Submitted:
22 December 2025
Posted:
24 December 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Patient Population
2.2. Data Collection
- In-hospital mortality;
- Need for respiratory support (non-invasive ventilation or invasive mechanical ventilation);
- Need for inotropic support;
- Total duration of intensive care stay (days).
2.3. Echocardiographic Assessment
- Tricuspid annular plane systolic excursion (TAPSE, mm) using M-mode in the apical 4-chamber view;
- Tissue Doppler–derived systolic velocity at the lateral tricuspid annulus (S RV, cm/s);
- Left ventricular ejection fraction (LVEF, %) using the biplane Simpson method;
- Left ventricular outflow tract velocity–time integral (LVOT VTI, cm) measured by pulsed-wave Doppler in the apical 5-chamber view;
- Early diastolic mitral inflow velocity (E, cm/s) and early diastolic mitral annular velocity (E′ LV, cm/s);
- E/E′ ratio as a surrogate for LV filling pressures [33].
2.4. Statistical Analysis
3. Results
3.1. Baseline Characteristics
3.2. Echocardiographic Parameters and Predictive Analysis for In-Hospital Mortality
3.4. Ventilation and Intensive Care Requirements
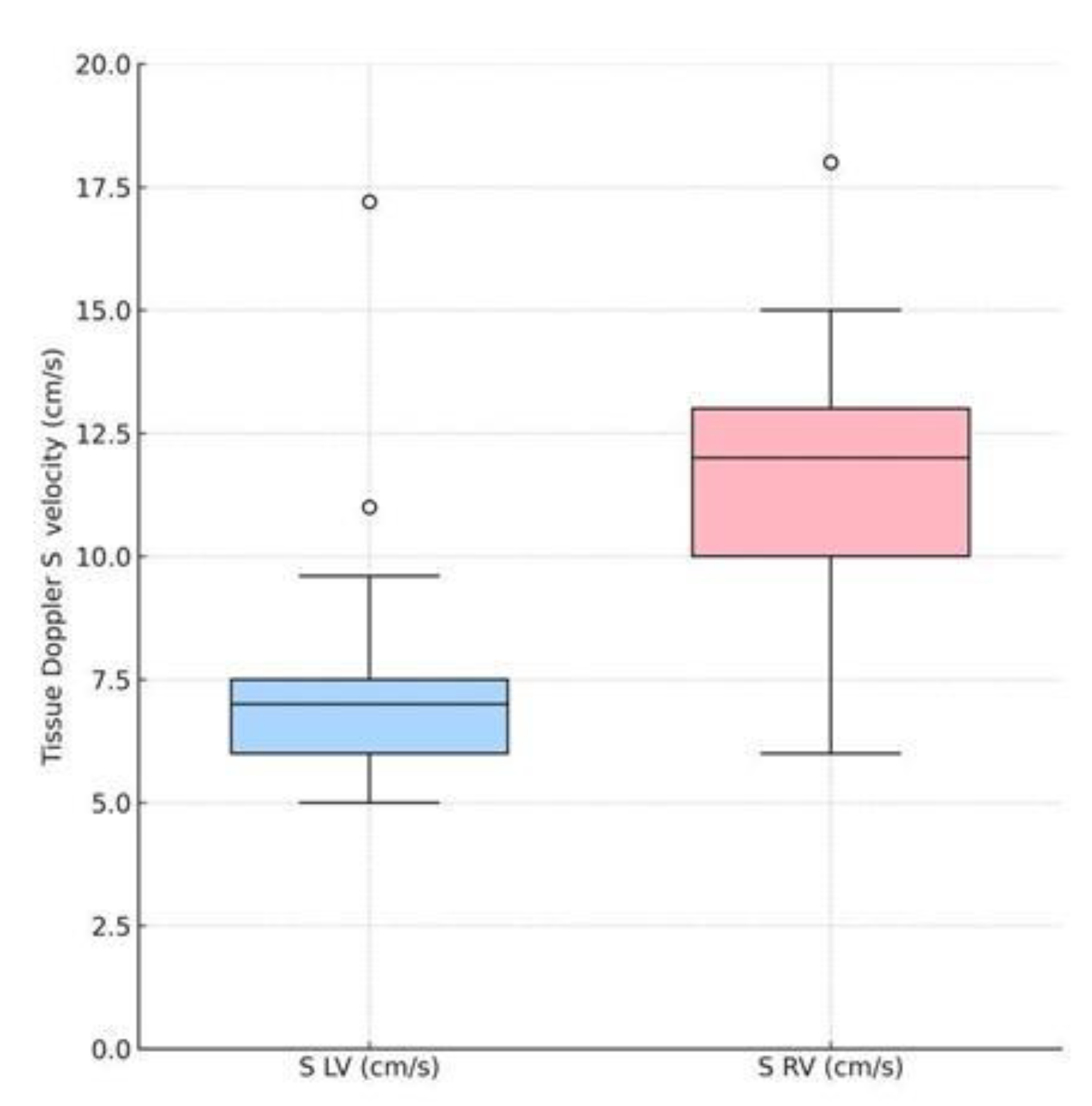
3.5. Comparative Analysis of S LV and S RV
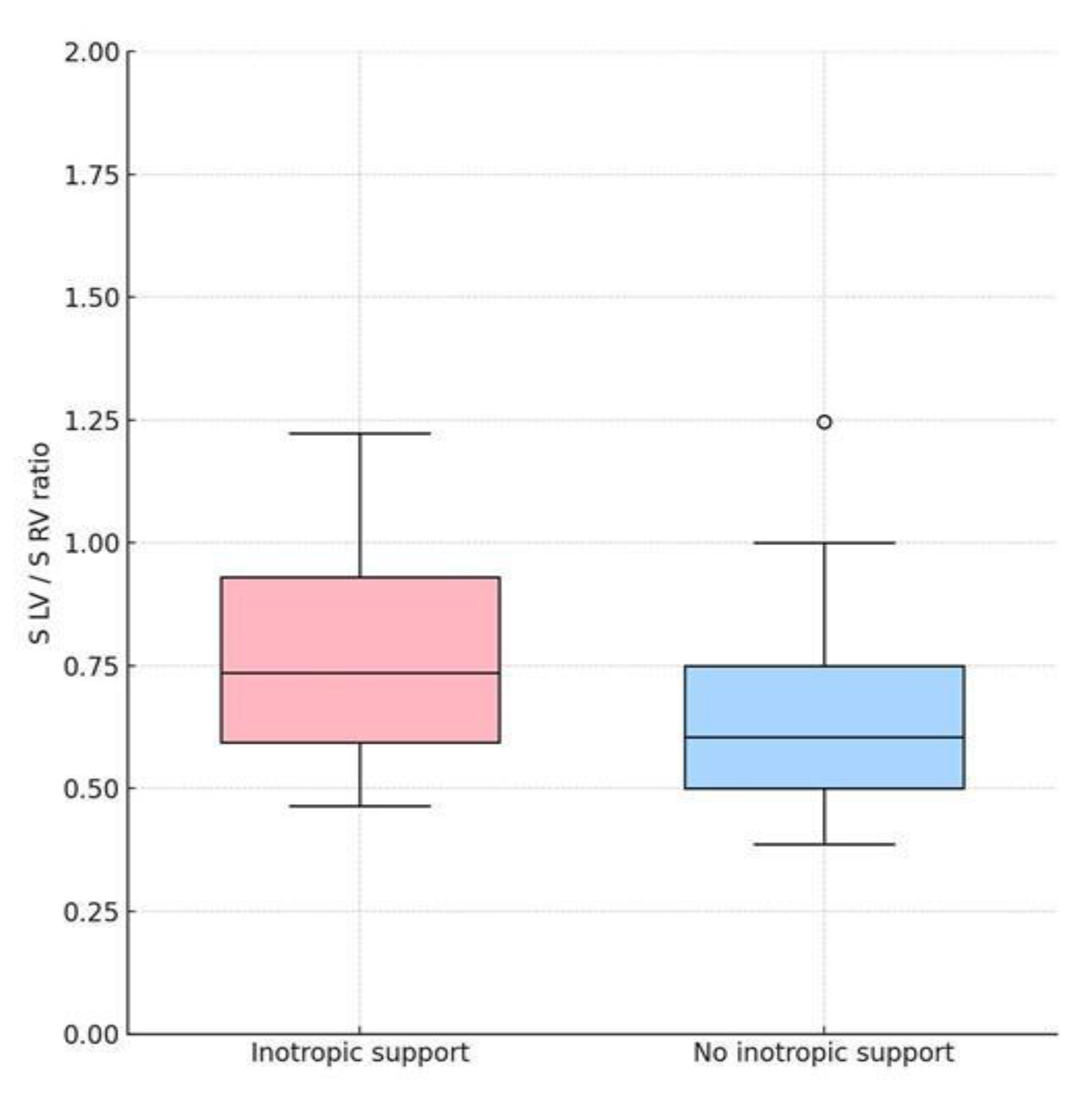
3.6. Association between Echocardiographic Parameters and Inotropic Support
4. Discussion
- Left ventricular longitudinal systolic function (S LV) was significantly lower than right ventricular function (S RV) at presentation, indicating predominant LV systolic impairment in the longitudinal axis despite preserved RV velocities.
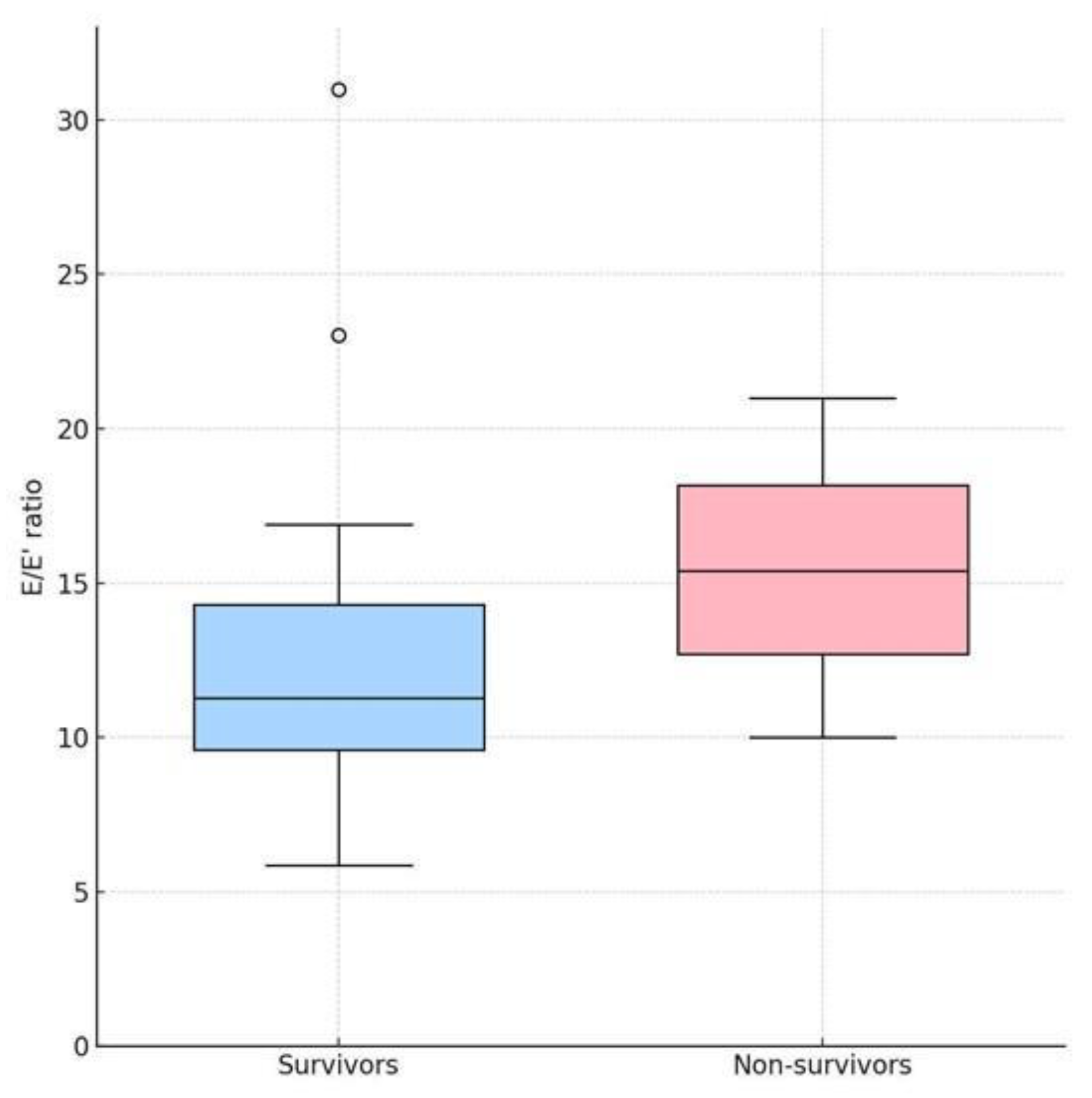
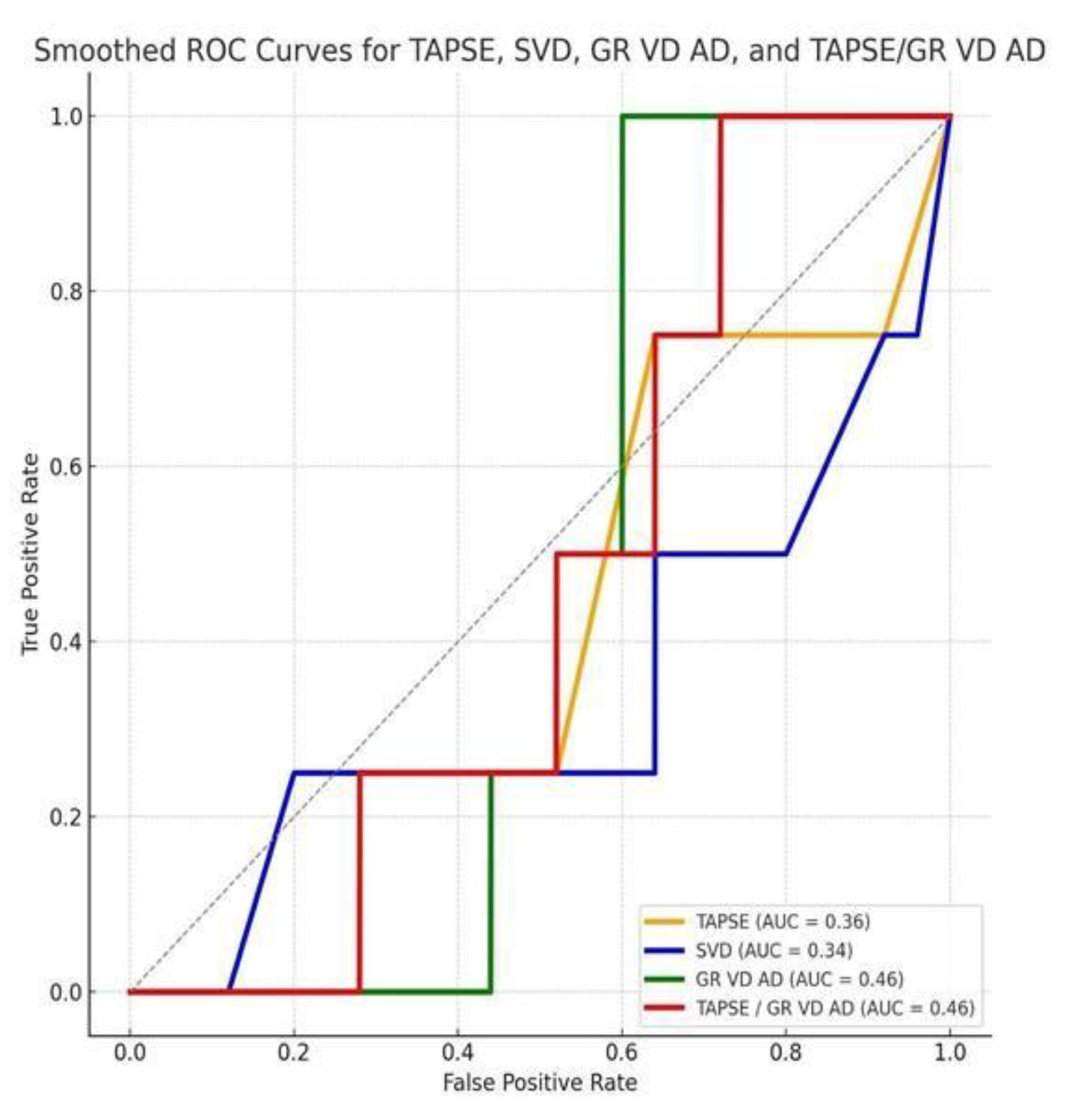
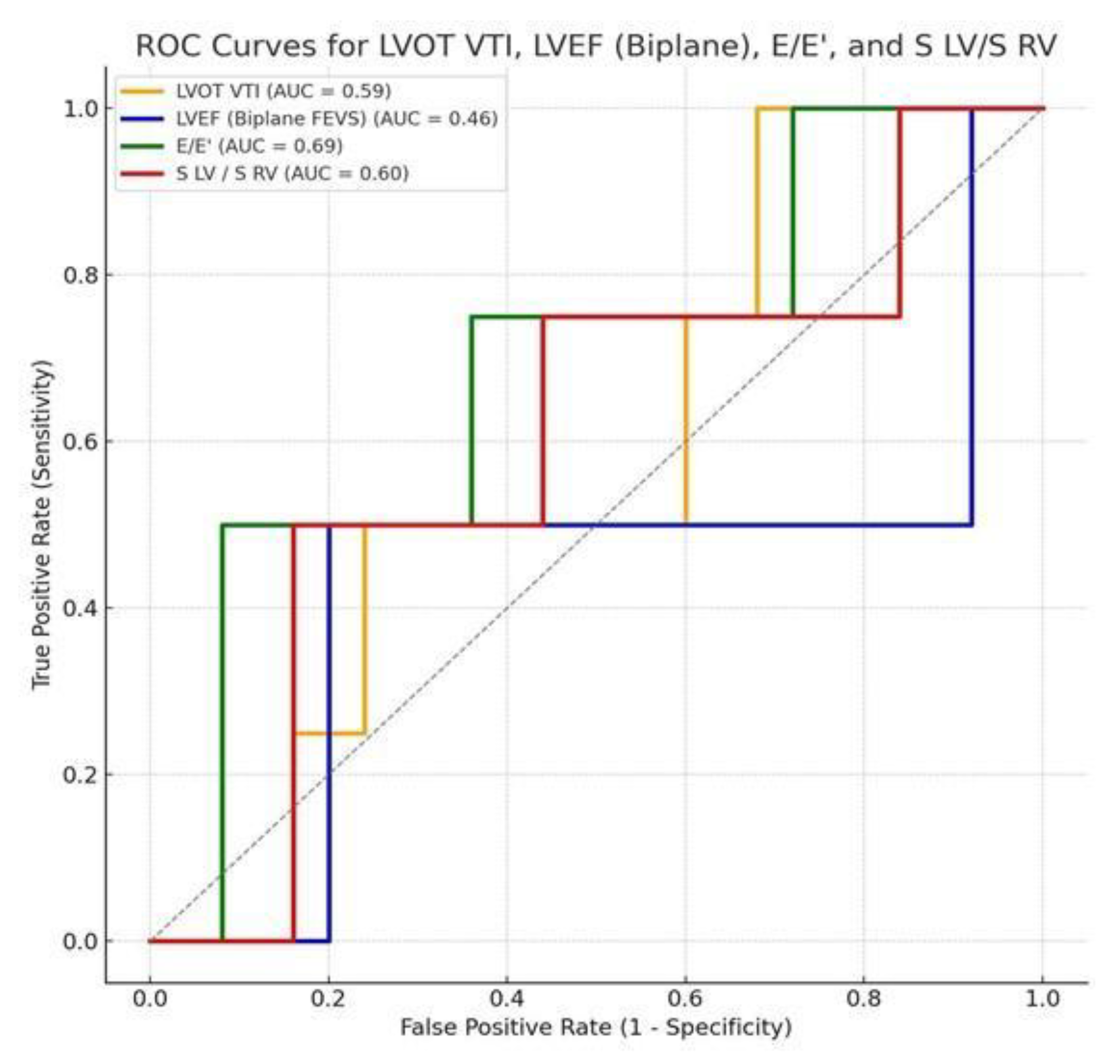
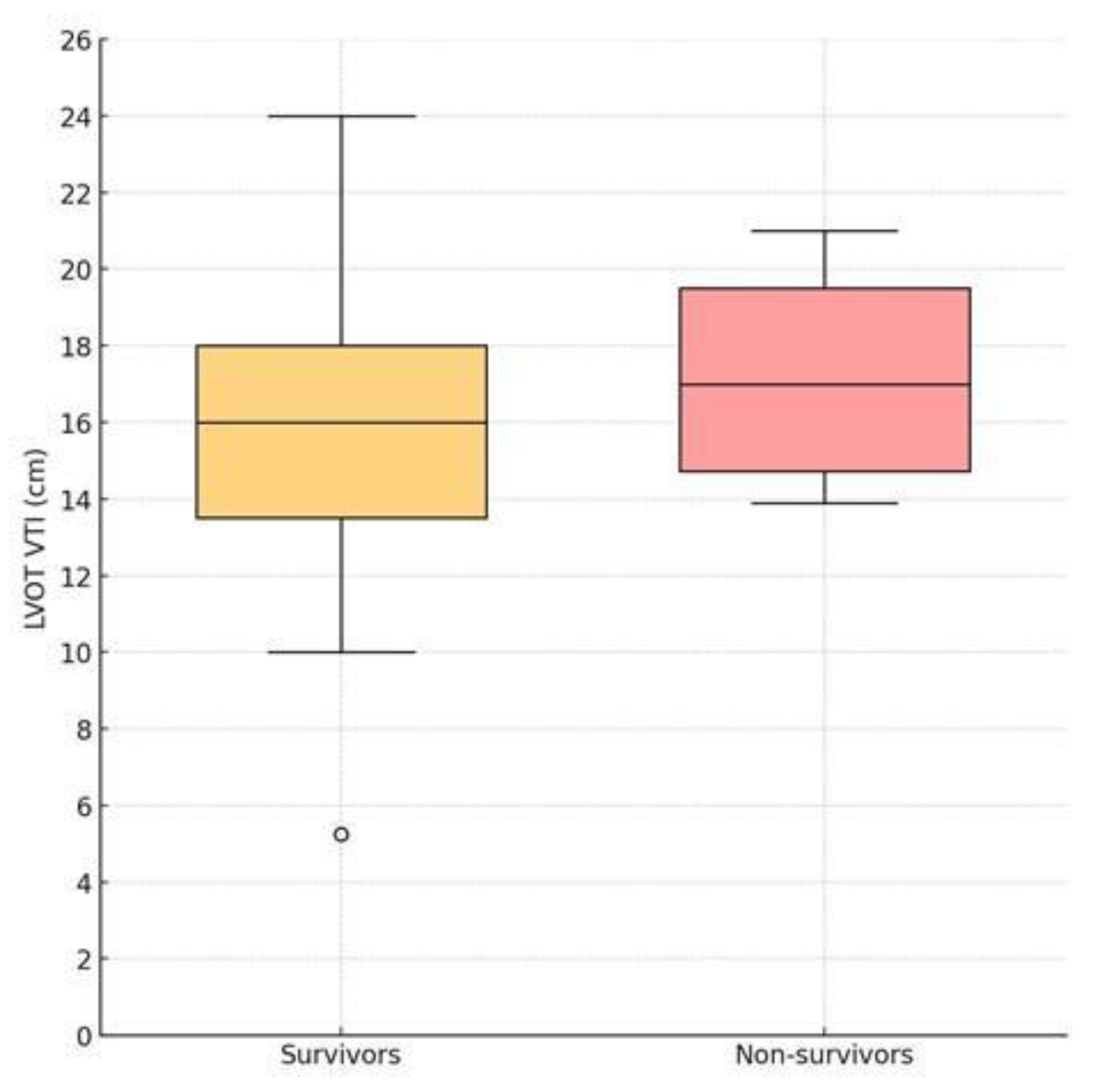
- No echocardiographic parameter demonstrated strong discriminatory power for in-hospital mortality. E/E′ ratio demonstrated the highest discriminatory performance (AUC = 0.69), but without statistical significance.Contrary to our initial hypothesis, LVOT VTI was not lower in non-survivors, but the ROC-derived cut-off of 13.9 cm overlapped with values previously reported as prognostically relevant in acute heart failure cohorts [12,20].
