Submitted:
05 December 2023
Posted:
07 December 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Data Collection
2.3. Outcomes
2.4. Statistical Analysis
3. Results
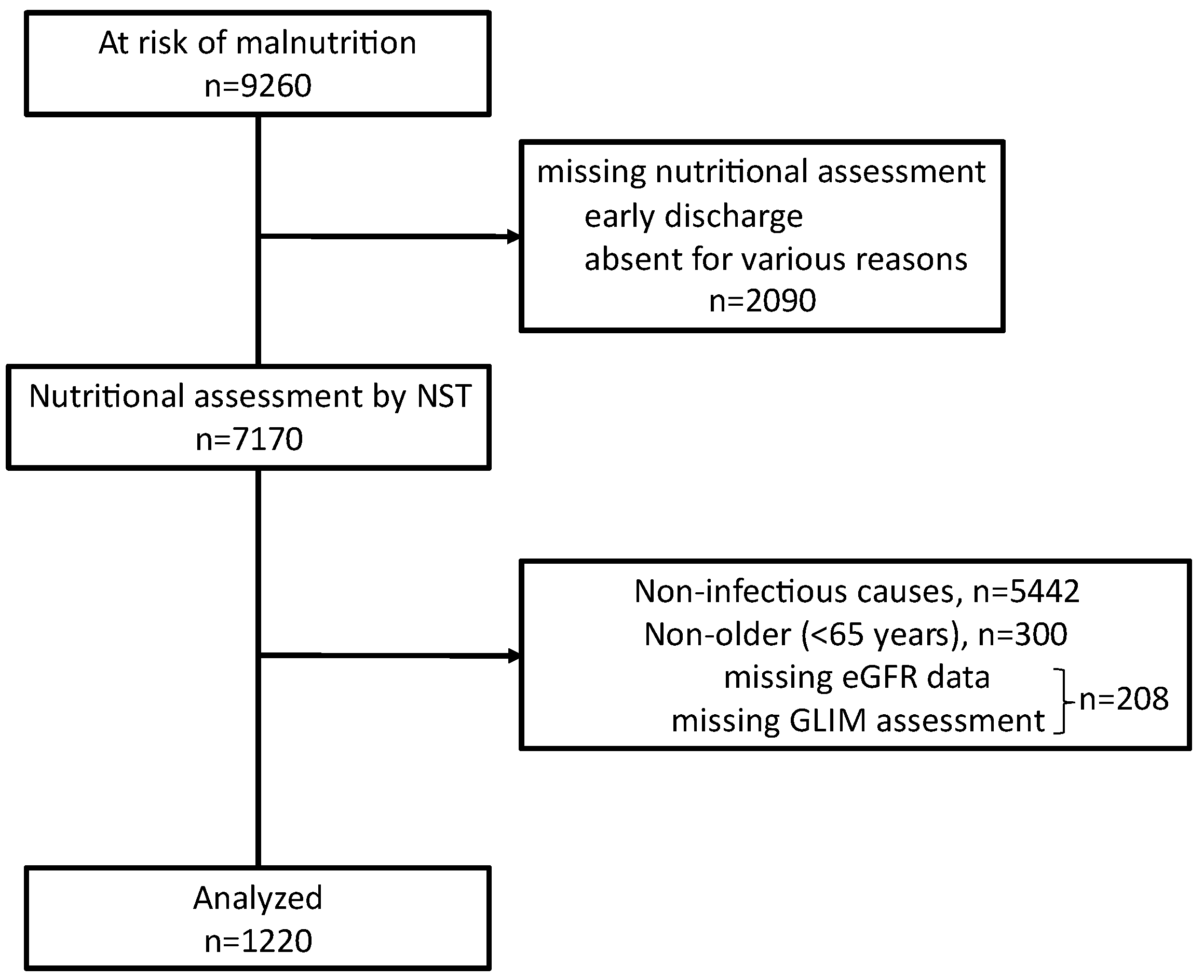
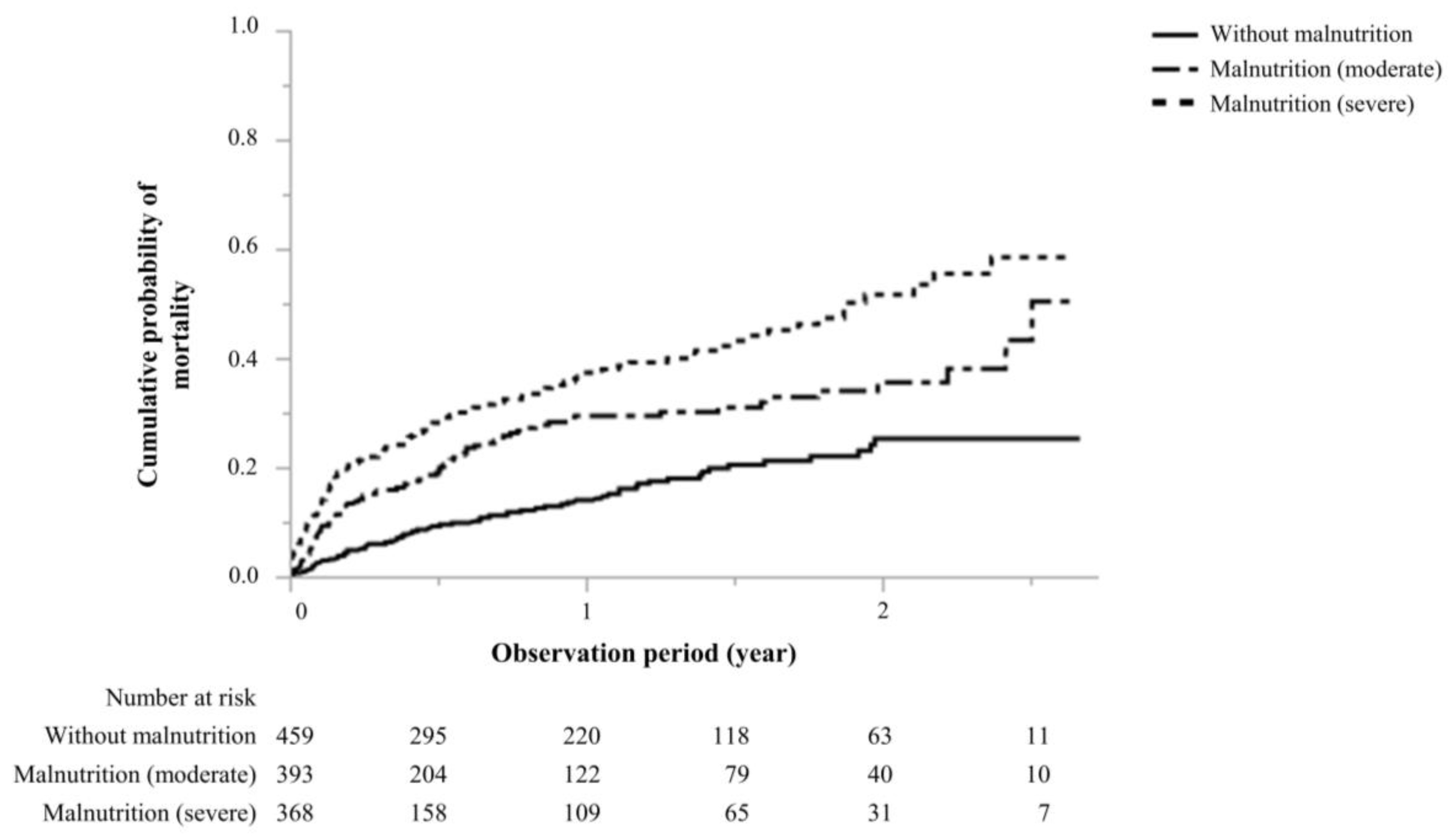
3.1. Association of Malnutrition with Kidney Function and Mortality
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Ramírez-Soto, M.C. Long-term, all-cause mortality risk after infection episodes in older adults. Lancet Healthy Longev 2023, 4, e452–e454. [Google Scholar] [CrossRef]
- Nielsen, S.L.; Lassen, A.T.; Gradel, K.O.; Jensen, T.G.; Kolmos, H.J.; Hallas, J.; Pedersen, C. Bacteremia is associated with excess long-term mortality: A 12-year population-based cohort study. J Infect 2015, 70, 111–126. [Google Scholar] [CrossRef]
- Dick, A.; Liu, H.; Zwanziger, J.; Perencevich, E.; Furuya, E.Y.; Larson, E.; Pogorzelska-Maziarz, M.; Stone, P.W. Long-term survival and healthcare utilization outcomes attributable to sepsis and pneumonia. BMC Health Serv Res 2012, 12, 432. [Google Scholar] [CrossRef] [PubMed]
- Correia, M.I.T.D.; Perman, M.I.; Waitzberg, D.L. Hospital malnutrition in Latin America: A systematic review. Clin Nutr 2017, 36, 958–967. [Google Scholar] [CrossRef]
- Tannou, T.; Koeberle, S.; Manckoundia, P.; Aubry, R. Multifactorial immunodeficiency in frail elderly patients: Contributing factors and management. Med Mal Infect 2019, 49, 167–172. [Google Scholar] [CrossRef] [PubMed]
- Bellanti, F.; Lo Buglio, A.; Quiete, S.; Pellegrino, G.; Dobrakowski, M.; Kasperczyk, A.; Kasperczyk, S.; Vendemiale, G. Comparison of three nutritional screening tools with the new glim criteria for malnutrition and association with sarcopenia in hospitalized older patients. J Clin Med 2020, 9. [Google Scholar] [CrossRef] [PubMed]
- Guenter, P.; Abdelhadi, R.; Anthony, P.; Blackmer, A.; Malone, A.; Mirtallo, J.M.; Phillips, W.; Resnick, H.E. Malnutrition diagnoses and associated outcomes in hospitalized patients: United States, 2018. Nutr Clin Pract 2021, 36, 957–969. [Google Scholar] [CrossRef] [PubMed]
- Kirkland, L.L.; Kashiwagi, D.T.; Brantley, S.; Scheurer, D.; Varkey, P. Nutrition in the hospitalized patient. J Hosp Med 2013, 8, 52–58. [Google Scholar] [CrossRef] [PubMed]
- Inciong, J.F.B.; Chaudhary, A.; Hsu, H.S.; Joshi, R.; Seo, J.M.; Trung, L.V.; Ungpinitpong, W.; Usman, N. Hospital malnutrition in northeast and Southeast Asia: A systematic literature review. Clin Nutr ESPEN 2020, 39, 30–45. [Google Scholar] [CrossRef] [PubMed]
