Submitted:
16 January 2024
Posted:
17 January 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Evolution of Definition of Early Chronic Pancreatitis (CP):
3. Risk Factors for Early CP
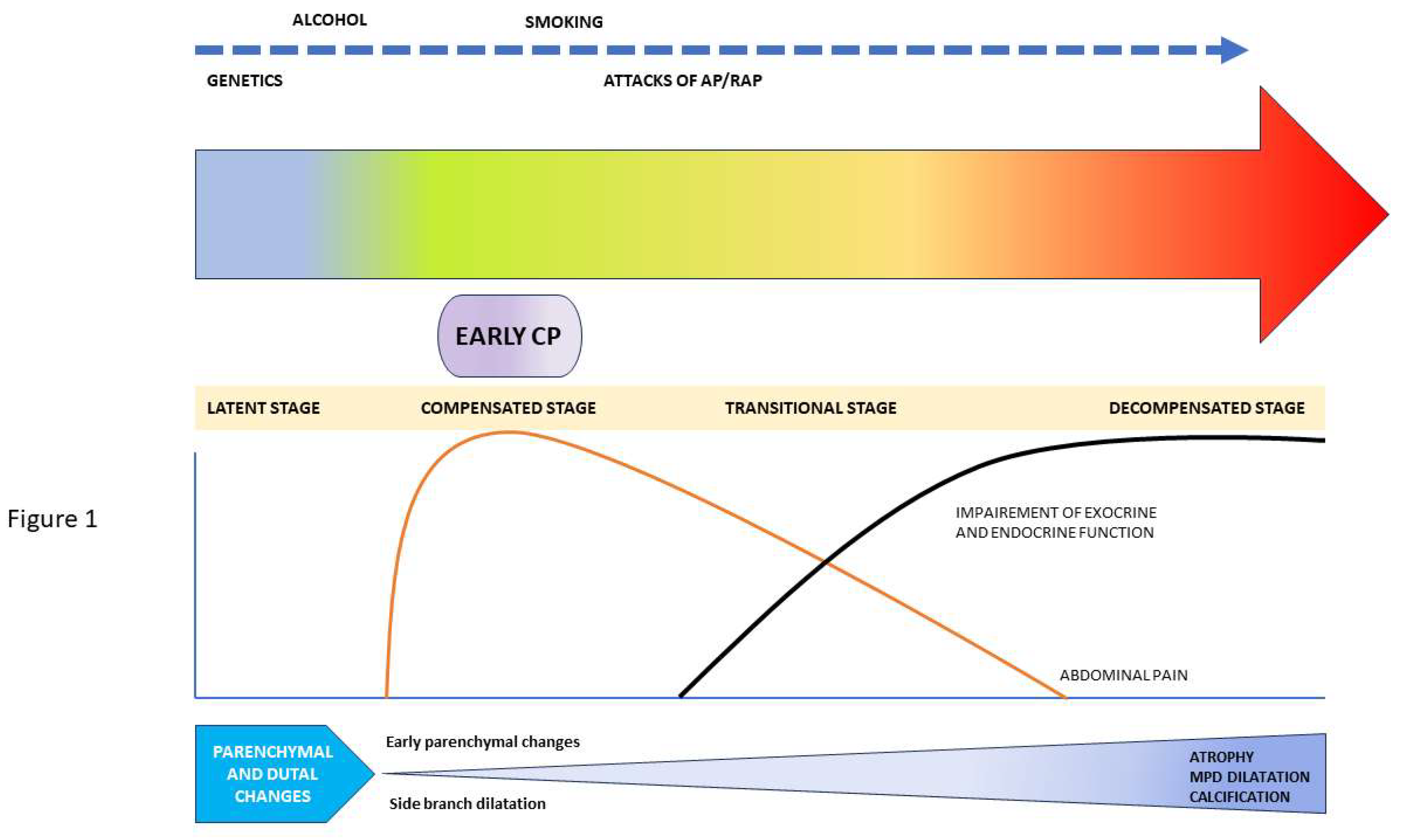
4. Natural History and Progression
5. Role of Imaging in ECP: A Diagnostic Conundrum
6. EUS in Early CP:
A. EUS Features of Early CP:
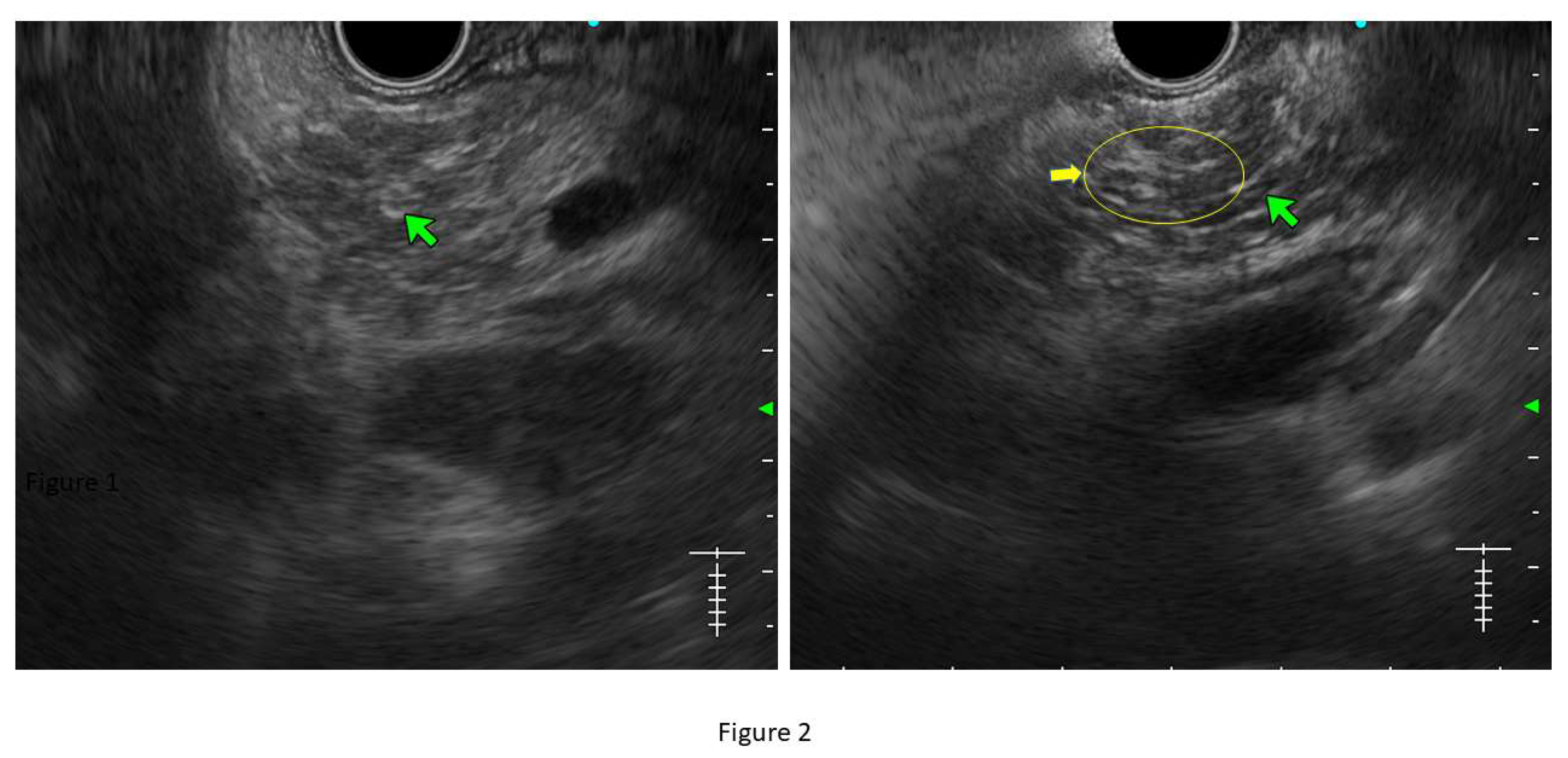
- Lobularity with and without honeycombing: Lobules are described as well-circumscribed reticulated areas ≥5 mm in size, with a relatively hyperechoic rim compared to the adjacent central area. When these lobules are non-contiguous, the EUS pattern is described as ‘lobularity without honeycombing.’ When at least 3 of such lobules are contiguously located in the body or tail region, the pattern is defined as ‘lobularity with honeycombing’ in EUS. (32,33) (Figure 2) The exact histopathological correlation of lobularity is not precisely known. Studies however, have demonstrated lobularity to correlate with increased fat and collagen in biopsy specimens, and in a recent study, lobularity was demonstrated to be associated with increased disease severity, higher level of inflammation, and a trend towards higher grade of fibrosis and atrophy compared to absence of lobularity on EUS. (34,35)
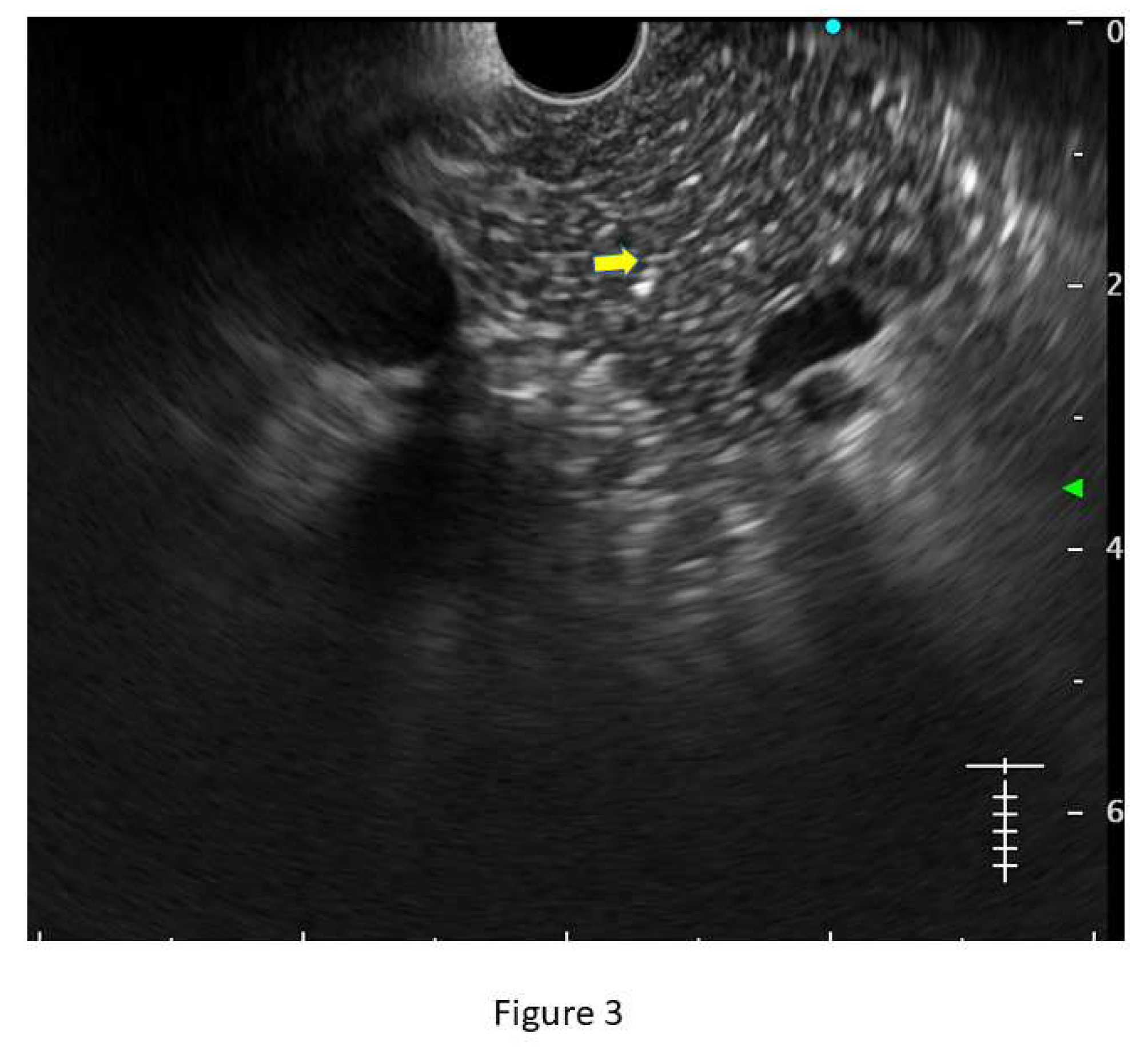