- No echocardiographic parameter was significantly associated with the need for invasive ventilation or inotropic support, but exploratory analysis suggested trends toward lower RV systolic velocities and altered interventricular balance in patients requiring hemodynamic support.
- Regarding intensive care stay, none of the echocardiographic indices correlated significantly with its duration. However, patients with higher mitral E velocity and reduced S LV tended to require longer intensive care hospitalization, suggesting that impaired LV filling and systolic imbalance may contribute to more complex trajectories [33,37].
4.1. Comparison with Previous Studies
4.2. Clinical Implications
4.3. Limitations
4.4. Future Directions
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AUC | area under the curve |
| BP | blood pressure |
| bpm | beats per minute |
| CPE | cardiogenic pulmonary edema |
| CW | continuous wave |
| E-wave (E) | peak early mitral inflow velocity |
| E/E′ | ratio of early mitral inflow velocity to early diastolic mitral annular velocity |
| ICU | intensive care unit |
| IMV | invasive mechanical ventilation |
| IQR | interquartile range |
| IVC | inferior vena cava |
| LV LVEF |
left ventricle left ventricular ejection fraction |
| LVOT | left ventricular outflow tract |
| LVOT VTI | left ventricular outflow tract velocity–time integral |
| NIV | non-invasive ventilation |
| NT-proBNP | N-terminal pro–B-type natriuretic peptide |
| PW | pulsed wave |
| ROC | receiver operating characteristic |
| RV RV-RA gradient |
right ventricle right ventricle–right atrium systolic pressure gradient |
| S LV | systolic velocity of the lateral mitral annulus |
| S RV | systolic velocity of the lateral tricuspid annulus |
| TAPSE | tricuspid annular plane systolic excursion |
References
- Gandhi, SK; Powers, JC; Nomeir, AM; Fowle, K; Kitzman, DW; Rankin, KM; Little, WC. The pathogenesis of acute pulmonary edema associated with hypertension. N Engl J Med. 2001, 344(1), 17–22. [Google Scholar] [CrossRef]
- Gheorghiade, M; De Luca, L; Fonarow, GC; Filippatos, G; Metra, M; Francis, GS. Pathophysiologic targets in the early phase of acute heart failure syndromes. Am J Cardiol. 2005, 96(6A), 11G–17G. [Google Scholar] [CrossRef]