- Ishigami, J.; Matsushita, K. Clinical epidemiology of infectious disease among patients with chronic kidney disease. Clin Exp Nephrol 2019, 23, 437–447. [Google Scholar] [CrossRef]
- Chang, C.H.; Fan, P.C.; Kuo, G.; Lin, Y.S.; Tsai, T.Y.; Chang, S.W.; Tian, Y.C.; Lee, C.C. Infection in advanced chronic kidney disease and subsequent adverse outcomes after dialysis initiation: A nationwide cohort study. Sci Rep 2020, 10, 2938. [Google Scholar] [CrossRef]
- Syed-Ahmed, M.; Narayanan, M. Immune dysfunction and risk of infection in chronic kidney disease. Adv Chronic Kidney Dis 2019, 26, 8–15. [Google Scholar] [CrossRef]
- Piccoli, G.B.; Cederholm, T.; Avesani, C.M.; Bakker, S.J.L.; Bellizzi, V.; Cuerda, C.; Cupisti, A.; Sabatino, A.; Schneider, S.; Torreggiani, M.; et al. Nutritional status and the risk of malnutrition in older adults with chronic kidney disease – Implications for low protein intake and nutritional care: A critical review endorsed by ERN-ERA and ESPEN. Clin Nutr 2023, 42, 443–457. [Google Scholar] [CrossRef]
- Rondel, A.L.M.A.; Langius, J.A.E.; de van der Schueren, M.A.E.; Kruizenga, H.M. The new ESPEN diagnostic criteria for malnutrition predict overall survival in hospitalised patients. Clin Nutr 2018, 37, 163–168. [Google Scholar] [CrossRef]
- Cederholm, T.; Barazzoni, R. Validity and feasibility of the global leadership initiative on malnutrition diagnostic concept in older people: A literature review from August 2021 to August 2022. Curr Opin Clin Nutr Metab Care 2023, 26, 23–31. [Google Scholar] [CrossRef]
- Balcı, C.; Tufan, G.; Özdemir, N.; Aksoy, S.; Öksüzoğlu, Ö.B.; Zengin, N.; Kars, A.; Halil, M. GLIM criteria as a valid tool for nutrition assessment and mortality prediction in treatment-naïve patients with cancer. Nutr Clin Pract 2023, 38, 798–806. [Google Scholar] [CrossRef] [PubMed]
- Yin, L.; Chong, F.; Huo, Z.; Li, N.; Liu, J.; Xu, H. GLIM-defined malnutrition and overall survival in cancer patients: A meta-analysis. JPEN J Parenter Enteral Nutr 2023, 47, 207–219. [Google Scholar] [CrossRef] [PubMed]
- Yang, W.; Guo, G.; Cui, B.; Li, Y.; Sun, M.; Li, C.; Wang, X.; Mao, L.; Hui, Y.; Fan, X.; et al. Malnutrition according to the Global Leadership Initiative on Malnutrition criteria is associated with in-hospital mortality and prolonged length of stay in patients with cirrhosis. Nutrition 2023, 105, 111860. [Google Scholar] [CrossRef] [PubMed]
