Submitted:
26 May 2023
Posted:
30 May 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Data source
2.2. Selection of study participants
2.3. Study design
2.4. Definition of outcomes
2.5. Statistical analysis
3. Results
3.1. Demographics
3.2. Incidence of NTM in ICS users
3.3. Risk of NTM in ICS users
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Adeloye, D.; Chua, S.; Lee, C.; Basquill, C.; Papana, A.; Theodoratou, E.; Nair, H.; Gasevic, D.; Sridhar, D.; Campbell, H.; et al. Global and regional estimates of COPD prevalence: Systematic review and meta-analysis. J Glob Health 2015, 5, 020415. [Google Scholar] [CrossRef] [PubMed]
- Collaborations, G.B.o.D.S. Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 2015, 385, 117–171. [Google Scholar] [CrossRef]
- Koarai, A.; Sugiura, H.; Yamada, M.; Ichikawa, T.; Fujino, N.; Kawayama, T.; Ichinose, M. Treatment with LABA versus LAMA for stable COPD: a systematic review and meta-analysis. BMC Pulm Med 2020, 20, 111. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.Y.; Chen, W.C.; Huang, C.H.; Hsiang, Y.P.; Sheu, C.C.; Chen, Y.C.; Lin, M.C.; Chu, K.A.; Lee, C.H.; Wei, Y.F. LABA/LAMA fixed-dose combinations versus LAMA monotherapy in the prevention of COPD exacerbations: a systematic review and meta-analysis. Ther Adv Respir Dis 2020, 14, 1753466620937194. [Google Scholar] [CrossRef]
- Martinez, F.J.; Rabe, K.F.; Ferguson, G.T.; Wedzicha, J.A.; Singh, D.; Wang, C.; Rossman, K.; St Rose, E.; Trivedi, R.; Ballal, S.; et al. Reduced All-Cause Mortality in the ETHOS Trial of Budesonide/Glycopyrrolate/Formoterol for Chronic Obstructive Pulmonary Disease. A Randomized, Double-Blind, Multicenter, Parallel-Group Study. Am J Respir Crit Care Med 2021, 203, 553–564. [Google Scholar] [CrossRef]
- Suissa, S.; Dell'Aniello, S.; Ernst, P. Comparative Effects of LAMA-LABA-ICS vs LAMA-LABA for COPD: Cohort Study in Real-World Clinical Practice. Chest 2020, 157, 846–855. [Google Scholar] [CrossRef]
