Discussion
Summary of Key Findings
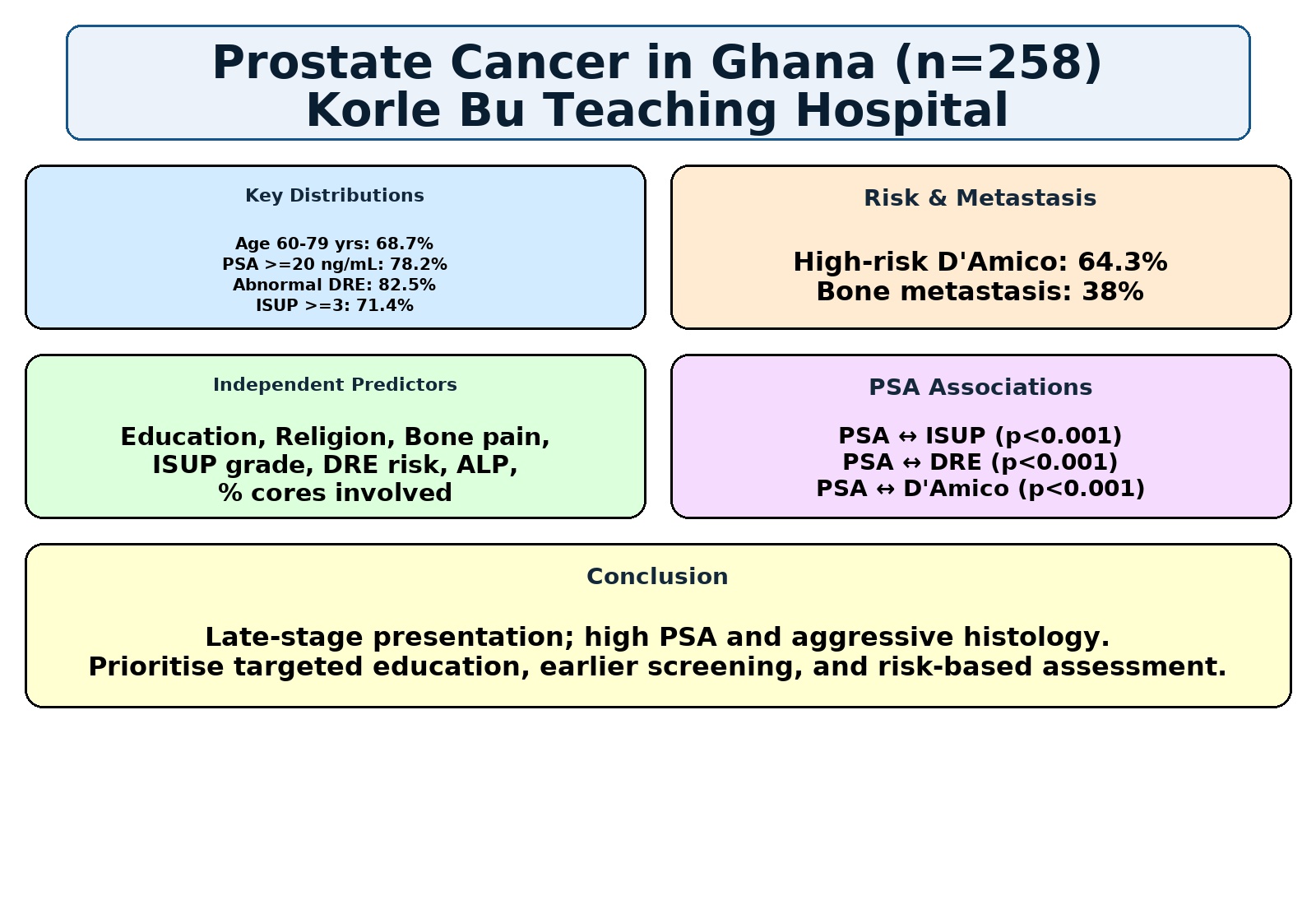
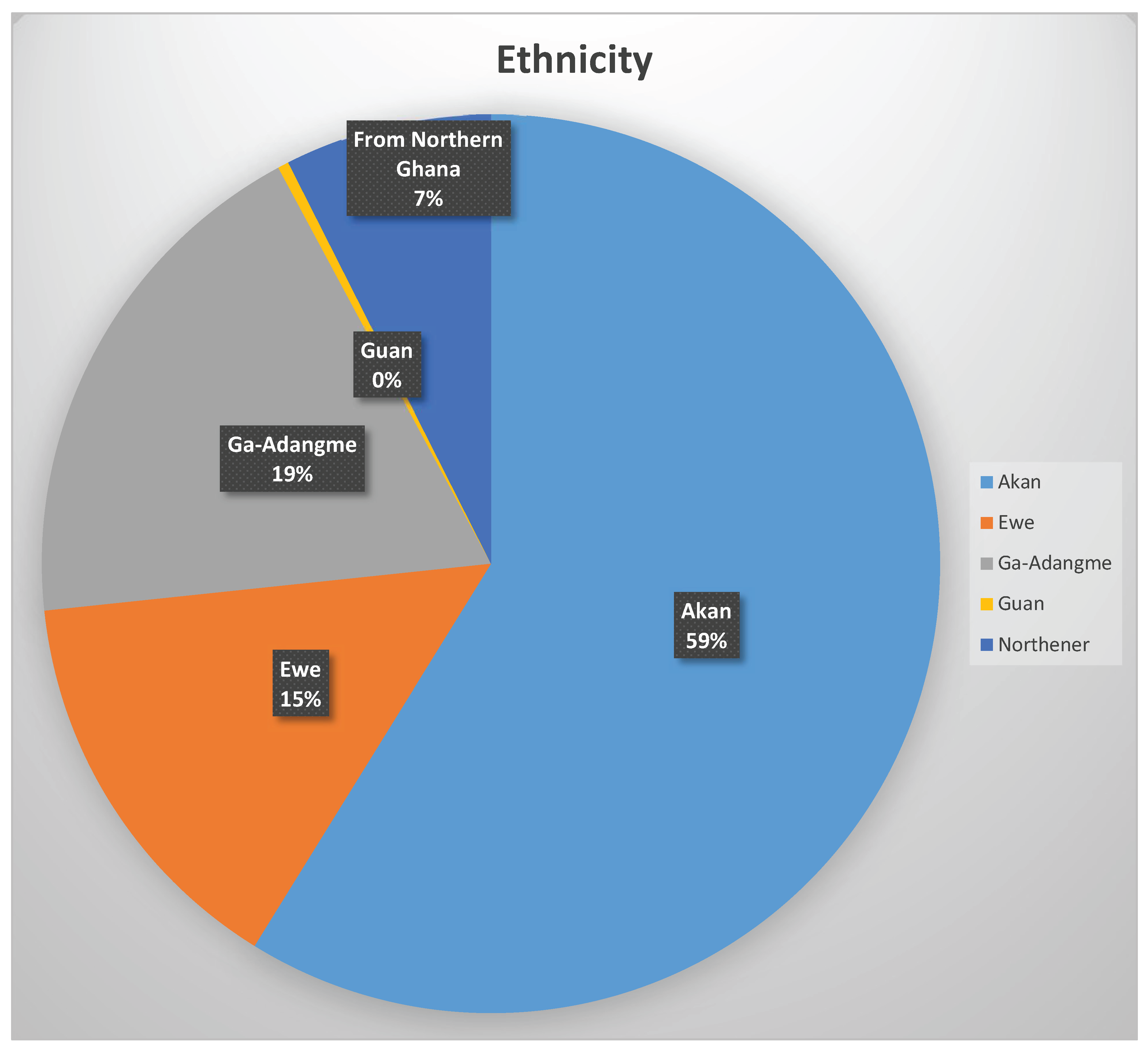
The study population was predominantly aged 60–79 years (68.7%), with 71.7% having PSA ≥20 ng/mL, 45.3% high risk DRE findings, 32.6.% high risk ISUP grade (≥4), 80.6% in the high-risk D’Amico category. Bone metastases were confirmed in 38% of cases. Educational level, religion, bone pain, and pathological factors—including ISUP grade (χ2 = 66.50, p < 0.001), DRE risk (χ2 = 34.85, p < 0.001), ALP (χ2 = 168.33, p < 0.001), percentage of cores involved (χ2 = 40.12, p = 0.029), and perineural invasion (χ2 = 7.505, p = 0.029)—were significantly associated with adverse clinicopathological parameters. Conversely, ethnicity (p = 0.940), occupation (p > 0.28), family history of prostate cancer (p = 0.572), smoking (p = 0.138), and prostate volume (p = 0.940) showed no significant associations.
PSA level was strongly associated with ISUP grade, DRE risk category, and D’Amico classification, with higher PSA corresponding to more advanced disease features. Multivariable logistic regression identified education, religion, bone pain, ISUP grade, DRE risk, ALP, and percentage of cores involved as independent predictors of severe disease, mirroring patterns in PSA, DRE, ISUP, and metastasis distribution, and reinforcing the importance of these factors in risk stratification.
