Submitted:
11 October 2023
Posted:
16 October 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Subjects
2.2. Methods
2.2.1. Specialist Diagnosis
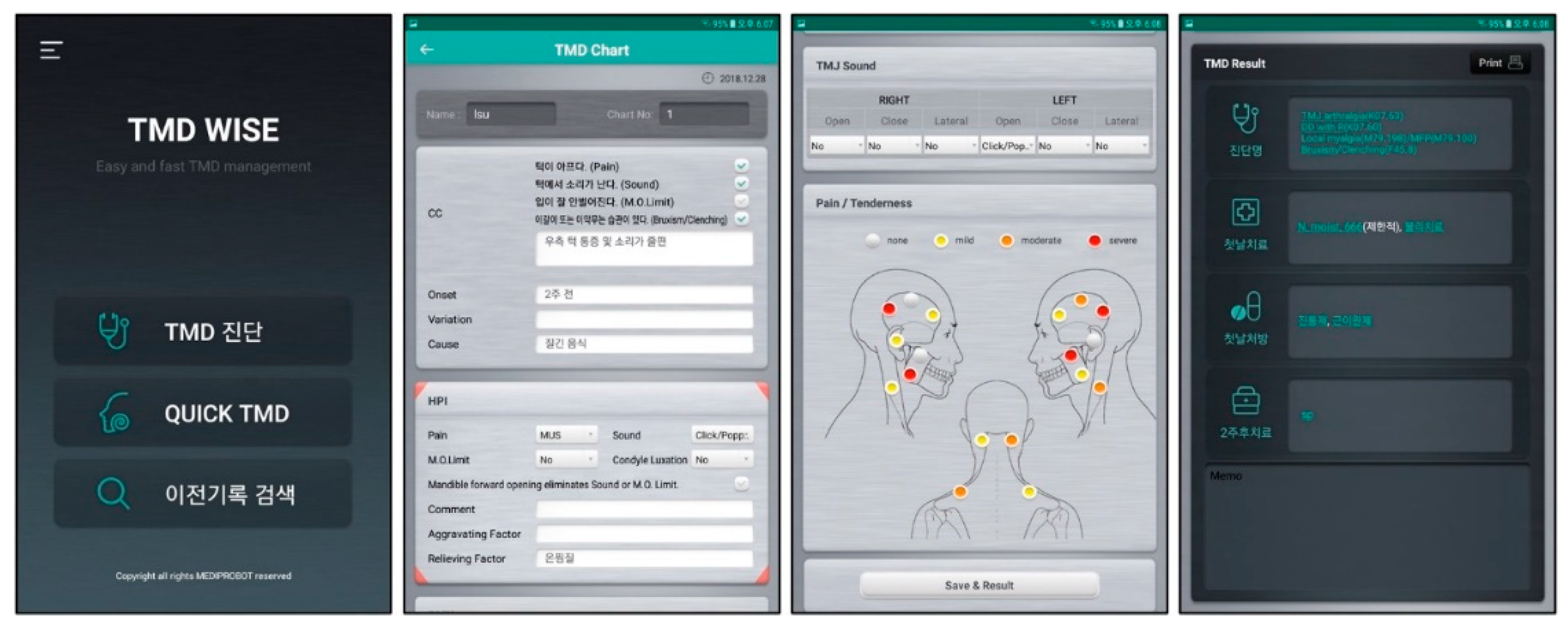
2.2.2. Diagnosis by the Diagnostic Mobile Application
2.2.3. Further Imaging
2.3. Statistical Analysis
3. Results
3.1. Validity Assessment
3.2. Imaging
4. Discussion
- (1)
- Comparing the concordance rate between the tool and specialists’ diagnoses.
- (2)
- Calculating sensitivity, specificity, and PPV for seven different diagnostic impressions.
- (3)
- Conducting additional evaluation using further imaging.
- (4)
- Comparing the clinical diagnosis made by specially trained clinicians with the actual imaging results.
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Dang, A.; Arora, D.; Rane, P. Role of digital therapeutics and the changing future of healthcare. J. Fam. Med. Prim. Care 2020, 9, 2207–2213. [Google Scholar] [CrossRef]
- Rastegayeva, I. The rise of digital therapeutics [monograph on the Internet] Dassault Systèmes Dassault Systèmes North America. 2019. Available online: https://blogs 3dscom/northamerica/the-rise-of-digital-therapeutics/ Updated 2019 Sept 10; Cited 2020 Jan 09.
- Martin, M. The dawn of digital therapeutics [monograph on the Internet] Platypus. Available from: http://blogcastacorg/2019/04/the-dawn-of-digital-therapeutics/ Updated 2019 Apr 16; Cited 2020 Jan 09.
