Submitted:
15 May 2023
Posted:
16 May 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methods
2.1. Subjects
2.2. Glucose monitoring devices
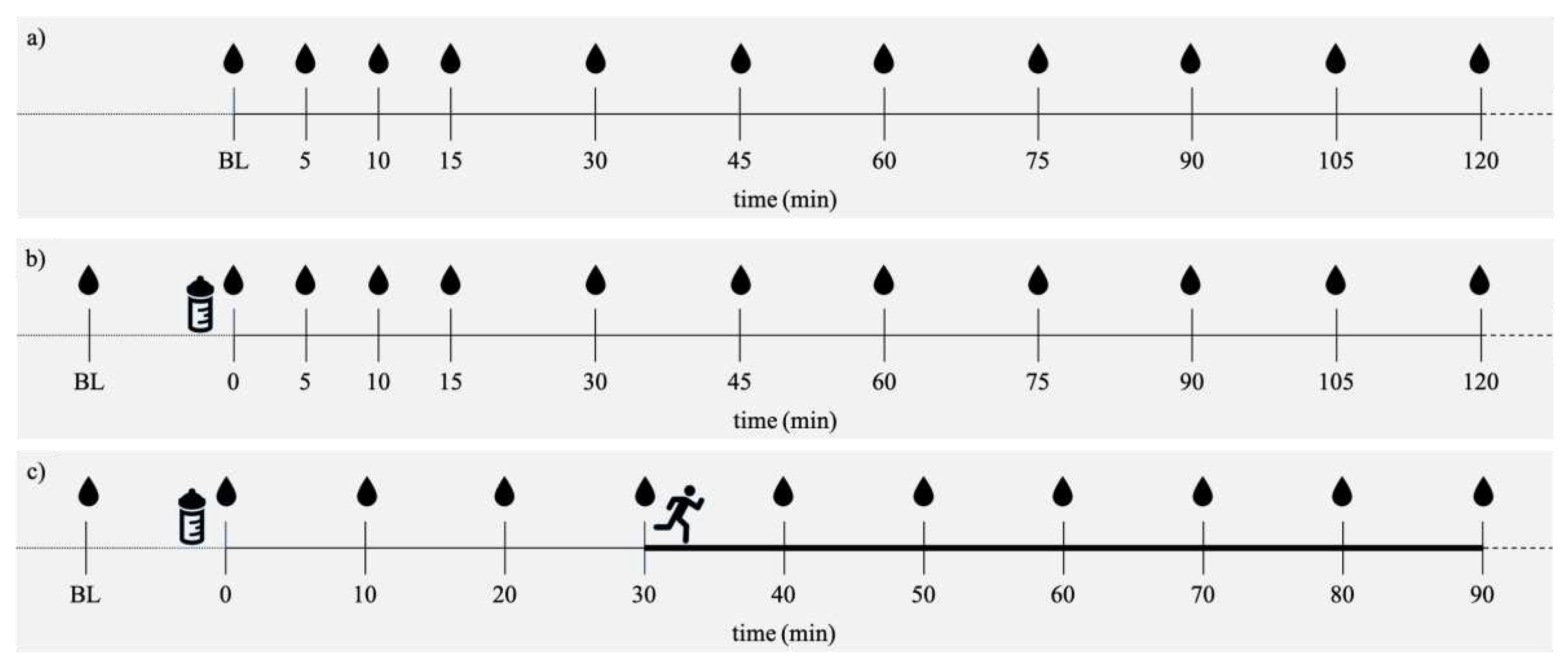
2.3. Test protocol
2.4. Data access and statistical analysis
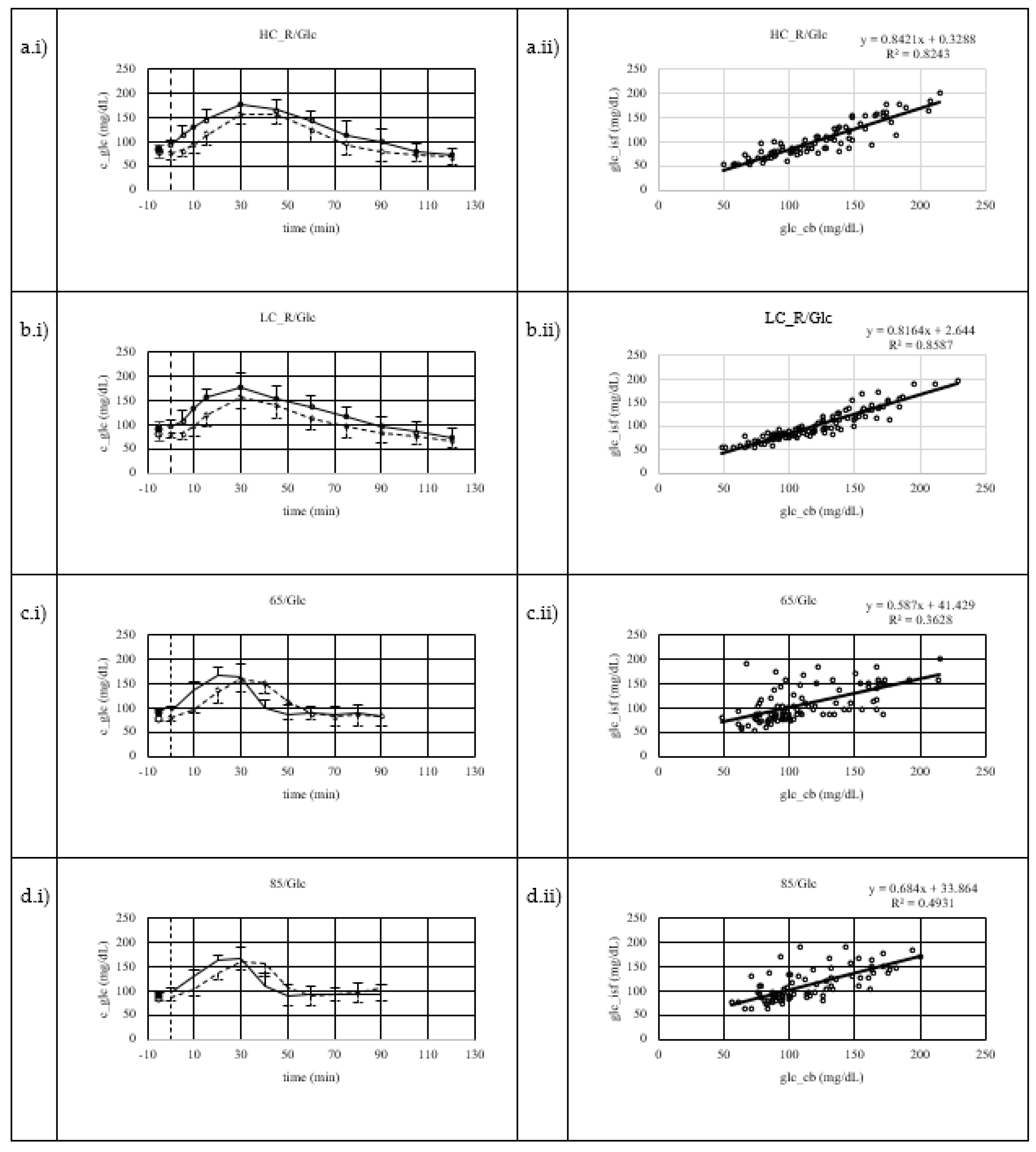
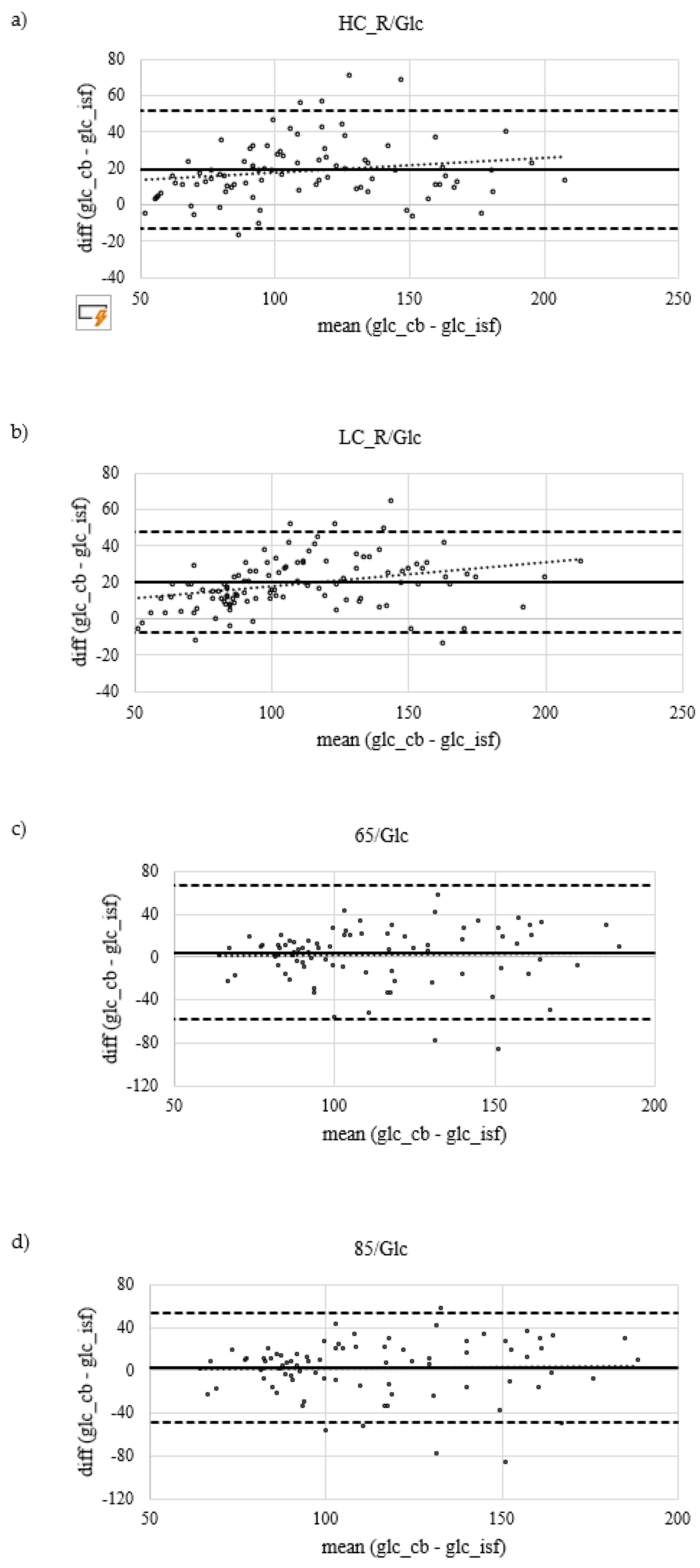
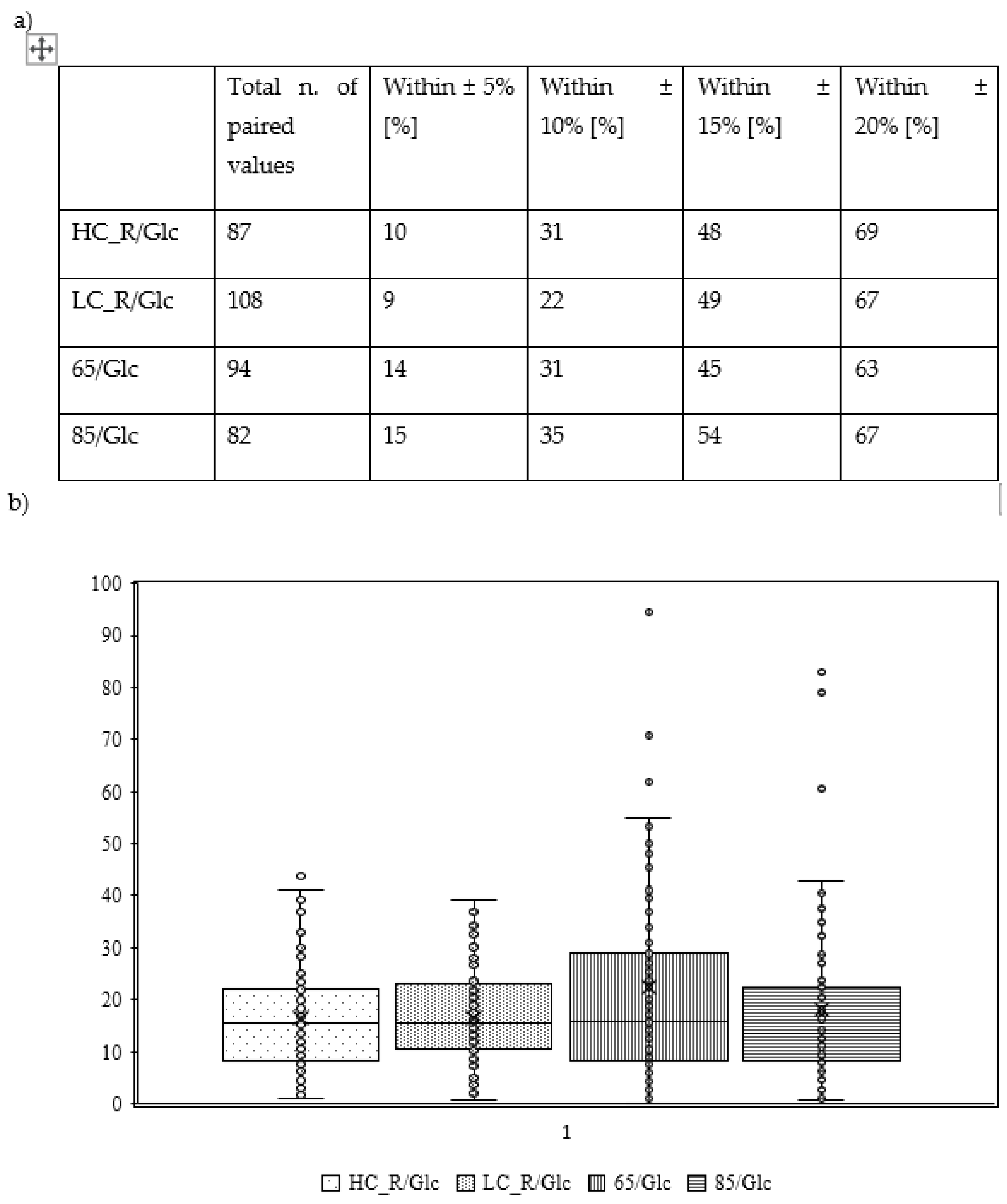
3. Results
3.1. Resting fasted condition
3.2. Resting postprandial condition
3.3. Resting postprandial condition – High carbohydrate dinner before test morning
3.4. Resting postprandial condition – Low carbohydrate dinner before test morning
3.5. Exercise at 65% HRmax
3.6. Exercise at 85% HRmax
4. Discussion
4.1. Impact of physical activity
4.2. Impact of CHO intake before testing
4.3. Conclusion for practical application
5. Limitations
6. Conclusions
Author Contributions
Funding
Data Sharing
Patient Consent for Publication
Ethics Approval
Acknowledgments
Competing Interests
References