- Cardoso, J.; Ferreira, A.J.; Guimarães, M.; Oliveira, A.S.; Simão, P.; Sucena, M. Treatable Traits in COPD - A Proposed Approach. Int J Chron Obstruct Pulmon Dis 2021, 16, 3167–3182. [Google Scholar] [CrossRef]
- Miravitlles, M.; Auladell-Rispau, A.; Monteagudo, M.; Vázquez-Niebla, J.C.; Mohammed, J.; Nuñez, A.; Urrútia, G. Systematic review on long-term adverse effects of inhaled corticosteroids in the treatment of COPD. Eur Respir Rev 2021, 30. [Google Scholar] [CrossRef]
- Park, S.C.; Kang, M.J.; Han, C.H.; Lee, S.M.; Kim, C.J.; Lee, J.M.; Kang, Y.A. Prevalence, incidence, and mortality of nontuberculous mycobacterial infection in Korea: a nationwide population-based study. BMC Pulm Med 2019, 19, 140. [Google Scholar] [CrossRef]
- Lee, H.; Myung, W.; Lee, E.M.; Kim, H.; Jhun, B.W. Mortality and Prognostic Factors of Nontuberculous Mycobacterial Infection in Korea: A Population-based Comparative Study. Clin Infect Dis 2021, 72, e610–e619. [Google Scholar] [CrossRef]
- Andréjak, C.; Nielsen, R.; Thomsen, V.; Duhaut, P.; Sørensen, H.T.; Thomsen, R.W. Chronic respiratory disease, inhaled corticosteroids and risk of non-tuberculous mycobacteriosis. Thorax 2013, 68, 256–262. [Google Scholar] [CrossRef] [PubMed]
- Brode, S.K.; Campitelli, M.A.; Kwong, J.C.; Lu, H.; Marchand-Austin, A.; Gershon, A.S.; Jamieson, F.B.; Marras, T.K. The risk of mycobacterial infections associated with inhaled corticosteroid use. Eur Respir J 2017, 50. [Google Scholar] [CrossRef] [PubMed]
- Cheol Seong, S.; Kim, Y.Y.; Khang, Y.H.; Heon Park, J.; Kang, H.J.; Lee, H.; Do, C.H.; Song, J.S.; Hyon Bang, J.; Ha, S.; et al. Data Resource Profile: The National Health Information Database of the National Health Insurance Service in South Korea. Int J Epidemiol 2017, 46, 799–800. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.H.; Kim, K.; Hyun, M.K.; Jang, E.J.; Lee, N.R.; Yim, J.J. Use of inhaled corticosteroids and the risk of tuberculosis. Thorax 2013, 68, 1105–1113. [Google Scholar] [CrossRef]