- Chioncel, O; Lainscak, M; Seferovic, PM; Anker, SD; Crespo-Leiro, MG; Harjola, VP; et al. Epidemiology and one-year outcomes in patients with chronic heart failure and preserved, mid-range and reduced ejection fraction: an analysis of the ESC Heart Failure Long-Term Registry. Eur J Heart Fail. 2017, 19(12), 1574–1585. [Google Scholar] [CrossRef]
- Ambrosy, AP; Fonarow, GC; Butler, J; Chioncel, O; Greene, SJ; Vaduganathan, M; et al. The global health and economic burden of hospitalizations for heart failure: lessons learned from hospitalized heart failure registries. J Am Coll Cardiol. 2014, 63(12), 1123–1133. [Google Scholar] [CrossRef]
- Collins, SP; Lindsell, CJ; Jenkins, CA; Harrell, FE; Fermann, GJ; Miller, KF; et al. Risk stratification in acute heart failure: rationale and design of the STRATIFY and DECIDE studies. Am Heart J. 2012, 164(6), 825–834. [Google Scholar] [CrossRef] [PubMed]
- Harjola, VP; Mebazaa, A; Čelutkienė, J; Bettex, D; Bueno, H; Chioncel, O; et al. Contemporary management of acute right ventricular failure: a statement from the Heart Failure Association and the Working Group on Pulmonary Circulation and Right Ventricular Function of the European Society of Cardiology. Eur J Heart Fail. 2016, 18(3), 226–241. [Google Scholar] [CrossRef] [PubMed]
- Lang, RM; Bierig, M; Devereux, RB; Flachskampf, FA; Foster, E; Pellikka, PA. American Society of Echocardiography’s Nomenclature and Standards Committee; Task Force on Chamber Quantification; American College of Cardiology Echocardiography Committee; American Heart Association; European Association of Echocardiography, European Society of Cardiology. Recommendations for chamber quantification. Eur J Echocardiogr. 2006, 7(2), 79–108. [Google Scholar] [CrossRef]
- Nagueh, SF; Smiseth, OA; Appleton, CP; Byrd, BF, 3rd; Dokainish, H; Edvardsen, T; et al. Recommendations for the evaluation of left ventricular diastolic function by echocardiography: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2016, 29(4), 277–314. [Google Scholar] [CrossRef] [PubMed]
