Submitted:
20 March 2024
Posted:
21 March 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methodology
2.1. Study Design, Setting, and Duration:
2.2. Study Population, Sample Selection Sampling Method
2.3. Description of Data Collection Instrument
2.4. Measurement of Study Outcome
2.5. Study Covariates
2.6. Statistical Analysis
2.7. Ethical Consideration
3. Results
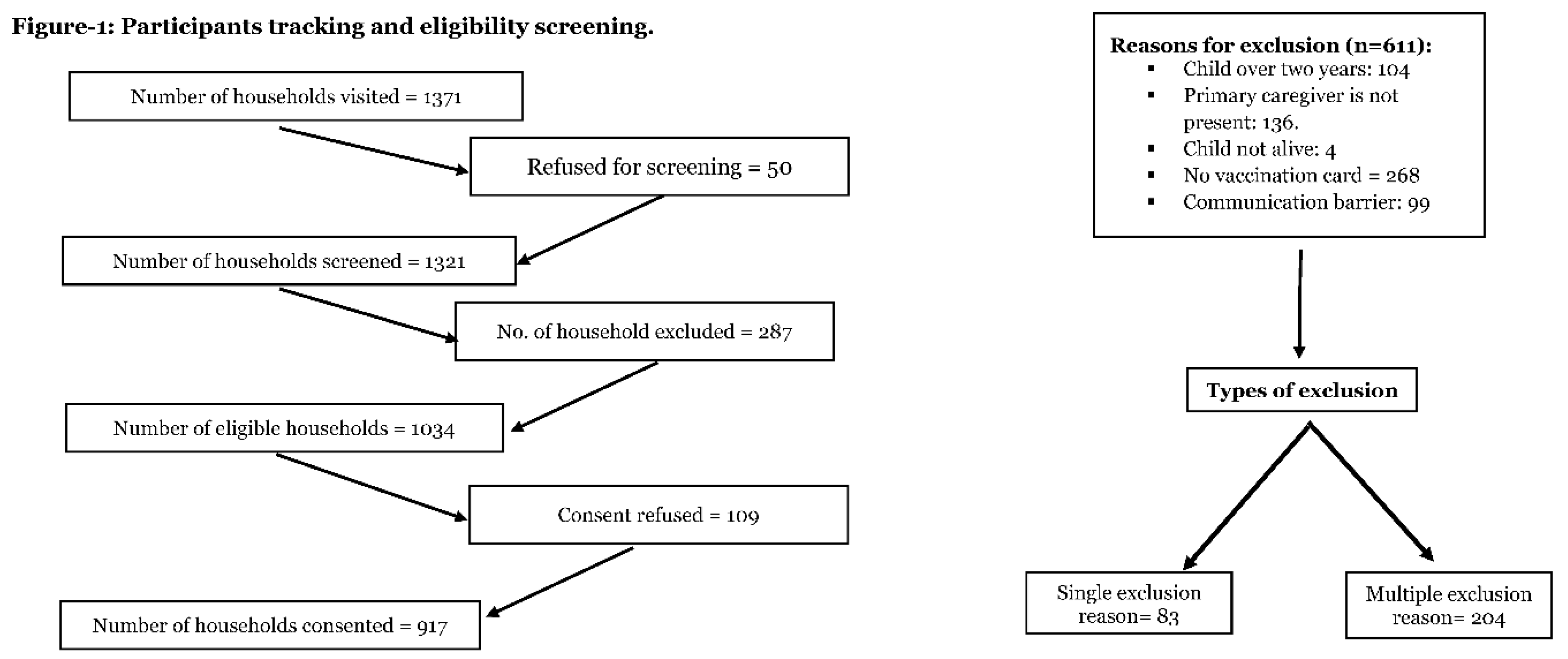
3.1. Screening, Eligibility, and Enrolment of Study Participants
3.2. Characteristics of Study Sample
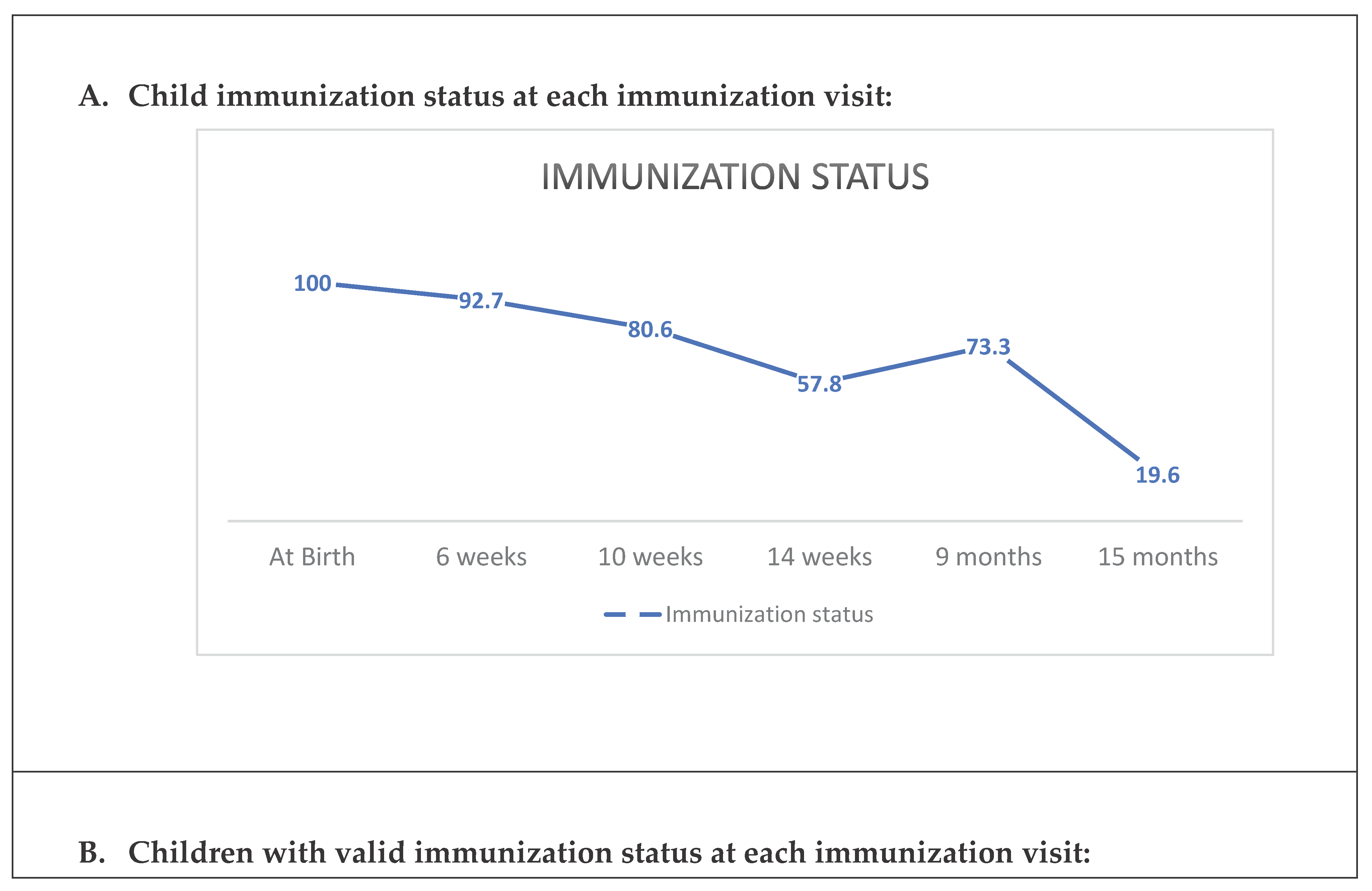
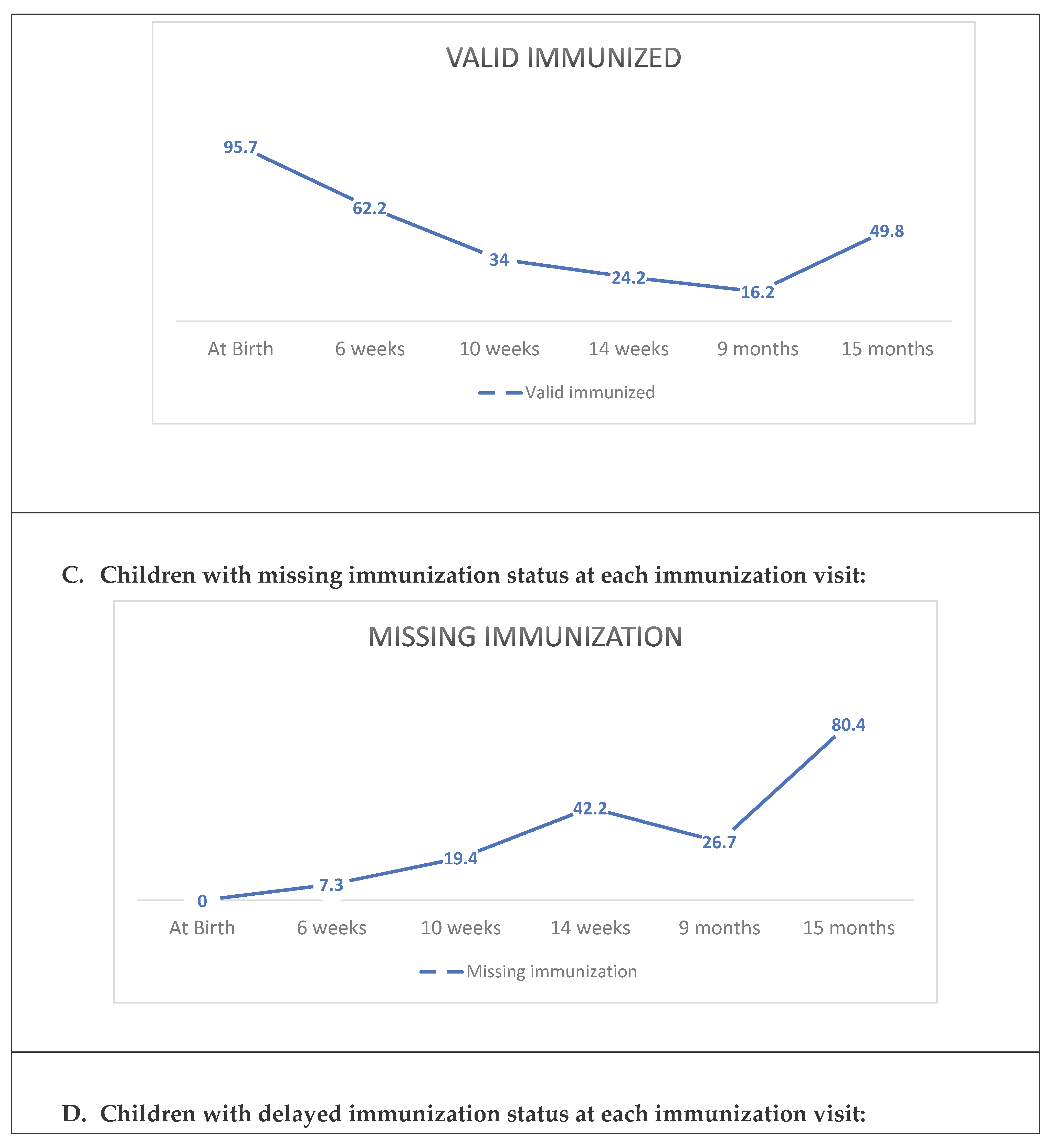
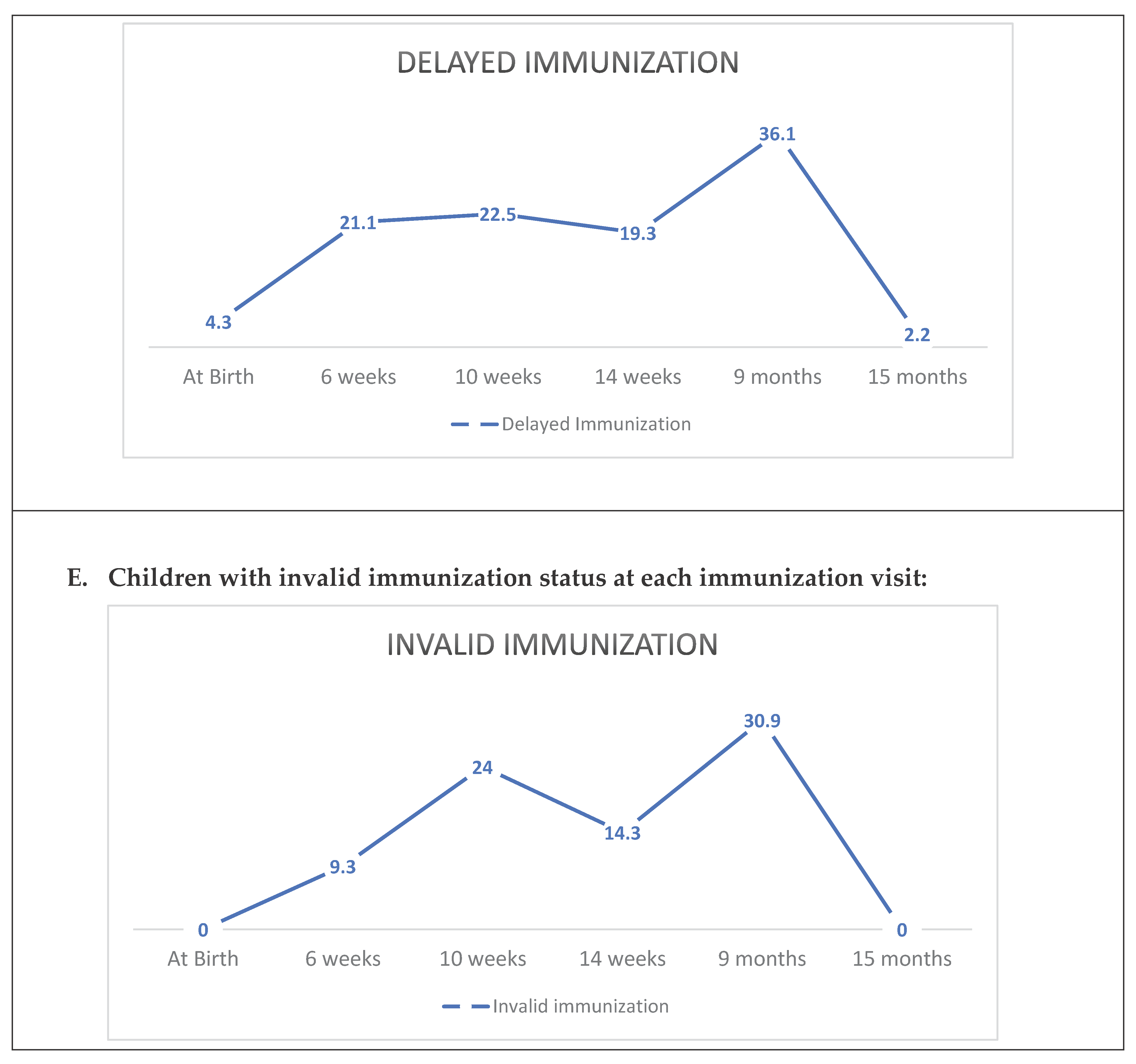
3.3. Infant Immunization Status for Different Immunization Visits
3.4. Determinants of Invalid, Delayed, and Missed Immunization
4. Discussion
4.1. Strengths and Limitations of the Study
4.2. Conclusion
Author’s contribution
Funding
Acknowledgments
Conflicts of Interest
References
- Kazi, A.M.; Ali, M. ; K A, Kalimuddin, H. ; Zubair, K.; Kazi, A.N.; et al. Geo-spatial reporting for monitoring of household immunization coverage through mobile phones: Findings from a feasibility study. International Journal of Medical Informatics. 2017, 107, 48–55. [Google Scholar] [CrossRef]