- Joaquín, C.; Alonso, N.; Lupón, J.; Gastelurrutia, P.; Pérez-Monstesdeoca, A.; Domingo, M.; Zamora, E.; Socias, G.; Ramos, A.; Bayes-Genis, A.; et al. Nutritional status according to the GLIM criteria in patients with chronic Heart Failure: Association with prognosis. Nutrients 2022, 14. [Google Scholar] [CrossRef]
- Shirai, Y.; Momosaki, R.; Kokura, Y.; Kato, Y.; Okugawa, Y.; Shimizu, A. Validation of Asian body mass index cutoff values for the classification of malnutrition severity according to the global leadership initiative on malnutrition criteria in patients with chronic obstructive pulmonary disease exacerbations. Nutrients 2022, 14. [Google Scholar] [CrossRef] [PubMed]
- Sánchez-Torralvo, F.J.; Pérez-Del-Río, V.; García-Olivares, M.; Porras, N.; Abuín-Fernández, J.; Bravo-Bardají, M.F.; García-de-Quevedo, D.; Olveira, G. Global subjective assessment and mini nutritional assessment short form better predict mortality than GLIM malnutrition criteria in elderly patients with hip fracture. Nutrients 2023, 15. [Google Scholar] [CrossRef]
- Díaz, G.; T D Correia, M.I.; Gonzalez, M.C.; Reyes, M. The global leadership initiative on malnutrition criteria for the diagnosis of malnutrition in patients admitted to the intensive care unit: A systematic review and meta-analysis. Clin Nutr 2023, 42, 182–189. [Google Scholar] [CrossRef]
- MacDonell, S.O.; Moyes, S.A.; Teh, R.; Dyall, L.; Kerse, N.; Wham, C. Is the utility of the GLIM criteria used to diagnose malnutrition suitable for bicultural populations? Findings from life and living in advanced age cohort study in New Zealand (LiLACS NZ). J Nutr Health Aging 2023, 27, 67–74. [Google Scholar] [CrossRef]
- Sipilä PN, Lindbohm JV, Batty GD, Heikkilä N, Vahtera J, Suominen S, Väänänen A, Koskinen A, Nyberg ST, Meri S, et al. Severe Infection and Risk of Cardiovascular Disease: A Multicohort Study. Circulation. 2023, 147, 1582–1593. [CrossRef]
- Stratton, R.J.; Hackston, A.; Longmore, D.; Dixon, R.; Price, S.; Stroud, M.; King, C.; Elia, M. Malnutrition in hospital outpatients and inpatients: Prevalence, concurrent validity and ease of use of the ‘malnutrition universal screening tool’ (“MUST”) for adults. Br J Nutr 2004, 92, 799–808. [Google Scholar] [CrossRef] [PubMed]
- Rubenstein, L.Z.; Harker, J.O.; Salvà, A.; Guigoz, Y.; Vellas, B. Screening for undernutrition in geriatric practice: Developing the short-form mini-nutritional assessment (MNA-SF). J Gerontol A Biol Sci Med Sci 2001, 56, M366–M372. [Google Scholar] [CrossRef] [PubMed]
