Submitted:
15 May 2023
Posted:
16 May 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
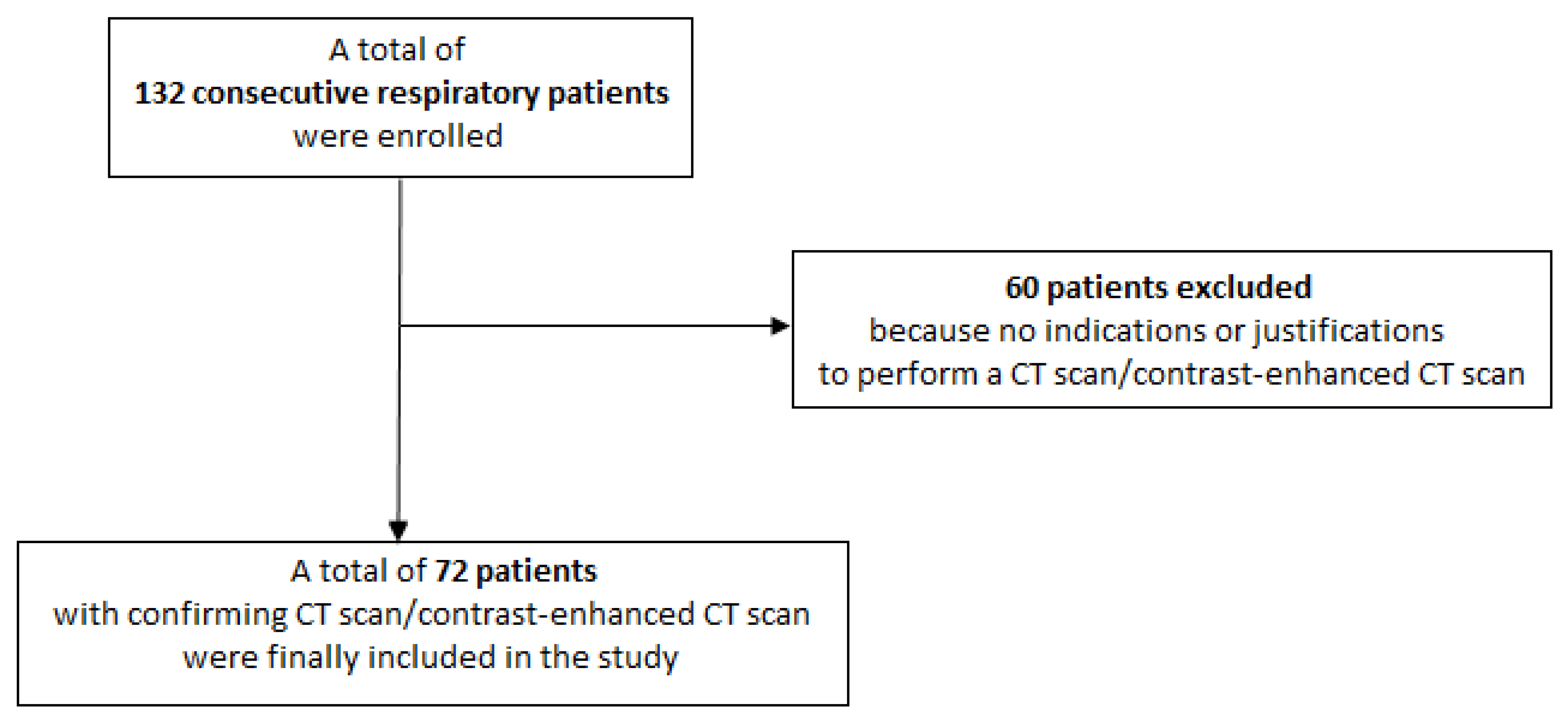
2.1. Patients Enrolment
2.2. Ultrasound Equipments
- -
- a high-end Esaote MyLab-Twice scanner (Esaote-Biomedica, Genoa, Italy) equipped with a low-mid frequency convex probe (3.5–5 MHz) and a high-definition linear transducer (8–12.5 MHz);
- -
- a wireless double-head linear (7.5-10 MHz) and convex (3,5-5 MHz) probe OTE-L/C501CD (OTE Medical, Cormano, MI) connected with a tablet-type display monitor on which the relative APP was installed.