- Aberer, F., Hajnsek, M., Rumpler, M., Zenz, S., Baumann, P. M., Elsayed, H., Puffing, A., Treiber, G., Pieber, T. R., Sourij, H., & Mader, J. K. (2017). Evaluation of subcutaneous glucose monitoring systems under routine environmental conditions in patients with type 1 diabetes: ABERER et al. Diabetes, Obesity and Metabolism, 19(7), 1051–1055. [CrossRef]
- Adolfsson, P., Nilsson, S., & Lindblad, B. (2011). Continuous glucose monitoring system during physical exercise in adolescents with type 1 diabetes: Physical exercise and diabetes. Acta Paediatrica, 100(12), 1603–1609. [CrossRef]
- Bally, L., Zueger, T., Pasi, N., Carlos, C., Paganini, D., & Stettler, C. (2016). Accuracy of continuous glucose monitoring during differing exercise conditions. Diabetes Research and Clinical Practice, 112, 1–5. [CrossRef]
- Bao, Y., Chen, L., Chen, L., Dou, J., Gao, Z., Gao, L., Guo, L., Guo, X., Ji, L., Ji, Q., Jia, W., Kuang, H., Li, Q., Li, Q., Li, X., Li, Y., Li, L., Liu, J., Ma, J., … On behalf of Chinese Diabetes Society. (2019). Chinese clinical guidelines for continuous glucose monitoring (2018 edition). Diabetes/Metabolism Research and Reviews, 35(6). [CrossRef]
