sustainability 2024, 16, 7110. [Google Scholar] [CrossRef]
- Shuaib, A. Transforming Healthcare with AI: Promises, Pitfalls, and Pathways Forward. Int. J. Gen. Med. 2024, ume 17, 1765–1771. [Google Scholar] [CrossRef]
- Pawlak, S. The Impact of Selected Lean Manufacturing Tools on the Level of Delays in the Production Process. A Case Study. Manag. Syst. Prod. Eng. 2024, 32, 103–107. [Google Scholar] [CrossRef]
| Category | Author(s) and year | Title | Key insights | Type of waste described | Lean tools/techniques | Cochrane Risk of Bias tool | CASP checklist |
| Lean in healthcare general application | Mahmoud et al. (2021) [16] | The impact of Lean management on Frontline Healthcare Professionals | Lean improves workflow, reduces stress, and enhances staff performance | Overproduction, Excess Motion | Value Stream Mapping (VSM), Kaizen | Low risk | Meets most CASP criteria |
| Tierney et al. (2022) [36] | Examining the Relationship Between the Lean Management System and Quality Improvement Care Processes | Lean management directly improves quality care and reduces inefficiencies in hospitals | Waiting, Overprocessing | Kaizen, Root Cause Analysis | Low risk | Meets all CASP criteria | |
| Bektas & Kiper (2022) [37] | Applications of Lean in Human Resources Management in Healthcare | Lean in HRM improves staff allocation and resource utilization in healthcare | Talent Misuse, Overproduction | 5S, Standardization | Low risk | Meets most CASP criteria | |
| van Rossum et al. (2016) [38] | Lean healthcare from a change management perspective | Lean principles facilitate organizational change and enhance process improvement | Waiting, Overprocessing | PDCA Cycle, Process Mapping | Unclear risk | Meets some CASP criteria | |
| Sloan et al. (2014) [39] | Lean in healthcare: History and recent developments | Historical and modern applications of lean in healthcare | Overproduction, Waiting | 5S, Standardization | Unclear risk | Meets some CASP criteria | |
| Bowe et al. (2021) [40] | Process Mapping and Lean Principles Applied to Orthognathic Surgery | Lean and process mapping improve efficiency and surgical outcomes | Overprocessing, Defects | Process Mapping, Kaizen, 5 Whys | Low risk | Meets most CASP criteria | |
| Lean in healthcare supply chain & waste management | Bharsakade et al. (2021) [7] | A lean approach to healthcare management using multi-criteria decision making | Lean optimizes healthcare supply chains and reduces waste | Overproduction, Excess Inventory | Multi-Criteria Decision Making (MCDM) | Low risk | Meets most CASP criteria |
| Borges et al. (2019) [41] | Lean Implementation in Healthcare Supply Chain: A Scoping Review | Lean streamlines supply chains, reducing waste and unnecessary inventory | Excess Inventory, Transportation | VSM, Just-In-Time (JIT) | Low risk | Meets all CASP criteria | |
| Crema & Verbano (2017) [42] | Lean management to Support Choosing Wisely in Healthcare | Lean aligns resource use with actual demand, preventing overproduction | Overproduction, Excess processing | Choosing Wisely Initiative, 5S | Low Risk | Meets most CASP criteria | |
| Burgess & Radnor (2013) [43] | Evaluating lean in healthcare | Evaluation of lean effectiveness in reducing waste and improving patient care | Waiting, Transportation | Process Mapping, Continuous Improvement | High Risk | Meets some CASP criteria | |
| Prado-Prado et al. (2020) [44] | Increasing competitiveness through the Implementation of lean management in healthcare | Lean improves competitiveness by streamlining processes and enhancing productivity | Overproduction, Talent misuse | Standardization, Process Mapping | Unclear Risk | Meets some CASP criteria | |
| Nazarali et al. (2017) [45] | The application of a “6S Lean” initiative to improve workflow for emergency eye examination rooms | 6S methodology removes inefficiencies in eye examination rooms, enhancing patient care | Waiting, Excess inventory, Overprocessing | 6S, VSM | Low Risk | Meets most CASP criteria | |
| Lean healthcare tools | De Barros et al. (2021) [46] | Lean Healthcare Tools for Processes Evaluation: An Integrative Review | Lean tools such as VSM and Kanban improve patient flow and care delivery in dental practices | Waiting, Defects, Overprocessing | VSM, Kanban, 5S | Low risk | Meets all CASP criteria |
| Flynn et al. (2018) [47] | The sustainability of lean in pediatric healthcare: A realist review | Lean principles improve the sustainability of healthcare operations, transferable to dental practices | Overprocessing, Waiting | Kaizen, Continuous Improvement | Low Risk | Meets all CASP criteria | |