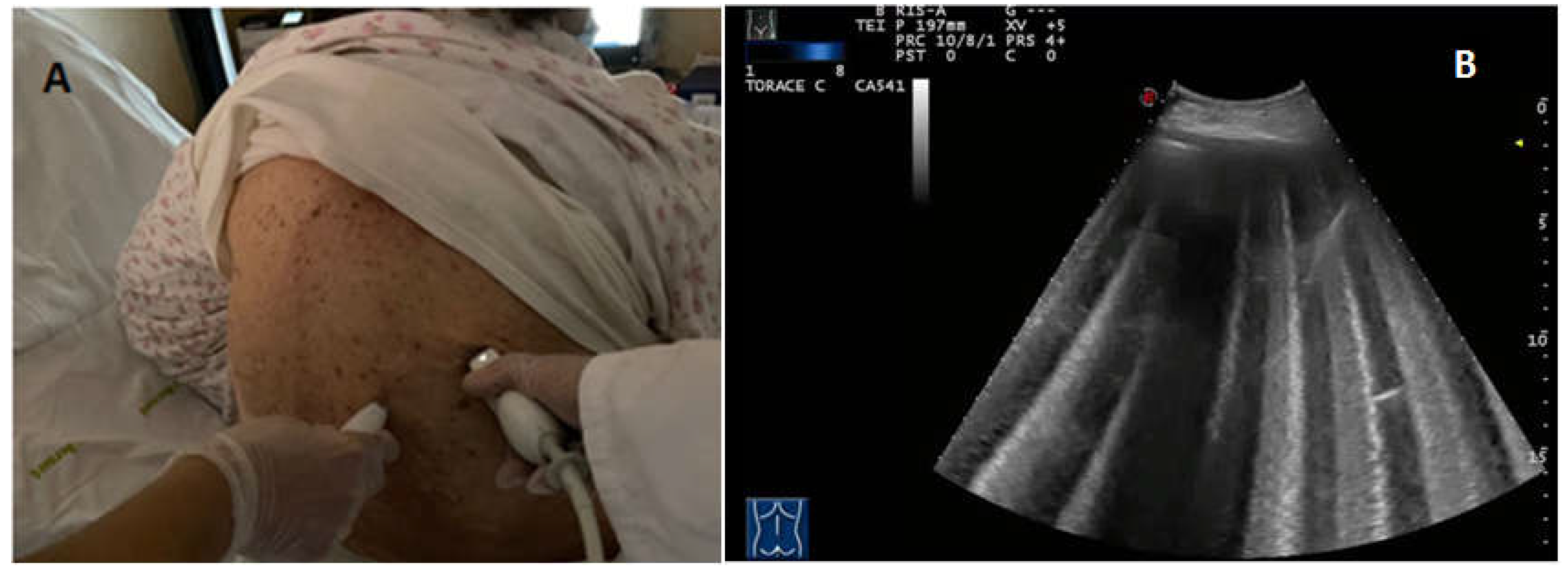
2.3. Examination Technique
2.4. Ultrasound findings definition
- -
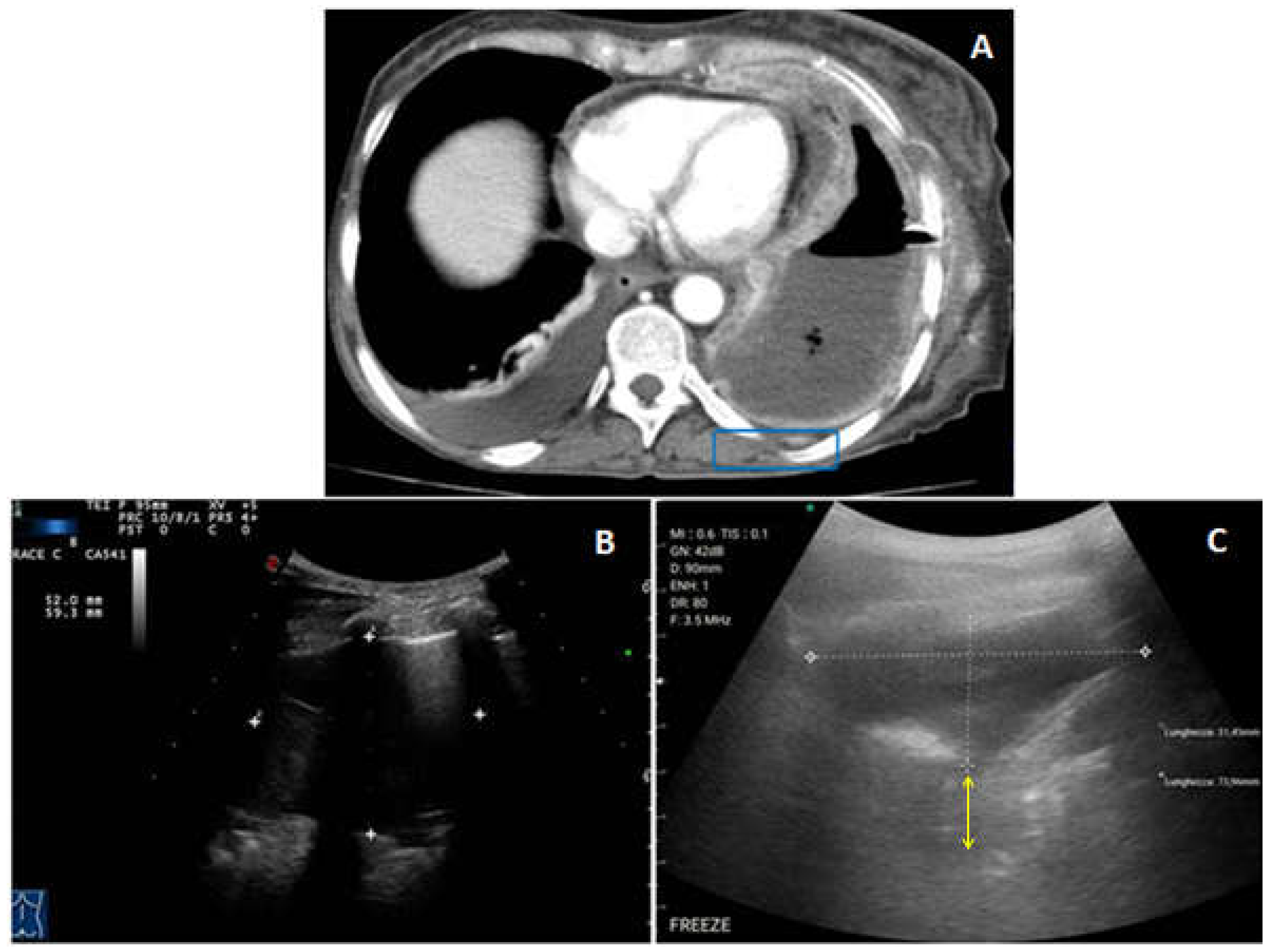
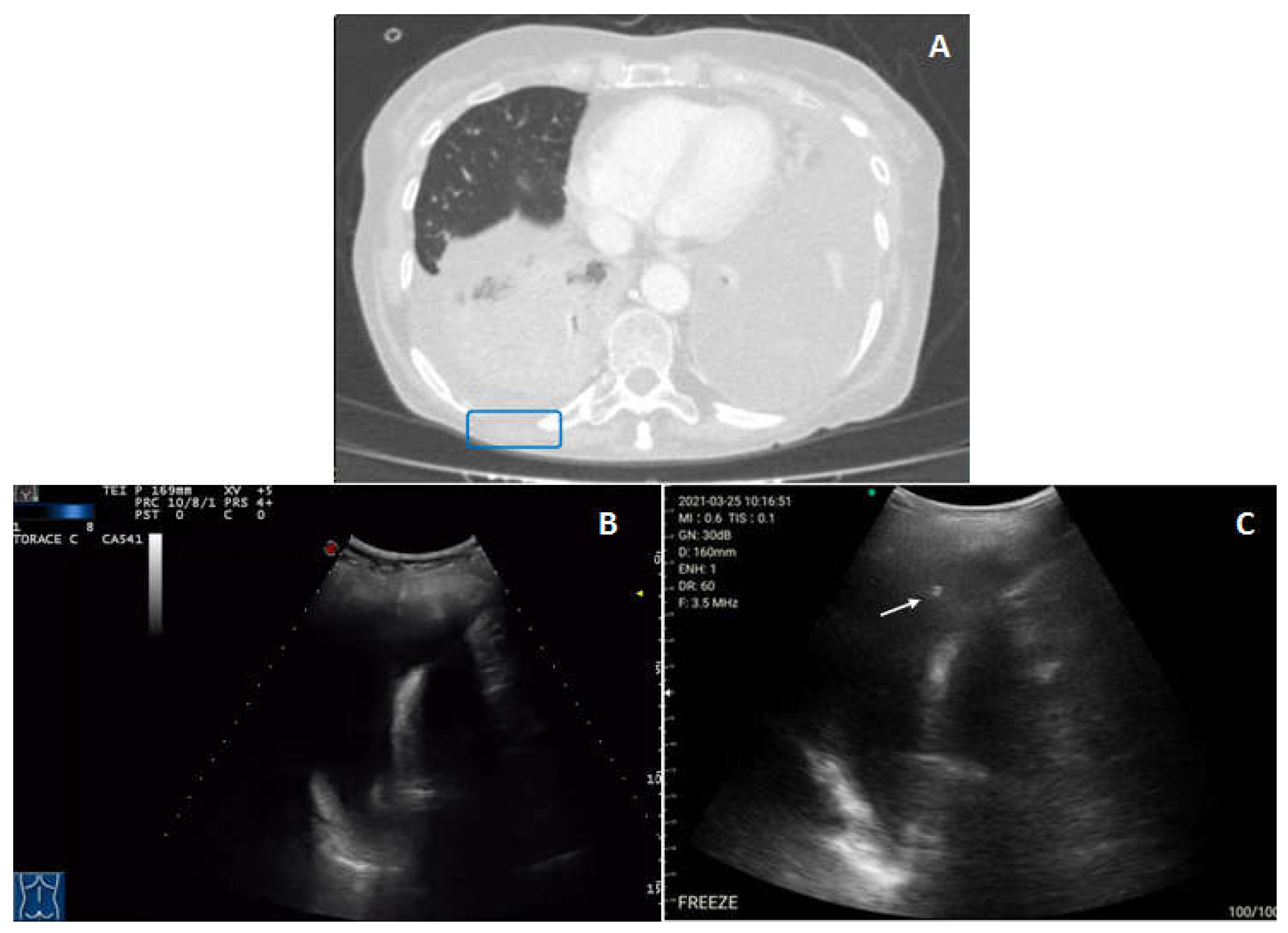