- Basu, A., Dube, S., Slama, M., Errazuriz, I., Amezcua, J. C., Kudva, Y. C., Peyser, T., Carter, R. E., Cobelli, C., & Basu, R. (2013). Time Lag of Glucose From Intravascular to Interstitial Compartment in Humans. Diabetes, 62(12), 4083–4087. 12. [CrossRef]
- Basu, A., Dube, S., Veettil, S., Slama, M., Kudva, Y. C., Peyser, T., Carter, R. E., Cobelli, C., & Basu, R. (2015). Time Lag of Glucose From Intravascular to Interstitial Compartment in Type 1 Diabetes. Journal of Diabetes Science and Technology, 9(1), 63–68. 1. [CrossRef]
- Bland, J. Bland, J., & Altman, D. (1986). Statistical methods for assessing agreement between two methods of clinical measurement. The Lancet, 8476(327), 307–310. 327. [CrossRef]
- Bowler, A.-L. M., Whitfield, J., Marshall, L., Coffey, V. G., Burke, L. M., & Cox, G. R. (2023). The Use of Continuous Glucose Monitors in Sport: Possible Applications and Considerations. International Journal of Sport Nutrition and Exercise Metabolism, 33(2), 121–132. [CrossRef]
- Brouns, F., Bjorck, I., Frayn, K. N., Gibbs, A. L., Lang, V., Slama, G., & Wolever, T. M. S. (2005). Glycaemic index methodology. Nutrition Research Reviews, 18(1), 145–171. 1. [CrossRef]
- Burke, L. M., Castell, L. M., Casa, D. J., Close, G. L., Costa, R. J. S., Desbrow, B., Halson, S. L., Lis, D. M., Melin, A. K., Peeling, P., Saunders, P. U., Slater, G. J., Sygo, J., Witard, O. C., Bermon, S., & Stellingwerff, T. (2019). International Association of Athletics Federations Consensus Statement 2019: Nutrition for Athletics. International Journal of Sport Nutrition and Exercise Metabolism, 29(2), 73–84. [CrossRef]
- Clavel, P., Tiollier, E., Leduc, C., Fabre, M., Lacome, M., & Buchheit, M. (2022). Concurrent Validity of a Continuous Glucose-Monitoring System at Rest and During and Following a High-Intensity Interval Training Session. International Journal of Sports Physiology and Performance, 17(4), 627–633. [CrossRef]
- Cohen, J. (1988). Statistical power analysis for the behavioral sciences (2. ed., reprint). Psychology Press.