- Manandhar, K.; Bajcharya, K.; Prajapati, R.; Shrestha, N.C. Prevalence and Predictors of Incomplete Immunization among Children Residing in the Slums of Kathmandu Valley: A Community Based Door-to-Door Survey. Kathmandu Univ Med J (KUMJ). 2018, 16, 8–13. [Google Scholar]
- Khaliq, A.; Sayed, S.A.; Hussaini, S.A.; Azam, K.; Qamar, M. Missed immunization opportunities among children under 5 years of age dwelling In Karachi city. Journal of Ayub Medical College, Abbottabad: JAMC. 2017, 29, 645. [Google Scholar] [PubMed]
- World Health Organisation. Immunisation coverage - Key facts 2020 [updated 2020, th; cited 2023 October, 5th]. Available from: https://www.who.int/news-room/fact-sheets/detail/immunization-coverage. 15 July.
- Restrepo-Méndez, M.C.; Barros, A.J.; Wong, K.L.; Johnson, H.L.; Pariyo, G.; Wehrmeister, F.C.; et al. Missed opportunities in full immunization coverage: findings from low-and lower-middle-income countries. Global health action. 2016, 9, 30963. [Google Scholar] [CrossRef] [PubMed]
- Centres for Disease Control Prevention. Vaccine recommendations and guidelines of the ACIP: contraindications and precautions. 2017.
- Centres for Disease Control Prevention. Vaccine recommendations and guidelines of the ACIP 2015 [Available from: https://www.cdc.gov/vaccines/hcp/acip-recs/vacc-specific/rabies.html.
- Wariri, O.; Utazi, C.E.; Okomo, U.; Sogur, M.; Murray, K.A.; Grundy, C.; Fofanna, S.; Kampmann, B. Timeliness of routine childhood vaccination among 12–35 months old children in The Gambia: Analysis of national immunisation survey data, 2019–2020. PloS one. 2023, 18, e0288741. [Google Scholar] [CrossRef] [PubMed]
- MacDonald, S.E.; Russell, M.L.; Liu, X.C.; Simmonds, K.A.; Lorenzetti, D.L.; Sharpe, H.; Svenson, J.; Svenson, L.W. Are we speaking the same language? An argument for the consistent use of terminology and definitions for childhood vaccination indicators. Human vaccines & immunotherapeutic. 2019, 15, 740–747. [Google Scholar] [CrossRef]
- Guerra, F.A. Delays in immunization have potentially serious health consequences. Pediatric Drugs. 2007, 9, 143–148. [Google Scholar] [CrossRef] [PubMed]
- Lochlainn, L.M.; de Gier, B.; van der Maas, N.; van Binnendijk, R.; Strebel, P.M.; Goodman, T.; de Melker, H.E.; Moss, W.J.; Hahné, S.J. Effect of measles vaccination in infants younger than 9 months on the immune response to subsequent measles vaccine doses: a systematic review and meta-analysis. The Lancet Infectious Diseases. 2019, 19, 1246–1254. [Google Scholar] [CrossRef] [PubMed]
- Borras, E.; Urbiztondo, L.; Costa, J.; Batalla, J.; Torner, N.; Plasencia, A.; Salleras, L.; Dominguez, A. ; Working Group for the Study of Measles Immunity in Children. Measles antibodies and response to vaccination in children aged less than 14 months: implications for age of vaccination. Epidemiology & Infection. 2012, 140, 1599–1606. [Google Scholar] [CrossRef]
- National Institute of Population Studies, N.P. ; Icf. Pakistan Demographic and Health Survey 2017-18. Islamabad, Pakistan: NIPS/Pakistan and ICF; 2019.