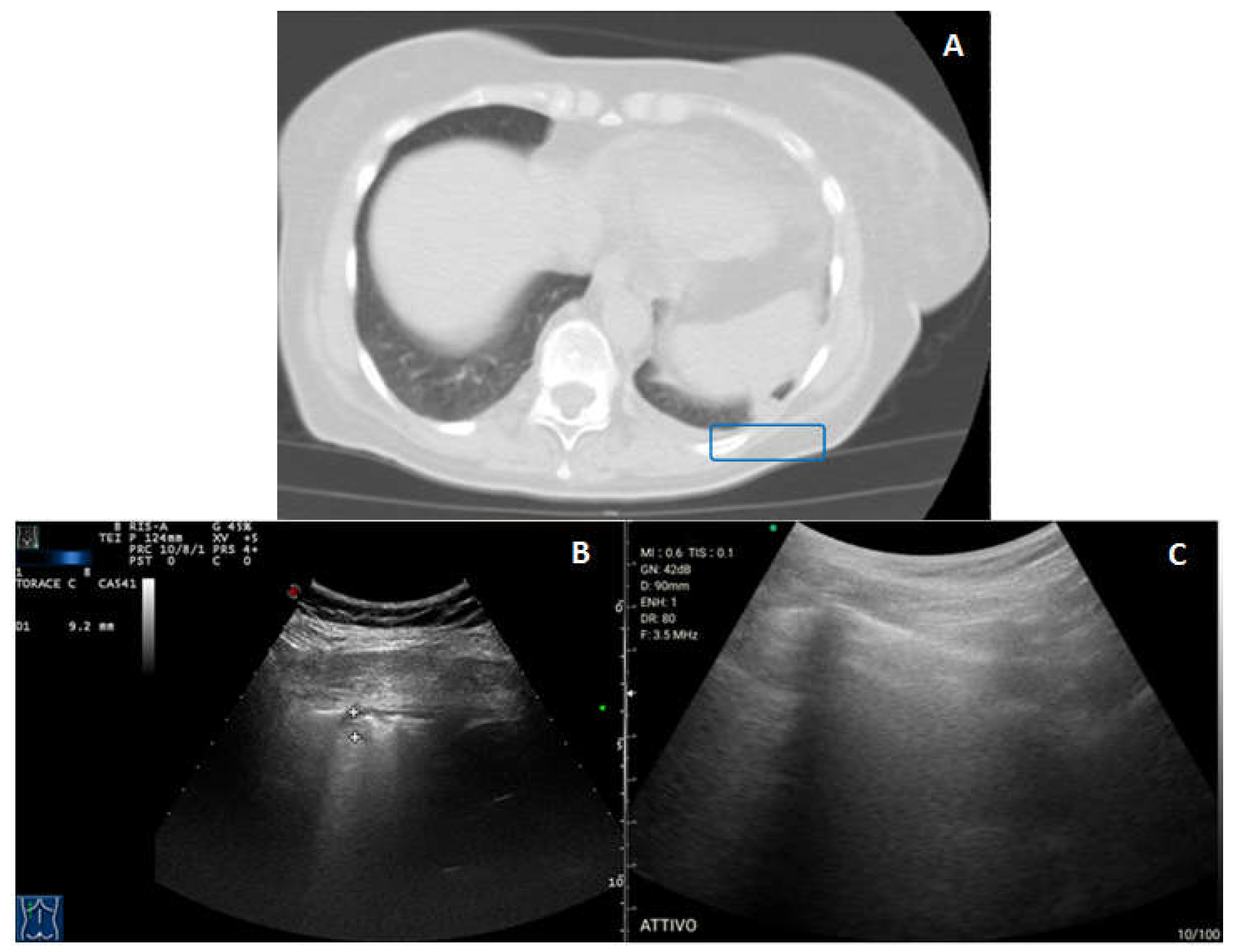
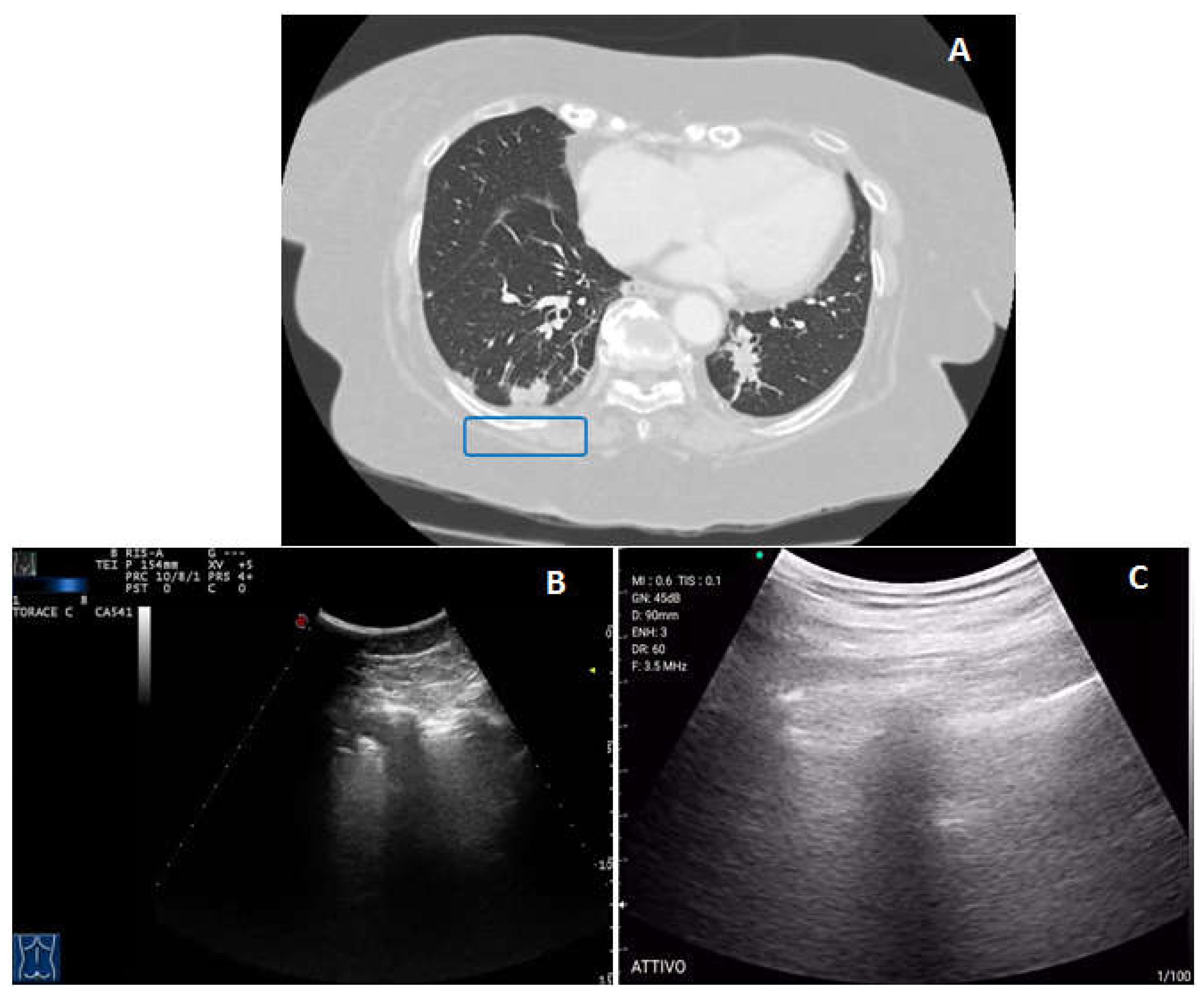
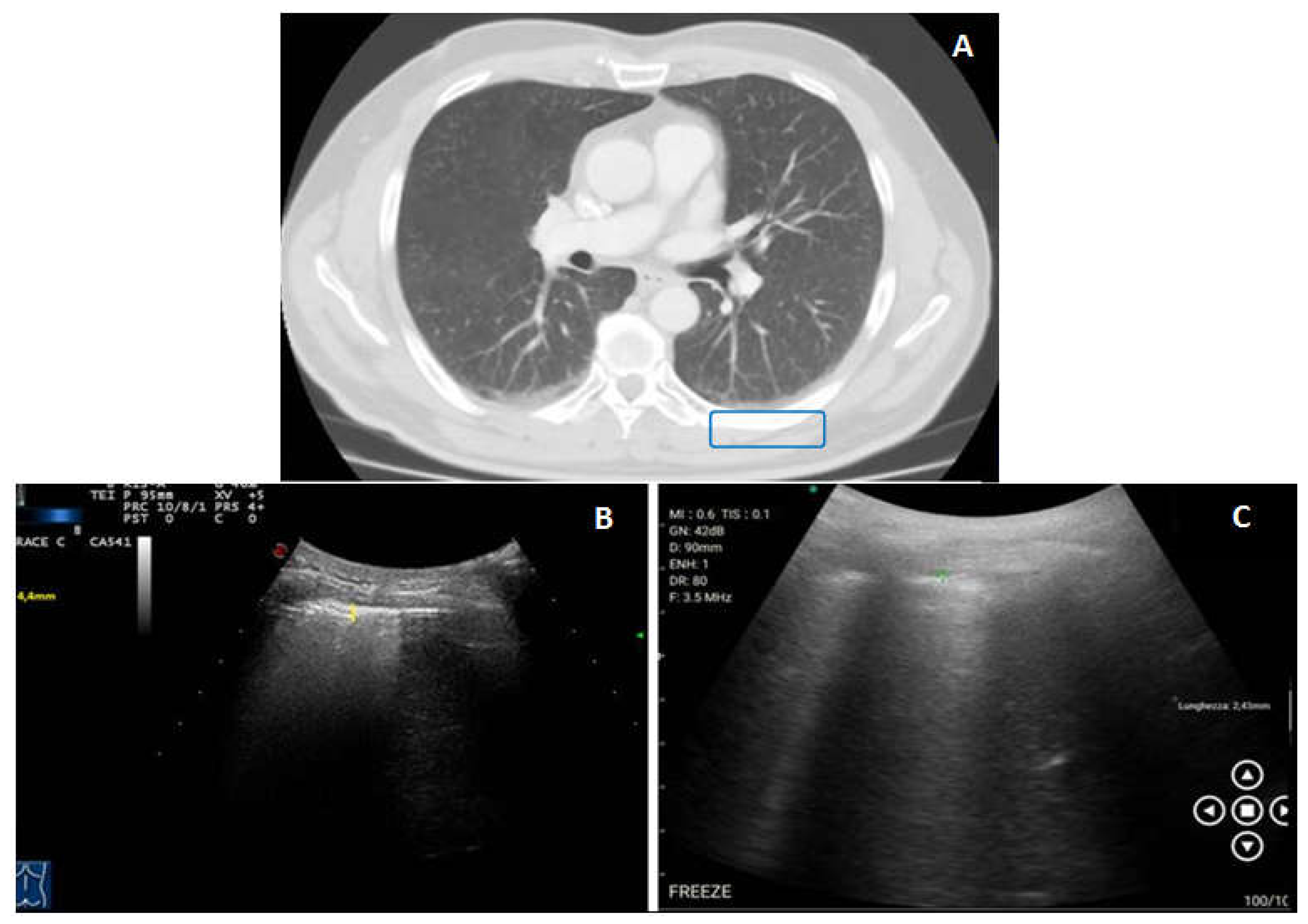
- Peripheral lung consolidations were defined as subpleural large hypoechoic or mixed hypo-hyperechoic areas interrupting the overlying pleural line echogenicity and characteristically showing blurred deep margins [1].
- -
- Pleural lesions were defined as focal hypoechoic or moderately echogenic pleural thickenings [1].
- -
- -
- Posterior pericardial effusion was defined as a build up of fluid in the space around the heart in a left anterior longitudinal scan [1].