| Morales-Contreras et al. (2020) [48] | Applying lean in process innovation in healthcare: The case of hip fracture | Process innovations using lean principles improve healthcare efficiency, relevant to dental practice | Overprocessing, Waiting | Process Innovation, PDCA | Unclear Risk | Meets most CASP criteria | |
| Freitas et al. (2023) [49] | Implementation of the lean healthcare System in the emergency room: A case study | Lean reduces wait times and improves patient throughput, applicable in dental practices | Waiting, Motion | Kaizen, 5 Whys | Low Risk | Meets all CASP criteria | |
| Milstein & Homer (2009) [50] | System dynamics as a conceptual framework for examining health disparities | System dynamics and lean principles address health disparities, applicable for equity in dental care | Talent misuse, Waiting | System Dynamics Model | Low Risk | Meets all CASP criteria | |
| Lean specifically in dentistry | Romanos & Gupta (2022) [15] | Applied lean principles in dental practice | Implementation of lean principles in dental practices improved operational efficiency and reduced waste | Overprocessing, Excess Inventory | Kaizen, 5S, VSM | Low risk | Meets all CASP criteria |
| Robinson et al. (2019) [51] | Clinical integration in a dental school clinic through an enhanced patient intake process | Lean management eliminates waste in dental school clinics, improving patient intake processes | Waiting, Defects | Process Mapping, VSM | Low risk | Meets all CASP criteria | |
| Robinson et al. (2016) [52] | Improving a dental school’s clinic operations using lean process improvement | Lean techniques streamline operations in dental schools, reducing inefficiencies | Overprocessing, Motion, Excess Inventory | Process Mapping, 5S, JIT | Low risk | Meets all CASP criteria | |
| Lean in other healthcare areas | Robinson et al. (2019) [53] | The use of lean in medical centers to enhance diagnostic processes | Lean principles enhance diagnostic processes, improving accuracy and efficiency | Overprocessing, Waiting | VSM, Continuous improvement | Low risk | Meets all CASP criteria |
| Kenney et al. (2015) [54] | Lean implementation in a pediatric healthcare setting: Lessons learned | Lean improves clinical efficiency and patient care in pediatric settings, applicable in dental care | Waiting, Defects | VSM, Kaizen, 5S | Unclear risk | Meets some CASP criteria | |
| Rosengarten et al. (2020) [55] | Enhancing patient safety in surgery: A lean approach | Lean principles reduce defects and improve safety in surgical procedures, transferable to dental surgeries | Defects, Overprocessing | VSM, 5 Whys | Low risk | Meets all CASP criteria | |
| Gordon et al. (2018) [56] | Using lean to improve efficiency in a Hospital’s Emergency department | Lean reduces wait times and improves efficiency in emergency departments, relevant for dental emergencies | Waiting, Motion | 6S, VSM | Low risk | Meets all CASP criteria | |
| Smith et al. (2019) [57] | The effect of lean principles on outpatient clinics | Lean principles improve outpatient clinic performance by minimizing waste | Waiting, Overproduction | Kanban, Kaizen | Low risk | Meets all CASP criteria | |
| Burns et al. (2020) [58] | Reducing surgical complications using lean tools | Lean reduces surgical complications and improves outcomes in healthcare | Defects, Overprocessing | 5 Whys, Root Cause Analysis | Low risk | Meets all CASP criteria | |
| Kowal et al. (2017) [59] | Lean in radiology: Improving Workflow and Reducing Patient Delays | Lean improves radiology department workflows and minimizes patient delays | Waiting, Motion | VSM, Continuous Improvement | Low risk | Meets all CASP criteria | |
| Newman et al. (2018) [60] | Lean in oncology: streamlining Cancer Treatment Processes | Lean principles streamline cancer treatment processes, leading to better outcomes | Waiting, Overprocessing | 5S, VSM | Low risk | Meets all CASP criteria | |
| Peirson et al. (2020) [61] | Improving Efficiency in a geriatric care facility using lean principles | Lean tools improve the efficiency of geriatric care processes | Waiting, Defects | PDCA, VSM | Low Risk | Meets all CASP criteria | |
| Marshall et al. (2017) [62] | Lean in mental health: Application to inpatient care | Lean principles are successfully applied to mental health inpatient care, improving outcomes | Waiting, Overprocessing | Process Mapping, 5 Whys | Low risk | Meets all CASP criteria |
| Key issues explored: | Number of articles | Percentages |
| 1. Lean implementation in general healthcare settings | 10 | 33.3% |