- Magambo, N.K.; Bajunirwe, F.; Bagenda, F. Geographic location of health facility and immunization program performance in Hoima district, western Uganda: a health facility level assessment. BMC Public Health. 2020, 20, 1–0. [Google Scholar] [CrossRef]
- Freeman, R.E.; Leary, C.S.; Graham, J.M.; Albers, A.N.; Wehner, B.K.; Daley, M.F.; Newcomer, S.R. Geographic proximity to immunization providers and vaccine series completion among children ages 0–24 months. Vaccine. 2023, 41, 2773–2780. [Google Scholar] [CrossRef]
- Siddique, M.; Iftikhar, S.; Dharma, V.K.; Shah, M.T.; Siddiqi, D.A.; Malik, A.A.; Chandir, S. Using geographic information system to track children and optimize immunization coverage and equity in Karachi, Pakistan. Vaccine. 2023, 41, 2922–2931. [Google Scholar] [CrossRef]
- Khaliq, A.; Elahi, A.A.; Zahid, A.; Lassi, Z.S. A survey exploring reasons behind immunization refusal among the parents and caregivers of children under two years living in urban slums of Karachi, Pakistan. International Journal of Environmental Research and Public Health. 2022, 19, 11631. [Google Scholar] [CrossRef]
- Khan, I.M.; Amber, W.; Chishti, A.L.; Hassan, K.A. Assessment of Complete Coverage of Expanded Program on Immunization in Children at Mayo Hospital Lahore, Pakistan. Journal of Islamabad Medical & Dental College. 2020, 9, 12–16. [Google Scholar] [CrossRef]
- Crocker-Buque, T.; Mindra, G.; Duncan, R.; Mounier-Jack, S. Immunization, urbanization, and slums – a systematic review of factors and interventions. BMC Public Health. 2017, 17, 556. [Google Scholar] [CrossRef] [PubMed]
- United Nation International Children's Fund. Pakistan: Key Demographic Indicators [Available from: Retrieved from: https://data.unicef.org/country/pak/ (last accessed on: , 2023). 7 March.
- Khaliq, A. ; Amreen, Jameel, N. ; Krauth, S.J. Knowledge and practices on the prevention and management of diarrhea in children under-2 years among women dwelling in urban slums of Karachi, Pakistan. Maternal and child health journal. 2022, 26, 1442–1452. [Google Scholar] [CrossRef] [PubMed]
- Shams, Z.I.; Shahid, M.; Nadeem, Z.; Naz, S.; Raheel, D.; Aftab, D.; et al. Town socio-economic status and road width determine street tree density and diversity in Karachi, Pakistan. Urban For Urban Green [Internet]. 2020, 47, 126473. [Google Scholar] [CrossRef]
- Henderson, R.H.; Sundaresan, T. Cluster sampling to assess immunization coverage: A review of experience with a simplified sampling method. Bull World Health Organ. 1982, 60, 253–260. [Google Scholar] [PubMed]
- World Health Organization. Immunization coverage cluster survey, reference manual. 2005.
- Centers for disease control and Prevention. Contraindications and Precautions [Internet]. 2023. Available from: https://www.cdc.gov/vaccines/hcp/acip-recs/general-recs/contraindications.pdf.