2.5. Rating of the Image Quality
2.6. Statistical Analysis
3. Results
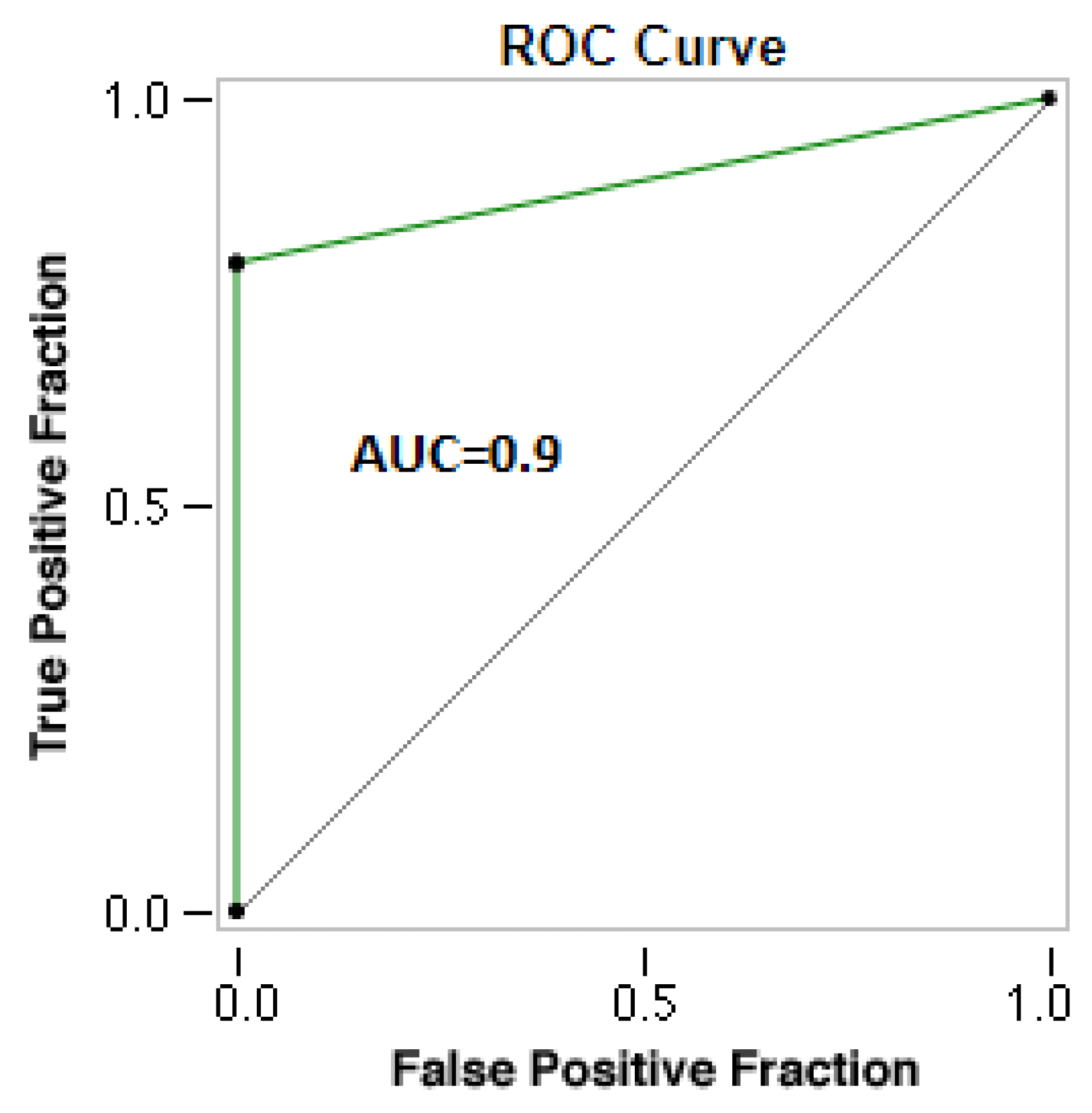
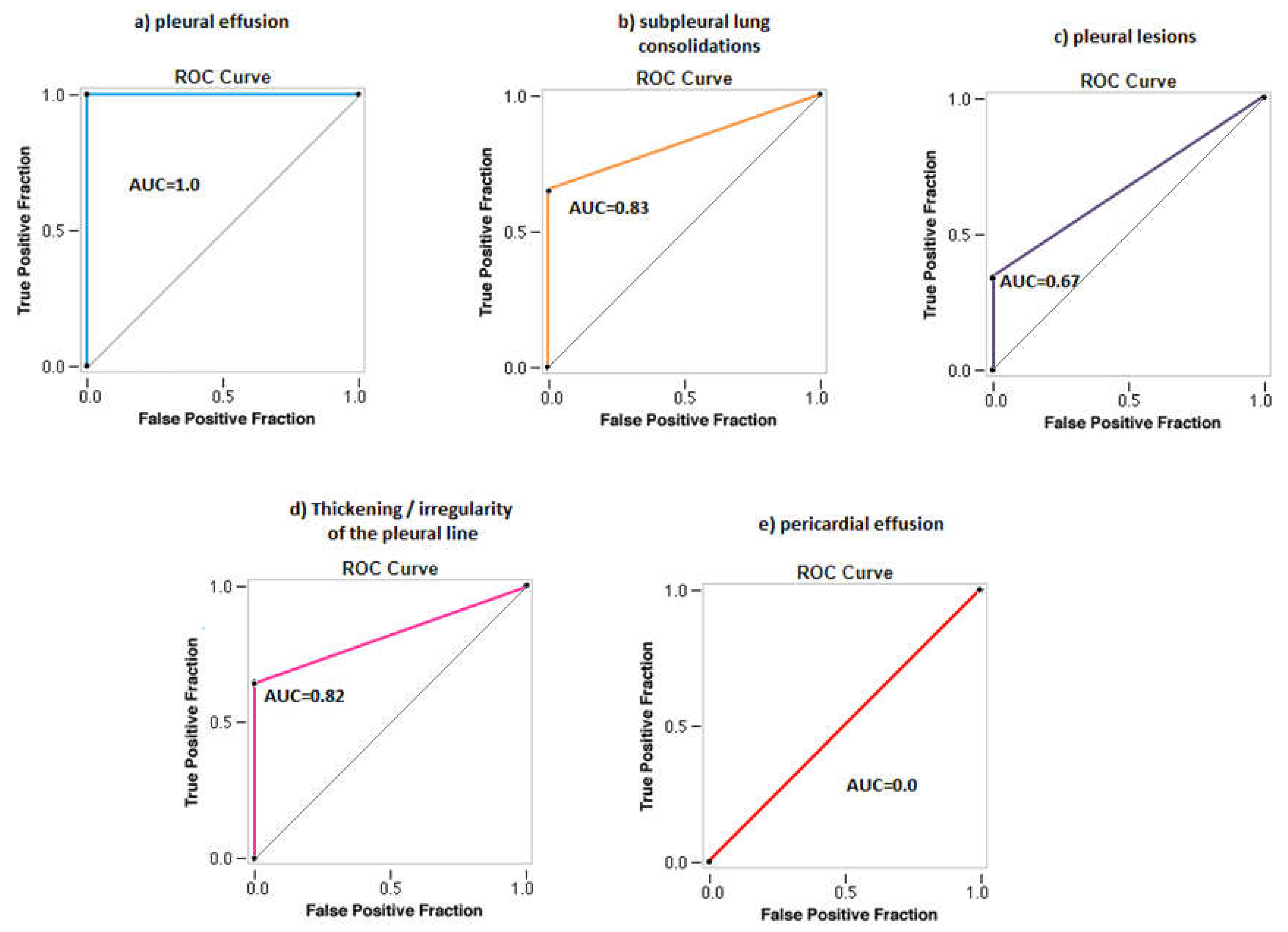
Diagnostic accuracy of the portable wireless ultrasound with respect to pleuro-pulmonary findings
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Sperandeo M, Rotondo A, Guglielmi G, Catalano D, Feragalli B, Trovato GM. Transthoracic ultrasound in the assessment of pleural and pulmonary diseases: use and limitations. Radiol Med. 2014;119(10):729-740. [CrossRef]
- Buda N, Kosiak W, Wełnicki M, et al. Recommendations for Lung Ultrasound in Internal Medicine. Diagnostics. 2020;10(8):597. [CrossRef]
- Yousefifard M, Baikpour M, Ghelichkhani P, et al. Screening Performance Characteristic of Ultrasonography and Radiography in Detection of Pleural Effusion; a Meta-Analysis. Emergency. 2016;4(1):1./pmc/articles/PMC4744606/. Accessed October 16, 2022.
- Sperandeo M, Maria C, Quarato I, et al. Effectiveness and Safety of Real-Time Transthoracic Ultrasound-Guided Thoracentesis. Diagnostics 2022, Vol 12, Page 725. 2022;12(3):725. [CrossRef]
