Submitted:
08 August 2023
Posted:
09 August 2023
You are already at the latest version
Abstract
Keywords:
Introduction
Abdominal migraine
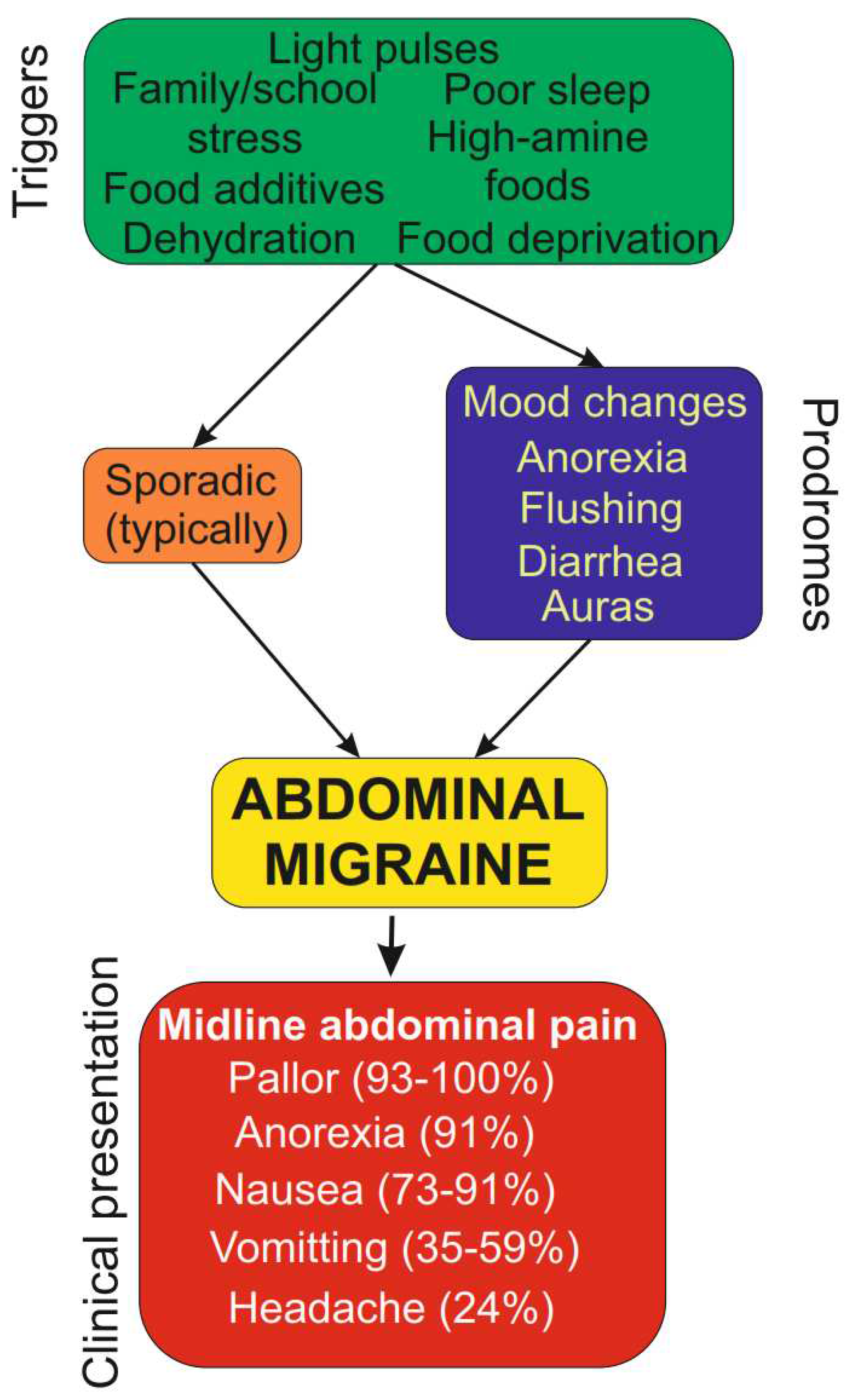
Triggers, diagnosis and clinical presentation
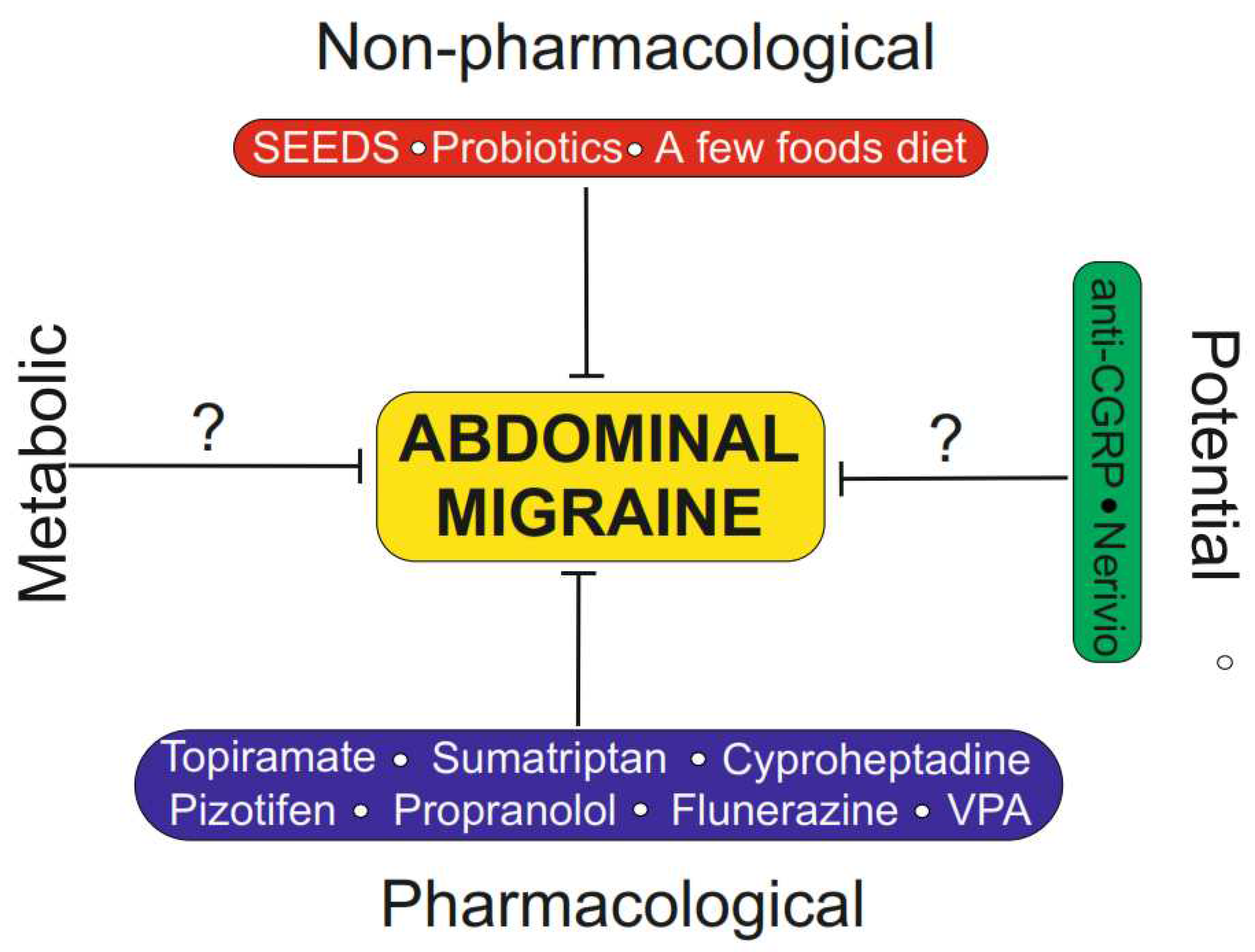
Treatment
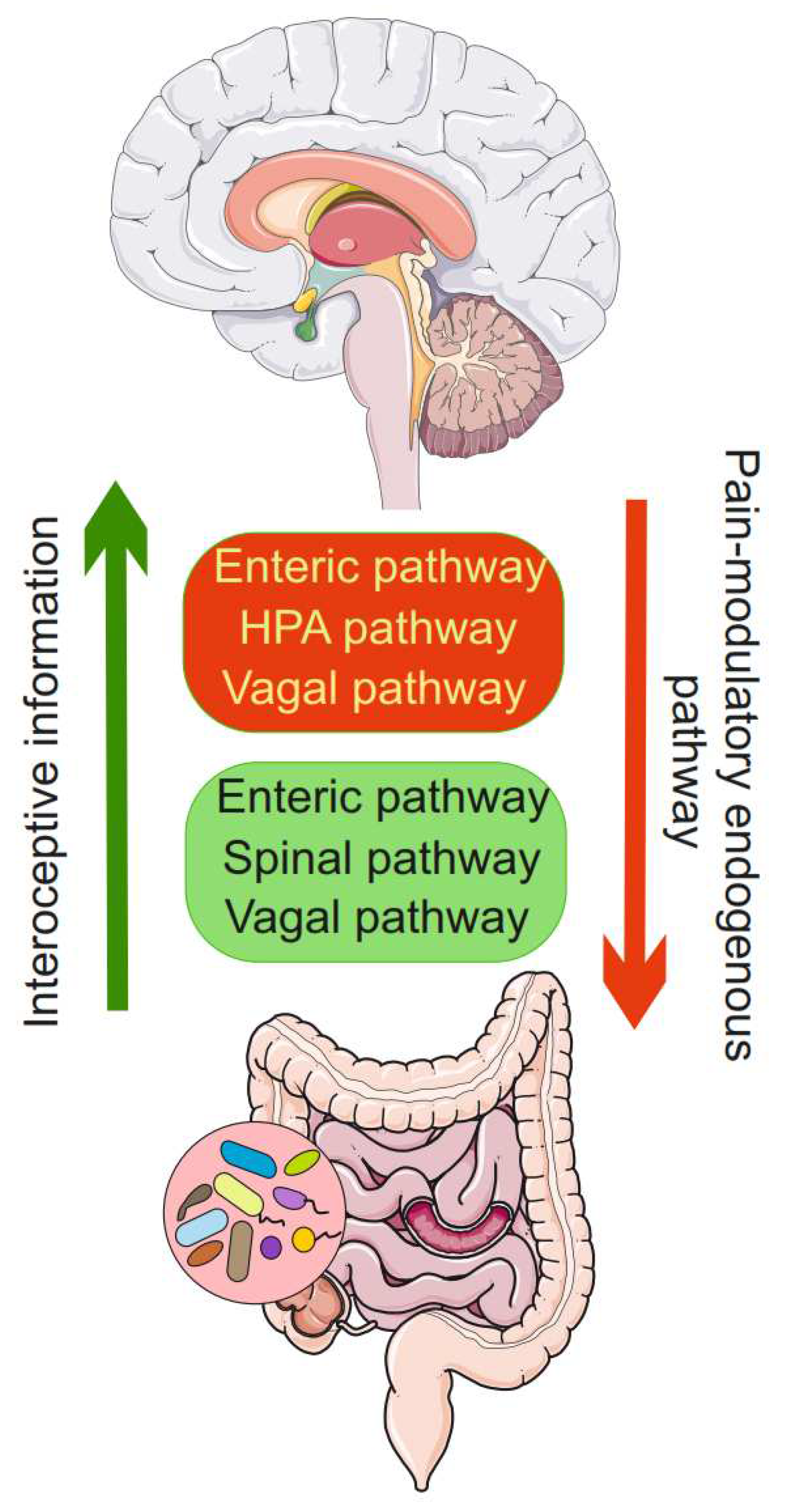
The gut-brain axis in migraine and functional gastrointestinal diseases
Metabolic abnormalities in migraine
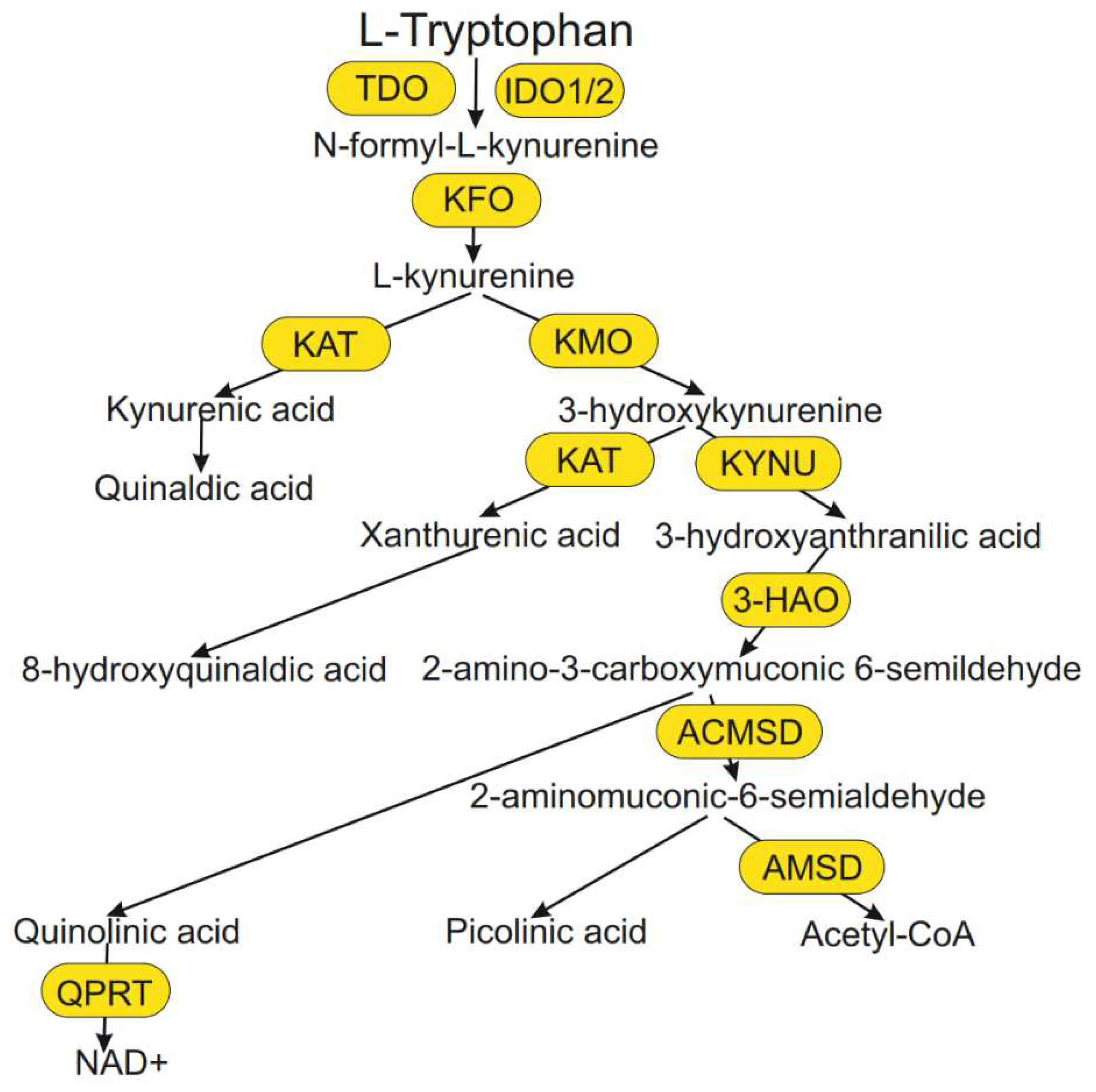
The kynurenine pathway of tryptophan metabolism and its role in the pathogenesis of migraine and functional gastrointestinal diseases
Obesity in children and its connection with migraine and the kynurenine pathway
Conclusions and perspectives
Author Contributions
Funding
Acknowledgements
Competing interest
Ethics approval and consent to participate
Consent for publication
Availability of data and materials
Abbreviations
References
- Azmy DJ, Qualia CM (2020) Review of abdominal migraine in children. Gastroenterol Hepatol (N Y) 16:632-639. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8132691/pdf/GH_16_632.pdf.
- Koppen IJ, Nurko S, Saps M, Di Lorenzo C, Benninga MA (2017) The pediatric rome iv criteria: What's new? Expert Rev Gastroenterol Hepatol 11:193-201. [CrossRef]
- Lenglar TL, Caula C, Moulding T, Lyles A, Wohrer D, Titomanlio L (2021) Brain to belly: Abdominal variants of migraine and functional abdominal pain disorders associated with migraine. J Neurogastroenterol Motil 27:482-494. [CrossRef]
- The international classification of headache disorders, 3rd edition (beta version) (2013). Cephalalgia 33:629-808. [CrossRef]
- Mani J, Madani S (2018) Pediatric abdominal migraine: Current perspectives on a lesser known entity. Pediatric Health Med Ther 9:47-58. [CrossRef]
- Abu-Arafeh I, Russell G (1995) Prevalence and clinical features of abdominal migraine compared with those of migraine headache. Arch Dis Child 72:413-417. [CrossRef]
- Al-Twaijri WA, Shevell MI (2002) Pediatric migraine equivalents: Occurrence and clinical features in practice. Pediatr Neurol 26:365-368. [CrossRef]
- Di Lorenzo C, Colletti RB, Lehmann HP, Boyle JT, Gerson WT, Hyams JS, Squires RH, Jr., Walker LS, Kanda PT (2005) Chronic abdominal pain in children: A technical report of the american academy of pediatrics and the north american society for pediatric gastroenterology, hepatology and nutrition. J Pediatr Gastroenterol Nutr 40:249-261. [CrossRef]
- Szperka CL, VanderPluym J, Orr SL, Oakley CB, Qubty W, Patniyot I, Lagman-Bartolome AM, Morris C, Gautreaux J, Victorio MC, Hagler S, Narula S, Candee MS, Cleves-Bayon C, Rao R, Fryer RH, Bicknese AR, Yonker M, Hershey AD, Powers SW, Goadsby PJ, Gelfand AA (2018) Recommendations on the use of anti-cgrp monoclonal antibodies in children and adolescents. Headache 58:1658-1669. [CrossRef]
- Lisicki M, Schoenen J (2020) Metabolic treatments of migraine. Expert Rev Neurother 20:295-302. [CrossRef]
- Gao K, Mu CL, Farzi A, Zhu WY (2020) Tryptophan metabolism: A link between the gut microbiota and brain. Adv Nutr 11:709-723. [CrossRef]
- Bosi A, Banfi D, Bistoletti M, Giaroni C, Baj A (2020) Tryptophan metabolites along the microbiota-gut-brain axis: An interkingdom communication system influencing the gut in health and disease. Int J Tryptophan Res 13:1178646920928984. [CrossRef]
- Erhardt S, Olsson SK, Engberg G (2009) Pharmacological manipulation of kynurenic acid: Potential in the treatment of psychiatric disorders. CNS Drugs 23:91-101. [CrossRef]
- Reinhard JF, Jr. (2004) Pharmacological manipulation of brain kynurenine metabolism. Ann N Y Acad Sci 1035:335-349. [CrossRef]
- Schwarcz R, Pellicciari R (2002) Manipulation of brain kynurenines: Glial targets, neuronal effects, and clinical opportunities. J Pharmacol Exp Ther 303:1-10. [CrossRef]