- Hird, N.; Ghosh, S.; Kitano, H. Digital health revolution: Perfect storm or perfect opportunity for pharmaceutical R&D? Drug Discov Today 2016, 21, 900–911. [Google Scholar] [PubMed]
- Schiffman, E.; Ohrbach, R.; Truelove, E.; Look, J.; Anderson, G.; Goulet, J.P.; List, T.; Svensson, P.; Gonzalez, Y.; Lobbezoo, F.; et al. . International RDC/TMD consortium network, international association for dental research; orofacial pain special interest group, international association for the study of pain. J. Oral Facial Pain Headache 2014, 28, 6–27. [Google Scholar] [CrossRef] [PubMed]
- Scrivani, S.J.; Keith, D.A.; Kaban, L.B. Temporomandibular disorders. N Engl J Med. 2008, 359, 2693–2705. [Google Scholar] [CrossRef] [PubMed]
- Scelza, G.; Amato, A.; Rongo, R.; Nucci, L.; D'Ambrosio, F.; Martina, S. Changes in COVID-19 Perception and in TMD Prevalence after 1 Year of Pandemic in Italy. Eur. J. Dent. 2022, 17, 771–776. [Google Scholar] [CrossRef] [PubMed]
- Michelotti, A.; Cioffi, I.; Festa, P.; Scala, G.; Farella, M. Oral parafunctions as risk factors for diagnostic TMD subgroups. J. Oral Rehabilitation 2010, 37, 157–162. [Google Scholar] [CrossRef] [PubMed]
- Association, A.D. HPI poll: Dentists see increased prevalence of stress-related oral health conditions. 2021, March.
- Colonna, A.; Guarda-Nardini, L.; Ferrari, M.; Manfredini, D. COVID-19 pandemic and the psyche, bruxism, temporomandibular disorders triangle. Cranio 2016, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Ohrbach, R.; Dworkin, S.F. The Evolution of TMD Diagnosis: Past, Present, Future. J Dent Res. 2016, 95, 1093–1101. [Google Scholar] [CrossRef]
- Choi, J.H.; Kim, I.K.; Oh, N.S.; Oh, S.S.; Kim, E.S.; Lee, S.H.; Yang, D.H. A Clinical Study in the Prognosis of the Temporomandibular disorder. J Korean Assoc Oral Maxillofac Surg. 2000, 26, 497–506. [Google Scholar]
- Young, A.; Gallia, S.; Ryan, J.; Kamimoto, A.; Korczeniewska, O.; Kalladka, M.; Khan, J.; Noma, N. Diagnostic Tool Using the Diagnostic Criteria for Temporomandibular Disorders: A Randomized Crossover-Controlled, Double-Blinded, Two-Center Study. J. Oral Facial Pain Headache 2021, 35, 241–252. [Google Scholar] [CrossRef]
- Yap, A.U.J.; Tan, K.B.C.; Hoe, J.K.E.; Yap, R.H.C.; Jaffar, J. On-line computerized diagnosis of pain-related disability and psychological status of TMD patients: a pilot study. J. Oral Rehabilitation 2001, 28, 78–87. [Google Scholar] [CrossRef]
- Lövgren, A.; Parvaneh, H.; Lobbezoo, F.; Häggman-Henrikson, B.; Wänman, A.; Visscher, C.M. Diagnostic accuracy of three screening questions (3Q/TMD) in relation to the DC/TMD in a specialized orofacial pain clinic. Acta Odontol. Scand. 2018, 76, 380–386. [Google Scholar] [CrossRef]
- Petersson, A. What you can and cannot see in TMJ imaging - an overview related to the RDC/TMD diagnostic system. J. Oral Rehabilitation 2010, 37, 771–778. [Google Scholar] [CrossRef]
- Akobeng, A.K. Understanding diagnostic tests 1: sensitivity, specificity and predictive values. Acta Paediatr. 2007, 96, 338–341. [Google Scholar] [CrossRef]
- Gallagher, J.E.; Hutchinson, L. Analysis of human resources for oral health globally: inequitable distribution. Int. Dent. J. 2018, 68, 183–189. [Google Scholar] [CrossRef] [PubMed]
- Benzian, H.; Williams, D. The challenge of oral disease: a call for global action. The oral health atlas, 2nd ed.; FDI World Dental Federation: Geneva, 2015. [Google Scholar]
- Organization, W.H. 2016. Global strategy on human resources for health: workforce 2030.