- Jeon, D. Infection Source and Epidemiology of Nontuberculous Mycobacterial Lung Disease. Tuberc Respir Dis (Seoul) 2019, 82, 94–101. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.J.; Oh, S.H.; Jeon, D.; Chang, C.L. Isolation and Antimicrobial Susceptibility of Nontuberculous Mycobacteria in a Tertiary Hospital in Korea, 2016 to 2020. Tuberc Respir Dis (Seoul) 2023, 86, 47–56. [Google Scholar] [CrossRef]
- Pathak, K.; Hart, S.; Lande, L. Nontuberculous Mycobacteria Lung Disease (NTM-LD): Current Recommendations on Diagnosis, Treatment, and Patient Management. Int J Gen Med 2022, 15, 7619–7629. [Google Scholar] [CrossRef] [PubMed]
- Winthrop, K.L.; Marras, T.K.; Adjemian, J.; Zhang, H.; Wang, P.; Zhang, Q. Incidence and Prevalence of Nontuberculous Mycobacterial Lung Disease in a Large U.S. Managed Care Health Plan, 2008-2015. Ann Am Thorac Soc 2020, 17, 178–185. [Google Scholar] [CrossRef]
- Andrejak, C.; Nielsen, R.; Thomsen, V.O.; Duhaut, P.; Sorensen, H.T.; Thomsen, R.W. Chronic respiratory disease, inhaled corticosteroids and risk of non-tuberculous mycobacteriosis. Thorax 2013, 68, 256–262. [Google Scholar] [CrossRef]
- Liu, V.X.; Winthrop, K.L.; Lu, Y.; Sharifi, H.; Nasiri, H.U.; Ruoss, S.J. Association between Inhaled Corticosteroid Use and Pulmonary Nontuberculous Mycobacterial Infection. Ann Am Thorac Soc 2018, 15, 1169–1176. [Google Scholar] [CrossRef]
- Shu, C.C.; Wei, Y.F.; Chen, K.H.; Chuang, S.; Wang, Y.H.; Wang, C.Y.; Wang, H.C. Inhaled Corticosteroids Increase Risk of Nontuberculous Mycobacterial Lung Disease: A Nested Case-Control Study and Meta-analysis. J Infect Dis 2022, 225, 627–636. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Q.; Li, S.; Zhou, W.; Yang, X.; Li, J.; Cao, J. Risk of Pneumonia with Different Inhaled Corticosteroids in COPD Patients: A Meta-Analysis. Copd 2020, 17, 462–469. [Google Scholar] [CrossRef] [PubMed]