- Matsuo, S.; Imai, E.; Horio, M.; Yasuda, Y.; Tomita, K.; Nitta, K.; Yamagata, K.; Tomino, Y.; Yokoyama, H.; Hishida, A.; et al. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis 2009, 53, 982–992. [Google Scholar] [CrossRef]
- Cederholm, T.; Jensen, G.L.; Correia, M.I.T.D.; Gonzalez, M.C.; Fukushima, R.; Higashiguchi, T.; Baptista, G.; Barazzoni, R.; Blaauw, R.; Coats, A.J.S.; et al. GLIM criteria for the diagnosis of malnutrition - A consensus report from the global clinical nutrition community. J Cachexia Sarcopenia Muscle 2019, 10, 207–217. [Google Scholar] [CrossRef] [PubMed]
- Mori, N.; Maeda, K.; Fujimoto, Y.; Nonogaki, T.; Ishida, Y.; Ohta, R.; Shimizu, A.; Ueshima, J.; Nagano, A.; Fukushima, R. Prognostic implications of the global leadership initiative on malnutrition criteria as a routine assessment modality for malnutrition in hospitalized patients at a university hospital. Clin Nutr 2023, 42, 166–172. [Google Scholar] [CrossRef] [PubMed]
- Maeda, K.; Ishida, Y.; Nonogaki, T.; Mori, N. Reference body mass index values and the prevalence of malnutrition according to the Global Leadership Initiative on Malnutrition criteria. Clin Nutr 2020, 39, 180–184. [Google Scholar] [CrossRef]
- Maeda, K.; Koga, T.; Nasu, T.; Takaki, M.; Akagi, J. Predictive accuracy of calf circumference measurements to detect decreased skeletal muscle mass and European Society for Clinical Nutrition and Metabolism-defined malnutrition in hospitalized older patients. Ann Nutr Metab 2017, 71, 10–15. [Google Scholar] [CrossRef]
- Barazzoni, R.; Jensen, G.L.; Correia, M.I.T.D.; Gonzalez, M.C.; Higashiguchi, T.; Shi, H.P.; Bischoff, S.C.; Boirie, Y.; Carrasco, F.; Cruz-Jentoft, A.; et al. Guidance for assessment of the muscle mass phenotypic criterion for the Global Leadership Initiative on Malnutrition (GLIM) diagnosis of malnutrition. Clin Nutr 2022, 41, 1425–1433. [Google Scholar] [CrossRef]
- Oguri, M.; Ishii, H.; Yasuda, K.; Sumi, T.; Takahashi, H.; Murohara, T. Combined prognostic value of malnutrition using GLIM criteria and renal insufficiency in elderly heart failure. ESC Heart Fail 2022, 9, 704–711. [Google Scholar] [CrossRef] [PubMed]
- O'Brien, W.J.; Gupta, K.; Itani, K.M.F. Association of Postoperative Infection With Risk of Long-term Infection and Mortality. JAMA Surg 2020, 155, 61–68. [Google Scholar] [CrossRef]