- Cervenka I, Agudelo LZ, Ruas JL (2017) Kynurenines: Tryptophan's metabolites in exercise, inflammation, and mental health. Science (New York, NY) 357. [CrossRef]
- Drummond PD (2006) Tryptophan depletion increases nausea, headache and photophobia in migraine sufferers. Cephalalgia 26:1225-1233. [CrossRef]
- Razeghi Jahromi S, Togha M, Ghorbani Z, Hekmatdoost A, Khorsha F, Rafiee P, Shirani P, Nourmohammadi M, Ansari H (2019) The association between dietary tryptophan intake and migraine. Neurol Sci 40:2349-2355. [CrossRef]
- Steiner TJ, Stovner LJ (2023) Global epidemiology of migraine and its implications for public health and health policy. Nature Reviews Neurology 19:109-117. [CrossRef]
- Wöber-Bingöl C (2013) Epidemiology of migraine and headache in children and adolescents. Curr Pain Headache Rep 17:341. [CrossRef]
- Kienbacher C, Wöber C, Zesch HE, Hafferl-Gattermayer A, Posch M, Karwautz A, Zormann A, Berger G, Zebenholzer K, Konrad A, Wöber-Bingöl C (2006) Clinical features, classification and prognosis of migraine and tension-type headache in children and adolescents: A long-term follow-up study. Cephalalgia 26:820-830. [CrossRef]
- Ozge A, Saşmaz T, Buğdaycı R, Cakmak SE, Kurt A, Kaleağası SH, Siva A (2013) The prevalence of chronic and episodic migraine in children and adolescents. Eur J Neurol 20:95-101. [CrossRef]
- Abu-Arafeh I, Callaghan M (2004) Short migraine attacks of less than 2 h duration in children and adolescents. Cephalalgia 24:333-338. [CrossRef]
- McAbee GN, Morse AM, Assadi M (2016) Pediatric aspects of headache classification in the international classification of headache disorders-3 (ichd-3 beta version). Curr Pain Headache Rep 20:7. [CrossRef]
- Gelfand AA (2015) Episodic syndromes that may be associated with migraine: A.K.A. "The childhood periodic syndromes". Headache 55:1358-1364. [CrossRef]
- Bellini B, Arruda M, Cescut A, Saulle C, Persico A, Carotenuto M, Gatta M, Nacinovich R, Piazza FP, Termine C, Tozzi E, Lucchese F, Guidetti V (2013) Headache and comorbidity in children and adolescents. J Headache Pain 14:79. [CrossRef]
- Farello G, Ferrara P, Antenucci A, Basti C, Verrotti A (2017) The link between obesity and migraine in childhood: A systematic review. Ital J Pediatr 43:27. [CrossRef]
- Tietjen GE, Brandes JL, Peterlin BL, Eloff A, Dafer RM, Stein MR, Drexler E, Martin VT, Hutchinson S, Aurora SK, Recober A, Herial NA, Utley C, White L, Khuder SA (2010) Childhood maltreatment and migraine (part ii). Emotional abuse as a risk factor for headache chronification. Headache 50:32-41. [CrossRef]
- Youssef PE, Mack KJ (2020) Episodic and chronic migraine in children. Dev Med Child Neurol 62:34-41. [CrossRef]
- Cervellin G, Lippi G (2015) Abdominal migraine in the differential diagnosis of acute abdominal pain. Am J Emerg Med 33:864.e863-865. [CrossRef]
- Winner P (2016) Abdominal migraine. Semin Pediatr Neurol 23:11-13. [CrossRef]
- Dignan F, Abu-Arafeh I, Russell G (2001) The prognosis of childhood abdominal migraine. Arch Dis Child 84:415-418. [CrossRef]
- Bentley D, Kehely A, al-Bayaty M, Michie CA (1995) Abdominal migraine as a cause of vomiting in children: A clinician's view. J Pediatr Gastroenterol Nutr 21 Suppl 1:S49-51. [CrossRef]
- Mortimer MJ, Good PA (1990) The ver as a diagnostic marker for childhood abdominal migraine. Headache 30:642-645. [CrossRef]
- Good PA (1995) Neurologic investigations of childhood abdominal migraine: A combined electrophysiologic approach to diagnosis. J Pediatr Gastroenterol Nutr 21 Suppl 1:S44-48. [CrossRef]
- Lagman-Bartolome AM, Lay C (2015) Pediatric migraine variants: A review of epidemiology, diagnosis, treatment, and outcome. Curr Neurol Neurosci Rep 15:34. [CrossRef]
