Submitted:
13 December 2023
Posted:
14 December 2023
You are already at the latest version
Abstract
Keywords:
Introduction
Material and Methods
Ethical Statement
Study Design and Cohort
Recruitment
Collection of History Data, Clinical Parameters, and Risk Scores Calculation:
Data Collection for Risk Score Calculation
Family History
Stature and Extremities
Skeletal Deformities
Joint function
Ophthalmologic Pathologies
General Diagnoses
Cardiovascular Pathology and Cumulative Risk Score
Further Comorbidities
Molecular Genetic Analysis
Data Acquisition and Cooperation Partners
Statistical Analysis
Results
Patient Cohort, Demographic Data and Representability of the Study Cohort
Family History Analysis and Distribution of Phenotypical Characteristics
Analysis of Genetic Variants and Correlation with Phenotype
Genetic Variants and Association with Genetic Disease
Discussion
Limitations
Conclusion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bossone E, Eagle KA. Epidemiology and management of aortic diseases: Aortic aneurysms and acute aortic syndromes. Nature Rev Card 2020;18:331-348. [CrossRef]
- Ostberg N, Zafar M, Ziganshin B, Elefteriades J. The genetics of thoracic aortic aneurysms and dissection: A clinical perspective. Biomolecules 2020;10:182. [CrossRef]
- Brownstein A, Kostiuk V, Ziganshin B, Zafar M, Kuivaniemi H, Body S, et al. Genes associated with thoracic aortic aneurysm and dissection: 2018 update and clinical implications. AORTA 2018;06:013-020. [CrossRef]
- Yuan X, Mitsis A, Nienaber CA. Current understanding of aortic dissection. Life 2020;12:1606. [CrossRef]
- Zhou Z, Cecchi AC, Prakash SK, Milewicz DM. Risk factors for thoracic aortic dissection. Genes 2022;13:1814. [CrossRef]
- Czerny M, Schmidli J, Adler S, van den Berg JC, Bertoglio L, Carrel T, et al. Current options and recommendations for the treatment of thoracic aortic pathologies involving the aortic arch: An expert consensus document of the European Association for Cardio-Thoracic Surgery (EACTS) and the European Society for Vascular Surgery (ESVS). Eur J Cardio-Thorac Surg 2019;55:133-162. [CrossRef]
- Von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The strengthening the reporting of observational studies in epidemiology (STROBE) statement: Guidelines for reporting observational studies. J Clin Epidemiol. 2008;61:344-349. [CrossRef]