- Lin, H.Y.; Hsiao, F.Y.; Huang, S.T.; Chen, Y.C.; Lin, S.W.; Chen, L.K. Longitudinal impact of distinct infection trajectories on all-cause mortality of older people in Taiwan: a retrospective, nationwide, population-based study. Lancet Healthy Longev 2023, 4, e508–e516. [Google Scholar] [CrossRef]
- Nicolau, J.; Ayala, L.; Sanchís, P.; Olivares, J.; Dotres, K.; Soler, A.G.; Rodríguez, I.; Gómez, L.A.; Masmiquel, L. Influence of nutritional status on clinical outcomes among hospitalized patients with COVID-19. Clin Nutr ESPEN 2021, 43, 223–229. [Google Scholar] [CrossRef]
- Wakasugi, M.; Kawamura, K.; Yamamoto, S.; Kazama, J.J.; Narita, I. High mortality rate of infectious diseases in dialysis patients: A comparison with the general population in Japan. Ther Apher Dial 2012, 16, 226–231. [Google Scholar] [CrossRef] [PubMed]
- Schaible, U.E.; Kaufmann, S.H.E. Malnutrition and infection: Complex mechanisms and global impacts. PLOS Med 2007, 4, e115. [Google Scholar] [CrossRef]
- Katona, P.; Katona-Apte, J. The interaction between nutrition and infection. Clin Infect Dis 2008, 46, 1582–1588. [Google Scholar] [CrossRef] [PubMed]
- Litjens, N.H.R.; van Druningen, C.J.; Betjes, M.G.H. Progressive loss of renal function is associated with activation and depletion of naive T lymphocytes. Clin Immunol 2006, 118, 83–91. [Google Scholar] [CrossRef]
- Montecino-Rodriguez, E.; Berent-Maoz, B.; Dorshkind, K. Causes, consequences, and reversal of immune system aging. J Clin Invest 2013, 123, 958–965. [Google Scholar] [CrossRef] [PubMed]
- Cheikh Hassan, H.I.; Tang, M.; Djurdjev, O.; Langsford, D.; Sood, M.M.; Levin, A. Infection in advanced chronic kidney disease leads to increased risk of cardiovascular events, end-stage kidney disease and mortality. Kidney Int 2016, 90, 897–904. [Google Scholar] [CrossRef] [PubMed]
- Pletinck, A.; Glorieux, G.; Schepers, E.; Cohen, G.; Gondouin, B.; Van Landschoot, M.; Eloot, S.; Rops, A.; Van de Voorde, J.; De Vriese, A.; et al. Protein-bound uremic toxins stimulate crosstalk between leukocytes and vessel wall. J Am Soc Nephrol 2013, 24, 1981–1994. [Google Scholar] [CrossRef] [PubMed]
- Sack, M.N.; Fyhrquist, F.Y.; Saijonmaa, O.J.; Fuster, V.; Kovacic, J.C. Basic Biology of Oxidative Stress and the Cardiovascular System: Part 1 of a 3-Part Series. J Am Coll Cardiol 2017, 70, 196–211. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.Y.; Yoo, T.H.; Hwang, Y.; Lee, G.H.; Kim, B.; Jang, J.; Yu, H.T.; Kim, M.C.; Cho, J.Y.; Lee, C.J.; et al. Indoxyl sulfate (IS)-mediated immune dysfunction provokes endothelial damage in patients with end-stage renal disease (ESRD). Sci Rep 2017, 7, 3057. [Google Scholar] [CrossRef] [PubMed]