- Shah, SJ; Katz, DH; Deo, RC. Phenotypic spectrum of heart failure with preserved ejection fraction. Heart Fail Clin Epub. 2014, 10(3), 407–18. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Ponikowski, P; Voors, AA; Anker, SD; Bueno, H; Cleland, JGF; Coats, AJS; ESC Scientific Document Group. 2016 ESC guidelines for the diagnosis and treatment of acute and chronic heart failure: the task force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur Heart J 2016, 37(27), 2129–2200. [Google Scholar] [CrossRef]
- Tan, C; Rubenson, D; Srivastava, A; Mohan, R; Smith, MR; Billick, K; et al. Left ventricular outflow tract velocity time integral outperforms ejection fraction and Doppler-derived cardiac output for predicting outcomes in a select advanced heart failure cohort. Cardiovasc Ultrasound 2017, 15(1), 18. [Google Scholar] [CrossRef] [PubMed]
- Núñez, J; Mainar, L; Bodí, V; Sanchis, J; Núñez, E; Miñana, G; et al. Valor pronóstico de la fracción de eyección del ventrículo izquierdo en pacientes con insuficiencia cardíaca aguda [Prognostic value of the left ventricular ejection fraction in patients with acute heart failure]. Med Clin (Barc) 2008, 131(5), 161–166. [Google Scholar] [CrossRef]
- Haddad, F; Doyle, R; Murphy, DJ; Hunt, SA. Right ventricular function in cardiovascular disease, part II: pathophysiology, clinical importance, and management of right ventricular failure. Circulation 2008, 117(13), 1717–1731. [Google Scholar] [CrossRef] [PubMed]
- Salzano, A; D’Assante, R; Iacoviello, M; Triggiani, V; Rengo, G; Cacciatore, F; Maiello, C; Limongelli, G; Masarone, D; Sciacqua, A; Filardi, PP; Mancini, A; Volterrani, M; Vriz, O; Castello, R; Passantino, A; Campo, M; Modesti, PA; De Giorgi, A; Arcopinto, M; Gargiulo, P; Perticone, M; Colao, A; Milano, S; Garavaglia, A; Napoli, R; Suzuki, T; Bossone, E; Marra, AM; Cittadini, A. T.O.S.CA. Investigators. Progressive right ventricular dysfunction and exercise impairment in patients with heart failure and diabetes mellitus: insights from the T.O.S.CA. Registry. Cardiovasc Diabetol 2022, 21(1), 108. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Zimbarra Cabrita, I; Ruisanchez, C; Dawson, D; Grapsa, J; North, B; Howard, LS; Pinto, FJ; Nihoyannopoulos, P; Gibbs, JS. Right ventricular function in patients with pulmonary hypertension; the value of myocardial performance index measured by tissue Doppler imaging. Eur J Echocardiogr. 2010, 11(8), 719–24. [Google Scholar] [CrossRef] [PubMed]