- Plon SE, Eccles DM, Easton D, Foulkes WD, Genuardi M, Greenblatt MS, et al. Sequence variant classification and reporting: Recommendations for improving the interpretation of cancer susceptibility genetic test results. Human Mutation 2008;29:1282-1291. [CrossRef]
- Renard M, Francis C, Ghosh R, Scott AF, Witmer PD, Adés LC, et al. Clinical validity of genes for heritable thoracic aortic aneurysm and dissection. J Am Coll Cardiol 2018;72:605-615. [CrossRef]
- Proost D, Vandeweyer G, Meester JAN, Salemink S, Kempers M, Ingram C, et al. (2015). Performant mutation identification using targeted next-generation sequencing of 14 thoracic aortic aneurysm genes. Human Mutation 2015;36:808-814. [CrossRef]
- Fang M, Yu C, Chen S, Xiong W, Li X, Zeng R, et al. (2017). Identification of novel clinically relevant variants in 70 Southern Chinese patients with thoracic aortic aneurysm and dissection by Next-Generation Sequencing. Sci Rep 2017;7:10035. [CrossRef]
- Ziganshin BA, Bailey AE, Coons C, Dykas D, Charilaou P, Tanriverdi LH, et al. (2015). Routine genetic testing for thoracic aortic aneurysm and dissection in a clinical setting. Ann Thorac Surg 2015;100:1604-1611. [CrossRef]
- Poninska JK, Bilinska ZT, Franaszczyk M, Michalak E, Rydzanicz M, Szpakowski E, et al. (2016). Next-generation sequencing for diagnosis of thoracic aortic aneurysms and dissections: Diagnostic yield, novel mutations, and genotype-phenotype corrections. J Transl Med 2016;14:115. [CrossRef]
- Wooderchak-Donahue W, VanSant-Webb C, Tvrdik T, Plant P, Lewis T, Stocks J, et al. (2015). Clinical utility of a next generation sequencing panel assay for Marfan and Marfan-like syndromes featuring aortopathy. Am J Med Genet 2015;167:1747-1757. [CrossRef]
- Campens L, Callewaert B, Muiño Mosquera L, Renard M, Symoens S, De Paepe AS, et al. Gene panel sequencing in heritable thoracic aortic disorders and related entities – results of comprehensive testing in a cohort of 264 patients. Orphanet J Rare Dis 2015;10:9. [CrossRef]
- Yang H, Luo M, Fu Y, Cao Y, Yin K, Li W, et al. (2016). Genetic testing of 248 Chinese aortopathy patients using a panel assay. Sci Rep 2016;6:33002. [CrossRef]