- Lanzi G, Balottin U, Fazzi E, Rosano FB (1983) The periodic syndrome in pediatric migraine sufferers. Cephalalgia 3 Suppl 1:91-93. [CrossRef]
- Bougea A, Spantideas N, Chrousos GP (2018) Stress management for headaches in children and adolescents: A review and practical recommendations for health promotion programs and well-being. J Child Health Care 22:19-33. [CrossRef]
- Robblee J, Starling AJ (2019) Seeds for success: Lifestyle management in migraine. Cleve Clin J Med 86:741-749. [CrossRef]
- Lee SY, Ryu HS, Choi SC, Jang SH (2020) A study of psychological factors associated with functional gastrointestinal disorders and use of health care. Clin Psychopharmacol Neurosci 18:580-586. [CrossRef]
- Devanarayana NM, Rajindrajith S, Perera MS, Nishanthanie SW, Karunanayake A, Benninga MA (2014) Association between functional gastrointestinal diseases and exposure to abuse in teenagers. J Trop Pediatr 60:386-392. [CrossRef]
- Fila M, Pawlowska E, Szczepanska J, Blasiak J (2023) Different aspects of aging in migraine. Aging and disease. [CrossRef]
- Russell G, Abu-Arafeh I, Symon DN (2002) Abdominal migraine: Evidence for existence and treatment options. Paediatr Drugs 4:1-8. [CrossRef]
- Newlove-Delgado TV, Martin AE, Abbott RA, Bethel A, Thompson-Coon J, Whear R, Logan S (2017) Dietary interventions for recurrent abdominal pain in childhood. Cochrane Database Syst Rev 3:Cd010972. [CrossRef]
- Symon DN, Russell G (1995) Double blind placebo controlled trial of pizotifen syrup in the treatment of abdominal migraine. Arch Dis Child 72:48-50. [CrossRef]
- Worawattanakul M, Rhoads JM, Lichtman SN, Ulshen MH (1999) Abdominal migraine: Prophylactic treatment and follow-up. J Pediatr Gastroenterol Nutr 28:37-40. [CrossRef]
- Kothare SV (2005) Efficacy of flunarizine in the prophylaxis of cyclical vomiting syndrome and abdominal migraine. Eur J Paediatr Neurol 9:23-26. [CrossRef]
- Kakisaka Y, Wakusawa K, Haginoya K, Saito A, Uematsu M, Yokoyama H, Sato T, Tsuchiya S (2010) Efficacy of sumatriptan in two pediatric cases with abdominal pain-related functional gastrointestinal disorders: Does the mechanism overlap that of migraine? J Child Neurol 25:234-237. [CrossRef]
- Raina M, Chelimsky G, Chelimsky T (2013) Intravenous dihydroergotamine therapy for pediatric abdominal migraines. Clin Pediatr (Phila) 52:918-921. [CrossRef]
- Corbo J (2003) The role of anticonvulsants in preventive migraine therapy. Curr Pain Headache Rep 7:63-66. [CrossRef]
- Tan V, Sahami AR, Peebles R, Shaw RJ (2006) Abdominal migraine and treatment with intravenous valproic acid. Psychosomatics 47:353-355. [CrossRef]
- Pearl NZ, Babin CP, Catalano NT, Blake JC, Ahmadzadeh S, Shekoohi S, Kaye AD (2023) Narrative review of topiramate: Clinical uses and pharmacological considerations. Adv Ther. [CrossRef]
- Hershey AD, Powers SW, Vockell AL, LeCates S, Kabbouche M (2002) Effectiveness of topiramate in the prevention of childhood headaches. Headache 42:810-818. [CrossRef]
- Hershey AD, Powers SW, Vockell AL, LeCates SL, Segers A, Kabbouche MA (2004) Development of a patient-based grading scale for pedmidas. Cephalalgia 24:844-849. [CrossRef]
- Kotb Elmala M, Suliman HA, Al-Shokary AH, Ibrahim AO, Kamal NM, Elshorbagy HH, Nasef KA, El Din Fathallah MG (2022) The impact of vitamin d(3) supplementation to topiramate therapy on pediatric migraine prophylaxis. J Child Neurol 37:833-839. [CrossRef]
- Arzani M, Jahromi SR, Ghorbani Z, Vahabizad F, Martelletti P, Ghaemi A, Sacco S, Togha M (2020) Gut-brain axis and migraine headache: A comprehensive review. J Headache Pain 21:15. [CrossRef]
- Fan PC, Kuo PH, Chang SH, Lee WT, Wu RM, Chiou LC (2009) Plasma calcitonin gene-related peptide in diagnosing and predicting paediatric migraine. Cephalalgia 29:883-890. [CrossRef]