- Belchamber, K.B.; Thomas, C.M.; Dunne, A.E.; Barnes, P.J.; Donnelly, L.E. Comparison of fluticasone propionate and budesonide on COPD macrophage and neutrophil function. Int J Chron Obstruct Pulmon Dis 2018, 13, 2883–2897. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.; Sun, J.; Huang, Q.; Liu, Y.; Yuan, M.; Ma, C.; Yan, H. Inhaled Corticosteroids and the Pneumonia Risk in Patients With Chronic Obstructive Pulmonary Disease: A Meta-analysis of Randomized Controlled Trials. Front Pharmacol 2021, 12, 691621. [Google Scholar] [CrossRef]
- Yu, I.; Park, S.; Hong, S.H.; Chang, M.S.; Lee, S.J.; Yong, S.J.; Lee, W.Y.; Kim, S.H.; Lee, J.H. Risk of Tuberculosis Caused by Fluticasone Propionate versus Budesonide in Chronic Obstructive Pulmonary Disease: A Nationwide Population-Based Study. J Pers Med 2022, 12. [Google Scholar] [CrossRef]
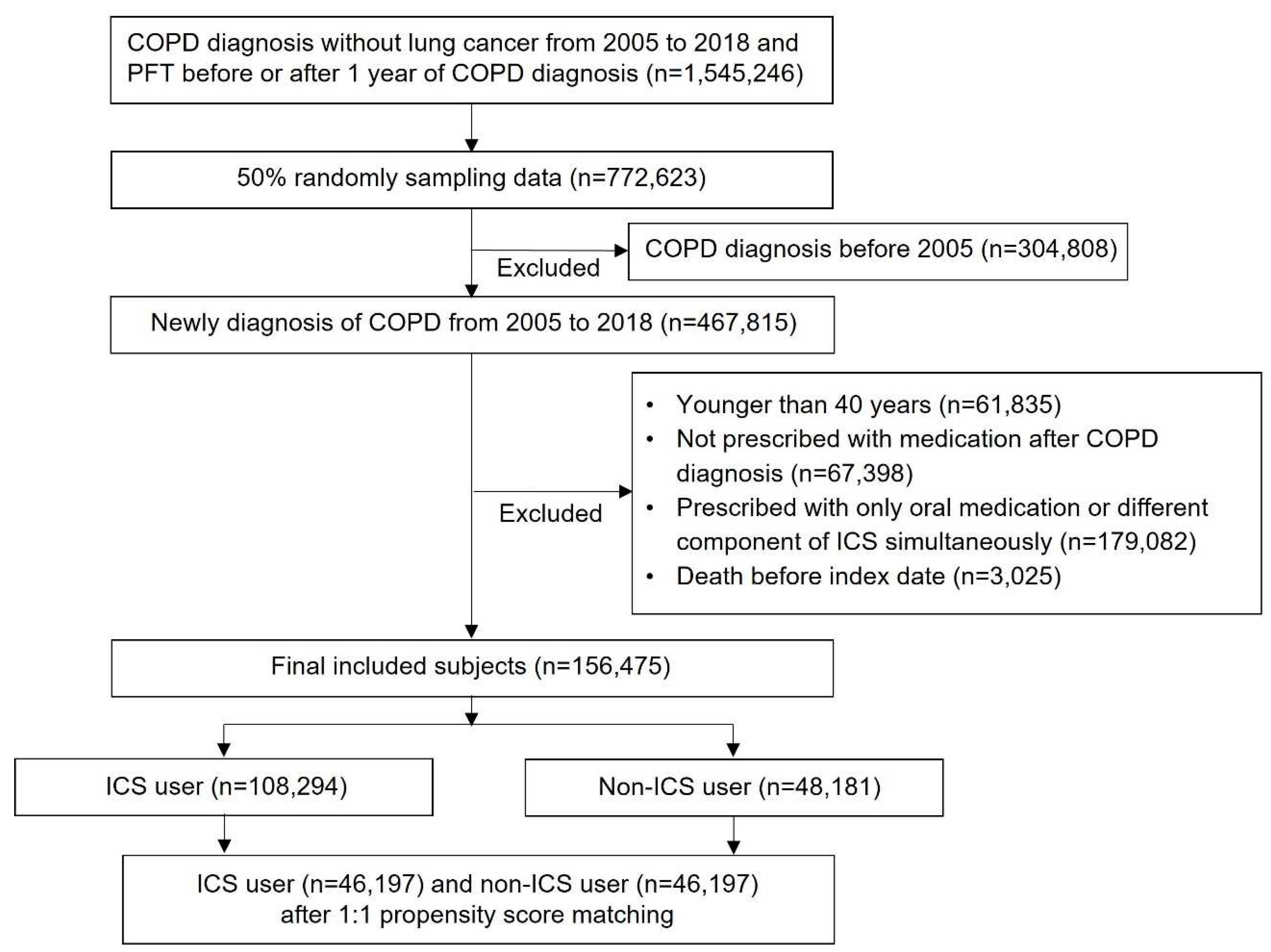
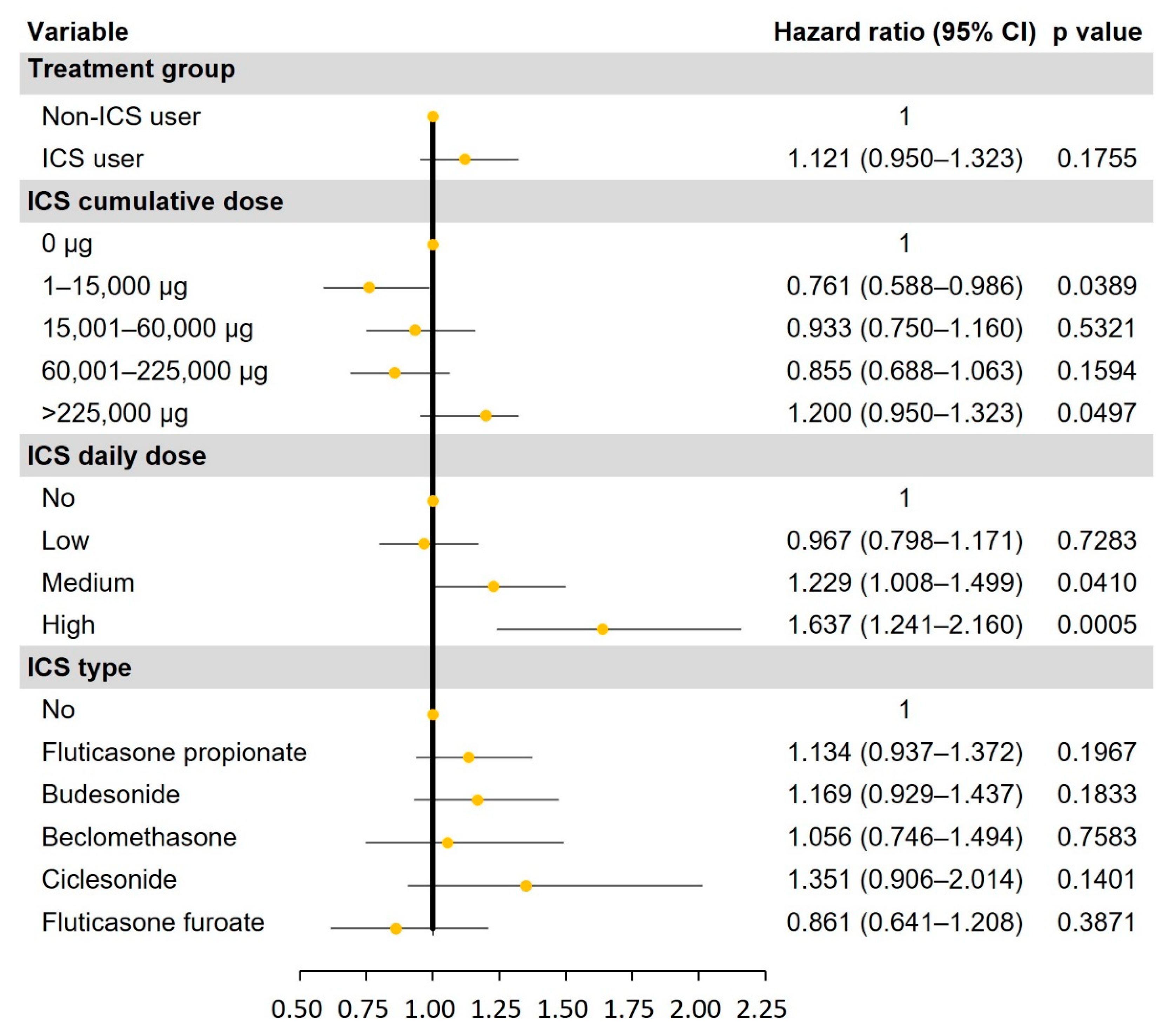
| ICS users (n=46,197) |
Non-ICS users (n= 46,197) |
p-value |
|||
| n | % | n | % | ||
| Age (years) | |||||
| Mean (SD) | 66.59(10.94) | 66.68(10.89) | 0.1860 | ||
| 40−49 | 3,348 | 7.25 | 3,315 | 7.18. | 0.3709 |
| 50−59 | 8,483 | 18.36 | 8,602 | 18.62 | |
| 60−69 | 14,467 | 31.32 | 14,661 | 31.74 | |
| 70−79 | 14,343 | 31.05 | 14,141 | 30.61 | |
| ≥ 80 | 5,556 | 12.03 | 5,478 | 11.86 | |
| Sex | |||||
| Male | 33,641 | 72.82 | 33,927 | 73.44 | 0.0338 |
| Female | 12,556 | 27.18 | 12,270 | 26.56 | |
| Comorbidity | |||||
| Bronchiectasis | 4,223 | 4.68 | 4,307 | 4.80 | 0.3398 |
| Diabetes | 16,028 | 17.77 | 15,935 | 17.76 | 0.5201 |
| Hypertension | 28,593 | 31.70 | 28,395 | 31.64 | 0.1803 |
| Heart failure | 10,531 | 11.68 | 10,497 | 11.69 | 0.7536 |
| Stroke | 11,369 | 12.60 | 11,233 | 12.52 | 0.2979 |
| Chronic kidney disease | 3,009 | 3.34 | 3,002 | 3.35 | 0.9256 |
| Chronic liver disease | 16,442 | 18.23 | 16,381 | 18.25 | 0.6750 |
| CCI | |||||
| Mean (SD) | 3.05 (2.09) | 3.10 (2.13) | <0.0001 | ||
| <2 | 12,644 | 27.37 | 12,050 | 26.08 | <0.0001 |
| ≥ 2 | 33,553 | 72.63 | 24,147 | 73.92 | |
| Bronchodilator | |||||
| SABA | 1,593 | 3.45 | 2,368 | 38.94 | <0.0001 |