Comparison with Existing Literature
The age distribution in this cohort showed a near-normal curve, with a mean age of 68.18 years (median 69 years, modal age 65 years, range 47–85 years). The closeness of the mean and median suggests a symmetric distribution, supporting the application of parametric statistical methods within the accepted levels of significance. These figures closely agree with those reported by Mensah et al. in 2016 for Ghanaian men undergoing prostate brachytherapy [
5], and are consistent with other local and international studies showing that the peak incidence of PCa occurs in the seventh decade of life [
6,
7,
21]. Globally, this age pattern is linked to cumulative DNA damage, epigenetic changes, and androgen-driven cellular proliferation in the prostate gland over time [
4].
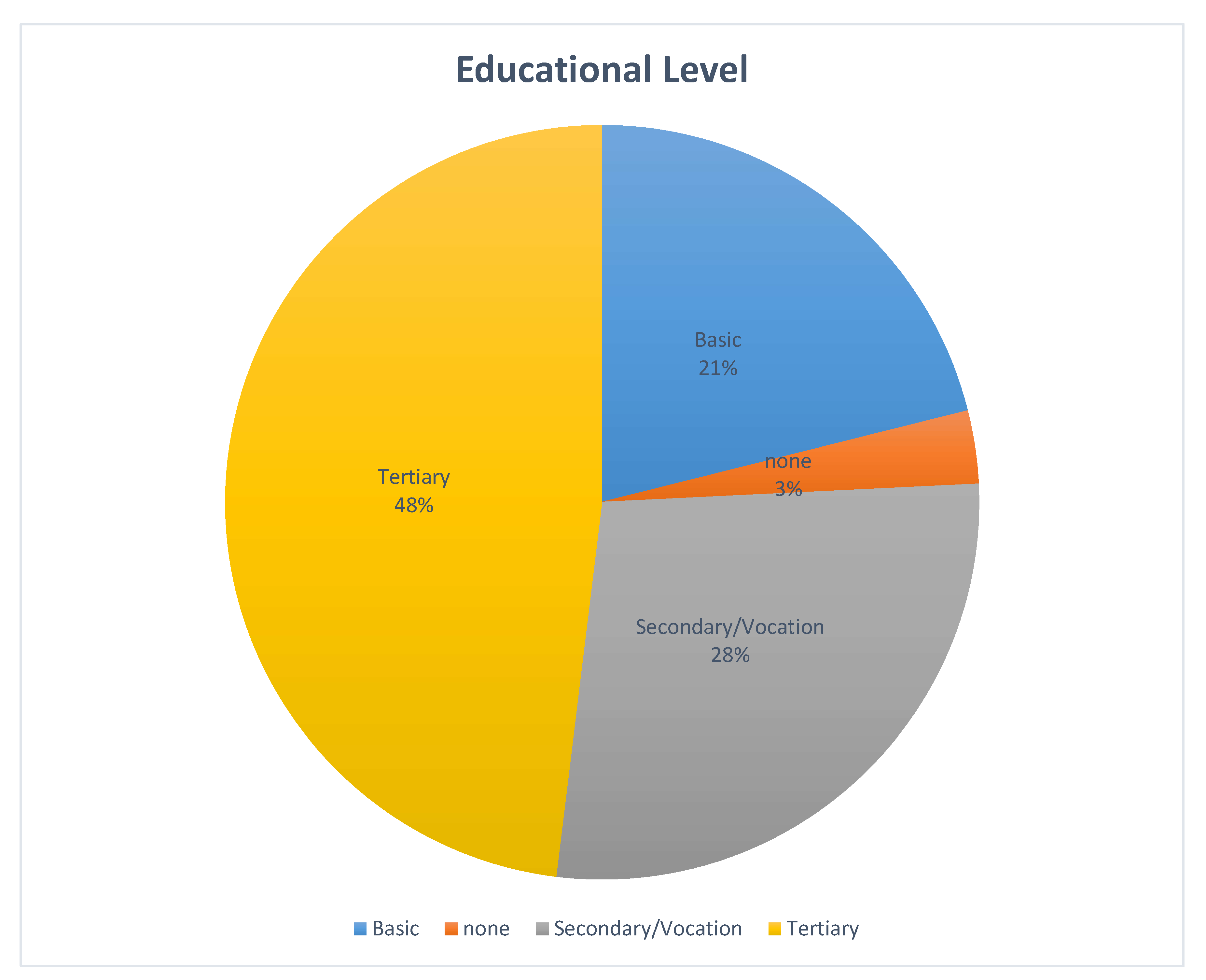
The high proportion of participants with tertiary education (48%) is notable and contrasts with earlier Ghanaian cancer cohorts reporting lower literacy rates [
15]. However, the majority still presented with advanced disease, indicating that higher education does not fully offset other barriers such as limited access to PSA screening, cultural beliefs, socioeconomic constraints, and delayed health-seeking behaviour. Similar findings in the United States suggest that while higher education may slightly increase PCa incidence—likely due to more frequent screening—it is also associated with lower mortality because of earlier detection and treatment [
15].