- Sela, S.; Shurtz-Swirski, R.; Cohen-Mazor, M.; Mazor, R.; Chezar, J.; Shapiro, G.; Hassan, K.; Shkolnik, G.; Geron, R.; Kristal, B. Primed peripheral polymorphonuclear leukocyte: A culprit underlying chronic low-grade inflammation and systemic oxidative stress in chronic kidney disease. J Am Soc Nephrol 2005, 16, 2431–2438. [Google Scholar] [CrossRef]
- Ishigami, J.; Jaar, B.G.; Rebholz, C.M.; Grams, M.E.; Michos, E.D.; Wolf, M.; Kovesdy, C.P.; Uchida, S.; Coresh, J.; Lutsey, P.L.; et al. Biomarkers of mineral and bone metabolism and 20-year risk of hospitalization with infection: The atherosclerosis risk in communities study. J Clin Endocrinol Metab 2017, 102, 4648–4657. [Google Scholar] [CrossRef]
| Phenotypic criteria | Etiologic criteria | ||||
| Involuntary weight loss (%) | Low BMI (kg/m2) | Reduced muscle mass | Reduced food intake or assimilation | Inflammation | |
| Moderate malnutrition | 5%−10% within the past 6 months, or 10%−20% beyond 6 months |
BMI < 18.5 kg/m2 for age < 70 years, BMI < 20 kg/m2 for age ≥ 70 years |
CC < 30.0 cm for men, CC < 29.0 cm for women |
50% of energy requirements > 1 week or any reduction in energy requirement for > 2 weeks or any chronic gastrointestinal condition that adversely impacts food assimilation or absorption |
Acute disease/injury or Chronic inflammatory disease or CRP level > 5 mg/L |
| Severe Malnutrition | >10% within the past 6 months, or >20% beyond 6 months |
BMI < 17.0 kg/m2 for age < 70 years, BMI < 17.8 kg/m2 for age ≥ 70 years |
CC < 27.0 cm for men, CC < 26.0 cm for women |
||
| All | Without malnutrition | With malnutrition (Moderate) |
With malnutrition (Severe) |
|
| Number | 1220 | 459 | 393 | 368 |
| Age (year) * | 80 (75-86) | 78 (72-84) | 81 (76-87) | 83 (77-88) |
| Male sex | 717 (58.8) | 297 (64.7) | 227 (57.8) | 193 (52.5) |
| Body mass index, kg/m2 * | 20.9 (18.8-23.2) | 22.4 (20.0-24.3)- | 20.1 (19.0-22.3) | 18.5 (17.0-20.6) |
| Serum albumin level (mg/dL) | 3.4 (3.0-3.9) | 3.5 (3.0–4.0) | 3.4 (3.0–3.9) | 3.4 (2.9–3.9) |
| CRP level (mg/dL) | 0.9 (0.2-4.9) | 0.7 (0.2-4.8) | 1.1 (0.2-5.1) | 0.8 (0.2-4.9) |
| eGFR (mL/min/1.73 m2) | 66 (43-84) | 66 (44–84) | 66 (44–83) | 65 (39–85) |