- Edward, J; Banchs, J; Parker, H; Cornwell, W. Right ventricular function across the spectrum of health and disease. Heart 2023, 109(5), 349–355. [Google Scholar] [CrossRef] [PubMed]
- Saxena, N; Rajagopalan, N; Edelman, K; López-Candales, A. Tricuspid annular systolic velocity: a useful measurement in determining right ventricular systolic function regardless of pulmonary artery pressures. Echocardiography 2006, 23(9), 750–755. [Google Scholar] [CrossRef]
- Sack, KL; Dabiri, Y; Franz, T; Solomon, SD; Burkhoff, D; Guccione, JM. Investigating the role of interventricular interdependence in development of right heart dysfunction during LVAD support: a patient-specific methods-based approach. Front Physiol. 2018, 9, 520. [Google Scholar] [CrossRef]
- Donker, DW; Sallisalmi, M; Broomé, M. Right-left ventricular interaction in left-sided heart failure with and without venoarterial extracorporeal membrane oxygenation support: a simulation study. ASAIO J 2021, 67(3), 297–305. [Google Scholar] [CrossRef]
- Popescu, DC; Ciobanu, M; Țînț, D; Nechita, AC. Linking Heart Function to Prognosis: The Role of a Novel Echocardiographic Index and NT-proBNP in Acute Heart Failure. Medicina 2025, 61, 1412. [Google Scholar] [CrossRef]
- Ural, D; Çavuşoğlu, Y; Eren, M; Karaüzüm, K; Temizhan, A; Yılmaz, MB; et al. Diagnosis and management of acute heart failure. Anatol J Cardiol. 2015, 15(11), 860–889. [Google Scholar] [CrossRef] [PubMed]
- Cotter, G; Moshkovitz, Y; Kaluski, E; Milo, O; Nobikov, Y; Schneeweiss, A; et al. The role of cardiac power and systemic vascular resistance in the pathophysiology and diagnosis of patients with acute congestive heart failure. Eur J Heart Fail. 2003, 5(4), 443–451. [Google Scholar] [CrossRef]
- World Medical Association. World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA 2013, 310(20), 2191–2194. [Google Scholar] [CrossRef]
- McCullough, PA; Nowak, RM; McCord, J; Hollander, JE; Herrmann, HC; Steg, PG; et al. B-type natriuretic peptide and clinical judgment in emergency diagnosis of heart failure: analysis from Breathing Not Properly (BNP) Multinational Study. Circulation 2002, 106(4), 416–422. [Google Scholar] [CrossRef]