- Riaz, A.; Husain, S.; Yousafzai, M.T.; Nisar, I.; Shaheen, F.; Mahesar, W.; et al. Reasons for non-vaccination and incomplete vaccinations among children in Pakistan. Vaccine. 2018, 36, 5288–5293. [Google Scholar] [CrossRef] [PubMed]
- Khowaja, A.R.; Zaman, U.; Feroze, A.; Rizvi, A.; Zaidi, A.K. Routine EPI coverage: subdistrict inequalities and reasons for immunization failure in a rural setting in Pakistan. Asia pacific journal of public health. 2015, 27, NP1050–NP9. [Google Scholar] [CrossRef] [PubMed]
- Qazi, U.; Malik, S.; Raza, U.A.; Saad, M.; Zeeshan, M.F.; Anwar, S. Compliance to timely vaccination in an Expanded Program on Immunization center of Pakistan. Vaccine. 2019, 37, 4618–4622. [Google Scholar] [CrossRef] [PubMed]
- Loulergue, P.; Pulcini, C.; Massin, S.; Bernhard, M.; Fonteneau, L.; Levy-Br€uhl, D.; Guthmann, J.P.; Launay, O. Validity of self-reported vaccination status among French healthcare students. Clinical Microbiology and Infection. 2014, 20, O1152–O1154. [Google Scholar] [CrossRef] [PubMed]
- Smith, L.E.; Amlôt, R.; Weinman, J. ; Yiend Jenny, Rubin, G. J. systematic review of factors affecting vaccine uptake in young children. Vaccine. 2017, 35, 6059–6069. [Google Scholar]
- Belt, R.V. ; Abdullah S, Mounier-Jack, S. ; Sodha, S.V.; Danielson, N.; Dadari I, Olayinka, F.; Ray, A.; Crocker-Buque, T. Improving Equity in Urban Immunization in Low- and Middle-Income Countries: A Qualitative Document Review. Vaccines. 2023, 11, 1200. [Google Scholar] [CrossRef]
- Dirirsa, K.; Makuria, M.; Mulu, E.; Deriba, B.S. Assessment of vaccination timeliness and associated factors among children in Toke Kutaye district, central Ethiopia: A Mixed study. Plos One. 2022, 17, e0262320. [Google Scholar] [CrossRef]
- Alghofaili M A, Aljuaid, S. O.; Alqahtani, N.; Alghufaili, M.; Abd-Ellatif, E.E. Factors Contributing to the Delayed Vaccination Among Children in Riyadh City, Saudi Arabia: A Cross-Sectional Study. Cureus. 2023, 15, e43188. [CrossRef]
- Alnumair, A.; Almulifi, A. Perceptions toward childhood vaccinations (side effects vs. benefits) among the parents living in Hail, Saudi Arabia. J Family Med Prim Care 2022, 11, 6285–6290. [Google Scholar] [CrossRef]
- Matta, P.; Mouallem, R.E.; Akel, M.; Hallit, S.; Khalife, M.F. Parents’ knowledge, attitude and practice towards children’s vaccination in Lebanon: role of the parent-physician communication.2000, 20, 1439.
| Visit number | Recommended age of immunization |
|---|---|
| Visit-1 | At birth |
| Visit-2 | 6 weeks |
| Visit-3 | 10 weeks |
| Visit-4 | 14 weeks |
| Visit-5 | 9 months |
| Visit-6 | 15 onths |
| Variable | Categories | Total | Valid | Invalid | Delayed | Missed |
|---|---|---|---|---|---|---|
| Child factors | ||||||
| Child sex | Male | 450 (49.1%) | 229 (50.1%) | 52 (47.2%) | 89 (53.9%) | 80 (43.2%) |
| Female | 467 (50.9%) | 228 (49.8%) | 58 (52.7%) | 76 (46.1%) | 105 (56.7%) | |
| Birth order | 4.00±1.82 | 3.80±1.79 | 4.12±1.84 | 4.12±1.83 | 4.34±1.81 | |
| Maternal demographic factors | ||||||
| Maternal age | 29.6±6.17 | 29.2±6.23 | 28.8±6.01 | 30.1±6.24 | 30.5±5.93 | |
| Maternal education | 4.42±2.29 | 4.84±2.27 | 4.43±2.25 | 4.31±2.26 | 3.49±2.11 | |
| Paternal demographic factors | ||||||
| Paternal age | 34.3±5.49 | 34.0±5.35 | 34.3±4.90 | 34.5±5.68 | 35.1±5.92 | |