- Hyperechoic foci without shadowing: Echogenic structures of ≥3mm in length and width without any posterior acoustic shadowing are defined as ‘hyperechoic foci without shadowing’ in the JPS definition. In standard definition, it is included under ‘hyperechoic foci.’ At least 3 such foci need to be present to be described as abnormal. The presence of acoustic shadowing signifies calcification. Histologically, they correspond to focal fibrosis. (Figure 3)
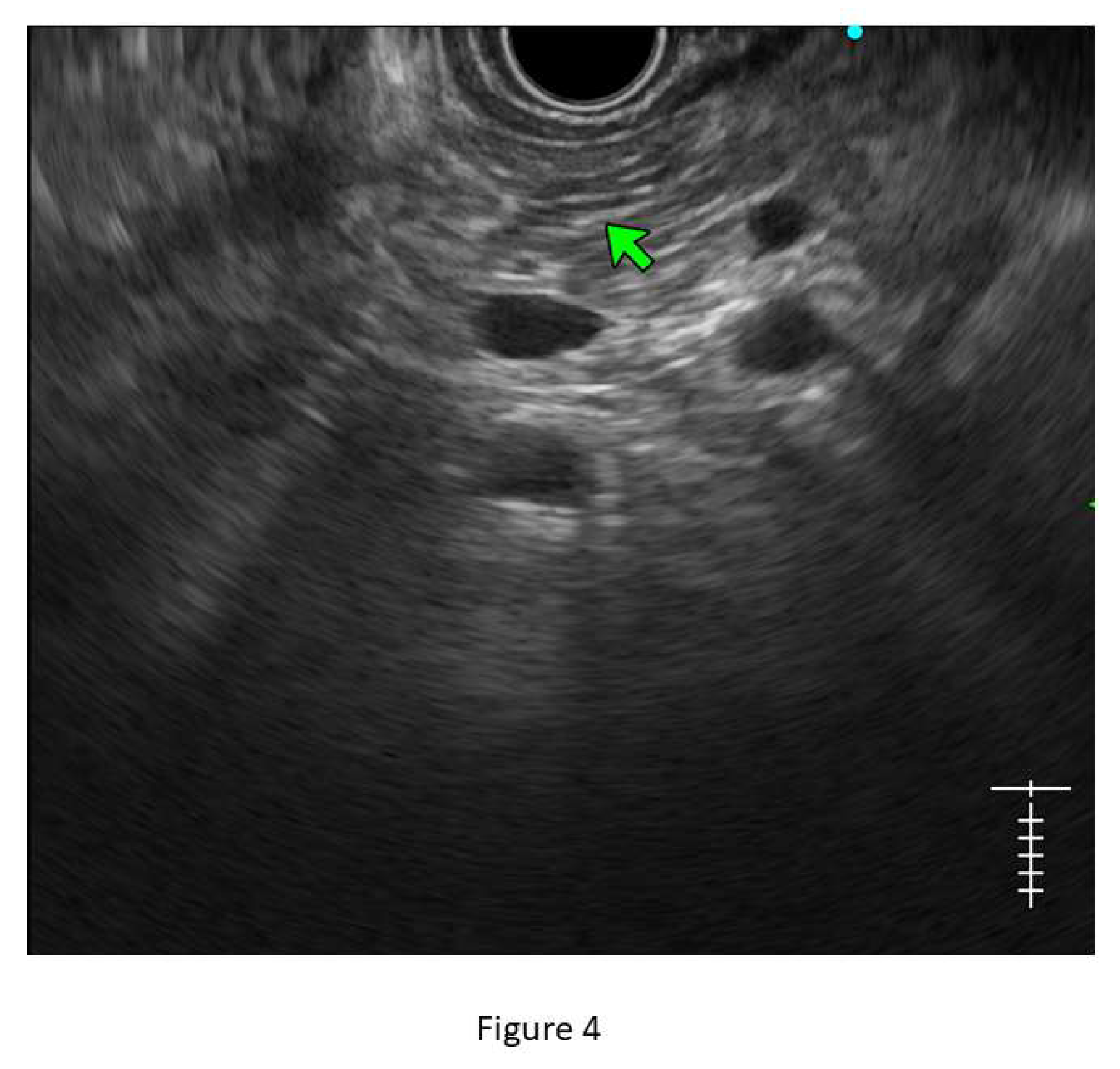
- Stranding: The presence of hyperechoic lines of ≥3 mm length in a minimum of two directions concerning the plane of imaging is described as ‘stranding’ in JPS criteria (in standard criteria, it is described as hyperechoic foci with stranding). Abnormal stranding is described when at least 3 such lines are noted. Stranding corresponds to bridging parenchymal fibrosis in histopathology. (Figure 4)
- Cysts: In EUS, they are described as Anechoic structures, with/ without septations, round or elliptical in shape, measuring ≥2 mm in short axis. Histologically, they correspond to pseudocysts or retention cysts.
- Dilatation of the side branches: It is defined as the presence of ≥3 anechoic, tubular structures communicating with the MPD, each ≥1 mm in width demonstrable in the body and tail region. Histologically, they correspond to the narrowing of the branch ducts due to micro-fibrosis.