- Maisel, AS; Krishnaswamy, P; Nowak, RM; McCord, J; Hollander, JE; Duc, P. Breathing Not Properly Multinational Study Investigators. Rapid measurement of B-type natriuretic peptide in the emergency diagnosis of heart failure. N Engl J Med. 2002, 347(3), 161–167. [Google Scholar] [CrossRef] [PubMed]
- Januzzi, JL, Jr.; Camargo, CA; Anwaruddin, S; Baggish, AL; Chen, AA; Krauser, DG; et al. The N-terminal pro-BNP investigation of dyspnea in the emergency department (PRIDE) study. Am J Cardiol. 2005, 95(8), 948–954. [Google Scholar] [CrossRef] [PubMed]
- Lang, RM; Badano, LP; Mor-Avi, V; Afilalo, J; Armstrong, A; Ernande, L; et al. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging 2015, 16(3), 233–271. [Google Scholar] [CrossRef]
- Mitchell, C; Rahko, PS; Blauwet, LA; Canaday, B; Finstuen, JA; Foster, MC; et al. Guidelines for performing a comprehensive transthoracic echocardiographic examination in adults: recommendations from the American Society of Echocardiography. J Am Soc Echocardiogr. 2019, 32(1), 1–64. [Google Scholar] [CrossRef]
- Rudski, LG; Lai, WW; Afilalo, J; Hua, L; Handschumacher, MD; Chandrasekaran, K; et al. Guidelines for the echocardiographic assessment of the right heart in adults: a report from the American Society of Echocardiography endorsed by the European Association of Echocardiography, a registered branch of the European Society of Cardiology, and the Canadian Society of Echocardiography. J Am Soc Echocardiogr. 2010, 23(7), 685–713. [Google Scholar] [CrossRef]
- Wu, VC; Takeuchi, M. Echocardiographic assessment of right ventricular systolic function. Cardiovasc Diagn Ther. 2018, 8(1), 70–79. [Google Scholar] [CrossRef]
- Nikitin, NP; Loh, PH; Silva, Rd; Ghosh, J; Khaleva, OY; Goode, K; et al. Prognostic value of systolic mitral annular velocity measured with Doppler tissue imaging in patients with chronic heart failure caused by left ventricular systolic dysfunction. Heart 2006, 92(6), 775–779. [Google Scholar] [CrossRef] [PubMed]
- Wang, M; Yip, GW; Wang, AY; Zhang, Y; Ho, PY; Tse, MK; et al. Tissue Doppler imaging provides incremental prognostic value in patients with systemic hypertension and left ventricular hypertrophy. J Hypertens. 2005, 23(1), 183–191. [Google Scholar] [CrossRef] [PubMed]