- Overwater E, Marsili L, Baars MJH, Baas AF, van de Beek I, Dulfer E, et al. (2018). Results of next-generation sequencing gene panel diagnostics including copy-number variation analysis in 810 patients suspected of heritable thoracic aortic disorders. Human Mutation 2018;39:1173-1192. [CrossRef]
- Renner S, Schüler H, Alawi M, Kolbe V, Rybczynski M, Woitschach R, et al. Next-generation sequencing of 32 genes associated with hereditary aortopathies and related disorders of connective tissue in a cohort of 199 patients. Gen Med 2019;21:1832-1841. [CrossRef]
- Duan D-M, Chiu H-H, Chen P-L, Yeh P-T, Yu C-W, Yang K-C, et al. Clinical manifestations and genetic characteristics in the Taiwan thoracic aortic aneurysm and dissection cohort – A prospective cohort study. J Form Med Assoc 2022;121:1093-1101. [CrossRef]
- Keravnou A, Bashiardes E, Michailidou K, Soteriou M, Moushi A, & Cariolou M. (2018). Novel variants in the ACTA2 and MYH11 genes in a Cypriot family with thoracic aortic aneurysms: A case report. BMC Med Gen 2018;19:208. [CrossRef]
- Guo D, Hostetler EM, Fan Y, Kulmacz RJ, Zhang D, Nickerson DA, et al. Heritable thoracic aortic disease genes in sporadic aortic dissection. J Am Coll Cardiol 2017;70:2728-2730. [CrossRef]
- Faggion Vinholo T, Brownstein AJ, Ziganshin BA, Zafar MA, Kuivaniemi H, Body SC, et al. Genes associated with thoracic aortic aneurysm and dissection: 2019 update and clinical implications. AORTA 2019;07:099-107. [CrossRef]
- Acharya M, Masselli D, Mariscalco G. Genetic screening in heritable thoracic aortic disease – Rationale, potentials, and pitfalls. Ind J Thorac Cardiovasc Surg 2022;38:24-35. [CrossRef]
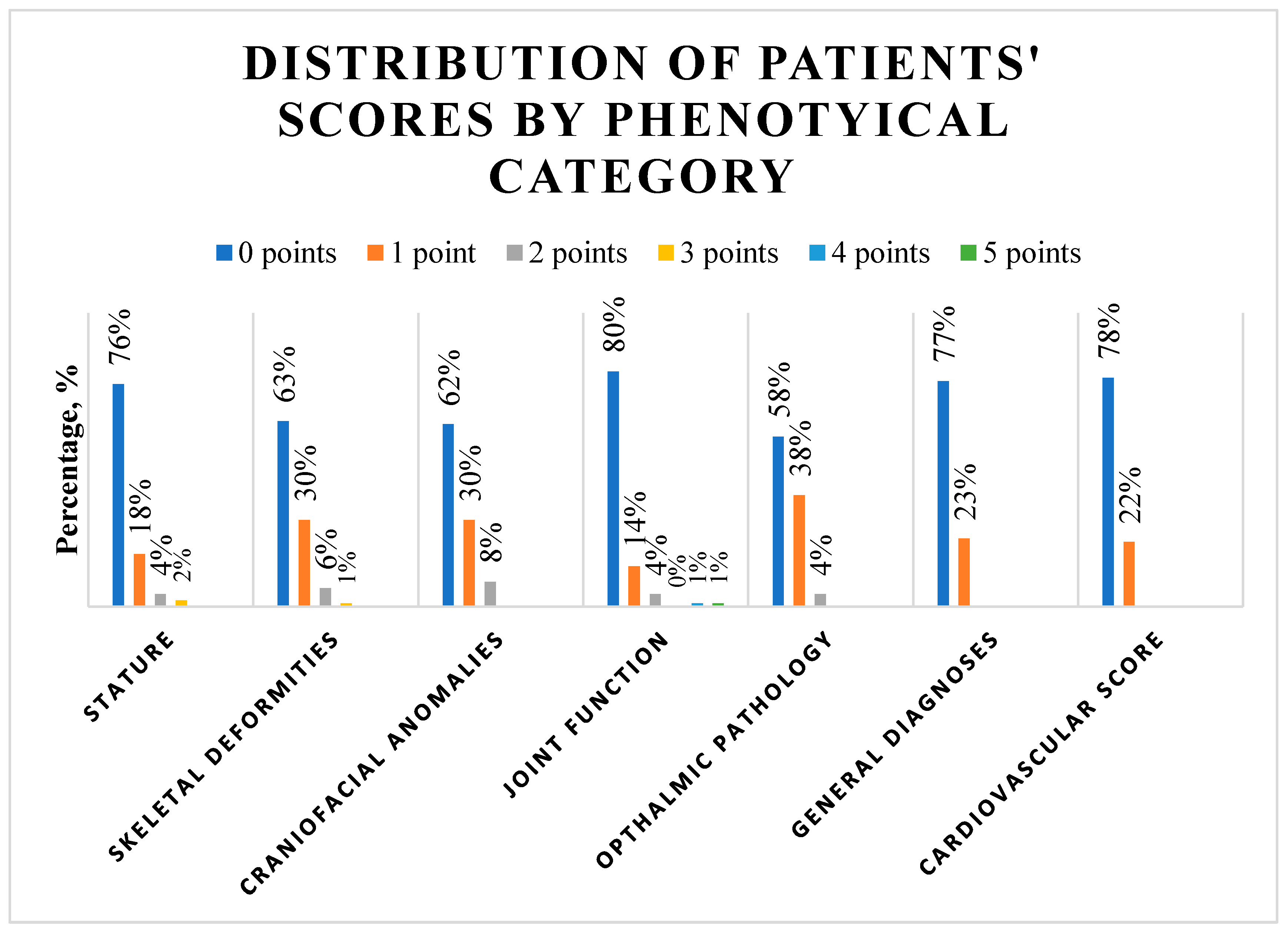
| Variable | No phenotypical signs | Present phenotypical signs | p-value |
|---|---|---|---|
| Number (percentage) | Number (percentage) | ||
| Age | 0.783 | ||
| under 45 years | 3 (11.5 %) | 23 (88.5 %) | |
| 45-65 years | 8 (16.0 %) | 42 (84.0 %) | |
| over 65 years | 2 (10.5 %) | 17 (89.5 %) | |
| Sex | 0.712 | ||
| males | 9 (13.4 %) | 58 (86.6 %) | |
| females | 4 (14.3 %) | 24 (85.7 %) | |
| Aortic pathology | 0.74 | ||
| Aortic aneurysm | 6 (15.4 %) | 33 (84.6 %) | |
| Aortic dissection | 7 (12.9 %) | 47 (87.1 %) | |
| Treatment | 0.478 | ||
| surgical | 10 (15.4 %) | 55 (84.6 %) | |
| endovascular | 3 (10.0 %) | 27 (90.0 %) | |
- Table 2. lists further the detailed results of gene variant distribution across the cohort.