| 2. Lean application in supply chain and waste management | 7 | 23.3% |
| 3. Lean principles specifically in dentistry | 8 | 26.7% |
| 4. Lean in other healthcare areas (e.g., Surgery, Emergency Care, Radiology) | 5 | 16.7% |
| Breakdown of specific issues: | ||
| • Workflow efficiency improvement | 20 | 66.7% |
| • Waste reduction and management | 17 | 56.7% |
| • Patient satisfaction and care quality enhancement | 15 | 50% |
| • Supply chain optimization | 9 | 30% |
| • Staff performance and resource utilization | 12 | 40% |
| • Error reduction and patient safety | 8 | 26.7% |
| • Sustainability of lean practices | 5 | 16.7% |
| • Lean tools and techniques application (e.g., VSM, 5S, Kaizen) | 25 | 83.3% |
| Theme | Number of articles | Percentage |
| Workflow efficiency | 15 | 30 |
| Patient satisfaction | 10 | 20 |
| Supply chain & inventory management | 8 | 16 |
| Cost reduction | 7 | 14 |
| Error reduction & safety | 6 | 12 |
| Sustainability of lean practices | 4 | 8 |
| Lean tool | Description & evidence study | Application in dentistry | Outcome | Impact on patient satisfaction | Example |
| Value Stream Mapping (VSM) | A tool used to visualize the flow of information and materials, identifying inefficiencies and waste (Flynn et al., 2018) [47]. | Maps out patient journeys from booking to treatment, identifying bottlenecks and delays. | Improved patient flow, and reduced wait times by eliminating non-value-adding activities. | Reduces patient wait times, improving the overall patient experience by eliminating bottlenecks. | A dental clinic redesigns patient check-in to reduce idle time, improving the overall experience. |
| 5S Methodology | A workplace organization tool with five principles: Sort, Set in Order, Shine, Standardize, and Sustain (Robinson et al., 2019) [52]. | Organizes clinical tools and materials for easy access, reducing time spent searching for items during treatment. | Reduced setup times, more efficient use of space, and enhanced productivity. | Creates a professional, organized environment that builds patient trust, improving satisfaction. | Dental clinics use 5S to reduce setup times, leading to quicker transitions between patients and improved service delivery. |
| Kaizen (Continuous Improvement) | Focuses on small, incremental changes made regularly to improve efficiency and patient care (Bektas & Kiper, 2022) [37]. | Regular meetings to review clinical processes, such as patient intake and sterilization. | Continuous enhancements in workflow efficiency and patient satisfaction. | Leads to ongoing improvements in patient care, communication, and service quality, enhancing patient trust. | Regular Kaizen meetings in dental clinics identify areas for improvement, such as reducing time between check-in and treatment. |
| Kanban | A visual tool used for managing inventory and ensuring materials are available without overstocking (Bharsakade et al., 2021) [7]. | Helps manage dental consumables like gloves, masks, and dental materials, preventing overstocking or shortages. | Reduced inventory costs and more efficient material use. | Ensures timely and uninterrupted care by preventing supply shortages, and improving patient satisfaction. | Dental clinics use Kanban to maintain optimal stock levels of consumables, preventing delays in treatment due to material shortages. |
| Root Cause Analysis (5 Whys) | Identifies the underlying cause of problems by asking “why” multiple times to reveal the root issue (Burns et al., 2020) [58]. | Investigates issues such as delayed appointments or patient dissatisfaction, tracing problems to their root causes. | Effective identification and resolution of recurring problems, reducing errors and improving patient care. | Resolves recurring issues, ensuring smoother, more reliable care and improved patient satisfaction. | A clinic uses the 5 Whys technique to discover inefficiencies in scheduling, improving appointment flow and reducing wait times for patients. |
| Just-In-Time (JIT) | Ensures materials and resources are available only when needed, reducing overproduction and excess inventory (Borges et al., 2019) [41]. | Applied to order supplies like dental implants only when necessary, minimizing overstocking and waste. | Reduced waste from expired or unnecessary materials and lower inventory costs. | Reduces patient wait times for treatments by ensuring necessary materials are available when needed. | Dental clinics use JIT to ensure that crowns or implants are available on time, reducing delays in treatments and enhancing patient satisfaction. |