- Sperandeo M, Maiello E, Graziano P, et al. Effectiveness and Safety of Transthoracic Ultrasound in Guiding Percutaneous Needle Biopsy in the Lung and Comparison vs. CT Scan in Assessing Morphology of Subpleural Consolidations. Diagnostics 2021, Vol 11, Page 1641. 2021;11(9):1641. [CrossRef]
- Whitson MR, Mayo PH. Ultrasonography in the emergency department. Crit Care. 2016;20(1):1-8. [CrossRef]
- Haji-Hassan M, Lenghel LM, Bolboacă SD. Hand-Held Ultrasound of the Lung: A Systematic Review. Diagnostics 2021, Vol 11, Page 1381. 2021;11(8):1381. [CrossRef]
- Stock KF, Klein B, Steubl D, et al. Comparison of a pocket-size ultrasound device with a premium ultrasound machine: diagnostic value and time required in bedside ultrasound examination. Abdom Imaging 2015 407. 2015;40(7):2861-2866. [CrossRef]
- Clark M, Ford C. Smartphone-, Tablet-, or App-Based Portable Ultrasound: A Review of Clinical Effectiveness. Smartphone-, Tablet-, or App-Based Portable Ultrasound A Rev Clin Eff. September 2019:1-6. https://www.ncbi.nlm.nih.gov/books/NBK549528/. Accessed October 11, 2022.