Bone metastases in 38% of patients confirm the high metastatic burden seen in sub-Saharan Africa, where late presentation remains common [
3,
8]. In contrast, PSA screening in high-income countries has shifted diagnosis towards localized disease. The skeletal distribution of metastases, predominantly to the axial skeleton, aligns with the “seed and soil” hypothesis in which PCa cells preferentially colonize marrow-rich bone sites [
5].
Our findings also point to sociodemographic modifiers of disease presentation. Education was inversely related to metastasis frequency (75% with no education vs. 30.9% with tertiary education), supporting the idea that health literacy facilitates earlier diagnosis. Similarly, religion showed significant associations with PSA category, Gleason score, ISUP grade, and PSA-age index—Muslim patients had over threefold higher odds of presenting with very high PSA (>124.48 ng/mL) and high-grade tumours compared to Christians. This may reflect differences in healthcare access, awareness, or cultural attitudes to screening.
Several pathological variables were strong predictors of bone metastases, including high PSA, elevated ALP, perineural invasion, higher ISUP grade, and advanced DRE category—all in keeping with established metastatic risk factors [
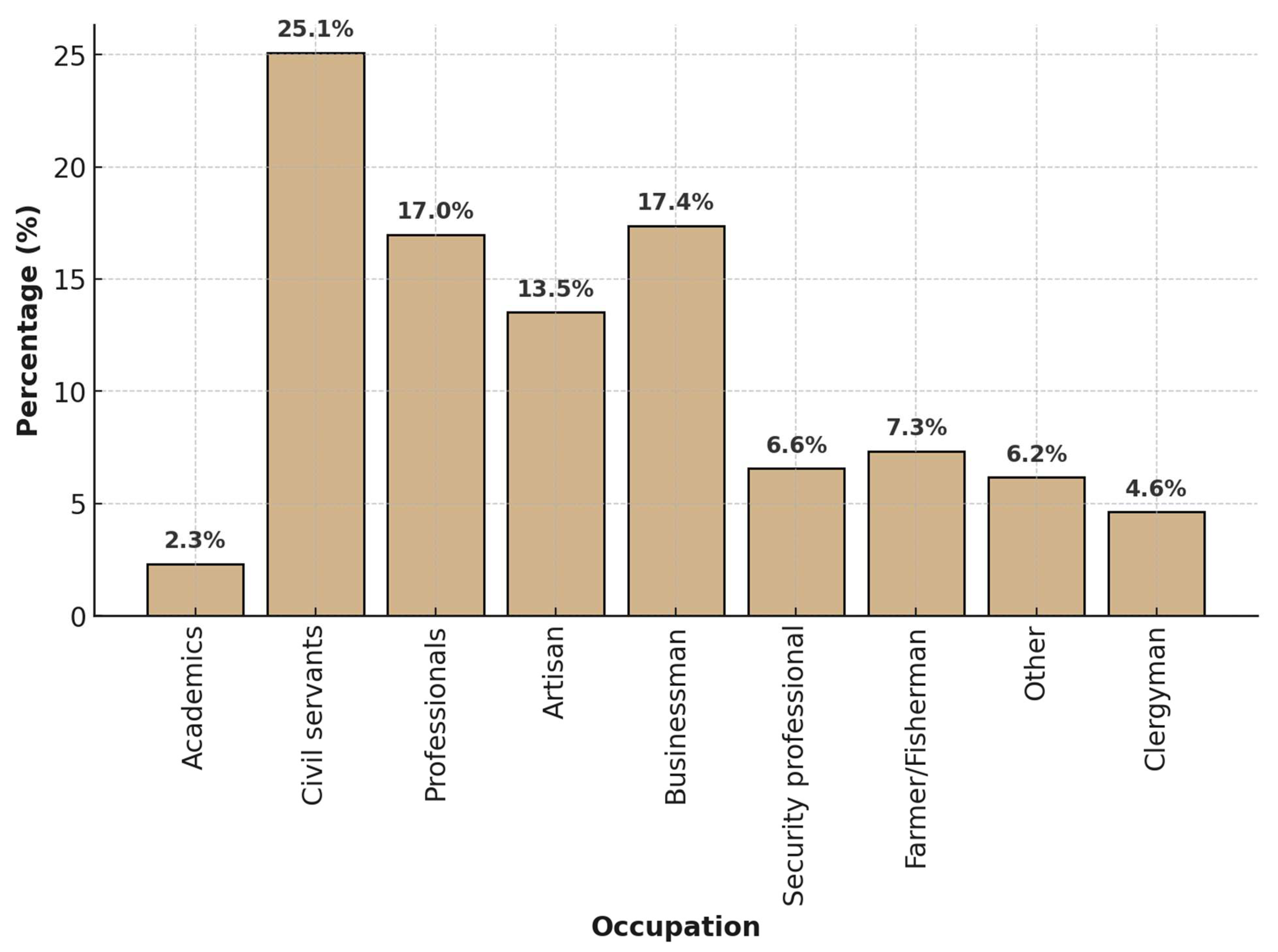
8,
10]. Conversely, ethnicity, occupation, smoking status, and family history showed no statistically significant association with metastasis, though small subgroup sizes may limit interpretation.