- Ehrhardt, N., & Al Zaghal, E. (2019). Behavior Modification in Prediabetes and Diabetes: Potential Use of Real-Time Continuous Glucose Monitoring. Journal of Diabetes Science and Technology, 13(2), 271–275. [CrossRef]
- Faccioli, S., Del Favero, S., Visentin, R., Bonfanti, R., Iafusco, D., Rabbone, I., Marigliano, M., Schiaffini, R., Bruttomesso, D., Cobelli, C., & on behalf of the PedArPan Study Group. (2017). Accuracy of a CGM Sensor in Pediatric Subjects With Type 1 Diabetes. Comparison of Three Insertion Sites: Arm, Abdomen, and Gluteus. Journal of Diabetes Science and Technology, 11(6), 1147–1154. [CrossRef]
- Færch, K., Amadid, H., Bruhn, L., Clemmensen, K. K. B., Hulman, A., Ried-Larsen, M., Blond, M. B., Jørgensen, M. E., & Vistisen, D. (2021). Discordance Between Glucose Levels Measured in Interstitial Fluid vs in Venous Plasma After Oral Glucose Administration: A Post-Hoc Analysis From the Randomised Controlled PRE-D Trial. Frontiers in Endocrinology, 12, 753810. [CrossRef]
- FDA. (2014). Self-monitoring Blood Glucose Test Systems for Over-the-Counter Use. 1–38.
