Submitted:
29 March 2024
Posted:
01 April 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Patients and Study Design
2.2. Diagnosis and Severity of HZ
2.3. The Clinical Phenotypes
2.4. Determination of RF and ACPA
2.5. Determination of Serum Titers of Anti-IFN-γ IgG with ELISA
2.6. Determination of Plasma Levels of IFN-γ, MCP-1 and IP-10
2.7. Statistical Analysis
3. Results
3.1. The Comparison of Clinical Characteristics, Laboratory Data, and HZ-Related Status between RA Patients with and without New-Onset HZ
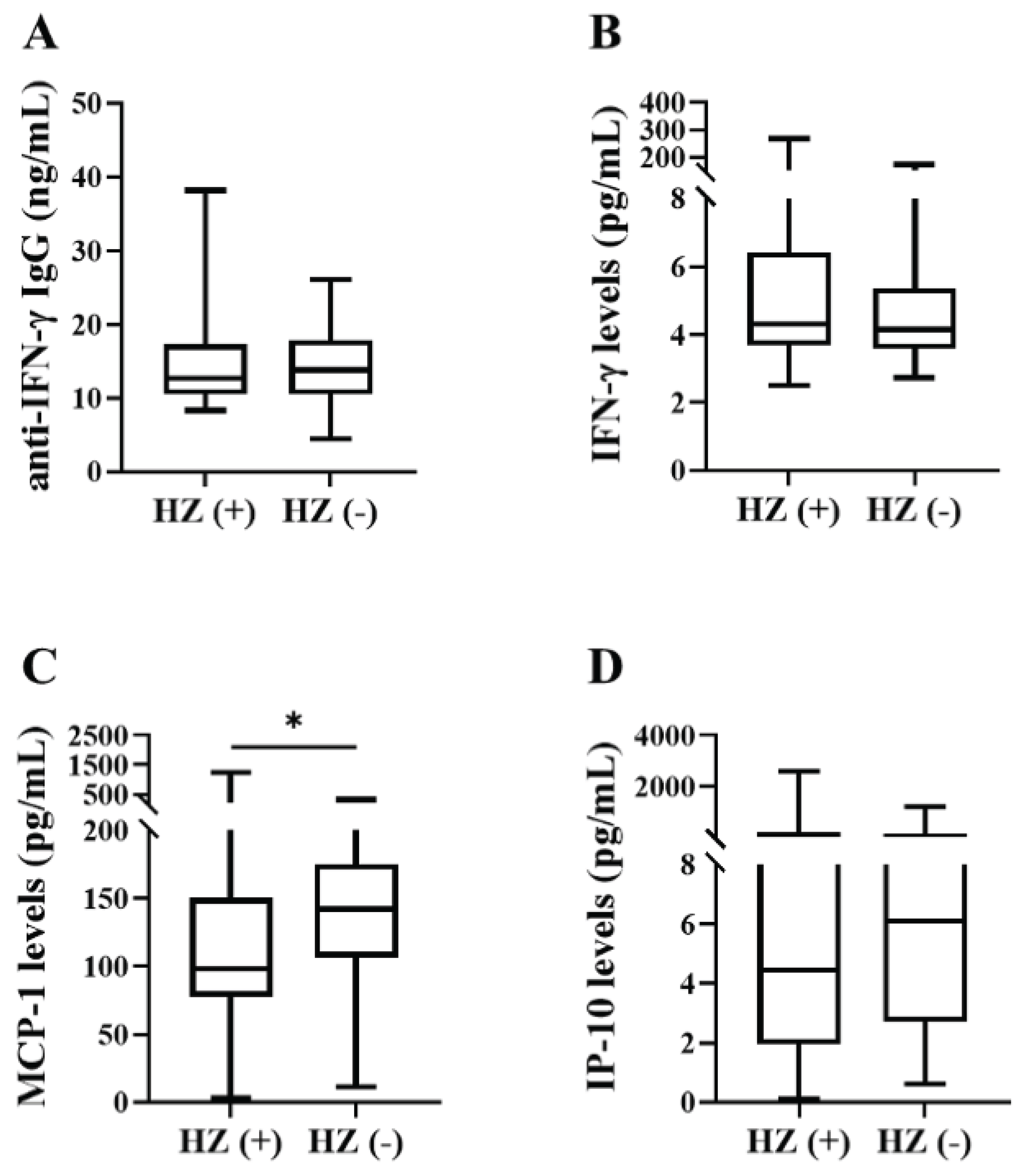
3.2. Comparison of the Titers of anti-IFN-γ IgG, Plasma Levels of IFN-γ, MCP-1, and IP-10 between RA Patients with and without HZ.