- Hyperechoic margin of the MPD: It is described when hyperechoic ductal wall over at least 50% of the MPD is demonstrated in the body and tail of pancreas. In a linear echoendoscope, MPD assessment on a long axis is difficult. Thus, this finding is often subjective and has low interobserver agreement. (36) Histologically, they correspond to periductal fibrosis. In the study by Sekine et al, the hyperechoic MPD wall was described to correlate with thinning of the ductal wall on surgical specimens. (35) (Figure 2)
B. Correlation between EUS Findings and Histology:
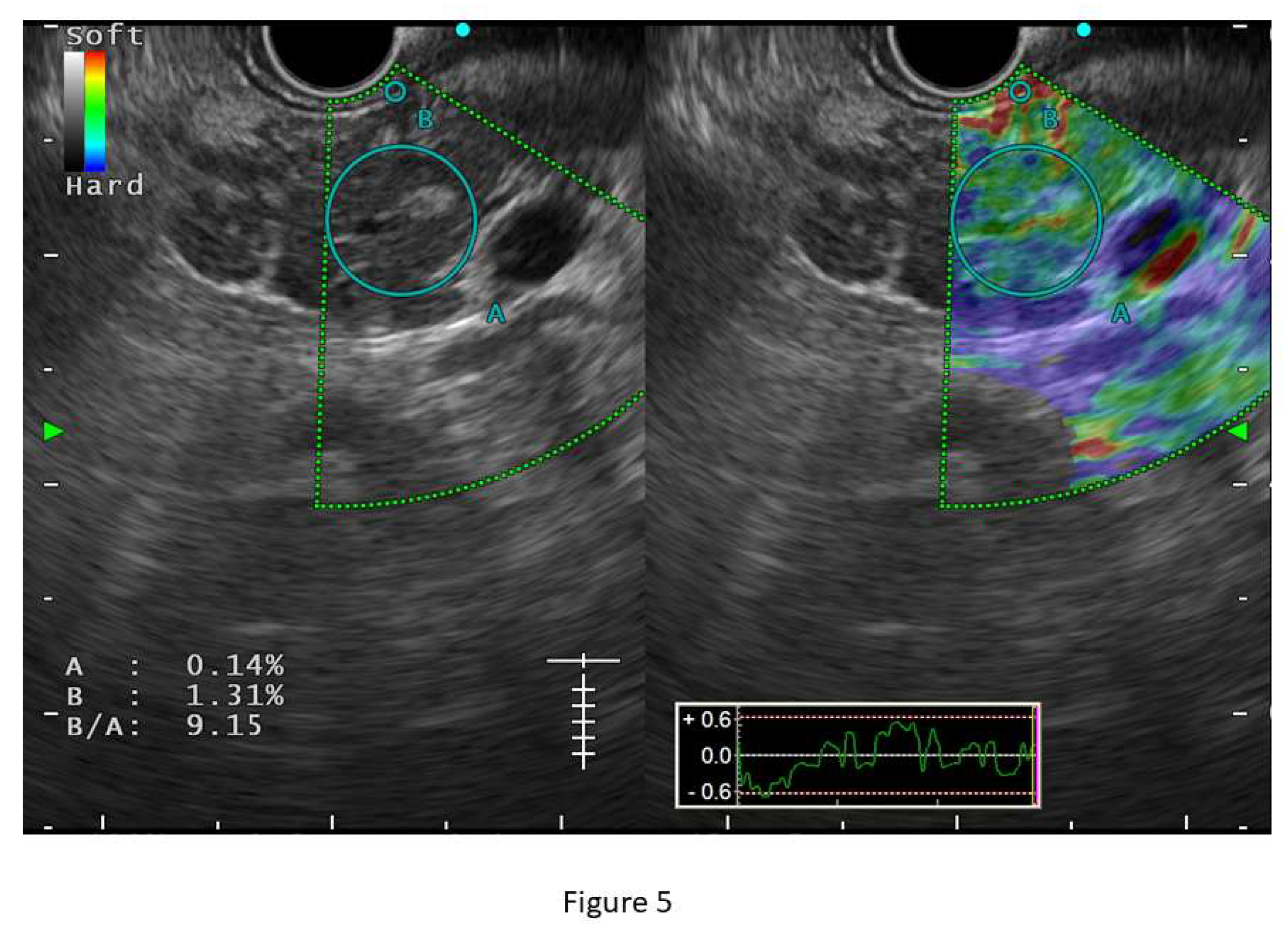
C. Role of EUS Elastography in Early CP:
7. Future Directions in Diagnosis of ECP
References
- Talamini G, Falconi M, Bassi C, Sartori N, Salvia R, Caldiron E, et al. Incidence of Cancer in The Course of Chronic Pancreatitis. American Journal of Gastroenterology. 1999 May;94(5):1253-60. [CrossRef]
- Malka D, Hammel P, Maire F, Rufat P, Madeira I, Pessione F, et al. Risk of pancreatic adenocarcinoma in chronic pancreatitis. Gut. 2002 Dec;51(6):849-52. [CrossRef]
- Shimosegawa T, Kataoka K, Kamisawa T, Miyakawa H, Ohara H, Ito T, et al. The revised Japanese clinical diagnostic criteria for chronic pancreatitis. Vol. 45, Journal of Gastroenterology. 2010. p. 584-91. [CrossRef]
- Yoshida M, Kinoshita Y, Watanabe M, Sugano K. JSGE Clinical Practice Guidelines 2014: standards, methods, and process of developing the guidelines. Vol. 50, Journal of Gastroenterology. Springer Japan; 2015. p. 4-10. [CrossRef]
- Ammann RW, Muellhaupt B, Meyenberger C, Heitz PU. Alcoholic nonprogressive chronic pancreatitis: prospective long-term study of a large cohort with alcoholic acute pancreatitis (1976-1992). Pancreas. 1994 May;9(3):365-73. [CrossRef]
- Whitcomb DC, Shimosegawa T, Chari ST, Forsmark CE, Frulloni L, Garg P, et al. International consensus statements on early chronic Pancreatitis. Recommendations from the working group for the international consensus guidelines for chronic pancreatitis in collaboration with The International Association of Pancreatology, American Pancreatic Association, Japan Pancreas Society, PancreasFest Working Group and European Pancreatic Club. Pancreatology. 2018 Jul 1;18(5):516-27. [CrossRef]
- Catalano MF, Sahai A, Levy M, Romagnuolo J, Wiersema M, Brugge W, et al. EUS-based criteria for the diagnosis of chronic pancreatitis: the Rosemont classification. Gastrointest Endosc. 2009 Jun;69(7):1251-61. [CrossRef]