- Feig, D. S., Donovan, L. E., Corcoy, R., Murphy, K. E., Amiel, S. A., Hunt, K. F., Asztalos, E., Barrett, J. F. R., Sanchez, J. J., de Leiva, A., Hod, M., Jovanovic, L., Keely, E., McManus, R., Hutton, E. K., Meek, C. L., Stewart, Z. A., Wysocki, T., O’Brien, R., … Pragnell, M. (2017). Continuous glucose monitoring in pregnant women with type 1 diabetes (CONCEPTT): A multicentre international randomised controlled trial. The Lancet, 390(10110), 2347–2359. [CrossRef]
- Fox, L., Beck, R., & Xing, D. (2010). Variation of Interstitial Glucose Measurements Assessed by Continuous Glucose Monitors in Healthy, Nondiabetic Individuals. Diabetes Care, 33(6), 1297–1299. 6. [CrossRef]
- Fox, S. (3rd), Haskell, W., & Naughton, J. (1968). Physical activity and the prevention of coronary heart disease. Preventive Medicine, 8(44), 950–967. 44. [CrossRef]
- Freckmann, G., Hagenlocher, S., Baumstark, A., Jendrike, N., Gillen, R. C., Rössner, K., & Haug, C. (2007). Continuous Glucose Profiles in Healthy Subjects under Everyday Life Conditions and after Different Meals. Journal of Diabetes Science and Technology, 1(5), 695–703. 5. [CrossRef]
- Freckmann, G., Pleus, S., Grady, M., Setford, S., & Levy, B. (2019). Measures of Accuracy for Continuous Glucose Monitoring and Blood Glucose Monitoring Devices. Journal of Diabetes Science and Technology, 13(3), 575–583. 13, 3, 575–583. [CrossRef]
- Giani, E., Macedoni, M., Barilli, A., Petitti, A., Mameli, C., Bosetti, A., Cristiano, A., Radovanovic, D., Santus, P., & Zuccotti, G. V. (2018). Performance of the Flash Glucose Monitoring System during exercise in youth with Type 1 diabetes. Diabetes Research and Clinical Practice, 146, 321–329. [CrossRef]
- Gijzen, K., Moolenaar, D. L. J., Weusten, J. J. A. M., Pluim, H. J., & Demir, A. Y. (2012). Is there a suitable point-of-care glucose meter for tight glycemic control? Evaluation of one home-use and four hospital-use meters in an intensive care unit. Clinical Chemistry and Laboratory Medicine (CCLM), 50(11), 1985–1992. [CrossRef]
- Heinemann, L., Schoemaker, M., Schmelzeisen-Redecker, G., Hinzmann, R., Kassab, A., Freckmann, G., Reiterer, F., & Re, L. D. (2020). Benefits and Limitations of MARD as a Performance Parameter for Continuous Glucose Monitoring in the Interstitial Space. Journal of Diabetes Science and Technology, 14(1), 135–150. [CrossRef]
- Hilliard, M. E., Levy, W., Anderson, B. J., Whitehouse, A. L., Commissariat, P. V., Harrington, K. R., Laffel, L. M., Miller, K. M., Van Name, M., Tamborlane, W. V., DeSalvo, D. J., & DiMeglio, L. A. (2019). Benefits and Barriers of Continuous Glucose Monitoring in Young Children with Type 1 Diabetes. Diabetes Technology & Therapeutics, 21(9), 493–498.
- Jeukendrup, A. (2014). A Step Towards Personalized Sports Nutrition: Carbohydrate Intake During Exercise. Sports Medicine, 44(S1), 25–33. [CrossRef]
- Jonvik, K. L., King, M., Rollo, I., Stellingwerff, T., & Pitsiladis, Y. (2022). New Opportunities to Advance the Field of Sports Nutrition. Frontiers in Sports and Active Living, 4, 852230. [CrossRef]
- Kerksick, C. M., Arent, S., Schoenfeld, B. J., Stout, J. R., Campbell, B., Wilborn, C. D., Taylor, L., Kalman, D., Smith-Ryan, A. E., Kreider, R. B., Willoughby, D., Arciero, P. J., VanDusseldorp, T. A., Ormsbee, M. J., Wildman, R., Greenwood, M., Ziegenfuss, T. N., Aragon, A. A., & Antonio, J. (2017). International society of sports nutrition position stand: Nutrient timing. Journal of the International Society of Sports Nutrition, 14(1), 33. [CrossRef]
- Lakens, D. (2013). Calculating and reporting effect sizes to facilitate cumulative science: A practical primer for t-tests and ANOVAs. Frontiers in Psychology, 4. [CrossRef]