| LAMA | 7,261 | 15.72 | 18,258 | 39.52 | <0.0001 |
| LABA | 37,871 | 68.99 | 2,421 | 5.24 | <0.0001 |
| LABA/LAMA | 5,472 | 11.84 | 12,150 | 26.30 | <0.0001 |
| Hospitalization before index date | |||||
| Yes | 2,950 | 6.39 | 2,426 | 5.25 | <0.0001 |
| No | 43,247 | 93.61 | 43,771 | 94.75 | |
| OCS prescription | |||||
| Yes | 34,764 | 75.25 | 34,416 | 74.50 | 0.0083 |
| No | 11,433 | 24.75 | 11,781 | 25.50 | |
| OCS prescription day | |||||
| Mean (SD) | 15.64 (26.86) | 6.07 (11.87) | <0.0001 | ||
| Interval from COPD diagnosis to index date | |||||
| Mean (SD) | 378.8 (842.4) | 400.9 (866.8) | <0.0001 | ||
| ICS use (n=46,197) | ||
| n | % | |
| ICS cumulative dose (μg) | ||
| Mean (SD) Median (Q1, Q3) |
242,280.8 (616,995.24) 60,000 (15,000, 225,000) |
|
| 0–5,000 | 11,751 | 25.77 |
| 15,001–60,000 | 11,749 | 25.77 |
| 60,001–225,000 | 10,814 | 23,72 |
| > 225,000 | 11,277 | 24.74 |
| ICS daily dose | ||
| Low | 26,919 | 59.04 |
| Medium | 15,202 | 33.34 |
| High | 3,470 | 7.61 |
| Type of ICS | ||
| Fluticasone propionate | 21,698 | 46.97 |
| Budesonide | 10,201 | 22.08 |
| Beclomethasone | 4,714 | 10.26 |
| Ciclesonide | 1,889 | 4.09 |
| Fluticasone furoate | 7,668 | 16.60 |
| Person year | NTM patients | Incidence rate (per 100,000) |
|
| Non-ICS users | 192202.11 | 440 | 228.93 |
| ICS users | 205324.15 | 495 | 241.08 |
| ICS cumulative dose (μg) | |||
| 0 – 15,000 | 35558.75 | 67 | 188.42 |
| 15,001 – 60,000 | 45879.23 | 99 | 215.78 |
| 60,001 – 225,000 | 48856.66 | 100 | 204.68 |
| > 225,000 | 71228.87 | 225 | 315.88 |
| ICS daily dose | |||
| Low | 105955.62 | 220 | 207.63 |
| Medium | 78401.15 | 205 | 261.48 |
| High | 17166.75 | 66 | 384.46 |
| Types of ICS | |||
| Fluticasone propionate | 116934.20 | 275 | 235.17 |
| Budesonide | 47242.98 | 114 | 241.31 |
| Beclomethasone | 15614.55 | 39 | 249.77 |
| Ciclesonide | 8499.94 | 26 | 305.88 |
| Fluticasone furoate | 17032.48 | 41 | 240.72 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