| eGFR group | ||||
| eGFR≥60 | 704 (57.7) | 262 (57.1) | 233 (59.3) | 209 (56.8) |
| eGFR 30-59 | 318 (26.1) | 131 (28.5) | 97 (24.7) | 90 (24.5) |
| eGFR<30 | 198 (16.2) | 66 (14.4) | 63 (16.0) | 69 (18.8) |
| Dialysis (hemodialysis or peritoneal dialysis) | 24 (2.0) | 11 (2.4) | 6 (1.5) | 7 (1.9) |
| Causes of infectious diseases | ||||
| Pneumonia * | 531 (43.5) | 160 (34.9) | 170 (43.3) | 201 (54.6) |
| Urinary tract | 90 (7.4) | 44 (9.6) | 23 (5.9) | 23 (6.3) |
| Gastrointestinal/liver/gall bladder | 180 (14.8) | 80 (17.4) | 70 (17.8) | 30 (8.2) |
| Skin/bone/muscle | 56 (4.6) | 29 (6.3) | 14 (3.6) | 13 (3.5) |
| Blood stream | 36 (3.0) | 13 (2.8) | 12 (3.1) | 11 (3.0) |
| Others | 327 (26.8) | 133 (29.0) | 104 (26.5) | 90 (24.5) |
| Comorbidities | ||||
| Diabetes mellitus* | 364 (29.8) | 125 (27.2) | 111 (28.2) | 128 (34.8) |
| COPD | 33 (2.7) | 9 (2.0) | 13 (3.3) | 11 (3.0) |
| Autoimmune disorders | 67 (5.5) | 28 (6.1) | 23 (5.9) | 16 (4.4) |
| Cardiovascular disease | 131 (10.7) | 43 (9.4) | 45 (11.5) | 43 (11.7) |
| Malignancy | 67 (5.5) | 24 (5.2) | 19 (4.8) | 24 (6.5) |
| Outcome | ||||
| Death * | 273 (22.4) | 66 (14.4) | 91 (23.2) | 116 (31.5) |
| Infection-related death * | 237 (86.8) | 52 (11.3) | 82 (20.9) | 103 (28.0) |
| Nutritional Status | |||
|---|---|---|---|
| Without | Moderate | Severe | |
| Incidence of mortality, n (%) | 66 (14.4) | 91 (23.2) | 116 (31.5) |
| Observation period (year) | 1.0 (0.2-1.6) | 0.5 (0.1-1.2) | 0.3 (0.1-1.2) |
| IR per 1000PY | 146.5 | 307.1 | 470.0 |
| Hazard ratio (95% CI) | |||
| Unadjusted model | 1.0 (reference) | 1.95 (1.42–2.68) * | 2.97 (2.20–4.03) * |
| Adjusted model 1 | 1.0 (reference) | 1.77 (1.29–2.44) * | 2.68 (1.96–3.66) * |
| Adjusted model 2 | 1.0 (reference) | 1.76 (1.28–2.42) * | 2.54 (1.86–3.48) * |
| Adjusted model 3 | 1.0 (reference) | 1.76 (1.28–2.42) * | 2.44 (1.78–3.33) * |
| All-Cause Mortality | |||
|---|---|---|---|
| Nutritional Status | eGFR Level | Unadjusted Model | Adjusted Model |
| Without malnutrition | ≥60 | 1.0 (reference) | 1.0 (reference) |
| 30-59 | 1.99 (1.10-3.61) * | 2.09 (1.15-3.79) * | |
| <30 | 3.62 (2.03-6.46) * | 3.94 (2.20-7.06) * | |
| With malnutrition (moderate/severe) | ≥60 | 2.92 (1.86-4.58) * | 2.58 (1.64–4.06) * |
| 30-59 | 3.98 (2.44-6.50) * | 3.49 (2.13–5.73) * | |
| <30 | 7.58 (4.76-12.07) * | 7.35 (4.57–11.8) * | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