- Sperandeo M, De Cata A, Molinaro F, et al. Ultrasound signs of pulmonary fibrosis in systemic sclerosis as timely indicators for chest computed tomography. Scand J Rheumatol. 2015;44(5):389-398. [CrossRef]
- Lacedonia D, Scioscia G, Giardinelli A, et al. The Role of Transthoracic Ultrasound in the Study of Interstitial Lung Diseases: High-Resolution Computed Tomography Versus Ultrasound Patterns: Our Preliminary Experience. Diagnostics. 2021;11(3):439. [CrossRef]
- Fryback DG, Thornbury JR. The Efficacy of Diagnostic Imaging. Med Decis Mak. 1991;11(2):88-94. [CrossRef]
- Clevert DA, Schwarze V, Nyhsen C, D’Onofrio M, Sidhu P, Brady AP. ESR statement on portable ultrasound devices. Insights Imaging. 2019;10(1). [CrossRef]
- Jung EM, Dinkel J, Verloh N, et al. Wireless point-of-care ultrasound: First experiences with a new generation handheld device. Clin Hemorheol Microcirc. 2021;79(3):463. [CrossRef]
- Sperandeo M, Rea G. Interstitial Lung Diseases. In: Thoracic Ultrasound and Integrated Imaging. Cham: Springer International Publishing; 2020:61-82. [CrossRef]
- Scioscia G, Lacedonia D, Quarato CMI, et al. Could transthoracic ultrasound be useful to suggest a small airways disease in severe uncontrolled asthma? Ann Allergy, Asthma Immunol. 2022;129(4):461-466. [CrossRef]
- Muniz RT, Mesquita ET, Souza Junior CV, Martins W de A. Pulmonary ultrasound in patients with heart failure—Systematic review. Arq Bras Cardiol. 2018;110(6):577-584. [CrossRef]
- Ross DW, Abbasi MM, Jhaveri KD, et al. Lung ultrasonography in end-stage renal disease: Moving from evidence to practice-a narrative review. Clin Kidney J. 2018;11(2):172-178. [CrossRef]
- Abbasi S, Shaker H, Zareiee F, et al. Screening performance of Ultrasonographic B-lines in Detection of Lung Contusion following Blunt Trauma; a Diagnostic Accuracy Study. Emerg (Tehran, Iran). 2018;6(1):e55. http://www.ncbi.nlm.nih.gov/pubmed/30584571. Accessed January 17, 2021.
- Cortellaro F, Colombo S, Coen D, Duca PG. Lung ultrasound is an accurate diagnostic tool for the diagnosis of pneumonia in the emergency department. Emerg Med J. 2012;29(1):19-23. [CrossRef]
- Chaari A, Bousselmi K, Assar W, et al. Usefulness of ultrasound in the management of acute respiratory distress syndrome. Int J Crit Illn Inj Sci. 2019;9(1):11-15. [CrossRef]
- Sriram KB, Singh M. Lung ultrasound B-lines in exacerbations of chronic obstructive pulmonary disease. Intern Med J. 2017;47(3):324-327. [CrossRef]
- Attanasi M, Porreca A, Piloni F, et al. New application of point-of-care lung ultrasound in pediatric asthma exacerbations. In: European Respiratory Journal. Vol 56. European Respiratory Society (ERS); 2020:4179. [CrossRef]
- Carlino MV, Mancusi C, De Simone G, et al. Interstitial syndrome-lung ultrasound B lines: a potential marker for pulmonary metastases? A case series. Ital J Med. 2018;12(3):223-226. [CrossRef]
- Sperandeo M, Varriale A, Sperandeo G, et al. Assessment of ultrasound acoustic artifacts in patients with acute dyspnea: a multicenter study. Acta radiol. 2012;53(8):885-892. [CrossRef]
- Sperandeo M, Varriale A, Sperandeo G, et al. Characterization of the normal pulmonary surface and pneumonectomy space by reflected ultrasound. J Ultrasound. 2011;14(1):22-27. [CrossRef]
- Ciccarese F, Chiesa AM, Feletti F, et al. The Senile Lung as a Possible Source of Pitfalls on Chest Ultrasonography and Computed Tomography. Respiration. 2015;90(1):56-62. [CrossRef]
- Winter DH, Manzini M, Salge JM, et al. Aging of the Lungs in Asymptomatic Lifelong Nonsmokers: Findings on HRCT. Lung. 2015;193(2):283-290. [CrossRef]
- Quarato CMI, Venuti M, Sperandeo M. The artificial count of artifacts for thoracic ultrasound: what is the clinical usefulness? J Clin Monit Comput. 2020. [CrossRef]
- Rea G, Trovato GM. A Farewell to B-Lines: Ageing and Disappearance of Ultrasound Artifacts as a Diagnostic Tool. Respiration. 2015;90(6):522-522. [CrossRef]
| Findings | High-end US machine | Wireless US device | p-value |
|---|---|---|---|
| Pleural effusion | 28 (39%) | 28 (38%) | 1.00 |
| Pulmonary consolidation | 20 (28%) | 13 (18%) | 0.23 |
| Pleural lesion | 3 (4%) | 1 (1%) | 0.62 |
| Thickening/irregularity of the pleural line | 31 (43%) | 20 (28%) | 0.08 |
| Pericardial effusion | 3 (4%) | 0 (0%) | 0.24 |
| Variable | Prevalence | TP | FP | TN | FN | Sensitivity | Specificity |
|---|---|---|---|---|---|---|---|
| Pleural effusion | 28 (39%) | 28 | 0 | 44 | 0 | 100% (87.66-100.00%) | 100% (91.96-100.00%) |
| Pulmonary consolidation | 20 (28%) | 13 | 0 | 52 | 7 | 65% (40.78-84.61%) | 100% (93.15-100.00%) |
| Pleural lesion | 3 (4%) | 1 | 0 | 69 | 2 | 33% (0.84-90.57%) | 100% (94.79-100.00%) |
| Thickening/irregularity of the pleural line | 31 (43%) | 20 | 0 | 41 | 10 | 67% (47.19-82.71%) | 100% (91.40-100.00%) |
| Pericardial effusion | 3 (4%) | 0 | 0 | 69 | 3 | 0%(0.00-70.76%) | 100% (94.79-100.00%) |
| Overall findings | 64 (89%) | 51 | 0 | 8 | 13 | 79.69% (67.77-88.72%) | 100% (63.06-100.00%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