- Fan PC, Kuo PH, Lee MT, Chang SH, Chiou LC (2019) Plasma calcitonin gene-related peptide: A potential biomarker for diagnosis and therapeutic responses in pediatric migraine. Front Neurol 10:10. [CrossRef]
- Gallai V, Sarchielli P, Floridi A, Franceschini M, Codini M, Glioti G, Trequattrini A, Palumbo R (1995) Vasoactive peptide levels in the plasma of young migraine patients with and without aura assessed both interictally and ictally. Cephalalgia 15:384-390. [CrossRef]
- Wang G, Tan T, Liu Y, Hong P (2020) Drugs for acute attack of pediatric migraine: A network meta-analysis of randomized controlled trials. Clin Neurol Neurosurg 195:105853. [CrossRef]
- Evers S (2022) Cgrp in childhood and adolescence migraine: (patho)physiological and clinical aspects. Curr Pain Headache Rep 26:475-480. [CrossRef]
- Fleming MA, 2nd, Ehsan L, Moore SR, Levin DE (2020) The enteric nervous system and its emerging role as a therapeutic target. Gastroenterol Res Pract 2020:8024171. [CrossRef]
- Furness JB, Callaghan BP, Rivera LR, Cho HJ (2014) The enteric nervous system and gastrointestinal innervation: Integrated local and central control. Advances in experimental medicine and biology 817:39-71. [CrossRef]
- Gwak MG, Chang SY (2021) Gut-brain connection: Microbiome, gut barrier, and environmental sensors. Immune Netw 21:e20. [CrossRef]
- Drewes AM, Olesen AE, Farmer AD, Szigethy E, Rebours V, Olesen SS (2020) Gastrointestinal pain. Nat Rev Dis Primers 6:1. [CrossRef]
- Mayer EA, Tillisch K (2011) The brain-gut axis in abdominal pain syndromes. Annu Rev Med 62:381-396. [CrossRef]
- Bielefeldt K, Christianson JA, Davis BM (2005) Basic and clinical aspects of visceral sensation: Transmission in the cns. Neurogastroenterol Motil 17:488-499. [CrossRef]
- Mayer EA, Naliboff BD, Craig AD (2006) Neuroimaging of the brain-gut axis: From basic understanding to treatment of functional gi disorders. Gastroenterology 131:1925-1942. [CrossRef]
- Porreca F, Ossipov MH, Gebhart GF (2002) Chronic pain and medullary descending facilitation. Trends Neurosci 25:319-325. [CrossRef]
- Berntson GG, Sarter M, Cacioppo JT (2003) Ascending visceral regulation of cortical affective information processing. Eur J Neurosci 18:2103-2109. [CrossRef]
- Aurora SK, Papapetropoulos S, Kori SH, Kedar A, Abell TL (2013) Gastric stasis in migraineurs: Etiology, characteristics, and clinical and therapeutic implications. Cephalalgia 33:408-415. [CrossRef]
- Devanarayana NM, Rajindrajith S, Benninga MA (2016) Abdominal migraine in children: Association between gastric motility parameters and clinical characteristics. BMC Gastroenterol 16:26. [CrossRef]
- Devanarayana NM, Rajindrajith S, Perera MS, Nishanthanie SW, Benninga MA (2013) Gastric emptying and antral motility parameters in children with functional dyspepsia: Association with symptom severity. J Gastroenterol Hepatol 28:1161-1166. [CrossRef]
- Shava U, Srivastava A, Mathias A, Kumar N, Yachha SK, Gambhir S, Poddar U (2021) Functional dyspepsia in children: A study of pathophysiological factors. J Gastroenterol Hepatol 36:680-686. [CrossRef]
- Parker A, Fonseca S, Carding SR (2020) Gut microbes and metabolites as modulators of blood-brain barrier integrity and brain health. Gut Microbes 11:135-157. [CrossRef]
- Chitkara DK, Camilleri M, Zinsmeister AR, Burton D, El-Youssef M, Freese D, Walker L, Stephens D (2005) Gastric sensory and motor dysfunction in adolescents with functional dyspepsia. J Pediatr 146:500-505. [CrossRef]
- Cucchiara S, Bortolotti M, Colombo C, Boccieri A, De Stefano M, Vitiello G, Pagano A, Ronchi A, Auricchio S (1991) Abnormalities of gastrointestinal motility in children with nonulcer dyspepsia and in children with gastroesophageal reflux disease. Dig Dis Sci 36:1066-1073. [CrossRef]
- Miller J, Khlevner J, Rodriguez L (2021) Upper gastrointestinal functional and motility disorders in children. Pediatr Clin North Am 68:1237-1253. [CrossRef]