- Albashir S, Bronner MP, Parsi MA, Walsh RM, Stevens T. Endoscopic ultrasound, secretin endoscopic pancreatic function test, and histology: Correlation in chronic pancreatitis. American Journal of Gastroenterology. 2010 Nov;105(11):2498-503. [CrossRef]
- Varadarajulu S, Eltoum I, Tamhane A, Eloubeidi MA. Histopathologic correlates of noncalcific chronic pancreatitis by EUS: a prospective tissue characterization study. Gastrointest Endosc. 2007 Sep;66(3):501-9. [CrossRef]
- Shimosegawa T, Kataoka K, Kamisawa T, Miyakawa H, Ohara H, Ito T, et al. The revised Japanese clinical diagnostic criteria for chronic pancreatitis. Vol. 45, Journal of Gastroenterology. 2010. p. 584-91. [CrossRef]
- Hegyi PJ, Soós A, Tóth E, Ébert A, Venglovecz V, Márta K, et al. Evidence for diagnosis of early chronic pancreatitis after three episodes of acute pancreatitis: a cross-sectional multicentre international study with experimental animal model. Sci Rep. 2021 Dec 1;11(1). [CrossRef]
- Lankisch PG, Breuer N, Bruns A, Weber-Dany B, Lowenfels AB, Maisonneuve P. Natural history of acute pancreatitis: A long-term population-based study. American Journal of Gastroenterology. 2009 Nov;104(11):2797-805. [CrossRef]
- Yadav, D. Alcohol Consumption, Cigarette Smoking, and the Risk of Recurrent Acute and Chronic Pancreatitis. Arch Intern Med. 2009 Jun 8;169(11):1035. [CrossRef]
- Bhutani MS, Arantes VN, Verma D, Moezzi J, Suryaprasad S, Kapadia AS, et al. Histopathologic Correlation of Endoscopic Ultrasound Findings of Chronic Pancreatitis in Human Autopsies. Pancreas. 2009 Oct;38(7):820-4. [CrossRef]
- Yusoff IF, Raymond G, Sahai A V. A prospective comparison of the yield of EUS in primary vs. recurrent idiopathic acute pancreatitis. Gastrointest Endosc. 2004 Nov;60(5):673-8. [CrossRef]
- Takeyama, Y. Long-Term Prognosis of Acute Pancreatitis in Japan. Clinical Gastroenterology and Hepatology. 2009 Nov;7(11 SUPPL.). [CrossRef]
- Petrone MC, Arcidiacono PG, Perri F, Carrara S, Boemo C, Testoni PA. Chronic pancreatitis-like changes detected by endoscopic ultrasound in subjects without signs of pancreatic disease: Do these indicate age-related changes, effects of xenobiotics, or early chronic pancreatitis? Pancreatology. 2010;10(5):597-602. [CrossRef]
- Masamune A, Kikuta K, Nabeshima T, Nakano E, Hirota M, Kanno A, et al. Nationwide epidemiological survey of early chronic pancreatitis in Japan. J Gastroenterol. 2017 Aug 1;52(8):992-1000. [CrossRef]
- Masamune A, Kikuta K, Kume K, Hamada S, Tsuji I, Takeyama Y, et al. Nationwide epidemiological survey of chronic pancreatitis in Japan: introduction and validation of the new Japanese diagnostic criteria 2019. J Gastroenterol. 2020 Nov 1;55(11):1062-71.