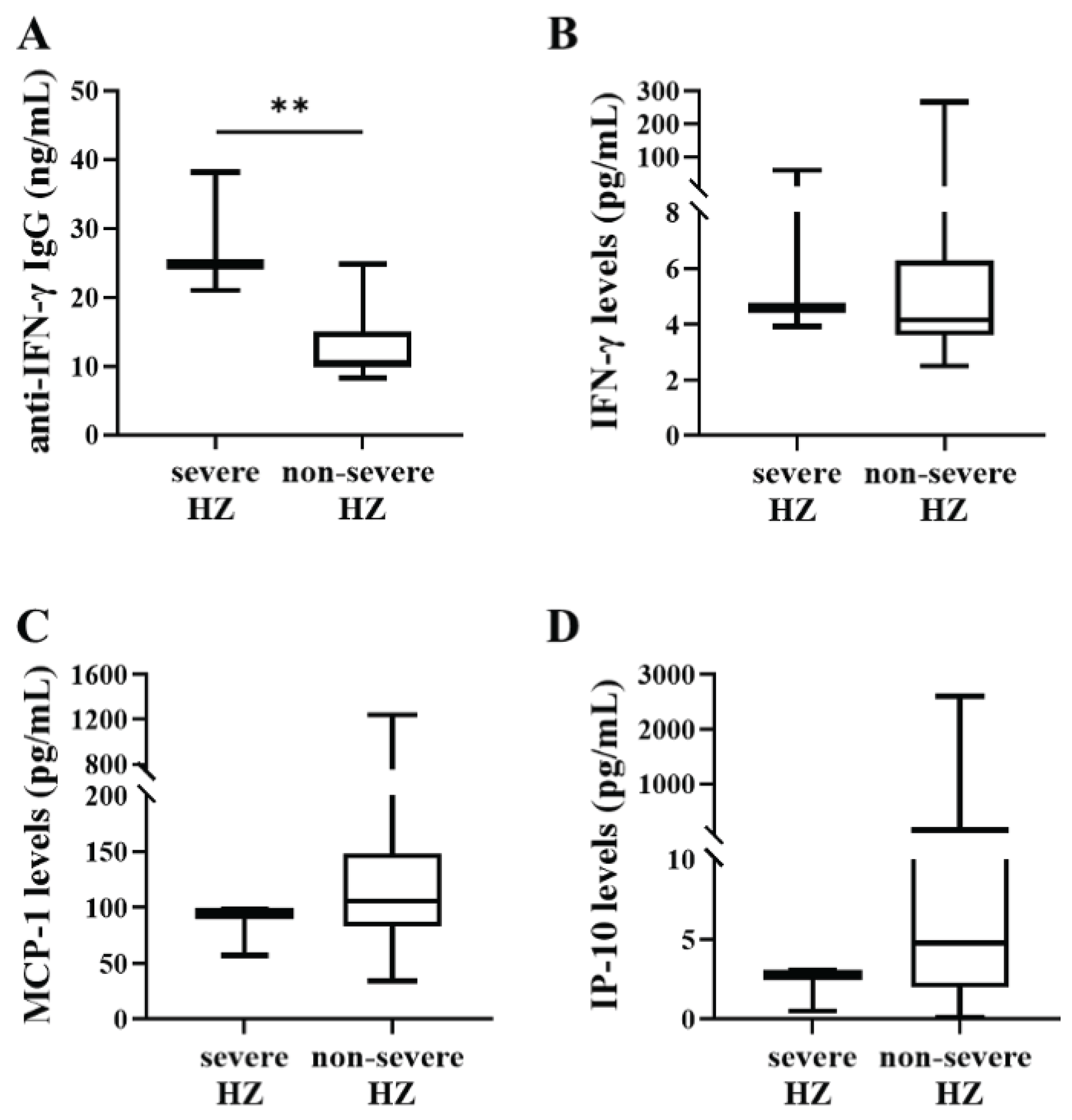
3.3. Comparison of the Titers of Anti-IFN-γ IgG, Plasma Levels of IFN-γ, MCP-1, and IP-10 between RA Patients with Severe and Non-Severe HZ.