- Riezzo G, Cucchiara S, Chiloiro M, Minella R, Guerra V, Giorgio I (1995) Gastric emptying and myoelectrical activity in children with nonulcer dyspepsia. Effect of cisapride. Dig Dis Sci 40:1428-1434. [CrossRef]
- Woodruff AE, Cieri NE, Abeles J, Seyse SJ (2013) Abdominal migraine in adults: A review of pharmacotherapeutic options. Ann Pharmacother 47:e27. [CrossRef]
- Borkum JM (2021) Brain energy deficit as a source of oxidative stress in migraine: A molecular basis for migraine susceptibility. Neurochem Res 46:1913-1932. [CrossRef]
- Rolfe DF, Brown GC (1997) Cellular energy utilization and molecular origin of standard metabolic rate in mammals. Physiological reviews 77:731-758. [CrossRef]
- Ashina M, Hansen JM, Do TP, Melo-Carrillo A, Burstein R, Moskowitz MA (2019) Migraine and the trigeminovascular system—40 years and counting. The Lancet Neurology 18:795-804. [CrossRef]
- Gazerani P (2020) Migraine and diet. Nutrients 12. [CrossRef]
- Gazerani P (2021) A bidirectional view of migraine and diet relationship. Neuropsychiatr Dis Treat 17:435-451. [CrossRef]
- Barbiroli B, Montagna P, Cortelli P, Funicello R, Iotti S, Monari L, Pierangeli G, Zaniol P, Lugaresi E (1992) Abnormal brain and muscle energy metabolism shown by 31p magnetic resonance spectroscopy in patients affected by migraine with aura. Neurology 42:1209-1214. [CrossRef]
- Montagna P, Cortelli P, Barbiroli B (1994) Magnetic resonance spectroscopy studies in migraine. Cephalalgia 14:184-193. [CrossRef]
- Lodi R, Iotti S, Cortelli P, Pierangeli G, Cevoli S, Clementi V, Soriani S, Montagna P, Barbiroli B (2001) Deficient energy metabolism is associated with low free magnesium in the brains of patients with migraine and cluster headache. Brain Res Bull 54:437-441. [CrossRef]
- Reyngoudt H, Paemeleire K, Descamps B, De Deene Y, Achten E (2011) 31p-mrs demonstrates a reduction in high-energy phosphates in the occipital lobe of migraine without aura patients. Cephalalgia 31:1243-1253. [CrossRef]
- Irwin S, Barmherzig R, Gelfand A (2017) Recurrent gastrointestinal disturbance: Abdominal migraine and cyclic vomiting syndrome. Curr Neurol Neurosci Rep 17:21. [CrossRef]
- Younis S, Hougaard A, Vestergaard MB, Larsson HBW, Ashina M (2017) Migraine and magnetic resonance spectroscopy: A systematic review. Curr Opin Neurol 30:246-262. [CrossRef]
- Kekelidze T, Khait I, Togliatti A, Benzecry JM, Wieringa B, Holtzman D (2001) Altered brain phosphocreatine and atp regulation when mitochondrial creatine kinase is absent. Journal of neuroscience research 66:866-872. [CrossRef]
- Belenguer P, Duarte JMN, Schuck PF, Ferreira GC (2019) Mitochondria and the brain: Bioenergetics and beyond. Neurotoxicity Research 36:219-238. [CrossRef]
- Fila M, Pawłowska E, Blasiak J (2019) Mitochondria in migraine pathophysiology - does epigenetics play a role? Arch Med Sci 15:944-956. [CrossRef]
- Lisicki M, D'Ostilio K, Coppola G, Parisi V, de Noordhout AM, Magis D, Schoenen J, Scholtes F, Versijpt J (2019) Age related metabolic modifications in the migraine brain. Cephalalgia 39:978-987. [CrossRef]
- Eising E, de Vries B, Ferrari MD, Terwindt GM, van den Maagdenberg AM (2013) Pearls and pitfalls in genetic studies of migraine. Cephalalgia 33:614-625. [CrossRef]
- Eising E, Huisman SMH, Mahfouz A, Vijfhuizen LS, Anttila V, Winsvold BS, Kurth T, Ikram MA, Freilinger T, Kaprio J, Boomsma DI, van Duijn CM, Järvelin MR, Zwart JA, Quaye L, Strachan DP, Kubisch C, Dichgans M, Davey Smith G, Stefansson K, Palotie A, Chasman DI, Ferrari MD, Terwindt GM, de Vries B, Nyholt DR, Lelieveldt BPF, van den Maagdenberg A, Reinders MJT (2016) Gene co-expression analysis identifies brain regions and cell types involved in migraine pathophysiology: A gwas-based study using the allen human brain atlas. Human genetics 135:425-439. [CrossRef]