PSA demonstrated robust associations with ISUP grade, DRE risk, and D’Amico classification, with increasing PSA levels corresponding to a higher proportion of aggressive histology and advanced clinical staging. Logistic regression further identified ISUP grades 4–5 and high-risk DRE findings as strongly predictive of PSA >100 ng/mL, highlighting their diagnostic and prognostic value.
Overall, this study reinforces the aggressive clinicopathological profile of prostate cancer in Ghanaian men, with frequent high-grade, high-stage presentations and a substantial metastatic burden. Public health strategies must therefore prioritize earlier detection through targeted screening and education, while also addressing systemic barriers to timely diagnosis and treatment.
What Is Already Known About This Topic
Prostate cancer is the most common malignancy among men in Ghana and sub-Saharan Africa, frequently presenting at advanced stages.
High PSA levels, abnormal digital rectal examination (DRE) findings, and high Gleason/ISUP grades are established markers of aggressive disease.
Late presentation is often attributed to limited screening, poor awareness, socioeconomic barriers, and cultural beliefs.
While some studies in Ghana have described demographic and clinical profiles, few have comprehensively examined associations between sociodemographic factors, lifestyle variables, and multiple clinicopathological indicators within the same cohort.
What This Study Adds
Provides simultaneous analysis of sociodemographic, lifestyle, and pathological variables with PSA, DRE risk category, ISUP grade, D’Amico classification, and bone metastases in a large Ghanaian cohort.
Demonstrates that lower educational attainment, certain religious affiliations, bone pain, high ALP, greater tumour core involvement, and high risk ISUP/DRE categories are independent predictors of severe disease.
Shows strong associations between PSA levels and both histological grade (ISUP) and clinical staging systems (DRE and D’Amico).
Highlights that ethnicity, occupation, smoking, and family history were not significantly associated with advanced disease in this population.
Offers evidence to support targeted community education, earlier screening, and risk-based assessment protocols in resource-limited settings.
Limitations of the Study
Firstly, the cross-sectional retrospective design relies on existing medical records, which may have incomplete or missing data for certain variables such as family history, comorbidities, and exact timing of symptom onset, potentially introducing information bias.
Secondly, this study was conducted at a single tertiary referral center in an urban setting, which might limit the generalizability of findings to prostate cancer patients from rural or underserved regions of Ghana with different socio-demographic characteristics and healthcare access.
Thirdly, the sample size, while sufficient for descriptive analysis, restricts the power of inferential statistics to detect smaller associations or perform multivariate analyses controlling for confounding variables.
Additionally, the study did not incorporate molecular or genetic analyses that could elucidate underlying biological differences in tumour behaviour among the studied population.
Finally, changes in referral patterns or diagnostic technologies during the study period were not accounted for, which may affect representativeness.
Future prospective multicenter studies with larger cohorts and inclusion of molecular profiling are recommended to address these limitations and provide a more comprehensive understanding of prostate cancer patterns in Ghana.
Conclusion
This study demonstrates that prostate cancer in Ghanaian men commonly presents at an advanced stage, with high PSA levels, aggressive histopathological features, and a substantial burden of bone metastases. Sociodemographic factors—particularly lower educational attainment and certain religious affiliations—along with clinical indicators such as bone pain, high ISUP grade, advanced DRE category, elevated ALP, and greater tumour core involvement, were strongly associated with disease severity. Multivariable analysis confirmed these as independent predictors of advanced presentation, underscoring their potential value in risk stratification where access to full diagnostic resources is limited. These findings highlight the urgent need for targeted community education, earlier screening, and streamlined referral pathways to improve detection and outcomes for prostate cancer in resource-constrained settings.