| Paternal education | 3.84±2.46 | 4.25±2.57 | 3.45±2.15 | 3.73±2.39 | 3.17±2.24 | |
| Household factors | ||||||
| Number of children delivered | 3.81±1.65 | 3.63±1.65 | 3.82±1.69 | 3.87±1.65 | 4.21±1.53 | |
| Total family size | 7.00±1.74 | 6.86±1.72 | 7.17±1.78 | 7.03±1.77 | 7.22±1.69 | |
| Place of childbirth | Hospital | 460 (50.2%) | 271 (59.2%) | 59 (53.6%) | 73 (44.2%) | 57 (30.8%) |
| Maternity centre | 446 (48.6%) | 183 (40.1%) | 50 (45.4%) | 90 (54.5%) | 123 (66.5%) | |
| Home | 11 (1.2%) | 3 (0.7%) | 1 (0.9%) | 2 (1.2%) | 5 (2.7%) | |
| Immunization knowledge and practices | ||||||
| Correct knowledge of vaccination centre visit in the first year | Yes | 498 (54.3%) | 282 (61.7%) | 69 (62.7%) | 89 (53.9%) | 58 (31.3%) |
| Correct knowledge of vaccination centre visit in the second year | Yes | 241 (26.3%) | 137 (29.9%) | 34 (30.9%) | 49 (29.6%) | 21 (11.3%) |
| Vaccination visit | First visit | 210 (22.9%) | 201 (43.9%) | 0 (0%) | 9 (5.4%) | 0 (0%) |
| Second visit | 204 (22.2%) | 127 (27.7%) | 19 (17.2%) | 43 (26.1%) | 15 (8.1%) | |
| Third visit | 191 (20.8%) | 65 (14.2%) | 46 (41.8%) | 43 (26.1%) | 37 (20%) | |
| Fourth visit | 161 (17.6%) | 39 (8.5%) | 23 (20.9%) | 31 (18.8%) | 68 (36.8%) | |
| Fifth visit | 105 (11.5%) | 17 (3.7%) | 22 (20%) | 38 (23%) | 28 (15.1%) | |
| Sixth visit | 46 (5%) | 8 (1.8%) | 0 (0%) | 1 (0.6%) | 37 (20%) | |
| Total | 917 (100%) | 457 (49.8%) | 110 (11.9%) | 165 (17.9%) | 185 (20.1%) | |
| Reasons for invalid, missed, and delayed immunization | ||||||
| Vaccination centre outside catchment area | Yes | 429 (47.2%) | 204 (44.6%) | 48 (43.6%) | 85 (51.5%) | 92 (49.7%) |
| Family decision maker is against immunization | Yes | 534 (58.7%) | 305 (66.7%) | 70 (63.6%) | 95 (57.6%) | 64 (34.6%) |
| Unavailability of vaccine in the vaccination centre | Yes | 495(54.5%) | 266(58.2%) | 61(55.4%) | 92(55.8%) | 76(41.1%) |
| Migration of family | Yes | 200 (22%) | 362 (79.2%) | 84 (73.6%) | 129 78.2%) | 134 (72.4%) |
| Cost of vaccine | Yes | 111 (12.2%) | 408 (89.3%) | 98 (89%) | 140 (84.8%) | 152 (82.2%) |
| Vaccine related side-effects | Yes | 432 (47.5%) | 264 (57.8%) | 55 (50%) | 78 (47.3%) | 80 (43.2%) |
| Child was sick | Yes | 555 (61.1%) | 298 (65.2%) | 75 (68.1%) | 103 (62.4%) | 79 (42.7%) |
| Doctor advised not to vaccinate | Yes | 263 (28.9%) | 369 (80.7%) | 81 (73.6%) | 111 (67.3%) | 85(45.9%) |
| Lack of knowledge about vaccination schedule | Yes | 648 (71.3%) | 145 (31.7%) | 14 (12.7%) | 44 (26.7%) | 58 (31.4%) |
| Lack of trust on Government | Yes | 271 (29.8%) | 103 (22.5%) | 83 (75.4%) | 103 (62.4%) | 93 (50.3%) |
| Too many vaccines traumatise the children | Yes | 392 (43.4%) | 238 (52.1%) | 61 (55.4%) | 102 (61.8%) | 0%) |
| Variable | Categories | Invalid | Delayed | Missed | |||
|---|---|---|---|---|---|---|---|
| Unadjusted | Adjusted | Unadjusted | Adjusted | Unadjusted | Adjusted | ||
| Child sex | Male | 0.89 (0.58 to 1.35) | - | 1.16 (0.81 to 1.66) | - | 0.75 (0.53 to 1.07) | - |
| Female | Ref | Ref | Ref | ||||
| Birth order | 1.10 (0.98 to 1.23) | - | 1.10 (0.99 to 1.21) | - | 1.18 (1.07 to 1.29) * | - | |
| Maternal age | 0.98 (0.95 to 1.02) | - | 1.02 (0.99 to 1.05) | - | 1.03 (1.00 to 1.06) | - | |
| Maternal education | 0.92 (0.84 to 1.01) | - | 0.90 (0.83 to 0.97) * | - | 0.75 (0.69 to 0.82) * | - | |