- Sheel ARG, Baron RD, Sarantitis I, Ramesh J, Ghaneh P, Raraty MGT, et al. The diagnostic value of Rosemont and Japanese diagnostic criteria for 'indeterminate' 'suggestive' 'possible' and 'early' chronic pancreatitis. Pancreatology. 2018 Oct 1;18(7):774-84. [CrossRef]
- Issa Y, Kempeneers MA, van Santvoort HC, Bollen TL, Bipat S, Boermeester MA. Diagnostic performance of imaging modalities in chronic pancreatitis: a systematic review and meta-analysis. Vol. 27, European Radiology. Springer Verlag; 2017. p. 3820-44. [CrossRef]
- Frøkjær JB, Akisik F, Farooq A, Akpinar B, Dasyam A, Drewes AM, et al. Guidelines for the Diagnostic Cross Sectional Imaging and Severity Scoring of Chronic Pancreatitis. Pancreatology. 2018 Oct 1;18(7):764-73. [CrossRef]
- Andersen PL, Madzak A, Olesen SS, Drewes AM, Frøkjaer JB. Quantification of parenchymal calcifications in chronic pancreatitis: relation to atrophy, ductal changes, fibrosis and clinical parameters. Scand J Gastroenterol. 2018 Feb 1;53(2):218-24. [CrossRef]
- Tirkes T, Shah ZK, Takahashi N, Grajo JR, Chang ST, Venkatesh SK, et al. Reporting standards for chronic pancreatitis by using CT, MRI, and MR cholangiopancreatography: The consortium for the study of chronic pancreatitis, diabetes, and pancreatic cancer. Radiology. 2019 Jan 1;290(1):207-15. [CrossRef]
- Ge QC, Zhang BZ, Zhang Y, Wang YD, Zhang JJ, Wu YF, et al. Comprehensive review of diagnostic modalities for early chronic pancreatitis. Vol. 27, World Journal of Gastroenterology. Baishideng Publishing Group Inc; 2021. p. 4342-57. [CrossRef]
- Tirkes T, Fogel EL, Sherman S, Lin C, Swensson J, Akisik F, et al. Detection of exocrine dysfunction by MRI in patients with early chronic pancreatitis. Abdominal Radiology. 2017 Feb 1;42(2):544-51. [CrossRef]
- Wang M, Gao F, Wang X, Liu Y, Ji R, Cang L, et al. Magnetic resonance elastography and T1 mapping for early diagnosis and classification of chronic pancreatitis. Journal of Magnetic Resonance Imaging. 2018 Sep 1;48(3):837-45. [CrossRef]
- Frøkjær JB, Akisik F, Farooq A, Akpinar B, Dasyam A, Drewes AM, et al. Guidelines for the Diagnostic Cross Sectional Imaging and Severity Scoring of Chronic Pancreatitis. Pancreatology. 2018 Oct 1;18(7):764-73. [CrossRef]
- Schreyer AG, Jung M, Riemann JF, Niessen C, Pregler B, Grenacher L, et al. S3 guideline for chronic pancreatitis - Diagnosis, classification and therapy for the radiologist. Vol. 186, RoFo Fortschritte auf dem Gebiet der Rontgenstrahlen und der Bildgebenden Verfahren. Georg Thieme Verlag; 2004. p. 1002-8. [CrossRef]
- DeWitt J, McGreevy K, LeBlanc J, McHenry L, Cummings O, Sherman S. EUS-guided Trucut biopsy of suspected nonfocal chronic pancreatitis. Gastrointest Endosc. 2005 Jul;62(1):76-84. [CrossRef]
- Wallace MB, Hawes RH, Durkalski V, Chak A, Mallery S, Catalano MF, et al. The reliability of EUS for the diagnosis of chronic pancreatitis: interobserver agreement among experienced endosonographers. Gastrointest Endosc. 2001 Mar;53(3):0294-9. [CrossRef]
- Yamamiya A, Irisawa A, Abe Y, Arisaka T, Ohnishi T, Hoshi K, et al. Diagnosing chronic pancreatitis by endoscopic ultrasound assessing the association between ultrasound and pathological findings: A narrative review. DEN Open. 2023 Apr;3(1). [CrossRef]
- Iglesias-García J, Lariño-Noia J, Lindkvist B, Domínguez-Muñoz JE. Endoscopic ultrasound in the diagnosis of chronic pancreatitis. Revista espanola de enfermedades digestivas. 2015 Apr;107(4):221-8.