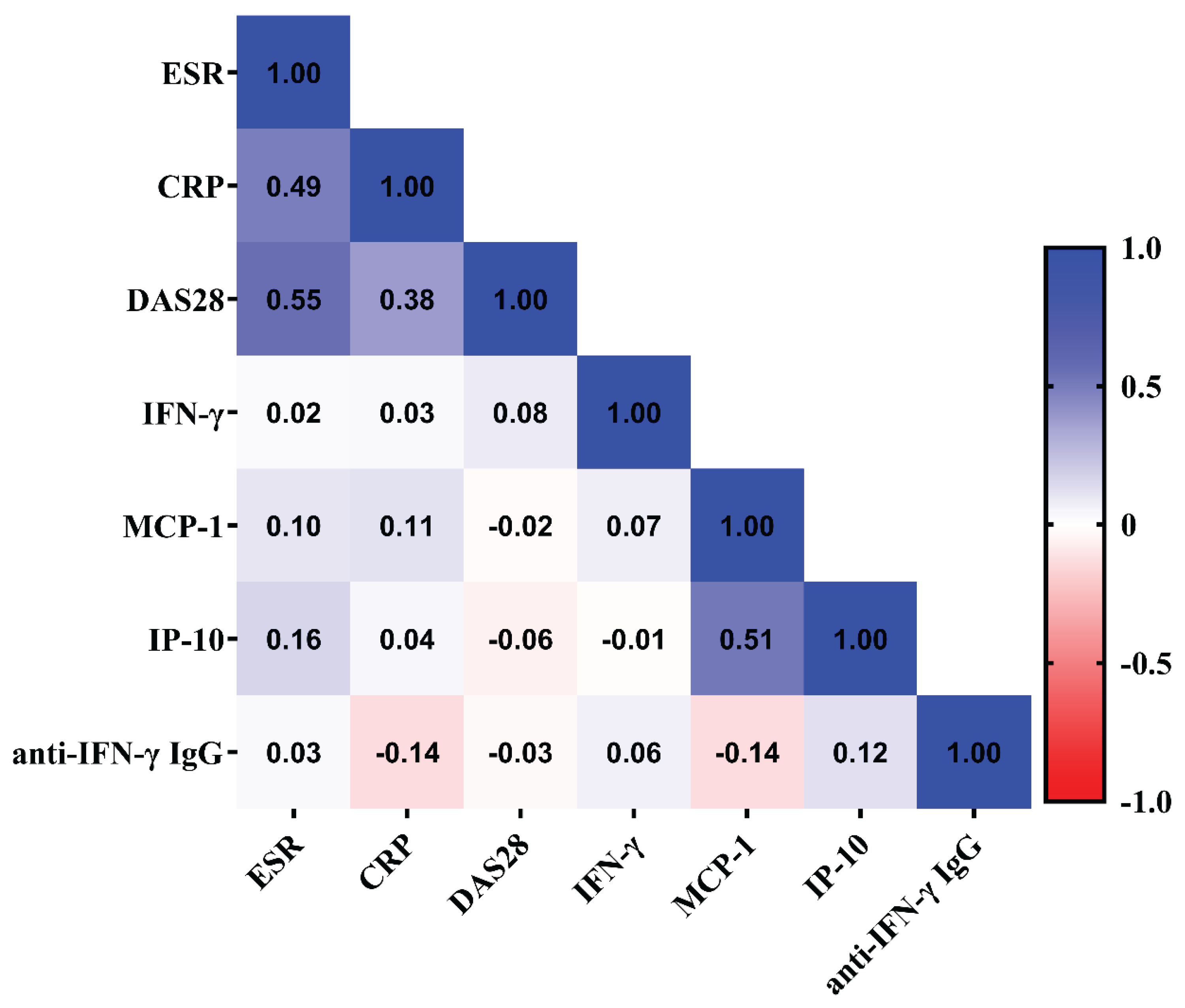
3.4. Association of Serum Titers of anti-IFN-γ IgG with RA Disease Activity and Inflammatory Parameters
4. Discussion
5. Conclusions
Author Contributions
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Schoenborn, J.R.; Wilson, C. Regulation of interferon-gamma during innate and adaptive immune responses. Adv Immunol. 2007, 96, 41–101. [Google Scholar]
- Shakya, A.K.; O’Callaghan, D.J.; Kim, S.K. Interferon gamma inhibits Varicella-Zoster virus replication in a cell line-dependent manner. J Virology 2019, 93, e00257–19. [Google Scholar] [CrossRef] [PubMed]
- Patel, S.Y.; Ding, L.; Brown, M.R.; Lantz, L.; Gay, T.; Cohen, S.; Martyak, L.A.; Kubak, B.; Holland, S.M. Anti-IFN-gamma autoantibodies in disseminated nontuberculous mycobacterial infections. J Immunol 2005, 175, 4769–4776. [Google Scholar] [CrossRef] [PubMed]
- Wipasa, J.; Chaiwarith, R.; Chawansuntati, K.; Praparattanapan, J.; Rattanathammethee. K.; Supparatpinyo, K. Characterization of anti-interferon-γ antibodies in HIV-negative immunodeficient patients infected with unusual intracellular microorganisms. Experimental Biology and Medicine 2018, 243, 621–626. [Google Scholar] [CrossRef] [PubMed]
- Browne, S.K.; Burbelo, P.D.; Chetchotisakd, P.; Suputtamongkol, Y.; Kiertiburanakul, S.; Shaw, PA.; Kirk, J.L.; Jutivorakool, K.; Zaman, R.; Ding, L.; et al. Adult-onset immunodeficiency in Thailand and Taiwan. N Engl J Med 2012, 36, 7725–734. [Google Scholar] [CrossRef] [PubMed]
- Chi, C.Y.; Chu, C.C.; Liu, J.P.; Lin, C.H.; Ho, M.W.; Lo, W.J.; Lin, P.C.; Chen, H.J.; Chou, C.H.; Feng, J.Y.; et al. Anti-IFN-γ autoantibodies in adults with disseminated nontuberculous mycobacterial infections are associated with HLA-DRB1*1602 and HLA-DQB1*0502 and the reactivation of latent varicella-zoster virus infection. Blood 2013, 121, 1357–1366. [Google Scholar] [CrossRef]
- Hong, G.H.; Ortega-Villa, A.M.; Hunsberger, S.; Chetchotisakd, P.; Anunnatsiri, S.; Mootsikapun, P.; Rosen, L.B.; Zerbe, C.S.; Holland, S.M. Natural history and evolution of anti-interferon-γ autoantibody-associated immunodeficiency syndrome in Thailand and the United States. Clin Infect Dis 2020, 71, 53–62. [Google Scholar] [CrossRef] [PubMed]