- Kaur S, Ali A, Siahbalaei Y, Ahmad U, Pandey AK, Singh B (2019) Could rs4379368 be a genetic marker for north indian migraine patients with aura?: Preliminary evidence by a replication study. Neuroscience letters 712:134482. [CrossRef]
- Zaki EA, Freilinger T, Klopstock T, Baldwin EE, Heisner KR, Adams K, Dichgans M, Wagler S, Boles RG (2009) Two common mitochondrial DNA polymorphisms are highly associated with migraine headache and cyclic vomiting syndrome. Cephalalgia 29:719-728. [CrossRef]
- Lisicki M, D'Ostilio K, Coppola G, Scholtes F, Maertens de Noordhout A, Parisi V, Schoenen J, Magis D (2018) Evidence of an increased neuronal activation-to-resting glucose uptake ratio in the visual cortex of migraine patients: A study comparing (18)fdg-pet and visual evoked potentials. J Headache Pain 19:49. [CrossRef]
- Plantone D, Pardini M, Rinaldi G (2021) Riboflavin in neurological diseases: A narrative review. Clin Drug Investig 41:513-527. [CrossRef]
- Bruijn J, Duivenvoorden H, Passchier J, Locher H, Dijkstra N, Arts WF (2010) Medium-dose riboflavin as a prophylactic agent in children with migraine: A preliminary placebo-controlled, randomised, double-blind, cross-over trial. Cephalalgia 30:1426-1434. [CrossRef]
- MacLennan SC, Wade FM, Forrest KM, Ratanayake PD, Fagan E, Antony J (2008) High-dose riboflavin for migraine prophylaxis in children: A double-blind, randomized, placebo-controlled trial. J Child Neurol 23:1300-1304. [CrossRef]
- Condò M, Posar A, Arbizzani A, Parmeggiani A (2009) Riboflavin prophylaxis in pediatric and adolescent migraine. J Headache Pain 10:361-365. [CrossRef]
- Aaseth J, Alexander J, Alehagen U (2021) Coenzyme q(10) supplementation - in ageing and disease. Mech Ageing Dev 197:111521. [CrossRef]
- Hershey AD, Powers SW, Vockell AL, Lecates SL, Ellinor PL, Segers A, Burdine D, Manning P, Kabbouche MA (2007) Coenzyme q10 deficiency and response to supplementation in pediatric and adolescent migraine. Headache 47:73-80. [CrossRef]
- Slater SK, Nelson TD, Kabbouche MA, LeCates SL, Horn P, Segers A, Manning P, Powers SW, Hershey AD (2011) A randomized, double-blinded, placebo-controlled, crossover, add-on study of coenzyme q10 in the prevention of pediatric and adolescent migraine. Cephalalgia 31:897-905. [CrossRef]
- Fila M, Chojnacki C, Chojnacki J, Blasiak J (2021) Nutrients to improve mitochondrial function to reduce brain energy deficit and oxidative stress in migraine. Nutrients 13. [CrossRef]
- Badawy AA (2017) Kynurenine pathway of tryptophan metabolism: Regulatory and functional aspects. Int J Tryptophan Res 10:1178646917691938. [CrossRef]
- Fukuwatari T (2020) Possibility of amino acid treatment to prevent the psychiatric disorders via modulation of the production of tryptophan metabolite kynurenic acid. Nutrients 12. [CrossRef]
- Hilmas C, Pereira EF, Alkondon M, Rassoulpour A, Schwarcz R, Albuquerque EX (2001) The brain metabolite kynurenic acid inhibits alpha7 nicotinic receptor activity and increases non-alpha7 nicotinic receptor expression: Physiopathological implications. J Neurosci 21:7463-7473. [CrossRef]
- Kessler M, Terramani T, Lynch G, Baudry M (1989) A glycine site associated with n-methyl-d-aspartic acid receptors: Characterization and identification of a new class of antagonists. J Neurochem 52:1319-1328. [CrossRef]
- Wang J, Simonavicius N, Wu X, Swaminath G, Reagan J, Tian H, Ling L (2006) Kynurenic acid as a ligand for orphan g protein-coupled receptor gpr35. The Journal of biological chemistry 281:22021-22028. [CrossRef]
- Burstein R, Yarnitsky D, Goor-Aryeh I, Ransil BJ, Bajwa ZH (2000) An association between migraine and cutaneous allodynia. 6: Ann Neurol 47.