- Loon, L. J. C., Greenhaff, P. L., Constantin-Teodosiu, D., Saris, W. H. M., & Wagenmakers, A. J. M. (2001). The effects of increasing exercise intensity on muscle fuel utilisation in humans. The Journal of Physiology, 536(1), 295–304. [CrossRef]
- Madden, J., O’Mahony, C., Thompson, M., O’Riordan, A., & Galvin, P. (2020). Biosensing in dermal interstitial fluid using microneedle based electrochemical devices. Sensing and Bio-Sensing Research, 29, 100348. [CrossRef]
- Mansournia, M. A., Collins, G. S., Nielsen, R. O., Nazemipour, M., Jewell, N. P., Altman, D. G., & Campbell, M. J. (2021). A CHecklist for statistical Assessment of Medical Papers (the CHAMP statement): Explanation and elaboration. British Journal of Sports Medicine, 55(18), 1009–1017. [CrossRef]
- Messer, L. H., Johnson, R., Driscoll, K. A., & Jones, J. (2018). Best friend or spy: A qualitative meta-synthesis on the impact of continuous glucose monitoring on life with Type 1 diabetes. Diabetic Medicine, 35(4), 409–418. [CrossRef]
- Moser, O., Eckstein, M. L., Mueller, A., Birnbaumer, P., Aberer, F., Koehler, G., Sourij, C., Kojzar, H., Holler, P., Simi, H., Pferschy, P., Dietz, P., Bracken, R. M., Hofmann, P., & Sourij, H. (2019). Impact of physical exercise on sensor performance of the FreeStyle Libre intermittently viewed continuous glucose monitoring system in people with Type 1 diabetes: A randomized crossover trial. Diabetic Medicine, 36(5), 606–611. [CrossRef]
- Moser, O., Riddell, M. C., Eckstein, M. L., Adolfsson, P., Rabasa-Lhoret, R., van den Boom, L., Gillard, P., Nørgaard, K., Oliver, N. S., Zaharieva, D. P., Battelino, T., de Beaufort, C., Bergenstal, R. M., Buckingham, B., Cengiz, E., Deeb, A., Heise, T., Heller, S., Kowalski, A. J., … Mader, J. K. (2020). Glucose management for exercise using continuous glucose monitoring (CGM) and intermittently scanned CGM (isCGM) systems in type 1 diabetes: Position statement of the European Association for the Study of Diabetes (EASD) and of the International Society for Pediatric and Adolescent Diabetes (ISPAD) endorsed by JDRF and supported by the American Diabetes Association (ADA). Diabetologia, 63(12), 2501–2520. [CrossRef]
- Moser, O., Yardley, J., & Bracken, R. (2018). Interstitial Glucose and Physical Exercise in Type 1 Diabetes: Integrative Physiology, Technology, and the Gap In-Between. Nutrients, 10(1), 93. [CrossRef]
- Muñoz Fabra, E. Muñoz Fabra, E., Díez, J.-L., Bondia, J., & Laguna Sanz, A. J. (2021). A Comprehensive Review of Continuous Glucose Monitoring Accuracy during Exercise Periods. Sensors, 21(2), 479. 2. [CrossRef]
- Nikolaidis, P. (2015). Maximal heart rate in soccer players: Measured versus age-predicted. Biomedical Journal, 38(1), 84. [CrossRef]
- Nowotny, B., Nowotny, P. J., Strassburger, K., & Roden, M. (2012). Precision and accuracy of blood glucose measurements using three different instruments: Validity of blood glucose measurement instruments. Diabetic Medicine, 29(2), 260–265. [CrossRef]
- Papadopoulou, S. D., Papadopoulou, S. K., Alipasali, F., Hatzimanouil, D., Rosemann, T., Knechtle, B., & Nikolaidis, P. T. (2019). Validity of Prediction Equations of Maximal Heart Rate in Physically Active Female Adolescents and the Role of Maturation. Medicina, 55(11), 735. [CrossRef]
- Rebrin, K., Steil, G. M., van Antwerp, W. P., & Mastrototaro, J. J. (1999). Subcutaneous glucose predicts plasma glucose independent of insulin: Implications for continuous monitoring. American Journal of Physiology-Endocrinology and Metabolism, 277(3), E561–E571. [CrossRef]