- Gupta, S.; Tatouli, I.P.; Rosen, L.B.; Hasni, S.; Alevizos, I.; Manna, Z.G.; Rivera, J.; Jiang, C.; Siegel, R.M.; Holland, S.M.; et al. Distinct functions of anti-interferon autoantibodies in systemic lupus erythematosus: a comprehensive analysis of anticytokine antibodies in common rheumatologic diseases. Arthritis Rheumatol. 2016, 68, 1677–1687. [Google Scholar] [CrossRef] [PubMed]
- Wu, U.I.; Wang, J.T.; Sheng, W.H.; Sun, H.Y.; Cheng, A.; Hsu, L.Y.; Chang, S.C.; Chen, Y.C. Incorrect diagnoses in patients with neutralizing anti-interferon-gamma autoantibodies. Clin Microbiol Infection 2020, 26, 1684.e1–1684.e6. [Google Scholar] [CrossRef]
- Smolen, J.S.; Aletaha, D.; McInnes, I.B. Rheumatoid arthritis. Lancet 2016, 388, 2023–2038. [Google Scholar] [CrossRef]
- Smitten, A.L.; Choi, H.K.; Hochberg, M.C.; Suissa, S.; Simon, T.A.; Testa, M.A.; Chan, K.A. The risk of herpes zoster in patients with rheumatoid arthritis in the United States and the United Kingdom. Arthritis Rheum 2007, 57, 1431–1438. [Google Scholar] [CrossRef] [PubMed]
- McDonald, J.R.; Zeringue, A.L.; Caplan, L.; Ranganathan, P.; Xian, H.; Burroughs, T.E.; Fraser, V.J.; Cunningham, F.; Eisen, S.A. Herpes zoster risk factors in a national cohort of veterans with rheumatoid arthritis. Clin Infect Dis 2009, 48, 1364–1371. [Google Scholar] [CrossRef] [PubMed]
- Liao, T.L.; Chen, Y.M.; Liu, H., J.; Chen, D.Y. Risk and severity of herpes zoster in patients with rheumatoid arthritis receiving different immunosuppressive medications: a case-control study in Asia. BMJ Open 2017, 7, e0140327. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, Y. Recent progress in treatments of rheumatoid arthritis: an overview of developments in biologics and small molecules, and remaining unmet needs. Rheumatology 2021, 60, vi12–vi20. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S.B.; Tanaka, Y.; Mariette, X.; Curtis, J.R.; Lee, E.B.; Nash, P.; Winthrop, K.L.; Charles-Schoeman, C.; Thirunavukkarasu, K.; DeMasi, R.; et al. Long-term safety of tofacitinib for the treatment of rheumatoid arthritis up to 8.5years: integrated analysis of data from the global clinical trials. Ann Rheum 2017, 76, 1253–1262. [Google Scholar] [CrossRef] [PubMed]