- Gallagher, J.; Wilson, N. The future dental workforce? British Dental Journal 2009, 206, 195–199. [Google Scholar] [CrossRef] [PubMed]
- Milani, R.S.; De Perière, D.D.; Lapeyre, L.; Pourreyron, L. Relationship Between Dental Occlusion and Posture. Cranio 2000, 18, 127–134. [Google Scholar] [CrossRef] [PubMed]
- Franco, A.L.; Gonçalves, D.; Castanharo, S.M.; Speciali, J.G.; E Bigal, M.; Camparis, C.M. Migraine is the Most Prevalent Primary Headache in Individuals with Temporomandibular Disorders. Journal of orofacial pain 2010, 24, 287–292. [Google Scholar]
- Shetty, S.; Pitti, V.; Babu, C.L.S.; Kumar, G.P.S.; Deepthi, B.C. Bruxism: A Literature Review. J. Indian Prosthodont. Soc. 2010, 10, 141–148. [Google Scholar] [CrossRef] [PubMed]
- LeResche, L.; Drangsholt, M. Epidemiology of orofacial pain: prevalence, incidence, and risk factors. Orofacial pain. From basic science to clinical management, 2nd ed.; Quintessence Publishing: Chicago, IL, USA, 2008; pp. 13–18. [Google Scholar]
- Okeson, J.P. 2019. Management of temporomandibular disorders and occlusion-E-book.: Elsevier Health Sciences.
- Ferreira, L.A.; Grossmann, E.; Januzzi, E.; de Paula, M.V.Q.; Carvalho, A.C.P. Diagnosis of temporomandibular joint disorders: indication of imaging exams. Braz. J. Otorhinolaryngol. 2016, 82, 341–352. [Google Scholar] [CrossRef] [PubMed]
- Dixon, D.C. Radiographic diagnosis oftemporomandibular disorders. Semin. Orthod. 1995, 1, 207–221. [Google Scholar] [CrossRef] [PubMed]
- Okeson, J.P.; de Leeuw, R. Differential diagnosis of temporomandibular disorders and other orofacial pain disorders. Dental Clinics 2011, 55, 105–120. [Google Scholar] [CrossRef] [PubMed]
- Mock, D. The differential diagnosis of temporomandibular disorders. Journal of orofacial pain 1999, 13, 246–250. [Google Scholar] [PubMed]
- Chu, K. An introduction to sensitivity, specificity, predictive values and likelihood ratios. Emerg. Med. 1999, 11, 175–181. [Google Scholar] [CrossRef]
- Shreffler, J. and M.R. Huecker. 2020. Diagnostic testing accuracy: Sensitivity, specificity, predictive values and likelihood ratios.
- Carvajal, D.N.; Rowe, P.C. Research and Statistics: Sensitivity, Specificity, Predictive Values, and Likelihood Ratios. Pediatr. Rev. 2010, 31, 511–513. [Google Scholar] [CrossRef] [PubMed]
- Smith, S.D. Diagnosis and treatment of temporomandibular joint disorders. J. Pain Symptom Manag. 1987, 2, 155–162. [Google Scholar] [CrossRef]
- Bezuur, J.N.; Habets, L.L.; Hansson, T.L. The recognition of craniomandibular disorders--a comparison between clinical, tomographical, and dental panoramic radiographical findings in thirty-one subjects. J Oral Rehabil. 1998, 15, 549–554. [Google Scholar] [CrossRef]
- Yap, A.U.; Lei, J.; Zhang, X.H.; Fu, K.Y. TMJ degenerative joint disease: Relationships between CBCT findings, clinical symptoms, and signs. Acta Odontologica Scandinavica 2023, 1–7. [Google Scholar] [CrossRef]
- Park, J.W.; Song, H.H.; Roh, H.S.; Kim, Y.K.; Lee, J.Y. Correlation between clinical diagnosis based on RDC/TMD and MRI findings of TMJ internal derangement. International journal of oral and maxillofacial surgery 2012, 41, 103–108. [Google Scholar] [CrossRef]
- Hwangbo, N.-K.; Woo, K.-C.; Kim, S.-T. Evaluation of Clinical Symptoms Improvement by Cognitive Behavioral Therapy Using a Smartphone Application in Patients with Temporomandibular Disorder. Healthcare 2023, 11, 1443. [Google Scholar] [CrossRef]
| Concordance rate | |
|---|---|
| Final diagnosis | 0.92921 |
| Provisional diagnoses | 0.855718 |
| Impression | Sensitivity | Specificity | Positive predictive value |
|---|---|---|---|
| Arthralgia | 0.891813 | 0.955696 | 0.977564 |
| Disc displacement with reduction | 0.950207 | 0.953668 | 0.950207 |
| Disc displacement without reduction | 0.97561 | 0.969499 | 0.740741 |
| Degenerative joint disease | 0.804348 | 0.949339 | 0.616667 |
| Muscle pain | 0.913525 | 0.938776 | 0.992771 |
| Spasm | 0.75 | 0.925403 | 0.075 |
| MRI | |
| Specialists’ diagnosis | 0.645833 |
| Application diagnosis | 0.583333 |
| Concordance rate | |
|---|---|
| Final diagnosis | 0.92921 |
| Provisional diagnoses | 0.855718 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