| Paternal age | 1.01 (0.97 to 1.04) | - | 1.02 (0.98 to 1.05) | - | 1.03 (1.00 to 1.07) * | - | |
| Paternal education | 0.87 (0.79 to 0.95) * | 0.81 (0.72 to 0.91) * | 0.91 (0.85 to 0.98) * | 0.90 (0.83 to 0.99) * | 0.82 (0.76 to 0.89) * | 0.81 (0.73 to 0.91) * | |
| Number of children delivered | 1.07 (0.94 to 1.22) | - | 1.09 (0.98 to 1.22) | - | 1.24 (1.12 to 1.39) * | - | |
| Total family size | 1.11 (0.98 to 1.25) | 1.05 (0.95 to 1.17) | 1.12 (1.02 to 1.24) * | ||||
| Place of childbirth | Hospital | Ref | - | Ref | - | Ref | - |
| Maternity centre | 1.25 (0.82 to 1.91) | 1.82 (1.27 to 2.62) * | 3.19 (2.21 to 4.60) * | ||||
| Home | 1.53 (0.15 to 14.97) | 2.47 (0.40 to 15.09) | 7.92 (1.84 to 34.10) * | ||||
| Correct knowledge of vaccination centre visit in the first year | Yes | Ref | Ref | Ref | Ref | Ref | Ref |
| No | 0.95 (0.62 to 1.47) | 0.99 (0.58 to 1.66) | 1.37 (0.96 to 1.97) | 1.20 (0.76 to 1.88) | 3.52 (2.45 to 5.07) * | 3.09 (1.80 to 5.31) * | |
| Correct knowledge of vaccination centre visit in the second year | Yes | Ref | - | Ref | - | Ref | - |
| No | 0.95 (0.60 to 1.50) | 1.01 (0.68 to 1.49) | 3.34 (2.03 to 5.49) * | ||||
| Vaccination visit | 2.38 (1.99 to 2.84) * | 2.73 (2.24 to 3.33) * | 2.20 (1.89 to 2.57) * | 2.59 (2.17 to 3.09) * | 3.67 (3.08 to 4.38) * | 5.51 (4.39 to 6.91) * | |
| Vaccination centre in catchment area | Yes | 0.94 (0.62 to 1.43) | - | 1.31 (0.91 to 1.87) | - | 1.24 (0.88 to 1.76) | - |
| No | Ref | Ref | Ref | ||||
| Family decision maker is against immunization | Yes | 1.17 (0.76 to 1.82) | - | 1.49 (1.03 to 2.16) * | - | 3.80 (2.64 to 5.45) * | - |
| No | Ref | Ref | Ref | ||||
| Vaccine availability issues | Yes | 1.14 (0.75 to 1.73) | 0.60 (0.36 to 0.99) * | 1.11 (0.77 to 1.59) | 0.82 (0.52 to 1.28) | 1.98 (1.40 to 2.81) * | 0.43 (0.25 to 0.73) * |
| No | Ref | Ref | Ref | Ref | Ref | Ref | |
| Migration of family | Yes | 1.23 (0.75 to 2.02) | - | 1.07 (0.69 to 1.67) | - | 1.42 (0.95 to 2.13) | - |
| No | Ref | Ref | Ref | ||||
| Cost of vaccine | Yes | 1.11 (0.56 to 2.17) | - | 1.55 (0.91 to 2.64) | - | 1.78 (1.08 to 2.94) * | - |
| No | Ref | Ref | Ref | ||||
| Vaccine related side-effects | Yes | 1.39 (0.92 to 2.12) | - | 1.54 (1.07 to 2.20) | - | 0.20 (0.15 to 0.27) * | - |
| No | Ref | Ref | Ref | ||||
| Child was sick | Yes | 0.89 (0.57 to 1.40) | - | 1.13 (0.78 to 1.65) | - | 2.50 (1.76 to 3.56) * | - |
| No | Ref | Ref | Ref | ||||
| Doctor advised not to vaccinate | Yes | 1.57 (0.96 to 2.55) | 1.40 (0.70 to 2.82) | 2.09 (1.40 to 3.14) * | 1.54 (0.85 to 2.79) | 5.01 (3.44 to 7.29) * | 2.73 (1.41 to 5.30) * |
| No | Ref | Ref | Ref | Ref | Ref | Ref | |
| Lack of knowledge about vaccination schedule | Yes | 3.22 (1.78 to 5.85) * | 4.00 (2.05 to 7.83) * | 1.28 (0.86 to 1.91) | 1.80 (1.11 to 2.91) * | 1.00 (0.69 to 1.45) | 1.86 (1.05 to 3.30) * |
| No | Ref | Ref | Ref | Ref | Ref | Ref | |
| Lack of trust on Government | Yes | 1.24 (0.76 to 2.02) | 1.89 (0.95 to 3.76) | 2.26 (1.53 to 3.34) * | 3.11 (1.76 to 5.49) * | 3.65 (2.52 to 5.28) * | 3.53 (1.84 to 6.78) * |
| No | Ref | Ref | Ref | Ref | Ref | Ref | |
| Too many vaccines traumatise the children | Yes | 0.87 (0.57 to 1.33) | - | 0.66 (0.46 to 0.96) * | - | 0.70 (0.49 to 1.00) | - |
| No | Ref | Ref | Ref | ||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