- Table 2. Distribution of genetic mutations across the study cohort.
- Table 2. lists further the detailed results of gene variant distribution across the cohort.
- Table 2. Distribution of genetic mutations across the study cohort.
|
Name of the gene |
Number of mutation detections (n =) | Proportion of the total number of mutation detections (in %) | Classic mutation (n =) |
Percentage of classic mutations to total number of Evidence of mutation (in %) |
Mutation variant (n =) |
Percentage of mutation variants in total number of mutation detections (in %) |
|---|---|---|---|---|---|---|
| FBN 1 | 13 | 32.5 | 3 | 7.5 | 10 | 25 |
| COL3A1 | 1 | 2.5 | 1 | 2.5 | 0 | 0 |
| SMAD3 | 1 | 2.5 | 0 | 0 | 1 | 2.5 |
| TGFB2 | 4 | 10.0 | 1 | 2.5 | 3 | 7.5 |
| TGFBR1 | 2 | 5.0 | 0 | 0 | 2 | 5.0 |
| MYLK | 2 | 5.0 | 0 | 0 | 2 | 5.0 |
| MYH11 | 8 | 20.0 | 0 | 0 | 8 | 20.0 |
| PRKG1 | 1 | 2.5 | 0 | 0 | 1 | 2.5 |
|
NOTCH3 |
1 | 2.5 | 1 | 2.5 | 0 | 0 |
|
NOTCH1 |
3 | 7.5 | 0 | 0 | 3 | 7.5 |
| TGFBR2 | 1 | 2.5 | 0 | 0 | 1 | 2.5 |
| ACTA2 | 2 | 5.0 | 0 | 0 | 2 | 5.0 |
| SMAD6 | 1 | 2.5 | 0 | 0 | 1 | 2.5 |
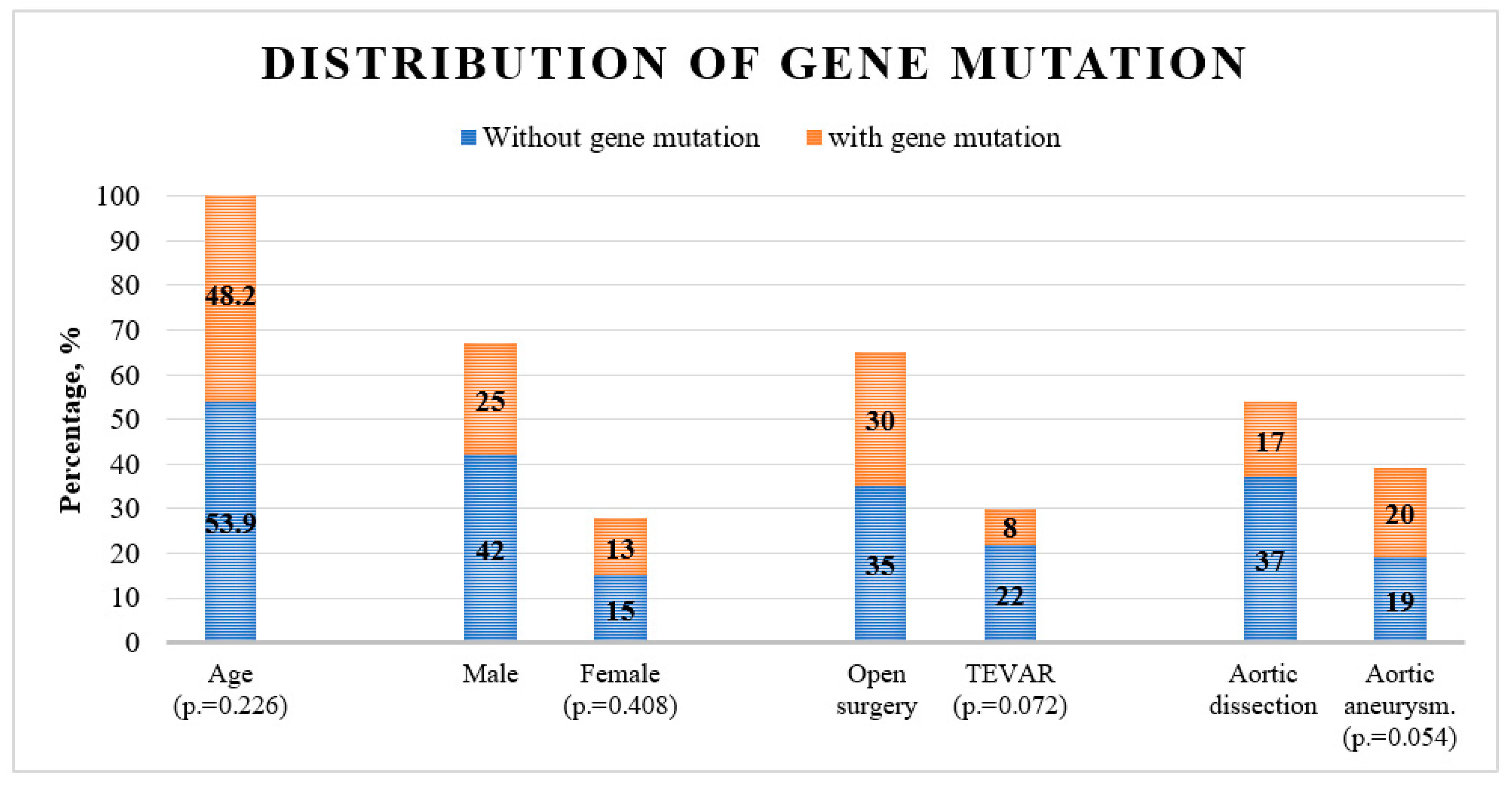
| Variable | Without gene mutation | With gene mutation | p-value |
|---|---|---|---|
| Mean (± standard deviation) | Mean (± standard deviation) | ||
| Age (in years) | 53.9 ± 10.5 | 48.2 ± 13.7 | 0.226 |
| Number (percentage) | Number (percentage) | ||
| Males | 42 (62.7 %) | 25 (37.3 %) | 0.408 |
| Females | 15 (53.6 %) | 13 (46.4 %) | |
| Open surgery | 35 (53.8 %) | 30 (46.2 %) | 0.072 |
| TEVAR | 22 (73.3 %) | 8 (26.7 %) | |
| Aortic aneurysm | 19 (48.7 %) | 20 (51.3 %) | 0.054 |
| Aortic dissection | 37 (68.5 %) | 17 (31.5 %) | |