- Nagueh, SF; Middleton, KJ; Kopelen, HA; Zoghbi, WA; Quiñones, MA. Doppler tissue imaging: a noninvasive technique for evaluation of left ventricular relaxation and estimation of filling pressures. J Am Coll Cardiol. 1997, 30(6), 1527–1533. [Google Scholar] [CrossRef] [PubMed]
- Kim, TK. T test as a parametric statistic. Korean J Anesthesiol. 2015, 68(6), 540–546. [Google Scholar] [CrossRef]
- McDonald, JH. Handbook of Biological Statistics, 3rd ed.; Sparky House Publishing: Baltimore, 2014. [Google Scholar]
- Youden, WJ. Index for rating diagnostic tests. Cancer 1950, 3(1), 32–35. [Google Scholar] [CrossRef]
- Núñez, J; de la Espriella, R; Rossignol, P; Voors, AA; Mullens, W; Metra, M; et al. Congestion in heart failure: a circulating biomarker-based perspective. A review from the Biomarkers Working Group of the Heart Failure Association, European Society of Cardiology. Eur J Heart Fail 2022, 24(10), 1751–1766. [Google Scholar] [CrossRef]
- Okura, H; Kubo, T; Asawa, K; Toda, I; Yoshiyama, M; Yoshikawa, J; Yoshida, K. Elevated E/E′ predicts prognosis in congestive heart failure patients with preserved systolic function. Circ J 2009, 73(1), 86–91. [Google Scholar] [CrossRef]
| Variable | Total (N=28) | Survivors (N=24) | Non-survivors (N=4) | p-Value |
|---|---|---|---|---|
| Age (years) | 73.82 ± 12.14 | 74.12 ± 11.68 | 72.00 ± 16.57 | 0.819 |
| Male sex, % | 61.9 | 64.7 | 50.0 | 0.618 |
| Smoking, % | 21.4 | 20.8 | 25.0 | 1.000 |
| Hypertension, % | 100.0 | 100.0 | 100.0 | 1.000 |
| Dyslipidemia, % | 96.4 | 100.0 | 75.0 | 0.143 |
| Obesity, % | 29.6 | 30.4 | 25.0 | 1.000 |
| Diabetes mellitus, % | 53.6 | 50.0 | 75.0 | 0.600 |
| Valvular heart disease, % | 71.4 | 75.0 | 50.0 | 0.555 |
| Systolic BP (mmHg) | 173.39 ± 38.52 | 172.58 ± 39.94 | 178.25 ± 33.05 | 0.772 |
| Diastolic BP (mmHg) | 99.39 ± 21.23 | 99.75 ± 22.59 | 97.25 ± 11.70 | 0.746 |
| Heart rate (bpm) | 105.61 ± 23.04 | 105.75 ± 24.69 | 104.75 ± 10.24 | 0.892 |
| NT-proBNP (pg/mL) | 10513.96 ± 10381.23 | 9955.83 ± 10293.27 | 13862.75 ± 11840.24 | 0.569 |
| TAPSE (mm) | 22.61 ± 8.20 | 23.29 ± 8.61 | 18.50 ± 3.32 | 0.072 |
| LVOT VTI (cm) | 16.20 ± 4.52 | 16.03 ± 4.72 | 17.23 ± 3.34 | 0.561 |
| RV-RA gradient (mmHg) | 28.93 ± 9.74 | 29.00 ± 10.51 | 28.50 ± 2.65 | 0.845 |