- Fleischmann, R.; Curtis, J.R.; Charles-Schoeman, C.; Mysler, E.; Yamaoka, K.; Richez, C.; Palac, H.; Dilley, D.; Liu, J.; Strengholt, S.; et al. Safety profile of Upadacitinib in patients at risk of cardiovascular disease: integrated post hoc analysis of the SELECT phase III rheumatoid arthritis clinical programme. Ann Rheum Dis 2023, 82, 1130–1141. [Google Scholar] [CrossRef] [PubMed]
- Hu, X.; Li, J.; Fu, M.; Zhao, X.; Wang, W. The JAK/STAT signaling pathway: From bench to clinic. Signal Transduct Target Ther 2021, 6, 402. [Google Scholar] [CrossRef] [PubMed]
- Raftery, N.; Stevenson, N.J. Advances in anti-viral immune defense: revealing the importance of the IFN JAK/STAT pathway. Cell Mol Life Sci 2017, 74, 2525–2535. [Google Scholar] [CrossRef] [PubMed]
- Aletaha, D.; Neogi, T.; Silman, A.J.; Funovits, J.; Felson, D.T.; Bingham, C.O. 3rd; Birnbaum, N.S.; Burmester, G.R.; Bykerk, V.P.; Cohen, M.D.; et al. 2010 rheumatoid arthritis classification criteria: an American College of Rheumatology/European League against Rheumatism collaborative initiative. Ann Rheum Dis 2010, 69, 1580–1588. [Google Scholar] [CrossRef]
- Prevoo, M.L.; van 't Hof, M.A.; Kuper, H.H.; van Leeuwen, M.A.; van de Putte, L.B.; van Riel, P.L. Modified disease activity scores that include twenty-eight-joint counts: development and validation in a prospective longitudinal study of patients with rheumatoid arthritis. Arthritis Rheum 1995, 38, 44–8. [Google Scholar] [CrossRef]
- Baxter, R.; Bartlett, J.; Fireman, B.; Marks, M.; Hansen, J.; Lewis, E.; Aukes, L.; Chen, Y.; Klein, N.P.; Saddier, P. Long-Term Effectiveness of the Live Zoster Vaccine in Preventing Shingles: A Cohort Study. Am J Epidemiol 2018, 187, 161–169. [Google Scholar] [CrossRef] [PubMed]
- Chen, P.K.; Liao, T.L.; Chang, S.H.; Yeo, K.J.; Chou, C.H.; Chen, D.Y. Anti-interferon-γ autoantibodies in patients with adult-onset Still’s diseases: association with opportunistic infections by inhibiting IFN-γ signaling chemokines. Front Med (Lausanne) 2023, 9, 1097514. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.; Chi, H.; Teng, J.; Meng, J.; Zhang, H.; Su, Y.; Liu, H.; Ye, J.; Shi, H.; Hu, Q.; et al. Neutralizing anti-IFN-γ IgG was increased in patients with systemic lupus erythematosus and associated with susceptibility to infection. Clin Rheumatol 2024, 43, 189–198. [Google Scholar] [CrossRef] [PubMed]