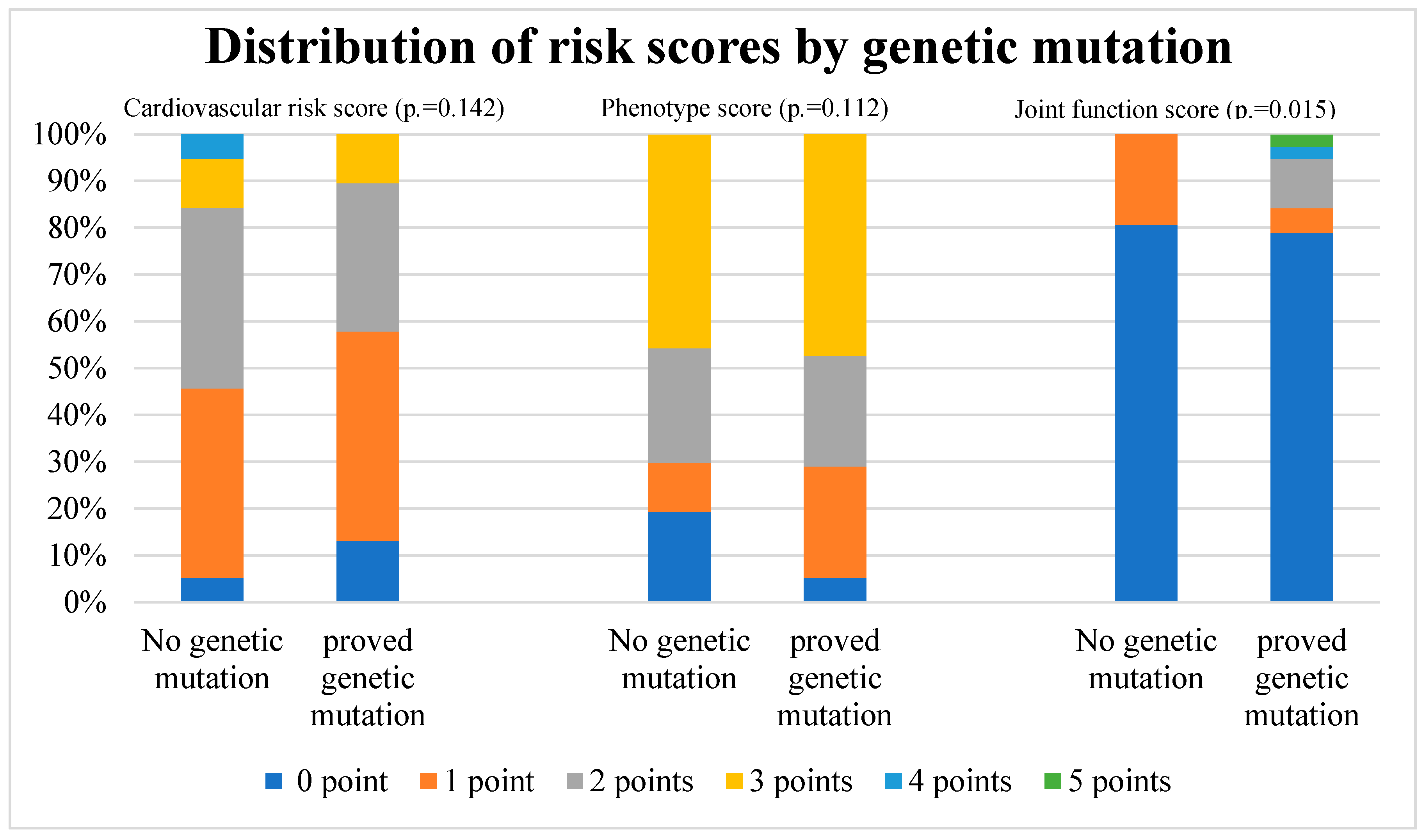
| Cardiovascular risk score | 0.142 | ||
| 0 point | 3 (5.3%) | 5 (13.2%) | |
| 1 point | 23 (40.4%) | 17 (44.7%) | |
| 2 points | 22 (38.6%) | 12 (31.6%) | |
| 3 points | 6 (10.5%) | 4 (10.5%) | |
| 4 points | 3 (5.3%) | 0 (0%) | |
| Phenotype score category | 0.122 | ||
| Score =0 | 11 (19.3 %) | 2 (5.3 %) | |
| Score =1 | 6 (10.5 %) | 9 (23.7 %) | |
| Score =2 | 14 (24.5 %) | 9 (23.7 %) | |
| Score >= 3 | 26 (45.6 %) | 18 (47.4 %) | |
| Joint function score | 0.015 | ||
| Score =0 | 46 (80.7%) | 30 (78.9%) | |
| Score =1 | 11 (19.3%) | 2 (5.3%) | |
| Score =2 | 0 (0%) | 4 (10.5%) | |
| Score =3 | 0 (0%) | 0 (0%) | |
| Score =4 | 0 (0%) | 1 (2.6%) | |
| Score =5 | 0 (0%) | 1 (2.6 %) | |
| Abbreviations: TEVAR = Thoracic Endovascular Aortic Repair. | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