| LVEF (%) | 38.68 ± 15.42 | 38.83 ± 15.07 | 37.75 ± 19.92 | 0.923 |
| Parameter | Survivors Median (IQR) | Non-Survivors Median (IQR) | p-value |
|---|---|---|---|
| E/E` | 11.37 (10.15-14.33) | 15.41 (12.70-18.17) | 0.291 |
| TAPSE | 20.00 (17.75-26.25) | 19.00 (17.75-19.75) | 0.323 |
| S RV | 12.00 (10.00-13.20) | 10.00 (8.25-11.75) | 0.339 |
| S LV | 6.90 (5.97-7.62) | 6.75 (6.12-7.12) | 0.669 |
| S LV /S RV | 0.60 (0.50-0.71) | 0.73 (0.59-0.83) | 0.533 |
| LVEF | 37.50 (26.75-47.25) | 38.00 (20.75-55.00) | 0.844 |
| LVOT VTI | 16.00 (13.38-18.25) | 17.00 (14.72-19.50) | 0.645 |
| Parameter | No ventilation | NIV | IMV | p-value |
|---|---|---|---|---|
| TAPSE | 19.00 [15.75–28.00] | 20.00 [17.50–24.00] | 20.50 [17.75–23.25] | 0.916 |
| S RV | 12.35 [10.50–13.60] | 11.70 [9.00–12.20] | 11.45 [9.75–12.43] | 0.483 |
| S LV | 6.70 [5.83–8.20] | 7.00 [6.00–7.75] | 6.75 [6.12–7.05] | 0.683 |
| S LV / S RV | 0.62 [0.48–0.73] | 0.62 [0.52–0.80] | 0.62 [0.57–0.69] | 0.865 |
| RV-RA gradient | 31.0 [17.75–40.25] | 29.0 [21.50–34.50] | 29.5 [26.75–35.50] | 0.816 |
| E/E’ | 12.29 [10.89–15.48] | 11.44 [9.97–13.92] | 13.61 [9.85–18.17] | 0.680 |
| LVOT VTI | 16.40 [13.55–21.75] | 15.00 [13.50–18.50] | 15.75 [14.72–17.62] | 0.800 |
| LVEF | 38.0 [27.25–54.00] | 38.0 [30.50–45.00] | 28.0 [20.75–40.00] | 0.580 |
| Parameter | Spearman ρ | p-value |
|---|---|---|
| TAPSE | -0.148 | 0.444 |
| S RV | -0.078 | 0.686 |
| S LV | -0.189 | 0.326 |
| S LV / S RV | -0.001 | 0.995 |
| RV-RA gradient | -0.055 | 0.777 |
| E-wave | 0.175 | 0.363 |
| E/E’ | 0.198 | 0.302 |
| LVOT VTI | 0.031 | 0.874 |
| LVEF | -0.175 | 0.365 |
| Parameter | No Inotrope Median (IQR) | Inotrope Median (IQR) | p-value |
|---|---|---|---|
| E/E′ | 12.02 (10.62–14.33) | 13.61 (9.38–18.17) | 0,874 |
| TAPSE (mm) | 19.50 (17.75–26.25) | 19.50 (17.75–20.50) | 0,448 |
| S RV (cm/s) | 12.00 (10.00–13.20) | 10.00 (8.25–11.75) | 0,339 |
| S LV (cm/s) | 6.90 (5.97–7.50) | 6.75 (6.12–8.00) | 0,973 |
| S LV / S RV | 0.60 (0.50–0.71) | 0.73 (0.59–0.93) | 0,393 |
| LVEF (%) | 38.50 (26.75–52.00) | 29.50 (20.75–42.25) | 0,449 |
| LVOT VTI (cm) | 16.20 (13.38–19.00) | 14.50 (13.97–16.50) | 0,792 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