- Liu YJ, Li YL, Fang ZH, Liao HL, Zhang YY, Lin J, Liu F, Shen JF (2022) Nmdars mediate peripheral and central sensitization contributing to chronic orofacial pain. Front Cell Neurosci 16:999509. [CrossRef]
- Curto M, Lionetto L, Negro A, Capi M, Fazio F, Giamberardino MA, Simmaco M, Nicoletti F, Martelletti P (2015) Altered kynurenine pathway metabolites in serum of chronic migraine patients. J Headache Pain 17:47. [CrossRef]
- Benbow T, Teja F, Sheikhi A, Exposto FG, Svensson P, Cairns BE (2022) Peripheral n-methyl-d-aspartate receptor activation contributes to monosodium glutamate-induced headache but not nausea behaviours in rats. Sci Rep 12:13894. [CrossRef]
- Kemp JA, Foster AC, Leeson PD, Priestley T, Tridgett R, Iversen LL, Woodruff GN (1988) 7-chlorokynurenic acid is a selective antagonist at the glycine modulatory site of the n-methyl-d-aspartate receptor complex. Proceedings of the National Academy of Sciences of the United States of America 85:6547-6550. [CrossRef]
- Chauvel V, Vamos E, Pardutz A, Vecsei L, Schoenen J, Multon S (2012) Effect of systemic kynurenine on cortical spreading depression and its modulation by sex hormones in rat. Exp Neurol 236:207-214. [CrossRef]
- Oláh G, Herédi J, Menyhárt A, Czinege Z, Nagy D, Fuzik J, Kocsis K, Knapp L, Krucsó E, Gellért L, Kis Z, Farkas T, Fülöp F, Párdutz A, Tajti J, Vécsei L, Toldi J (2013) Unexpected effects of peripherally administered kynurenic acid on cortical spreading depression and related blood-brain barrier permeability. Drug Des Devel Ther 7:981-987. [CrossRef]
- Tuka B, Nyári A, Cseh EK, Körtési T, Veréb D, Tömösi F, Kecskeméti G, Janáky T, Tajti J, Vécsei L (2021) Clinical relevance of depressed kynurenine pathway in episodic migraine patients: Potential prognostic markers in the peripheral plasma during the interictal period. J Headache Pain 22:60. [CrossRef]
- Hyams JS, Di Lorenzo C, Saps M, Shulman RJ, Staiano A, van Tilburg M (2016) Functional disorders: Children and adolescents. Gastroenterology. [CrossRef]
- Gelfand AA, Goadsby PJ, Allen IE (2015) The relationship between migraine and infant colic: A systematic review and meta-analysis. Cephalalgia 35:63-72. [CrossRef]
- Qubty W, Gelfand AA (2016) The link between infantile colic and migraine. Curr Pain Headache Rep 20:31. [CrossRef]
- Trivić I, Hojsak I (2018) Initial diagnosis of functional gastrointestinal disorders in children increases a chance for resolution of symptoms. Pediatr Gastroenterol Hepatol Nutr 21:264-270. [CrossRef]
- van Hemert S, Breedveld AC, Rovers JM, Vermeiden JP, Witteman BJ, Smits MG, de Roos NM (2014) Migraine associated with gastrointestinal disorders: Review of the literature and clinical implications. Front Neurol 5:241. [CrossRef]
- Zhang D, Zhang Y, Sang Y, Zheng N, Liu X (2019) The relationship between infant colic and migraine as well as tension-type headache: A meta-analysis. Pain Res Manag 2019:8307982. [CrossRef]
- Eminson DM (2007) Medically unexplained symptoms in children and adolescents. Clinical Psychology Review 27:855-871. [CrossRef]
- Apley J, Naish N (1958) Recurrent abdominal pains: A field survey of 1,000 school children. Arch Dis Child 33:165-170. [CrossRef]
- Myint K, Jacobs K, Myint A-M, Lam SK, Lim YA-L, Boey CC-M, Hoe SZ, Guillemin GJ (2021) Psychological stresses in children trigger cytokine- and kynurenine metabolite-mediated abdominal pain and proinflammatory changes. Frontiers in Immunology 12. [CrossRef]
- Burr RL, Gu H, Cain K, Djukovic D, Zhang X, Han C, Callan N, Raftery D, Heitkemper M (2019) Tryptophan metabolites in irritable bowel syndrome: An overnight time-course study. J Neurogastroenterol Motil 25:551-562. [CrossRef]
- Clarke G, McKernan DP, Gaszner G, Quigley EM, Cryan JF, Dinan TG (2012) A distinct profile of tryptophan metabolism along the kynurenine pathway downstream of toll-like receptor activation in irritable bowel syndrome. Front Pharmacol 3:90. [CrossRef]
- Kennedy PJ, Allen AP, O'Neill A, Quigley EM, Cryan JF, Dinan TG, Clarke G (2015) Acute tryptophan depletion reduces kynurenine levels: Implications for treatment of impaired visuospatial memory performance in irritable bowel syndrome. Psychopharmacology (Berl) 232:1357-1371. [CrossRef]
- Keszthelyi D, Troost FJ, Jonkers DM, Kruimel JW, Leue C, Masclee AA (2013) Decreased levels of kynurenic acid in the intestinal mucosa of ibs patients: Relation to serotonin and psychological state. J Psychosom Res 74:501-504. [CrossRef]
- Li P, Zheng J, Bai Y, Wang D, Cui Z, Li Y, Zhang J, Wang Y (2020) Characterization of kynurenine pathway in patients with diarrhea-predominant irritable bowel syndrome. Eur J Histochem 64. [CrossRef]
- Ramachandran R, Wang Z, Saavedra C, DiNardo A, Corr M, Powell SB, Yaksh TL (2019) Role of toll-like receptor 4 signaling in mast cell-mediated migraine pain pathway. Mol Pain 15:1744806919867842. [CrossRef]
- Chang FY, Lu CL (2013) Irritable bowel syndrome and migraine: Bystanders or partners? J Neurogastroenterol Motil 19:301-311. [CrossRef]
- Viera AJ, Hoag S, Shaughnessy J (2002) Management of irritable bowel syndrome. 1: Am Fam Physician 66, 1867.