| Standard Work | Standardizes processes for routine tasks to ensure consistency and efficiency in care delivery (Sloan et al., 2014) [39]. | Standardized workflows for procedures such as dental cleanings, chair setup, and sterilization. | Consistent, high-quality care with fewer errors and improved staff efficiency. | Ensures consistent, reliable care, contributing to increased patient satisfaction. | Standardizing patient intake and hygiene procedures ensures consistent care quality, leading to higher patient satisfaction. |
| Poka-Yoke (Error Proofing) | A method of designing systems that prevent mistakes before they occur by incorporating fail-safes and checks (Rosengarten et al., 2020) [55]. | Error-proofing protocols in sterilization or clinical documentation prevent mistakes like incomplete sterilization. | Enhanced patient safety and reduced clinical errors, improving overall care quality. | Reduces errors such as billing mistakes or treatment delays, leading to smoother, more reliable patient care. | Dental clinics use error-proofing techniques to prevent scheduling or billing errors, reducing frustration and enhancing the overall patient experience. |
| Type of waste | Lean tools | Circular economy principle | Practices | Outcomes in dentistry | Innovative ideas from other fields |
| Overproduction | Just-In-Time (JIT) | Resource optimization & minimization of waste | Ordering materials only when needed, reducing stockpiling of dental materials. | Reduced waste from expired materials, lower inventory costs, enhanced resource use. | Manufacturing: Implement JIT to reduce surplus and prevent materials from becoming obsolete, as seen in automotive production. |
| Waiting | Value Stream Mapping (VSM) | Improved Efficiency & Time optimization | Mapping patient flow from intake to treatment, reducing waiting periods in the clinic. | Shorter patient wait times, smoother workflow, increased patient satisfaction. | Retail: Use VSM to streamline customer service and reduce checkout times, increasing customer retention. |
| Excess Inventory | Kanban | Closed-Loop Systems & inventory control | Visual management system to prevent overstocking of consumables like gloves and masks. | Better stock management, decreased costs, and more efficient ordering processes. | Logistics: Implement Kanban for real-time inventory management, minimizing overstocking and enhancing supply chain performance. |
| Motion (Unnecessary movement) | 5S | Circular design & space efficiency | Organizing treatment areas for optimal movement and accessibility of tools. | Improved ergonomics for dental staff, faster procedure setups, enhanced patient care. | Hospitality: Use 5S to streamline kitchen layouts in restaurants for faster food preparation and delivery. |
| Defects | Root Cause Analysis (5 Whys) | Quality control & process standardization | Identifying and resolving the root causes of frequent procedural errors. | Reduced treatment errors, increased patient safety, fewer repeated procedures. | Pharmaceuticals: RCA is used to investigate the root causes of drug manufacturing errors, ensuring higher product quality. |
| Overprocessing | Standard work | Standardization & uniform processes | Standardized treatment protocols for common dental procedures, reducing unnecessary steps. | Consistency in treatment quality, reduced procedure times, increased efficiency. | Construction: Use standard work to streamline repetitive tasks, ensuring consistent quality and faster project delivery. |
| Waste of resources | Poka-Yoke (Error Proofing) | Resource Preservation & Error Prevention | Implementing fail-safes in sterilization processes to avoid contamination. | Improved patient safety, fewer sterilization-related errors, better regulatory compliance. | Electronics: Poka-Yoke is used in electronics manufacturing to ensure that components are assembled correctly, reducing defects. |
| Talent misuse | Kaizen (Continuous improvement) | Workforce optimization & skills enhancement | Involving the entire dental team in continuous improvement initiatives, identifying better ways to utilize staff. | Enhanced employee engagement, optimized workflows, increased job satisfaction. | Tech startups: Adopt Kaizen to empower employees to suggest improvements in workflow efficiency, boosting innovation and job satisfaction. |
| Circular economy practice | Manufacturing example | Adoption in dentistry | Outcome |
| Industrial symbiosis [63] | Collaboration where waste from one process is used as input for another, reducing material waste and increasing efficiency. | Dental clinics can return unused materials to manufacturers for recycling or collaborate with other industries for material reuse. | Reduced waste, lowered material costs, and sustainable supply chain. |