- Romijn, J. A., Coyle, E. F., Sidossis, L. S., Rosenblatt, J., & Wolfe, R. R. (2000). Substrate metabolism during different exercise intensities in endurance-trained women. Journal of Applied Physiology, 88(5), 1707–1714. [CrossRef]
- Schierbauer, J. R., Günther, S., Haupt, S., Zimmer, R. T., Zunner, B. E. M., Zimmermann, P., Wachsmuth, N. B., Eckstein, M. L., Aberer, F., Sourij, H., & Moser, O. (2022). Accuracy of Real Time Continuous Glucose Monitoring during Different Liquid Solution Challenges in Healthy Adults: A Randomized Controlled Cross-Over Trial. Sensors, 22(9), 3104. [CrossRef]
- Shah, V. N., DuBose, S. N., Li, Z., Beck, R. W., Peters, A. L., Weinstock, R. S., Kruger, D., Tansey, M., Sparling, D., Woerner, S., Vendrame, F., Bergenstal, R., Tamborlane, W. V., Watson, S. E., & Sherr, J. (2019). Continuous Glucose Monitoring Profiles in Healthy Nondiabetic Participants: A Multicenter Prospective Study. The Journal of Clinical Endocrinology & Metabolism, 104(10), 4356–4364. [CrossRef]
- Siegmund, T. Siegmund, T., Heinemann, L., Kolassa, R., & Thomas, A. (2017). Discrepancies Between Blood Glucose and Interstitial Glucose—Technological Artifacts or Physiology: Implications for Selection of the Appropriate Therapeutic Target. Journal of Diabetes Science and Technology, 11(4), 766–772. [CrossRef]
- Spronk, I., Kullen, C., Burdon, C., & O’Connor, H. (2014). Relationship between nutrition knowledge and dietary intake. British Journal of Nutrition, 111(10), 1713–1726. 10. [CrossRef]
- Steffl, M., Kinkorova, I., Kokstejn, J., & Petr, M. (2019). Macronutrient Intake in Soccer Players—A Meta-Analysis. Nutrients, 11(6), 1305. [CrossRef]
- Steineck, I. I. K., Mahmoudi, Z., Ranjan, A., Schmidt, S., Jørgensen, J. B., & Nørgaard, K. (2019). Comparison of Continuous Glucose Monitoring Accuracy Between Abdominal and Upper Arm Insertion Sites. Diabetes Technology & Therapeutics, 21(5), 295–302. [CrossRef]
- Tanaka, Y., Ogata, H., Park, I., Ando, A., Ishihara, A., Kayaba, M., Yajima, K., Suzuki, C., Araki, A., Osumi, H., Zhang, S., Seol, J., Takahashi, K., Nabekura, Y., Satoh, M., & Tokuyama, K. (2021). Effect of a single bout of morning or afternoon exercise on glucose fluctuation in young healthy men. Physiological Reports, 9(7). [CrossRef]
- Teymourian, H., Tehrani, F., Mahato, K., & Wang, J. (2021). Lab under the Skin: Microneedle Based Wearable Devices. Advanced Healthcare Materials, 10(17), 2002255. [CrossRef]
- Thomas, T., Erdman, K. A., & Burke, L. M. (2016). Nutrition and Athletic Performance. Medicine & Science in Sports & Exercise, 48(3), 543–568. [CrossRef]
- Villena Gonzales, W., Mobashsher, A., & Abbosh, A. (2019). The Progress of Glucose Monitoring—A Review of Invasive to Minimally and Non-Invasive Techniques, Devices and Sensors. Sensors, 19(4), 800. [CrossRef]
- Witt, S., Wohlfahrt, G., & Schomburg, D. (2000). Conserved arginine-516 of Penicillium amagasakiense glucose oxidase is essential for the efficient binding of β-D-glucose. 7.
- Zaharieva, D. P. Zaharieva, D. P., Turksoy, K., McGaugh, S. M., Pooni, R., Vienneau, T., Ly, T., & Riddell, M. C. (2019). Lag Time Remains with Newer Real-Time Continuous Glucose Monitoring Technology During Aerobic Exercise in Adults Living with Type 1 Diabetes. Diabetes Technology & Therapeutics, 21(6), 313–321. [CrossRef]
| HC-Dinner | MC-Dinner | LC-Dinner | |
|---|---|---|---|
| Energy (kcal/kg BW) | 11.44 | 11.14 | 10.78 |
| Carbohydrate (g/kg BW) | 1.97 | 1.25 | 0.51 |
| Protein (g/kg BW) | 0.34 | 0.60 | 0.42 |
| Fat (g/kg BW) | 0.21 | 0.40 | 0.78 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