- Krisnawati, D.I.; Liu, Y.C.; Lee, Y.J.; Wang, Y.T.; Chen, C.L.; Tseng, P.C.; Lin, C.F. Functional neutralization of anti-IFN-gamma autoantibody in patients with non-tuberculous mycobacteria infection. Sci. Rep 2019, 9, 5682. [Google Scholar] [CrossRef]
- Lin, YG.; Gong, J.; Zhang, M.; Xue, W.; Barnes, P.F. Production of monocyte chemoattractant protein-1 in tuberculosis patients. Infect Immun 1998, 66, 2319–22. [Google Scholar] [CrossRef] [PubMed]
- Krisnawati, D.I.; Liu, Y.C.; Lee, Y.J.; Wang, Y.T.; Chen, C.L.; Tseng, P.C.; Shen, T.J.; Lin, C.F. Blockade effects of anti-interferon-(IFN-)γ autoantibody on IFN-γ-regulated antimicrobial immunity. J Immunol Res 2019, 2019, 162925. [Google Scholar] [CrossRef] [PubMed]
- Caruso, A.; Turano, A. Natural antibodies to interferon-γ. Biotherapy 1997, 10, 29–37. [Google Scholar] [CrossRef]
- Karin, N. Induction of protective therapy for autoimmune diseases by targeted DNA vaccines encoding pro-inflammatory cytokines and chemokines. Curr Opin Mol Ther 2004, 6, 27–33. [Google Scholar]
| Characteristics | RA with HZ (n=24) |
RA without HZ (n=42) |
p-value |
|---|---|---|---|
| Age at study entry, years | 58.7 ±7.3 | 59.2 ± 7.7 | 0.995 |
| Female, n (%) | 18 (75.0%) | 34 (81.0%) | 0.755 |
| RA disease duration, years | 5.9 ± 1.9 | 3.0 ± 1.8* | 0.020 |
| Prior HZ history, n (%) | 7 (29.2%) | 5 (11.9%) | 0.103 |
| Baseline ESR, mm/hr | 48.9 ± 25.5 | 49.7 ± 22.5 | 0.739 |
| Baseline C-reactive protein, mg/dL | 2.84 ± 3.05 | 2.93 ± 2.75 | 0.424 |
| Baseline DAS28 score | 6.01 ± 1.12 | 6.54 ± 0.84 | 0.053 |
| RF-positivity, n (%) | 18 (75.0%) | 33 (78.6%) | 0.767 |
| ACPA-positivity, n (%) | 19 (79.2%) | 29 (69.0%) | 0.767 |
| Concomitant steroids dose, mg/day | 5.85 ± 1.85 | 3.02 ± 1.81*** | <0.001 |
| Use of steroids≧5mg/day, n (%) | 21 (87.5%) | 4 (9.5%)*** | <0.001 |
| JAKi monotherapy, n (%) | 10 (41.7%) | 15 (37.5%) | 0.792 |
| Concomitant csDMARDs, n (%) | |||
| Methotrexate | 8 (33.3%) | 8 (19.0%) | 0.238 |
| Hydroxychloroquine | 6 (25.0%) | 19 (45.2%) | 0.121 |
| Leflunomide | 2 (8.3%) | 4 (9.5%) | 1.000 |
| The used JAKi | |||
| Tofacitinib, n (%) | 19 (38.0%) | 31 (62.0%) | NA |
| Baricitinib, n (%) | 1 (25.0%) | 3 (75.0%) | NA |
| Upadacitinib, n (%) | 4 (33.3%) | 8 (66.7%) | NA |
| Current smoker, n (%) | 5 (20.8%) | 4 (9.5%) | 0.268 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