- Inomata N, Masuda A, Yamakawa K, Takenaka M, Tsujimae M, Toyama H, et al. Lobularity rather than hyperechoic foci/stranding on endoscopic ultrasonography is associated with more severe histological features in chronic pancreatitis. Journal of Gastroenterology and Hepatology (Australia). 2023 Jan 1;38(1):103-11. [CrossRef]
- Sekine M, Tanaka A, Akimoto M, Miura T, Fujiwara J, Noda H, et al. A Comparative Study of Endoscopic Ultrasonography and Histopathology Images for the Diagnosis of Early Chronic Pancreatitis. Pancreas. 2021 Sep 1;50(8):1173-9. [CrossRef]
- Koh CJ, Lakhtakia S, Kida M, Lesmana CRA, Ang TL, Vu CKF, et al. Defining the endoscopic ultrasound features of chronic pancreatitis in Asians: A multicenter validation study. Endoscopy. 2021 Jun 1;53(6):595-602. [CrossRef]
- LeBlanc JK, Chen JH, Al-Haddad M, Juan M, Okumu W, McHenry L, et al. Endoscopic Ultrasound and Histology in Chronic Pancreatitis. Pancreas. 2014 Apr;43(3):440-4. [CrossRef]
- Yamabe A, Irisawa A, Bhutani MS, Sato A, Maki T, Takasaki Y, et al. Validity of Endoscopic Ultrasound Findings of Chronic Pancreatitis: Evaluation from the Viewpoint of Disease Risk Factors. Digestion. 2021 Feb 1;102(2):289-97. [CrossRef]
- Yamashita Y, Tanioka K, Kawaji Y, Tamura T, Nuta J, Hatamaru K, et al. Utility of elastography with endoscopic ultrasonography shear-wave measurement for diagnosing chronic pancreatitis. Gut Liver. 2020 Sep 1;14(5):659-64. [CrossRef]
- Iglesias-Garcia J, Domínguez-Muñoz JE, Castiñeira-Alvariño M, Luaces-Regueira M, Lariño-Noia J. Quantitative elastography associated with endoscopic ultrasound for the diagnosis of chronic pancreatitis. Endoscopy. 2013;45(10):781-8. [CrossRef]
- Kuwahara T, Hirooka Y, Kawashima H, Ohno E, Ishikawa T, Kawai M, et al. Quantitative diagnosis of chronic pancreatitis using EUS elastography. J Gastroenterol. 2017 Jul 1;52(7):868-74. [CrossRef]
- Yamashita Y, Tanioka K, Kawaji Y, Tamura T, Nuta J, Hatamaru K, et al. Endoscopic ultrasonography shear wave as a predictive factor of endocrine/exocrine dysfunction in chronic pancreatitis. Journal of Gastroenterology and Hepatology (Australia). 2021 Feb 1;36(2):391-6. [CrossRef]
- Domínguez-Muñoz JE, Lariño-Noia J, Alvarez-Castro A, Nieto L, Lojo S, Leal S, et al. Endoscopic ultrasound-based multimodal evaluation of the pancreas in patients with suspected early chronic pancreatitis. United European Gastroenterol J. 2020 Aug 1;8(7):790-7. [CrossRef]
- Wiersema MJ, Hawes RH, Lehman GA, Kochman ML, Sherman S, Kopecky KK. Prospective Evaluation of Endoscopic Ultrasonography and Endoscopic Retrograde Cholangiopancreatography in Patients with Chronic Abdominal Pain of Suspected Pancreatic Origin. Endoscopy. 1993 Nov 17;25(09):555-64. [CrossRef]
|
Clinical signs 1) Repeated upper abdominal pain 2) Abnormal pancreatic enzyme levels in the serum or urine 3) Abnormal pancreatic exocrine function 4) Continuous heavy drinking of alcohol equivalent to or more than 80 g/day of pure ethanol |
Imaging findings (Either a or b)
|
|
Clinical features (1) Repeated epigastric or back pain (2) Outlier of pancreatic enzyme levels in the serum or urine (3) Outlier of pancreatic exocrine function (4) Continuous heavy drinking of alcohol equivalent to or more than 60 g/day of pure ethanol (EtOH 60g/day) or pancreatitis-related susceptibility genes Continuous heavy drinking of alcohol (5) Previous history of acute pancreatitis |
|
Imaging findings of early chronic pancreatitis (Either a or b) a. More than two features among the following four features of EUS findings including at least one of (1)-(2) (1) Hyperechoic foci; non-shadowing/Stranding (2) Lobularity [Non-honeycombing/ honeycombing type] (3) Hyperechoic main pancreatic duct margin (4) Dilated side branches b. Irregular dilatation of more than three duct branches on ERCP or MRCP findings |
| Criteria | Definition | Histopathological attributes |
|---|---|---|
| Lobularity with honey-combing | Presence of ≥3 EUS-defined lobules (reticulated areas surrounded by ≥5 mm rim-like hyperechoic structures) in the body or tail region | Interlobular fibrosis |
| Lobularity without honey-combing | Presence of non-contiguous lobularity | |
| Hyperechoic foci without shadowing | Echogenic structures ≥3 mm without acoustic shadow | Focal fibrosis |
| Hyperechoic stranding | At least three hyperechoic lines of ≥3 mm in length in different planes of the image | Bridging fibrosis |
| Cysts | Anechoic structures, with/ without septations, round or elliptical in shape | Pseudocyst or retention cyst |
| Dilated side branches | Presence of ≥3 tubular anechoic structures arising from the MPD, each ≥1 mm in width, indicative of micro-fibrosis | Ductal ectasia |
| Hyperechoic MPD margin | Echogenic structure involving at least 50% of the MPD | Periductal fibrosis; thickened ductal wall. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