| Closed-loop supply chains [64] | Products are designed to be reused, refurbished, or recycled to keep materials in circulation for longer. | Clinics can partner with suppliers offering take-back programs for dental tools and packaging. | Reduced environmental impact, lower operational waste, and promotion of sustainable product lifecycle. |
| Additive manufacturing (3D Printing) [65] | Custom parts are produced on-demand, minimizing material waste and reducing excess production. | Clinics can use 3D printing for patient-specific dental restorations, minimizing the need for large inventories and reducing material waste. | Reduced waste, faster production, better patient outcomes due to customization, and lower reliance on mass production. |
| Product life extension (Repair, Refurbishment, Remanufacturing) [66] | Manufacturers extend product life through repair, refurbishment, or remanufacturing instead of discarding. | Clinics can refurbish or remanufacture dental instruments (e.g., handpieces) instead of purchasing new ones. | Reduced environmental impact, cost savings, and longer-lasting tools. |
| Material substitution with sustainable alternatives in multiple industries [2] | Substitution of harmful materials with sustainable, biodegradable, or recycled alternatives in manufacturing. | Clinics can switch to biodegradable or recyclable materials for single-use items like suction tips, plastic cups, or sterilization wraps. | Reduced plastic waste and lower environmental footprint through sustainable material use. |
| Modular design for dental equipment [67] | Products are designed with modular components, allowing upgrades and repairs instead of replacing entire units. | Dental equipment can be designed modularly so individual parts like motors or attachments can be upgraded or replaced without purchasing new equipment. | Lower costs, reduced waste, and improved sustainability through repairable equipment. |
| Zero-waste manufacturing [34] | Processes are designed where all waste is reused, recycled, or repurposed, eliminating waste. | Clinics can adopt zero-waste principles by recycling all materials and minimizing packaging waste through bulk purchases and reusable containers. | Significant reduction in waste, increased recycling rates, and movement toward a zero-waste dental practice. |
| Servitization [68] | Shift from selling products to offering maintenance and support services, extending product life and reducing frequent replacements. | Suppliers can offer service contracts for maintenance and repair, extending the life of dental equipment like chairs and diagnostic tools. | Extended product lifespan, reduced capital expenditure for new equipment, and minimized resource consumption. |
| No. | Educational activity | Description | Key studies |
| 1 | Training programs on lean fundamentals [51,54] | Formal training programs on lean principles (VSM, 5S, Kaizen, Root Cause Analysis), embedded in CPD and curricula for healthcare professionals. | Training programs in dental schools and healthcare settings emphasize understanding lean concepts to reduce waste and improve workflow. |
| 2 | Hands-on workshops and simulations [45,47] | Engaging participants in simulations, role-playing, and problem-solving activities to teach lean principles in practical settings. | Workshops focusing on organizing workspaces, improving patient flow, and reducing waste are essential for skill development. |
| 3 | Mentorship and lean leadership programs [16,37] | Developing lean champions who mentor staff and ensure the long-term success of lean practices. | Establishment of mentorship programs where leaders guide their peers in adopting and sustaining lean practices over time. |
| 4 | Interdisciplinary learning and collaboration [48,49] | Collaborative projects across departments or specialties that encourage sharing of ideas and process improvements. | Collaboration between different departments or specialties helps solve common inefficiencies through shared lean projects in healthcare and dental settings. |
| 5 | Continuous learning through feedback loops [52,58] | Establishing a continuous feedback loop where staff regularly assess and adjust processes based on recent performance and metrics. | Creating regular feedback sessions that monitor progress, allowing staff to reflect on lean implementation and identify areas for further improvement. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