- Chojnacki C, Poplawski T, Blonska A, Konrad P, Chojnacki J, Blasiak J (2023) The usefulness of the low-fodmap diet with limited tryptophan intake in the treatment of diarrhea-predominant irritable bowel syndrome. Nutrients 15. [CrossRef]
- Christmas DM, Badawy AA, Hince D, Davies SJ, Probert C, Creed T, Smithson J, Afzal M, Nutt DJ, Potokar JP (2010) Increased serum free tryptophan in patients with diarrhea-predominant irritable bowel syndrome. Nutr Res 30:678-688. [CrossRef]
- Sanyaolu A, Okorie C, Qi X, Locke J, Rehman S (2019) Childhood and adolescent obesity in the united states: A public health concern. Glob Pediatr Health 6:2333794x19891305. [CrossRef]
- Spinelli A, Buoncristiano M, Kovacs VA, Yngve A, Spiroski I, Obreja G, Starc G, Pérez N, Rito AI, Kunešová M, Sant'Angelo VF, Meisfjord J, Bergh IH, Kelleher C, Yardim N, Pudule I, Petrauskiene A, Duleva V, Sjöberg A, Gualtieri A, Hassapidou M, Hyska J, Burazeri G, Petrescu CH, Heinen M, Takacs H, Zamrazilová H, Bosi TB, Sacchini E, Pagkalos I, Cucu A, Nardone P, Gately P, Williams J, Breda J (2019) Prevalence of severe obesity among primary school children in 21 european countries. Obes Facts 12:244-258. [CrossRef]
- Dietz WH (1998) Health consequences of obesity in youth: Childhood predictors of adult disease. 5: Pediatrics 101.
- Kelsey MM, Zaepfel A, Bjornstad P, Nadeau KJ (2014) Age-related consequences of childhood obesity. Gerontology 60:222-228. [CrossRef]
- Rolland-Cachera MF, Deheeger M, Maillot M, Bellisle F (2006) Early adiposity rebound: Causes and consequences for obesity in children and adults. Int J Obes (Lond) 30 Suppl 4:S11-17. [CrossRef]
- Weiss R, Bremer AA, Lustig RH (2013) What is metabolic syndrome, and why are children getting it? Ann N Y Acad Sci 1281:123-140. [CrossRef]
- Engin A (2017) The definition and prevalence of obesity and metabolic syndrome. Advances in experimental medicine and biology 960:1-17. [CrossRef]
- Lister NB, Baur LA, Felix JF, Hill AJ, Marcus C, Reinehr T, Summerbell C, Wabitsch M (2023) Child and adolescent obesity. Nat Rev Dis Primers 9:24. [CrossRef]
- Bigal ME, Lipton RB (2006) Obesity is a risk factor for transformed migraine but not chronic tension-type headache. Neurology 67:252-257. [CrossRef]
- Verrotti A, Di Fonzo A, Agostinelli S, Coppola G, Margiotta M, Parisi P (2012) Obese children suffer more often from migraine. Acta Paediatr 101:e416-421. [CrossRef]
- Törk I (1990) Anatomy of the serotonergic system. Ann N Y Acad Sci 600:9-34; discussion 34-35. [CrossRef]
- van Galen KA, ter Horst KW, Serlie MJ (2021) Serotonin, food intake, and obesity. Obesity Reviews 22:e13210. [CrossRef]
- Ferrari MD, Odink J, Tapparelli C, Van Kempen GM, Pennings EJ, Bruyn GW (1989) Serotonin metabolism in migraine. Neurology 39:1239-1242. [CrossRef]
- Hamel E (2007) Serotonin and migraine: Biology and clinical implications. Cephalalgia 27:1293-1300. [CrossRef]
- Deen M, Christensen CE, Hougaard A, Hansen HD, Knudsen GM, Ashina M (2016) Serotonergic mechanisms in the migraine brain – a systematic review. Cephalalgia 37:251-264. [CrossRef]
- Humphrey PP (1991) 5-hydroxytryptamine and the pathophysiology of migraine. J Neurol 238 Suppl 1:S38-44. [CrossRef]
- Deen M, Hansen HD, Hougaard A, Nørgaard M, Eiberg H, Lehel S, Ashina M, Knudsen GM (2018) High brain serotonin levels in migraine between attacks: A 5-ht4 receptor binding pet study. NeuroImage: Clinical 18:97-102. [CrossRef]
- Pinhas-Hamiel O, Frumin K, Gabis L, Mazor-Aronovich K, Modan-Moses D, Reichman B, Lerner-Geva L (2008) Headaches in overweight children and adolescents referred to a tertiary-care center in israel. Obesity (Silver Spring) 16:659-663. [CrossRef]
- Moyer BJ, Rojas IY, Kerley-Hamilton JS, Hazlett HF, Nemani KV, Trask HW, West RJ, Lupien LE, Collins AJ, Ringelberg CS, Gimi B, Kinlaw WB, Tomlinson CR (2016) Inhibition of the aryl hydrocarbon receptor prevents western diet-induced obesity. Model for ahr activation by kynurenine via oxidized-ldl, tlr2/4, tgfβ, and ido1. Toxicology and Applied Pharmacology 300:13-24. [CrossRef]
- Lischka J, Schanzer A, Baumgartner M, de Gier C, Greber-Platzer S, Zeyda M (2022) Tryptophan metabolism is associated with bmi and adipose tissue mass and linked to metabolic disease in pediatric obesity. Nutrients 14:286. https://www.mdpi.com/2072-6643/14/2/286.
- Tan KM-L, Tint M-T, Kothandaraman N, Yap F, Godfrey KM, Lee YS, Tan KH, Gluckman PD, Chong Y-S, Chong MFF, Eriksson JG, Cameron-Smith D (2022) Association of plasma kynurenine pathway metabolite concentrations with metabolic health risk in prepubertal asian children. International Journal of Obesity 46:1128-1137. [CrossRef]
- Chojnacki C, Gąsiorowska A, Popławski T, Błońska A, Konrad P, Zajdler R, Chojnacki J, Blasiak J (2023) Reduced intake of dietary tryptophan improves beneficial action of budesonide in patients with lymphocytic colitis and mood disorders. Nutrients 15. [CrossRef]
- Chojnacki C, Gąsiorowska A, Popławski T, Konrad P, Chojnacki M, Fila M, Blasiak J (2023) Beneficial effect of increased tryptophan intake on its metabolism and mental state of the elderly. Nutrients 15. [CrossRef]
- Chojnacki C, Popławski T, Chojnacki J, Fila M, Konrad P, Blasiak J (2020) Tryptophan intake and metabolism in older adults with mood disorders. Nutrients 12. [CrossRef]
- Chojnacki C, Popławski T, Konrad P, Fila M, Błasiak J, Chojnacki J (2022) Antimicrobial treatment improves tryptophan metabolism and mood of patients with small intestinal bacterial overgrowth. Nutr Metab (Lond) 19:66. [CrossRef]
- Sandyk R (1992) L-tryptophan in neuropsychiatric disorders: A review. Int J Neurosci 67:127-144. [CrossRef]
- Wei L, Singh R, Ro S, Ghoshal UC (2021) Gut microbiota dysbiosis in functional gastrointestinal disorders: Underpinning the symptoms and pathophysiology. JGH Open 5:976-987. [CrossRef]
- Bai J, Shen N, Liu Y (2023) Associations between the gut microbiome and migraines in children aged 7-18 years: An analysis of the american gut project cohort. Pain Manag Nurs 24:35-43. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



